Communication: Essential in Life and Dentistry
A veneer case illustrating ideal collaboration with patient and laboratory
Communication is the basis of our lives, and we would certainly be handicapped without it. Every day we communicate with each other in some way or another; we convey messages through both words and actions. This certainly holds true with our interactions with our patients and colleagues.
Effective patient communication is one key to delivering quality care. Good communication is not only extremely necessary for informed consent and patient acceptance, but it is also a means to avoid errors, improve quality, and achieve ideal results. An equally important key to quality care, especially when delivering indirect restorations to the anterior segment, is laboratory communication. Proper communication is critical, especially when restoring one or two anterior teeth in an attempt to match the intricacies of the existing dentition.
Case Presentation
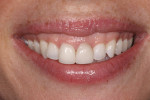
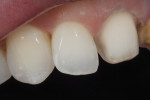
A female patient presented with a chief complaint of being unhappy with the shape and color of the existing veneers on teeth Nos. 8 and 9 (Figure 1). Preoperative photos were taken and diagnostic casts were made and mounted on an articulator with a face-bow transfer to evaluate the existing restorations. From this, a list of problems in regards to the anterior restorations was discussed and reviewed with the patient, and the author and patient finalized exactly what would be addressed, which included:
Canted midline
Tooth size and shape discrepancy
Color difference as compared to the natural dentition
The next step on the journey to an ideal result was to first correct the cant and size discrepancies. It was explained to the patient that she and the author would review the diagnostic wax-up prior to moving forward because it would serve as a template for both the final restorations and for the provisionals she would wear during fabrication of the veneers. The existing mounted casts and preoperative photographs were sent to the laboratory for a diagnostic wax-up of Nos. 8 and 9 with very specific instructions of what to correct. Along with the wax-up, the lab returned a silicone matrix for fabrication of the provisionals, as well as reduction guides to ensure that proper preparation was achieved for the lab to have enough room to satisfy the esthetic demands. An appointment was scheduled with the patient to review the wax-up. Once accepted by the patient, treatment could proceed.
Treatment Protocol
The patient presented for the preparation, impressioning, and provisionalization appointment. Following achievement of profound anesthesia with 3.6 cc 4% Septocaine® (Septodont, www.septodontusa.com) via infiltration, the soft tissue was re-contoured with an Odyssey® Diode Laser at 1.2 W (Ivoclar Vivadent, www.ivoclarvivadent.us) to achieve symmetry in shape and gingival architecture between the two central incisors. The existing veneers were removed and the underlying teeth were prepared. Following final preparation and prior to impressioning, Expasyl® (Kerr, www.kerrdental.com) was placed in the gingival sulcus for retraction and hemostasis and allowed to sit for 3 minutes as the patient bit down on Comprecaps (Coltene, www.coltene.com). After 3 minutes, the Expasyl was rinsed with copious irrigation. A full upper-arch impression was taken with light and heavy body polyvinylsiloxane (Ivoclar Vivadent). A counter-impression in alginate, face-bow transfer, and stick bite were taken.
Laboratory Communication
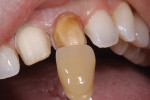
At this point, it was important to gather and share as much information about the underlying teeth for the laboratory, so that the proper stump dies can be fabricated. As evident in the stump photo (Figure 2), there was a significant difference in the underlying stump shade between Nos. 8 and 9. If this were not communicated to the laboratory properly, it would indeed affect the color of the final prostheses and almost definitely result in an incorrect shade match between the two veneers as well as between the veneers and the natural dentition.
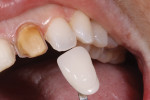
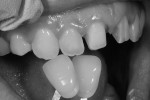
Next, communication of the shade and characterizations of the natural dentition were recorded and shared with the laboratory so that a replication of nature can take place. To be truly effective, communication with the laboratory must go far beyond the too often seen prescription, “Fabricate 2 veneers shade B1.” In this case, a shade tab first was photographed against the natural dentition (Figure 3), represented by No. 7, with a VITA 3D-MASTER shade tab 0M3 (VITA Zahnfabrik, www.vita-zahnfabrik.com). An additional photo with a similar shade tab was taken and converted to black and white so the value of the chosen shade tab could be confirmed (Figure 4). Finally, a polarized photograph (polar_eyes, Photomed, www.photomed.net) of the natural tooth No. 7 was taken so that the laboratory could clearly see any translucencies, haloes, or additional incisal effects needed in the final restorations (Figure 5). A cross-polarization filter, polar_eyes is designed to eliminate unwanted reflections on the teeth that are caused by the flash. A detailed lab slip, along with all of the photographs taken, was submitted to the laboratory.
