Contralateral/Opposite-Arch Zirconia Crown Restoration of Two Mandibular Primary First Molars
A tooth-colored solution to restoring damaged primary teeth
Restoration of severely carious, malformed, or fractured primary first molars has been best achieved for more than half a century using preformed stainless steel crowns.1-3 When properly adapted and cemented on correctly prepared teeth, such crown forms are ideal in every respect except one—they are silver colored. Many children enjoy their silver "super hero" or "princess" teeth, and many parents have no concerns with their silver color. However, more and more modern-day parents desire tooth-colored tooth repair, whether for "fillings" or full coronal coverage.
In the past few years, preformed zirconia crowns have been introduced by a number of manufacturers, not only for primary anterior teeth, but also for primary molars. These crown forms have extraordinary strengths and can withstand routine masticatory and occlusal impact forces without fracturing. They also have a natural tooth-colored appearance and are generally imperceptible at routine conversation distance.
The biggest difference when using zirconia crowns versus stainless steel crowns is that preparation of the tooth must be adapted to the selected crown, unlike the stainless steel crown procedure, in which the crown form must be adapted to ideally fit the prepared tooth.
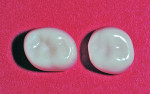
From the occlusal view, maxillary primary first molars are rounder than mandibular primary first molars, which can be described as roughly rhomboidal with curved sides and corners (Figure 1). In the rare instance that a mandibular primary first molar is rounder than normal, a clinician can substitute a contralateral/opposing-arch stainless steel crown form to fit the lower molar more ideally.3 For example, a crown designated as UL6 (upper left size 6) might fit a mandibular right primary first molar better than the LR6 (lower right size 6), or even the LR5 or LR7. The authors could find no reports of similarly substituting a contralateral/opposing-arch zirconia primary first molar crown in that clinical circumstance. This report documents such a case.
Case Presentation
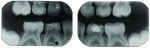
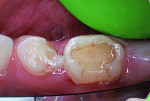
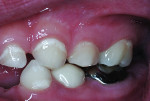
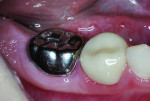
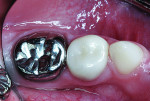
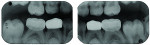
A 7-year-old boy presented with caries of his mandibular primary first and second molars involving multiple surfaces of each tooth (Figure 2 and Figure 3). The mandibular right primary first molar also had a buccal coronal shear fracture associated with a distal surface caries lesion (Figure 3). Full-coverage crowns were indicated for all four mandibular primary molars. The right second molar had a large occluso-lingual resin-modified glass-ionomer restoration that had been placed as an interim sedative filling months before (Figure 3). The boy's mother said that she would prefer tooth-colored crowns for the first primary molars and had no preference for the second molars. She scheduled her son for two restorative dentistry appointments. The plan was to restore the first molars with zirconia crowns (NuSmile® ZR, NuSmile, www.nusmile.com) and use stainless steel crown forms for the second molars.
The patient's medical history was unremarkable, and he was most cooperative for routine treatment. On the first visit, after achieving right inferior alveolar block anesthesia, a rubber dam clamp was placed on the primary second molar, securing the rubber dam using the "slit dam" method (Figure 4).4 Even though the patient was 7 years old, his permanent first molars had not yet erupted.
Treatment Protocol
To select a suitable mandibular first molar crown, several crowns were held up against the bitewing radiograph on a fluorescent light box to match mesio-distal dimension. No mandibular molar crown matched ideally, but the maxillary left primary first molar crown designated D6L matched closely. It was thought that the sizing discrepancy resulted from the tooth being less rhomboidal than most mandibular first primary molars.
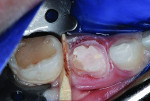
After placement of a wooden wedge between the molars, the occlusal surface was reduced by 1.5 mm to 2 mm using a water-cooled cylindrical diamond bur at high speed. The same bur was used to create a circumferential shoulder preparation just below the free gingival margin (Figure 5). Vertical cement retention slots were cut on all four axial surfaces. This unique preparation differed from that recommended by the manufacturer, which includes a 20% (0.5 mm to 1.25 mm) circumferential reduction on all four axial surfaces and a feather-edge margin extending 1 mm to 2 mm under the free gingival margin. The shoulder preparation and vertical slots were used simply because in this case that preparation adapted to the unadaptable crown form.
