Conservative Gingiva Addition/Reduction
Pink restorative materials offer a minimally invasive solution
Hugh Flax, DDS, AAACD, MICOI
Large class III defects create a vertical and horizontal deficiency in the edentulous ridge. Often, bone and soft-tissue surgical procedures fall short of achieving a natural esthetic result. There are limitations in the hard- and soft-tissue healing process and in multiple adjacent implants in the esthetic zone. These limitations may often necessitate the use of gingiva-colored “pink” restorative materials. When applied properly, prosthetic gingiva can overcome the limitations of grafting and should be considered in the initial treatment plan.1 This article demonstrates prosthetically driven modalities of additive/reductive care that are often needed to best serve patients.2
Case Presentation
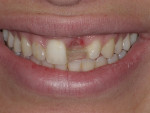
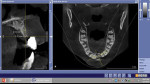
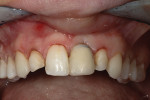
A healthy 20-year-old woman presented with a loose Maryland bridge that replaced tooth No. 9 using a preexisting porcelain-fused-to-gold crown as a pontic (Figure 1). The patient, who had a long history of anxious and unsuccessful dental treatments in this area, was interested in long-term options to improve both the esthetics and the stability of her smile. Preliminary photographs and a GALILEOS CBCT (Sirona; www.sironausa.com) were taken to three-dimensionally evaluate existing bone volume for implant therapy (Figure 2).
Because of a very large vertical and horizontal defect in the premaxilla, the patient was advised of the need for a sizeable initial osseous autograft that could also require one to three soft-tissue procedures, which together could take almost 6 to 9 months to complete prior to implant placement. Given the large time/financial investment, the patient opted for a predictable, less surgically aggressive plan that employed additive pink prosthetic materials in the defect area and closed-flap Erbium laser gingival osseous treatment to create a more-ideal “frame” around the much-smaller lateral incisors and an ovate pontic site.
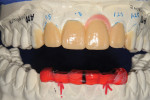
To properly plan the smile design and functional needs in this situation, the lab technician performed a detailed diagnostic wax-up. It laid out areas needing occlusal modifications with a reduction jig, as well as gingival reshaping/additions and tooth augmentations (Figure 3). This wax-up is a critical communication tool for collaboration between the restorative team and the apprehensive patient.
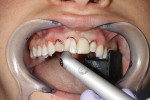
After a period of time to equilibrate, remove posterior decay, and whiten, the smile enhancement was begun, starting with altering the gingival frame as predetermined in the blueprint. After marking the changes in the soft tissue, the Erbium LiteTouch™ (AMD LASERS, www.amdlasers.com) was used to perform gingivoplasty with a chisel-shaped tip at the settings 200 mJ, 2.2 W, and 11 Hz with moderate distilled water irrigation (Figure 4 and Figure 5). The Maryland bridge was removed and gingivoplasty continued to create an ovate pontic space to allow esthetic and biologic success. Additionally, the sulci were sounded to bone, and normal 3-mm depths were noted to allow for proper biologic width.3 As a result, no closed-flap osseous modification was needed.
For esthetic color and proportional management, bonding was performed on each canine using All-Bond Universal™ (BISCO, www.bisco.com) and Estelite Omega® Shades B1, Bleach, and MW (Tokuyama Dental America; www.tokuyama-us.com). Conservative tooth preparation with intraenamel depth was performed for veneers on teeth Nos. 7 and 10, and a cantilever bridge abutment was performed on tooth No. 8, while using a preparation guide created from the diagnostic wax-up. Preparation shades were assessed and photographed, and all bite measurements were created to give to the laboratory. Full-arch polyvinyl siloxane impressions were made for the upper preparations and the opposing arch.
Provisionalization was started using a bleach-shade bis-Acryl material guided by a scalloped and relined silicone putty matrix. A tooth-focused “scaffold” was trimmed to the gingiva-restorative margins, as well as occlusal and esthetic modifications.
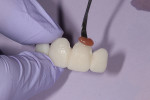
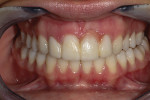
Gingival prosthetic enhancement of the pontic was performed using Beautifil II Gingiva (Shofu Dental Corporation; www.shofu.com) after treating the gingival area of tooth No. 9 with a microabrasive and composite resin. Using composite instruments and a camel’s hair brush, Beautifil II was easily sculpted (Figure 6), first extraorally and then with the provisional seated on the teeth to blend into the actual soft tissue and cured intraorally for 20 seconds and extraorally on all surfaces for an added 40 seconds. Gross adjustment was done with carbide burs, and polishing was performed in sequence with Shofu’s OneGloss Point and Super-Snap Extreme Discs, followed by a high-gloss finish with a SuperBuff Disc applying DirectDia Paste. The provisional was cemented reversibly, and the patient returned a week later for final shade selection and fine-tuning. She was ecstatic about the initial results (Figure 7).
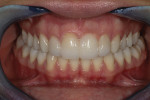
Our technician created an e.max® (Ivoclar Vivadent; www.ivoclarvivadent.com) central incisor cantilever bridge connected to veneers created for the laterals, which enhanced the functional strength that would have been reduced by the large pontic area. The restoration was bonded in place, following patient approval, using a select etch-bonding technique (Figure 8). Resin removal and occlusal adjustments were performed and an esthetic nighttime appliance created.
Conclusion
After many years of frustration, the patient has renewed confidence because of her new appearance. Although an implant would be an ideal correction of her problem, circumstances and patient temperament did not allow for a definitive surgical and restorative procedure. Fortunately, we have excellent materials and technology to offer a highly effective, minimally invasive solution to create not only an exceptional clinical result but a “raving fan” as well.
References
1. Coachman C, Salama M, Garber D, Calamita M, et al. Prosthetic gingival reconstruction in a fixed partial restoration. Part 1: introduction to artificial gingiva as an alternative therapy. Int J Periodontics Restorative Dent. 2009;29(5):471-477.
2. Garber D. The esthetic dental implant: letting restoration be the guide. J Oral Implantol. 1996;22(1):45-50.
3. Kois JC. Altering gingival levels: the restorative connection, Part I: Biologic variables. J Esthet Dent. 1994;6(1):3-9.
For more information, contact:
Shofu
800-827-4638
www.shofu.com
About the Author
Hugh Flax, DDS, AAACD, MICOI
Private Practice
Atlanta, Georgia