Direct Resin Restoration: A complete technique from preparation to polishing
Gregori M. Kurtzman, DDS, MAGD
Direct resin restorations are the most common treatment rendered in the general practice. A systematic approach to preparation and placement of these restorations improves efficiency and predictability and simplifies finishing. The case presented here outlines a technique for direct resin restoration that includes careful material selection and a finishing and polishing protocol providing highly esthetic, durable outcomes.
Adhesive Considerations
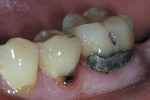
In this case, caries and defective restorative materials (Figure 1) were removed with carbides and diamonds with a high-speed handpiece. Subsequent adhesive selection dictated how the smear layer would be managed and how much enamel was present after preparation.
Total-etch adhesives (ie, fifth generation) require removal of the smear layer, which occurs when the dentin is acid-etched. Self-etch adhesives (seventh generation) are able to penetrate through the smear layer to create a hybrid layer with the underlying dentin.1 Maintenance of the smear layer with self-etch adhesives is associated with much lower postoperative sensitivity compared to the use of total-etch adhesives.2 Total-etch adhesive systems are therefore recommended when large areas of enamel are present around the preparation, whereas self-etch adhesives provide a more predictable bond and superior strength to dentin and are recommended when the preparation is predominantly supported by dentin.3 Some clinicians use a selective-etch technique (self-etch plus separate etch in enamel only) as this maximizes bond strength, but is also much more technique sensitive.
Direct Resin Placement
The teeth were isolated and a sectional matrix (Slick Band™ XR, Garrison Dental Solutions, https://garrisondental.com) was placed on the distal of the second premolar. A Composi-Tight® 3D Fusion (Garrison Dental Solutions) wedge was placed interproximally. A Composi-Tight 3D ring (Garrison Dental) was placed to shape the composite.
A selective-etch, self-etch adhesive (Connexio Bond, Centrix Dental, www.centrixdental.com) was mixed and applied with a Benda® Micro applicator (Centrix) to the dentin surface only, and then light-cured for 20 seconds. In this case, to ensure the highest bond to the enamel margins, a selective-etch technique was used. Onyx™, a 40% phosphoricacid-etching gel (Centrix), was applied to the enamel only, rinsed after 20 seconds, and then air-dried. An additional coat of adhesive was applied to all enamel and dentin surfaces and light-cured.
A thin layer of VersaFlo (Centrix) was applied into the proximal box and across the pulpal floor as a liner and then light-cured. As flowable composite resins adapt better than stiffer composites (hybrids, microfills, and nanoresins), they seal the dentin better, decreasing the risk of postoperative sensitivity.4,5 The remainder of the proximal box was filled to the level of the pulpal floor with VersaLite Composite Resin (Centrix) and light-cured. A final layer of VersaLite Composite Resin was placed and the appropriate anatomy formed before light-curing. If the preparation is very deep, a layer of VersaFlo Flowable Composite (Centrix) can be placed over the flowable liner, as this has a deeper depth of cure and can be placed in thicker increments (up to 4 mm). For anterior restoratives, a final layer of chameleon-like microfill can be placed for maximum esthetics and overlayed with a nanoresin as the final layer. The author’s preference is to use a final layer of microhybrid or nanoresin because of its better wear characteristics and higher gloss potential after polishing.6 The ring, wedge, and matrix were then removed and the cervical preparations addressed.
Connexio Self-Etch Bond was applied to both cervical preparations with a Benda micro applicator and light-cured. Under occlusal loading during mastication or tooth-to-tooth contact, the tooth can microflex, leading to restoration “pop-out” or opening of the gingival margin. Stiffer resins have a modulus of elasticity greater than the tooth, and are therefore prone to this in the cervical area. Flowable resins are more flexible, having similar modulus of elasticity as the teeth, and are less prone to issues on the cervical. Because this is a low-wear area, the flowable resins are ideally suited as the final restorative material. As a result of the depth of the preparation, VersaFlo Flowable Composite Resin was applied to fill half the cervical preparations and light-cured. A final layer of VersaLite was placed to full contour and light-cured.
