Digital Dentures
A paradigm shift in analog dentistry
David A. Burt, DDS, FICOI, FICD
The problem of edentulism or the total absence of one’s teeth has plagued mankind for centuries. Unlike many other animals that have an unlimited number of teeth or a dentition that continues to grow in their lifespan, humans possess only two sets, with the second or permanent set having to last a majority of one’s lifetime. These teeth are subjected to many environmental stresses and disease processes, which can leave one with the total loss of teeth well before the end of life.
Management of this condition up until the last 100 years has had limited success. The Etruscans gave us the first known attempts at tooth replacement by fabricating metal frameworks in which human or animal teeth were inserted around 700 BC.1 Wood was used by the Japanese in the early 16th century using softened beeswax for the impressions and then meticulously carving the wood to match the impression. In 1770, Alex Duchateau made the first porcelain dentures, which was the beginning of replacement teeth that were more durable and meant for function as well as appearance. Around 1850, vulcanite became the material of choice for dentures.2 It was a hard compound derived from rubber and it could be formed on models with porcelain teeth embedded in it to make it a reasonable dentition replacement exhibiting the first real attempt at form, fit, and function. The 20th century brought us acrylics and plastics, which are the standard of today. Although there has been a long history of advancement in denture materials, the fact remains that the way these prostheses are made is by hand. The labor-intensive requirements of hand setting the teeth, and preparing the prosthesis for fabrication is still the norm today, as it was centuries ago.
The explosion of technology in dentistry has shown that up to 60% of crown-and-bridge work is currently being done using a digital workflow by laboratories3 and CAD/CAM has allowed them to do far more using less manpower. With more than 31% of all adults over the age of 65 being edentulous today, and that number growing each year because of our aging population, the struggle to provide dental care for a growing edentulous population is increasing and dental labs will need to adjust accordingly. Many labs today are already experiencing a technician shortage along with an aging population of talented workers with the wisdom of years in designing dentures.5 Analog denture fabrication may not be able to keep up with the future demand.
This handcrafted, time-consuming approach to denture making has recently been challenged by the utilization of CAD/CAM and 3D printing.6 Along with the creation and development of software to establish the placement of teeth in a virtual environment, the new workflow represents an enormous step forward in the century old methods of denture making.
Since the first published report in 1994 of theoretical models and protocols by CAD/CAM, there have been a growing number of companies to refine the process and come out with a viable prosthesis. Pala (www.paladigitaldentures.com), Dentca (https://dentca.com), and Avadent (www.avadent.com) represent a few of the manufacturers able to deal with computer tomography, which allows software designers to read or see inner aspects of impressions to create positive virtual models of a human arch. Although the software programs developed by these companies are proprietary and a complete analysis of them is not available, a rationale for how they accomplish the process has been provided to the dental public. There are 26 anatomic landmarks including the fovea palatinus, hamular notch, incisive papilla, and others, which make up the human maxilla and mandible. Landmarks such as these are critical to lab technicians when beginning to decide where to place teeth to replicate what has been lost. Staub studied over 5,500 human models to determine that there are constant parameters or data points that are stable and reproducible when comparing one individual to another.7 He concluded that the masticatory apparatus is a determined data set, which can be recorded mathematically using clearly defined reference points. Staub further postulated that these cranial reference points can be the basis for a very close reconstruction of a person’s original dentition. The Staub system of cranial reference points is used to determine the basis of tooth position in an arch such as the intermolar distance or molar position, the interincisal distance or canine position, and the incisocervical length, which denture manufacturers have used in making mold sizing based on the central incisor length and width.
Dental software programs also use anthropometric averages, which is the science that deals with the systematic measurements of size, weight, and proportions of the human body. Body mass index is a typical example of an anthropometric study and such measurements are most likely used to refine tooth position, arch set up, and compensation for ridge resorption.
