Maximizing Esthetics and Function with Immediate Implant Placement
A guide to ensuring stability and ideal positioning
Jason Kim, DDS
The concept of immediate implant placement has taken on a new role in the treatment planning of dental implants. With this approach, it is no longer a prerequisite to let an extraction site heal for 4 to 6 months before placing a dental implant. Provided that certain criteria are met, implants can now be placed at the time of extraction. Original protocol was such that in order for dental implants to be successful, they had to be submerged for a period of time to achieve osseointegration.1 There is now evidence to support the fact that implants can be placed at the time of extraction and both achieve osseointegration and maximize esthetics and function.2,3 There are benefits to being able to simultaneously extract a tooth and place an implant. There are fewer surgeries involved, it takes less time to complete the case, and hard and soft tissues can be preserved. Along with the benefits also come some risk factors. Some of these may include but are not limited to: implant failure, infection, bone resorption, and soft tissue recession.4
In cases of immediate implant placement, it is imperative to have a prosthetically driven treatment plan. The final restoration must be determined prior to having any type of surgical treatment. If a prosthetically driven approach is taken, the type of restoration will dictate the treatment flow for the case. Implant position will determine whether a screw- or cement-retained restoration can be fabricated.
A screw-retained restoration has its advantages in that there is always retrievability. The other advantage is not having complications related to over-retained cement in the gingival sulcus. For a screw-retained restoration, the implant placement must be in a lingually inclined position. That position must allow the screw access hole to emerge from the cingulum of the tooth to be restored. The slightest change in angulation negates the ability to have a screw-retained restoration but can still be restored as a cement-retained restoration.5 Depending on clinician preference, the ability to have a screw- or cement-retained restoration is dependent upon appropriate implant placement.
Primary Stability
Patients today are not only asking to complete their cases faster, but implant companies are claiming to reduce treatment times with newer implant technologies and improved surgical techniques.
Immediate implant placement can be implemented provided that specific parameters are met. When planning for immediate implant placement, the first criterion that must be met is primary stability. To achieve primary stability, the implant must extend beyond the apex of the socket by 4 mm. Anything less than this may compromise the initial stability. The implant must engage bone beyond the apex because the extraction socket dimensions are going to be much larger than the size of the implant being placed. In cases involving the anterior esthetic zone, one must be wary of the tissue remodeling that will occur following tooth extraction. The result is more buccal bone resorption than the lingual wall.6
Extraction
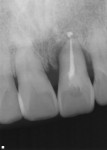
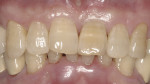
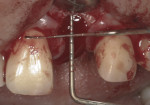
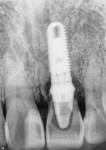
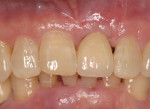
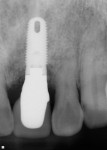
There are specific guidelines that must be met for one to be able to extract a tooth and place an implant at the same time. Figure 1 and Figure 2 show a preoperative radiograph and photograph of a failing tooth that is periodontally involved. When placing an implant at the time of extraction, care must be taken to remove the tooth as atraumatically as possible. The main purpose of this is to preserve as much bone as possible, especially the buccal plate. Any fracture of the buccal plate, especially at the crest where it is thinnest, can compromise the intended result with implant placement. This can be done utilizing periotomes, elevators, and piezosurgery technology, among others. The socket is then debrided to eliminate any infection, soft tissue, and granulation tissue. Planning should have already involved evaluating whether a thick or thin soft tissue biotype is present. A thick biotype will promote long-term stability as well as allow for flapless extraction and implant placement. Thin biotypes are more prone to recession following healing, which allows the implant to show through, compromising esthetics.
3D Implant Positioning
Step 1
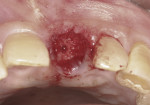
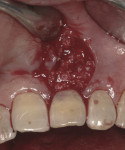
The next phase is to begin the osteotomy preparation. In the anterior esthetic zone, it is important to engage the palatal wall of the socket. This must be initiated approximately two thirds of the way down the socket.7 Figure 3 shows the direction of the osteotomy in relation to the palatal wall. This will ensure that the implant does not perforate the thin buccal wall and engages the denser bone of the palatal wall. In posterior regions, it is best to stay slightly more lingual and to go beyond the apex of the socket to ensure adequate initial primary stability.
Step 2
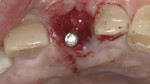
The implant should be placed inside the incisal line angle of the adjacent teeth. This will ensure adequate facial bone thickness for long-term stability and keep the implant from protruding too far facially (Figure 4).