Finishing and Polishing
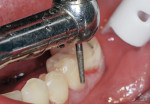
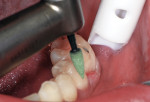
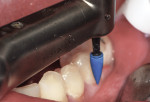
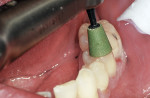
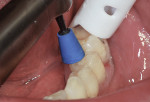
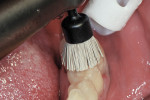
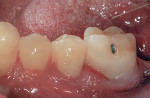
Finishing was initiated by shaping and contouring the composite restorations with a finishing diamond (Komet USA, www.kometusa.com) in a high-speed handpiece with water spray (Figure 2). Once the shape and contour were established, the buccal surface was polished using a medium (green) Couture Diamond Finishing Point in a slow-speed handpiece with very light pressure and water spray (Figure 3). This was repeated with the ultrafine (blue) Diamond Polishing Point using very light pressure and water spray to reach a high gloss finish (Figure 4). A Couture Diamond Finishing Cup in medium (green) and Couture Diamond Polishing Cup in ultrafine (blue) were utilized to polish the occlusal surface (Figure 5 and Figure 6). The cups work well on the occlusal surface, and fit its anatomy, whereas the points are better suited to the buccal/lingual and proximal surfaces. Very light pressure with water spray is recommended, as higher pressure will actually leave a rough surface after application. An alternative to using water with the cups is the use of Couture Diamond Polishing Paste as a lubricant during polishing. For maximum polish and the smoothest surface finish, use the Couture Diamond Polishing Brush (Centrix), also used with light pressure and water application at a slow speed (Figure 7). The final restorations demonstrate a very smooth, highly polished finish, providing a durable restoration (Figure 8).
Conclusion
Direct resin restorations can be simplified with the Couture restorative system, providing predicable results and culminating in a highly polished, direct restoration with minimal effort in just a few simple steps. A surface with better polish on the resin yields less plaque and stain adherence, and provides long-term esthetics.7 Additionally, this has a positive effect on gingival marginal health due to less plaque retention, meaning lower inflammation. With significant research showing the role of oral inflammation in systemic health, it is more important than ever that clinicians take all available steps to finish restorations to maximize hard- and soft-tissue health.
Disclosure
Gregori M. Kurtzman, DDS, MAGD, has received honoraria from Centrix Dental for writing this article.
References
1. Mine A, De Munck J, Cardoso MV, et al. Dentin-smear remains at self-etch adhesive interface [published online August 13 2014]. Dent Mater. 2014;30(10): 1147-1153.
2. Yousaf A, Aman N, Manzoor MA, et al. Postoperative sensitivity of self etch versus total etch adhesive. J Coll Physicians Surg Pak. 2014;24(6):383-386.
3. Ozer F, Blatz MB. Self-etch and etch-and-rinse adhesive systems in clinical dentistry. Compend Contin Educ Dent. 2013;34(1):12-14, 16, 18; quiz 20, 30.
4. Sadeghi M. Influence of flowable materials on microleakage of nanofilled and hybrid Class II composite restorations with LED and QTH LCUs. Indian J Dent Res. 2009;20(2):159-163.
5. Lokhande NA, Padmai AS, Rathore VP, et al. Effectiveness of flowable resin composite in reducing microleakage - an in vitro Study. J Int Oral Health. 2014;
6(3):111-114.
6. St Germain H, Samuelson BA. Surface characteristics of resin composite materials after finishing and polishing. Gen Dent. 2015;63(2):26-32.
7. Jefferies SR. Abrasive finishing and polishing in restorative dentistry: a state-of-the-art review. Dent Clin North Am. 2007;51(2):379-397.
Gregori M. Kurtzman, DDS, MAGD
Private Practice
Silver Spring, Maryland
For more information, contact:
Centrix, Inc.
800-235-5862