While traditional denture fabrication requires up to five patient visits and digital denture workflow claims a savings of two to three patient visits, as well as up to 50% reduction in chairtime and turnaround time at the lab.8 A further analysis of both methods can help to highlight the efficiency claimed by the digital technique.
Traditional Workflow
Taking records for a traditional set of dentures typically involves first acquiring a preliminary impression using alginate.9 The impression is then poured up and a custom tray is fabricated on the model. The patient is then brought back for a second visit where the final impression is achieved using either rubber base, polyether, or polyvinyl material. This impression is a refinement of the first and includes landmarks as well as border molding of the vestibules to make a master model on which the denture will be fabricated. A wax bite rim is then built on this model and the patient is scheduled for determination of vertical dimension of occlusion (VDO), centric relation (CR), occlusal plane, and general tooth position using the bite rim as a guide for the laboratory technician to be able to set teeth. When considering the measurement of VDO, dentists have been known to use a wide variety of instruments and objects to record and verify this. Boley gauges, calipers, tongue depressors, and dots on the face from a pen, have all been used.10 Many clinicians have developed their own process using parts of multiple systems to arrive at what they hope will be enough information for the lab to figure out the prescribed appearance of the dentures. CR or physiologic occlusion is also a measurement11 in that unless one uses some form of Gothic arch tracing to check protrusive, retrusive, and lateral excursions, one cannot effectively verify that the patient is able to duplicate it multiple times12 before capturing it on the bite rims.
In addition, most dentists do not pick the mould of teeth to be used but rather let the laboratory technician choose the central anterior tooth shape and size based on his or her preference and experience, along with any marks that were made on the wax rims by the dentist.
Digital denture workflow differs from traditional methods in that the first patient visit captures all impressions with border molding, CR, occlusal plane, VDO, and smile line. The CAD/CAM software can analyze the records, pick the appropriate tooth mould, and design a functional set up in a virtual reality. Adjustments and a try-in are accomplished with a computer rather than a wax spatula. There is a realization of eliminating two patient visits, over an hour of chairtime, and labor by a technician to physically set the teeth and festoon the case in comparison to the current analog process.
The fourth visit for the traditional method is the wax try-in of the setup, with the primary evaluation being that of esthetics, VDO, and CR. Because the teeth are held in place by wax on a shellac rim, it is very difficult to ascertain any function, denture retention, or even phonetics, due to the weakness of the wax holding the teeth and the inability of the base to closely approximate the intaglio. Adjustments have to be made by heating the base around teeth and then moving them by hand. Discrepancies of multiple teeth are difficult to correct and can leave the practitioner frustrated.
Digital denture workflow uses the data provided to create a simulated setup of a proposed denture, and when finished, sends it to the 3D printer for fabrication. The prototype denture is printed from a polymethyl methacrylate (PMMA) material and is basically the new denture in all aspects, including tooth mould, fit, occlusion, and base thickness. Advantages of a digital process is that a clinician can perform a more comprehensive evaluation of fit and function because the intaglio has been duplicated and the teeth are a replication of the selected mould in PMMA. Checking phonetics and even eating are possible with the try-in. Any changes that need to be addressed on the prototype are handled by trimming the material with a slow-speed handpiece or by marking it with a permanent marker.
In both methods, the case is sent back to the laboratory for finishing and processing of the dentures using standard injection techniques. The dentures are now ready for delivery to the patient.
Case Presentation
While denture fabrication can be challenging, the immediate denture adds another element of difficulty to the overall procedure. The presence of anterior teeth can prevent a check of esthetics at the try-in phase as well as create a space limitation of the denture base and teeth due to the unresorbed premaxilla at the time of extraction and delivery.
