Bulk-Fill Composites for Posterior Restorations
A time-saving, economical solution with esthetic benefits
For more than 2 decades, composite materials have been used as an esthetic alternative to metal restorations in the posterior region, which bears a great deal of masticatory load. As materials have improved, the use of posterior composites has become more frequent in recent years.1
Early clinical data on composite restorations in the posterior region were not encouraging, primarily due to the materials' insufficient mechanical properties. The low abrasion resistance of those composite materials led to loss of restoration contours. Marginal deterioration, fractures, and leakage following polymerization shrinkage were additional reasons for the limited lifespan of early posterior composite restorations.2-5 In recent years, most of these deficiencies have been greatly reduced as a result of material improvements in composite and adhesive systems.6 Nevertheless, the negative effects of polymerization shrinkage—such as poor marginal integrity, insufficient adherence to the cavity walls, or cusp deflections—still represent the greatest problems in composite-based materials.7
For the permanent direct restoration of primary carious lesions or the replacement of old, insufficient restorations in the posterior region, hybrid composites or hybrid composites modified with nanoparticles are today's materials of choice. Success is dependent upon the correct use of the matrix technique and adequate moisture control of the cavity.8 The incremental layering technique used with these materials involves placement of layers with a maximum thickness of 2 mm for each increment. Each increment is polymerized separately for 10 to 40 seconds, depending on the light intensity of the curing device and shade/translucency of the composite. In large posterior tooth cavities, this can be a lengthy procedure that takes a considerable amount of the clinician's time.
The use of bulk-fill composites has become an alternative to the complex, time-consuming incremental technique. It allows the dental professional to process composite restorations in less time, providing a more economical option.9,10 while maintaining desirable esthetics.
The Economics of Posterior Composites
Despite the fact that amalgam has been used successfully for decades, it is generally no longer acceptable to many patients both for esthetic reasons and because of concerns about potential side effects. In fact, so many patients request metal-free restorations in the treatment of posterior tooth defects that a significant number of dentists no longer offer amalgam. Gold inlay restorations are also increasingly being refused due to patients' desire for tooth-colored restorations.11,12
Composite restorations have proven highly successful in the treatment of posterior teeth.13 For best clinical outcomes when placing increments, the basic rules for the adhesive technique must be followed, including observance of the curing depth of each individual layer of composite, sufficient light polymerization, and careful finishing and polishing.14 In general, adhesive restorations show a great deal of technique sensitivity. The same material handled by different operators often shows highly significant variations in the level of success achieved.15
Observing the rules of adhesive technique correctly can be extremely time-consuming for the dentist. The clinician's time must be reflected in the cost of the dental visit; however, many patients are simply financially unable to take on higher costs.
Dentists regularly find themselves in one or more of the following clinical situations with patients requiring permanent posterior restoration for whom cost is a major concern:
The patient refuses amalgam.
Currently available glass ionomer cements (and derivatives) and other cement restoratives are not suitable due to an increased risk of fracture or wear in the areas affected by masticatory loads.16-18
The additional costs for incremental direct composite restorations exceeds the patient's budget.
Crowning is neither indicated nor in the patient's budget.
For these cases, the chosen treatment must show both reasonable clinical performance in the highly stressed posterior teeth and be economically sensible for the dentist to deliver. Accordingly, the desire for restorative materials that are faster and easier to process and can therefore be offered at a lower price is totally understandable.10,19
Conservative dentistry would benefit from a less technique-sensitive, esthetic alternative to amalgam, whose clinical longevity it would ideally combine with the structurally stabilizing properties of the adhesive technique. The optical properties of such a material matter somewhat less to patients for posterior teeth, as long as the result is not metallic or extremely opaque. In the author's view, it would also be a major advantage if a tooth-colored posterior material need not be laboriously applied using the polychromatic multi-layer technique, unlike highly esthetic composite restorations.
The Bulk-Fill Option
Understanding the needs of practitioners, a number of composite manufacturers have focused on material development to simplify composite-based restoration techniques in the posterior region. In these new fast-track systems, simplified bonding agents (usually single-step, self-conditioning adhesive systems) are used in combination with low-shrinkage, mechanically stable composite materials that can be applied directly into the cavities in larger increments.19-21
These bulk-fill composites should, with the best possible quality of marginal adaptation, be easy to handle22 and less technique sensitive with the additional benefit of saving time in placement.23 As many of these bulk-fill composites are only supplied in a single shade, selection of the matching shade is also no longer required. Despite this, the use of these materials results in adequately esthetically pleasing results, especially in comparison with amalgam and glass ionomer cements. For the purpose of a comprehensive "fast-track" technique, these composites are normally used in combination with self-conditioning bonding agents, without the use of separate enamel-dentin etching.
The material properties of these composites are comparable to conventional light-curing composites.24 Data from clinical trials show good intraoral performance.25-30
Case Presentation
The following clinical case is a step-by-step representation of the replacement of an old, insufficient amalgam restoration in a first upper molar using a bulk-fill technique.
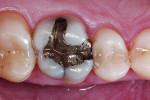
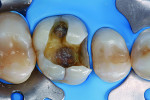
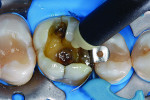
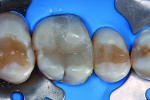
A male patient complained of thermic irritation in his first upper molar, which contained an old amalgam restoration (Figure 1). During the clinical inspection, the tooth reacted sensitively in the cold test but showed no negative reaction to the percussion test. In consultation with the patient, it was decided to replace the amalgam restoration. After an explanation of the possible treatment alternatives, the patient decided on a direct bulk-fill composite restoration.