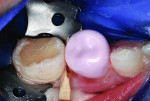
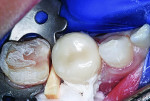
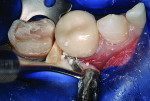
A UL6 pink NuSmile try-in crown (NuSmile) was placed on the preparation to verify fit (Figure 6). Mesio-distal dimension of the crown was satisfactory. Explorer probing confirmed that the buccal and lingual margins were confluent with the tooth surfaces. After initial preparation of the second molar for placement of a stainless steel crown, the UL6 zirconia crown was luted to the first molar using RelyX™ Luting Plus resin-modified glass-ionomer cement (3M ESPE, www.3mespe.com) (Figure 7). Excess cement was removed using a Hollenback #3 Carver (Figure 8). Stainless steel crown repair of the second molar then was completed in the usual manner.3
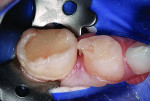
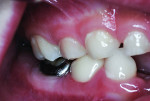
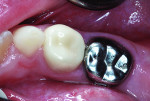
At a subsequent appointment, the left primary first molar was restored using a NuSmile maxillary right primary first molar zirconia crown (UR6), and the primary second molar was restored with a stainless steel crown. The four primary molars were photographed in occlusion 6 months after treatment (Figure 9 and Figure 10). Fourteen months after treatment, the crowns were again photographed (Figure 11 through Figure 13), and bitewing radiographs recorded (Figure 14).
Discussion
It is not common for contralateral/opposite-arch crown substitution to be required in clinical pediatric dentistry. Manufacturers of stainless steel crown forms and zirconia crowns offer a variety of primary first molar crown sizes, and most often, a suitable size can be selected. In this patient, as evidenced by the 14-month postoperative bitewing film, the mesio-distal dimension of the left first molar was perfectly duplicated by the UR6 zirconia crown. However, the UL6 zirconia crown used to restore the mandibular right primary first molar showed a slight mesial overhang on the postoperative bitewing film. While clinically insignificant, that is indicative of how difficult it can be to perfectly fit a preformed zirconia crown that, unlike a stainless steel crown, cannot be manipulated for ideal fit.
Slight marginal gingival inflammation was noted at the 6-month and 14-month re-evaluation appointments. It is difficult to determine whether that was due to less than ideal brushing and flossing or a reaction of the gingiva to the stainless steel or ceramic margins. Regardless, home care instructions were reinforced for the parent and child at each visit.
Resin-modified glass-ionomer luting cement (RelyX) was used to cement both the stainless steel crowns and zirconia crowns in this case. Since that time, other good cements have come become available for luting primary molar crowns, including Ceramir® Crown & Bridge (Doxa Dental Inc, ceramirus.com) and BioCem™ (NuSmile). Ceramir is a bioactive calcium aluminate-glass ionomer.5,6 BioCem, according its Material Safey Data Sheet, is a type of resin-modified glass-ionomer cement including a blend of diurethane and other methacrylates, modified polyacrylic acid, and amorphous silica.
Although preformed zirconia crowns for primary molars offer dentists new challenges, such as achieving ideal fit and controlling bleeding during cementation, they have rapidly found a place in clinical pediatric dentistry and undoubtedly will become a mainstay method of restoring severely carious, malformed, or otherwise damaged primary teeth.
References
1. Humphrey WP. Uses of chrome steel in children's dentistry. Dent Surv. 1950;26:945-949.
2. Full CA, Walker JD, Pinkham JR. Stainless steel crowns for deciduous molars. J Am Dent Assoc. 1974;89(2):360-364.
3. Croll TP. Preformed posterior stainless steel crowns: an update. Compendium Contin Educ Dent. 1999;20(2):89-106.
4. Croll TP. Alternative methods for use of the rubber dam. Quintessence Int. 1985;16(6):387-392.
5. Jefferies SR, Pameijer CH, Appleby DC, Boston D, Lööf J. A bioactive dental luting cement--its retentive properties and 3-year clinical findings. Compend Contin Educ Dent. 2013;34(spec iss 1):2-9.
6. Jefferies S. Bioactive and biomimetic restorative materials: a comprehensive review. Part II. J Esthet Restor Dent. 2014;26(1):27-39.
About the Author
Theodore P. Croll, DDS
Private Practice
Doylestown, Pennsylvania
Affiliate Professor
Department of Pediatric Dentistry UW School of Dentistry
Seattle, Washington
Adjunct Professor
Department of Pediatric Dentistry, UT Health Science Center
San Antonio, Texas
Kevin J. Donly, DDS, MS
Professor and Chair
Department of Developmental Dentistry, UT Health Science Center
San Antonio, Texas
For more information, contact:
NuSmile
800-346-5133
www.nusmile.com