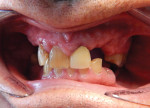
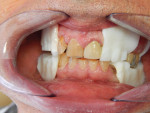
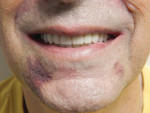
The patient presented with a severely broken down dentition as well as significant bite collapse, with a chief complaint of fractured teeth to the point that his existing maxillary partial would not stay in place and it was extremely difficult to eat (Figure 1). A review of his medical history revealed medical care for type 2 diabetes and high blood pressure. The treatment plan for maxillary and mandibular immediate dentures was presented and accepted. The case was determined to be ideal for using the Pala Digital Denture System (Heraeus Kulzer, www.heraeusdentalusa.com) because of the reduced visits and quick turnaround from the lab. The patient was then scheduled for the initial visit.
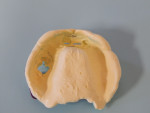
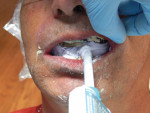
In the digital version of denture creation, all records needed for the final result are recorded in one visit. This involves taking regular analog impressions using polyvinyl siloxane and special trays provided with the Pala system, which record the ridge anatomy as well as the buccal fold and vestibular areas. In this case, the trays were cut out to allow the existing teeth to not interfere with seating of the tray. Border molding (Figure 2) was done at the time of the initial impression by using a two-part impression of heavy-body polyvinyl first, followed by a wash of a light-body polyvinyl and performing normal muscle movements to ascertain flange length (Figure 3), with the result being the use of these impressions as the master model for the denture.
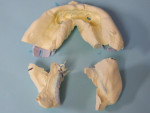
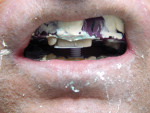
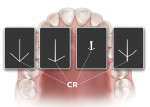
The impressions were then cut and separated (Figure 4) so as to prevent impingement of the trays with each other during the remainder of the procedure. When both impressions were completed, an intraoral tracing device was then plugged into the mandibular tray (Figure 5), similar to a Coble balancer, and the patient’s desired VDO was then determined by raising or lowering the pin (Figure 6). The Pala system includes tools to quantify the VDO before starting the case and then at any time until the end of record taking. Once the VDO was established and verified, and the number recorded, the patient then performed protrusive, retrusive, and lateral excursions, which are scribed by the VDO pin onto the maxillary tray pad.13 The lines drawn by the patient’s mandible represent the gothic arch tracing of the patient’s mandible with most recordings of these movements being either the shape of an arrow or one that resembles a chicken foot.14 The tip of the arrow, or the back of the chicken foot, represents the patient’s CR and was checked to determine if the patient could duplicate these movements (Figure 7). When this position could be reproduced to the clinician’s satisfaction, the trays were then locked in their respective position by using a fast-set bite registration material (Figure 8). The whole apparatus was then removed from the patient’s mouth, and the final measurement taken and recorded was the lip length from the premaxilla, using the other instrument provided. This measurement aids the designers in determining the amount of “show” of the maxillary incisors beyond the upper lip. These impressions and measurements represent all that was needed to fabricate the final dentures, which took an hour or less to record. The patient was dismissed and the case, along with the complete prescription, was sent to the laboratory.
The laboratory digitally scanned the impressions and sent the data to the design center where the software took over and duplicated the spatial relations of the arches. The impressions were fixed to then make a virtual articulator. Placement of the arches as well as the tooth set-up has been handled by proprietary software using data, such as the Staub Cranial Reference. This system can map more than 26 anatomic landmarks and determine the typical intermolar width, intercanine width, and incisocervical length of teeth that will fit the scanned arches.
The prototype denture was 3D printed and sent to the author’s office for a patient try-in and check of the VDO and CR (Figure 9). In this case, the VDO was found to be excessive and the correction was to reduce the posteriors of the try-in, thus allowing for a reduction in the vertical dimension. Bite registration material was then injected between the rims to record this new VDO. The case was then returned to the laboratory for any corrections made to the try-ins. The dentures were then fabricated using traditional injection techniques and returned to the office for delivery.