Provisional Phase
At this point, provisional restorations were fabricated using the silicone matrix fabricated from the diagnostic wax-up (InstaTemp, Sterngold, www.sterngold.com). They were trimmed out of the mouth and cemented with spot etch and flowable resin. The patient was then sent home and scheduled to return in 24 hours following evaluation of the provisionals by herself and her family.
At the follow-up appointment 24 hours later, the patient informed the author that she was thrilled with everything about the provisionals. Photographs of the provisionals were taken (Figure 6) and submitted to the laboratory. Since no adjustments were made to the provisionals, the lab was instructed to duplicate the wax-up exactly to create the final prostheses. The final restoration chosen were pressed Empress veneers (Ivoclar Vivadent) utilizing the cut back technique for the requested characteristics.
Final Delivery
The patient returned 3 weeks later for insertion. Once again local anesthetic was administered. The provisionals were removed and the preparations were first cleaned with aluminum oxide via PrepStart™ (Danville, www.danvillematerials.com), followed by a chlorhexidine scrub. The veneers were tried in with clear CHOICE™ try-in paste (BISCO, www.bisco.com) and a photograph was taken to confirm the value and color match. The veneers were then treated as per the manufacturer’s instructions. Size 0 cord (Ultradent, www.ultradent.com) was placed in the gingival sulcus of Nos. 8 and 9. The preparation surfaces were etched for 15 seconds with 37% phosphoric acid with benzalkonium chloride (BISCO). They were then rinsed for 15 seconds and blotted dry with a cotton roll to avoid desiccation. Two coats of ALL-BOND 3® (BISCO) were applied for 10 seconds each, followed by air drying and light curing for 10 seconds after each coat. The veneers were cemented with CHOICE™ 2 translucent cement (BISCO) as per the manufacturer’s instructions. Following cementation, finishing, polishing, and occlusal adjustments, the patient was dismissed.
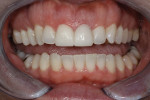
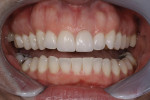
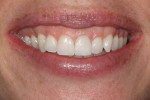
The patient returned 2 weeks later for a follow-up appointment and postoperative photographs (Figure 7 and Figure 8), which demonstrate how the overall dynamic of her smile changed drastically for the better. The improvements to the shape, size, and color of the newly inserted veneers made for one happy patient.
Importance of Effective Communication
They say that one key to a successful relationship requires paying attention to the small moments and investing them with attention and importance. This can make a big difference toward a couple’s overall satisfaction in their relationship. The same holds true for our relationships with our laboratories and, more importantly, our patients. In spite of the increased importance placed on communication, many practitioners and laboratories continue to struggle with this skill and are unable to communicate their thoughts and ideas effectively. This inability could make it nearly impossible for them to deliver exceptional dentistry and ultimately stand in the way of what could be a wonderful career in dentistry.
About the author
Adamo E. Notarantonio, DDS, FICOI, AAACD
Huntington Bay Dental
Huntington, New York
References
1. Photographic Documentation and Evaluation in Cosmetic Dentistry: A Guide to Accreditation Photography. Madison, WI: American Academy of Cosmetic Dentistry; 2009.
2. Loiacano P, Pascoletti L. Photography in Dentistry: Theories and Techniques in Modern Documentation. Hanover Park, IL: Quintessence Publishing Co; 2012.
3. Chu SJ, Devigus A, Paravina, RD, Mieleszko A. Fundamentals of Color: Shade Matching and Communication in Esthetic Dentistry. Hanover Park, IL: Quintessence Publishing Co; 2010.
4. Dawson PE. Functional Occlusion: From TMJ to Smile Design. St. Louis, MO: Mosby, Inc; 2007.
5. Hamlett KM, Rosenthal LW. Steps in creating a beautiful smile. Journal of Cosmetic Dentistry. 2008;20(4):92-96.
6. Alex G. Is total etch dead? Evidence suggests otherwise. Compend Contin Educ Dent. 2012;33(1):12-4, 16-22, 24-5; quiz 26, 38.
7. Suh B.I. Principles of Adhesive Dentistry: A Theoretical and Clinical Guide for Dentists. Newtown, PA: AEGIS Publications, LLC; 2013.
8. Alex G. Preparing porcelain surfaces for optimal bonding. Compend Contin Educ Dent. 2008;29(6):2-14.