Step 3
Maintain a space of at least 1.5 mm from adjacent tooth to the implant. Depth of implant placement should be 3 to 4 mm below the cementoenamel junction of the adjacent teeth or the free gingival margin. Maintaining this depth will give enough “running room” to create the proper emergence profile (Figure 5).8
The size of the implant should be determined by the amount of space between the adjacent teeth and available bone around the implant. Traditional protocol called for the widest diameter implant to be placed into the socket so as to obliterate the socket. It is now understood that a minimum of 1.5 mm of space between the implant and the adjacent must be maintained with at least 1 mm of bone circumferentially around the implant.
Step 4
Maintain at least 2 mm of facial bone thickness for long-term esthetic stability.9 Having a narrower diameter implant placed at the time of extraction will leave a gap between the implant and buccal plate.
This gap, if less than 2 mm, does not require any bone grafting. If the gap distance is greater than 2 mm, grafting is recommended.10 As a result of the thin buccal plate remaining after extraction, grafting the void as well as the facial bone is carried out regardless of the space between the implant and bone. This means having to raise a flap to graft the facial plate to ensure a minimum of 2 mm of facial bone thickness (Figure 6).
Temporization
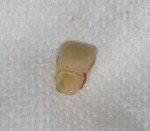
To maximize esthetics, the patient’s natural tooth can be used as a provisional. If the root is cut off and the tooth hollowed out, it can be relined over the temporary abutment (Figure 7). A temporary abutment supported the cemented natural provisional during healing (Figure 8). Maximum soft tissue support maturation is achieved after 4 months. The natural provisional allows for proper emergence development.
A radiograph and photograph after final crown insertion (Figure 9 and Figure 10) verified the preservation of bone and soft tissue support. According to Tarnow and colleagues, papilla formation will occur if the distance from the contact point to the interproximal crest of bone is 5 mm or less.11
Conclusion
Immediate implant placement can be a predictable procedure provided that certain guidelines are followed. This treatment option, along with provisionalization, will enhance and preserve osseous and gingival architecture for long-term stability. Though this procedure can be technique sensitive, it goes without saying that proper treatment planning and case selection will allow for optimal results that will give maximum function and esthetics.
References
1. Adell R, Lekholm U, Rockler B, Bránemark PI. A 15-year study of osseointegrated implants in the treatment of the edentulous jaw. Int J Oral Surg. 1981;10(6):387-416.
2, Kan JY, Rungcharassaeng K, Lozada J. (2003) Immediate placement and provisionalization of maxillary anterior single implants: 1-year prospective study. Int J Oral Maxillofac Implants. 2003;18(1):31-39.
3. Wöhrle PS. Single-tooth replacement in the aesthetic zone with immediate provisionalization: fourteen consecutive case reports. Prac Periodontics Aesthet Dent. 1998;10(9):1107-1114.
4. Araujo MG, Sukekava F, Wennstrom JL, Lindhe J. Tissue modeling following implant placement in fresh extraction sockets. Clin Oral Implants Res. 2006; 17(6):615-624.
5. Hebel KS, Gajjar RC. Cement-retained versus screw-retained implant restoration: achieving optimal occlusion and esthetics in implant dentistry. J Prosthet Dent. 1997;77(1):28-35.
6. Botticelli D, Berglundh T, Lindhe J. Hard-tissue alterations following immediate implant placement in extraction sites. J Clin Periodontol. 2004;31(10):820-828.
7. Misch CE. Anterior single-tooth replacement: surgical considerations. In: Misch CE, ed. Contemporary Implant Dentistry. 3rd ed. St Louis, Mo: Mosby; 2008:755-758.
8. Sonick MK. The maxillary central incisor implant: A guide for ideal esthetic implant placement. Inside Dentistry. 2005;1(1):72-76.
9. Huynh-Ba G, Pjetursson BE, Sanz M, et al. Analysis of the socket bone wall dimensions in the upper maxilla in relation to immediate implant placement. Clin Oral Implants Res. 2010;21(1);37-42.
10. Chen ST, Wilson TG Jr, Hämmerle CH. Immediate or early placement of implants following tooth extraction: review of biologic basis, clinical procedures, and outcomes. Int J Oral Maxillofac Implants. 2004;19 Suppl:12-25.
11. Tarnow DP, Cho SC, Wallace SS. The effect of inter-implant distance on the height of inter-implant bone crest. J Periodontal. 2000;71(4):546-549.