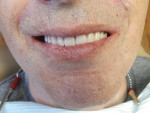
The patient’s third and final visit was for surgical extraction of all remaining teeth and seating of the prostheses (Figure 10). A soft reline was placed in the lower for initial comfort, while only minor adjustments were made to the upper using pressure indicator paste and visually checking for blanched tissue. The patient was pleased with the retention of the dentures. The occlusion was checked and adjusted and the patient was satisfied with the esthetics of the case. The patient was sent home and returned in 1 week for suture removal and further adjustments of sore spots in the peripheral flange area and the intaglio as needed (Figure 11 and Figure 12).
Conclusion
The Pala Digital Denture System has shown dentistry that the denture-making process can become more efficient in time, number of visits, and laboratory turnaround. While the initial patient visit still uses analog impressions, the remainder of the workflow uses CAD/CAM and 3D printing to reveal a true paradigm shift in the way dentistry approaches patient care.15
Disclosure
The author received an honorarium from Heraeus Kulzer for writing this article.
References
1. Edentulous: A Brief History of Dentures. www.premierexhibitions.com/exhibitions/4/4 bodies-exhibition/blog/edentulous-brief history-dentures. Accessed December 22, 2016.
2. British Dental Association. Teeth and dentures. www.bda.org/museum/collections/teeth-and-dentures. Accessed December 22, 2016.
3. Molinaro K. Digital Trends You Need to Know. NADL Materials and Equipment survey, https://lmtmag.com/articles/digital-trends-you-need-to-know. 2014. Accessed jnuary 3, 2017. 2015.
4. Centers for Disease Control and Prevention. Vargas CM, Kramarow EA, Yellowitz JA. The Oral Health of Older Americans. Trends in Health and Aging. https://www.cdc.gov/nchs/data/ahcd/agingtrends/03oral.pdf. Accessed January 12, 2017.
5. Schweiger J, Güth JF, Edelhoff D, Stumbaum J. Virtual evaluation for CAD-CAM-fabricated complete dentures. J Prosthet Dent. 2016 Aug 1. [Epub ahead of print.]
6. Battersby J. CAD/CAM – The end for dental labs or a new beginning? https://www.dentistryiq.com/articles/2014/05/cad-cam-the-end-for-dental-labs-or-a-new-beginning.html. 2014. Accessed January 3, 2017.
7. Staub Cranial Healthy Dentures Theoretical Summary. January 2011. www.staub-cranial-de/dokumente/StaubCranial-Healthy-dentures Jan 2011. Accessed December 22, 2016.
8. Dichter D. Conventional Complete Denture Fabrication in 9 Steps. Spear Education. https://www.speareducation.com/spear-review/2015/10/conventional-complete-denture-fabrication-in-9-steps. Accessed October 21, 2016.
9. Barzilay I. Saving time and money with the right impression material. https://www.dentaleconomics.com/articles/print/volume-100/issue-3/features/saving-time-and-money-with-the-right-impression-material.html. Accessed January 3, 2017.
10. Medwedeff FM. Oral reconstruction: an instrument to establish vertical and physiologic occlusion. J Am Dent Assoc. 1983;107(3) 443-445.
11. Thakur M, Jain V, Parkash H, Kumar P. A comparative evaluation of static and functional methods for recording centric relation and condylar guidance: a clinical study. J Indian Prosthodont Soc. 2012;12(3):175-181.
12. Mysore AR, Aras MA. The magic slate as recording medium for Gothic arch tracing. J Prosthet Dent. 2012;108(1):60.
13. Daher T, Lobel WA, Massad J, et al. Predictable technique to register Retruded Contact Position (RCP) using a disposable jaw relation recording device. Compend Contin Educ Dent. 2015;36(5):323-329; quiz 330.
14. Radz GM. Digital dentures: achieving precision and esthetics. Dent Today. 2016;35(6):77-78, 80.
15. Kattadiyil MT, Alhelal A. J Prosthet Dent. 2016 Oct 27. Pii:s0022-3913(16) 30375-4. Doi:10-1016/prosdent.2016.08.017