For this case, the author chose the high-viscosity, sculptable hybrid composite x-tra fil (filler content: 86% by weight, 70.1% by volume) (VOCO, www.voco.com), which exhibits reduced shrinkage (1.7%) on a traditional methacrylate basis. It is available in a transparent universal shade, which allows the practitioner to place a maximum of 4-mm composite increments in a bulk-fill technique for Class I and II defects. Unlike low-viscosity bulk-fill composites, which must be covered by a 2-mm occlusal capping layer using another methacrylate-based hybrid composite suitable for posterior teeth,31 x-tra fil makes it possible to completely restore the whole cavity with one material. With a light-curing device with a light intensity between 500 to 800 mW/cm², the polymerization time is 20 seconds; this is reduced to 10 seconds, if the light intensity is at least 800 mW/cm².
Treatment Protocol
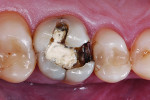
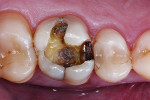
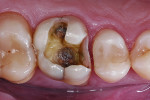
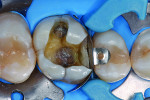
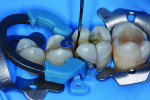
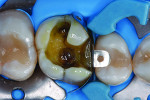
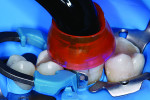
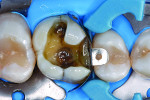
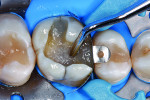
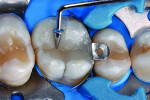
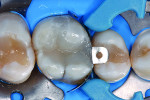
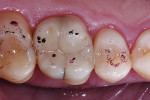
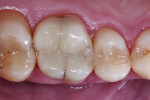
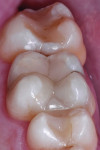
Treatment began with thoroughly cleaning the affected tooth of external deposits using a fluoride-free prophylaxis paste and a rubber cup. After careful removal of the insufficient amalgam restoration while conserving the remaining hard tissue (Figure 2 and Figure 3), the tooth was excavated, and the cavity was completely prepared and finished with a fine-grit diamond bur (Figure 4). Figure 5 shows the preparation after placement of the rubber dam. The rubber dam ensures that the working area remains clean of contamination, which would result in markedly poorer adhesion of the composite to the dental hard tissues and endanger the long-term success of the composite restoration. Additionally, the rubber dam protects the patient from irritating substances such as the adhesive system, and enables the dental team to avoid the need to change cotton rolls or allow for patient rinsing.
A sectional metal matrix system was used to delimit the triple-surface cavity (Figure 6). To optimize the contours, the matrix was carefully molded with a hand instrument. The formation of physiologically contoured proximal surfaces with tight contacts to neighboring teeth still represents a challenge when using direct composite restorations. In contrast to amalgam, composites show a certain viscoelastic recovery from distortion, which is often seen as undesirable by the user and complicates the adaptation of matrices to the neighboring tooth by packing pressure.32,33
The deepest area of the cavity was measured using a scaled periodontal probe, as x-tra fil can be applied in the bulk technique in a layer thickness of up to 4 mm (Figure 7). The universal adhesive Futurabond M+ (VOCO) was selected for bonding. This adhesive can be used with or without prior application of phosphoric acid. In this clinical case, the adhesive was applied using the self-etch technique. Ample amounts of adhesive were applied and distributed in the area of the cavity using a microbrush (Figure 8). It must be ensured that all cavity areas are sufficiently covered by the adhesive. After at least 20 seconds of carefully scrubbing the adhesive into the hard dental tissues, the solvent was carefully evaporated with oil-free compressed air from the bonding agent (Figure 9), which was subsequently light-cured for 10 seconds (Figure 10).
The result was a shiny cavity surface that was evenly covered with adhesive (Figure 11). This should be carefully checked, as any areas of cavity that appear dull are an indication that an insufficient amount of adhesive has been applied to those sites. In the worst case, this could result in reduced bonding of the restoration in these areas and, at the same time, in reduced dentin sealing, which may lead to postoperative sensitivity. If such areas are found in the visual inspection, additional bonding agent is selectively applied.
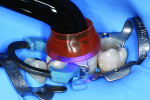
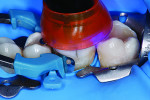
The composite x-tra fil in translucent universal shade was applied in the bulk technique in a layer thickness of 4 mm, starting at the deepest area of the defect, and was adapted carefully to the cavity floor and walls (Figure 12). The first increment of the translucent composite was polymerized with a curing light (intensity > 800 mW/cm²) for 10 seconds (Figure 13). With a second layer of x-tra fil, the cavity was completely filled up to the occlusal surface and the anatomy was shaped (Figure 14 and Figure 15). After 10 seconds of polymerization (light intensity > 800 mW/cm²) (Figure 16), the matrix system was removed and the restoration was checked for imperfections (Figure 17).
Once the rubber dam was removed, the fissure relief and fossae were finished with a pear-shaped finishing diamond bur. A point-shaped fine-grit diamond was then used to finish the convexity of the cusps and triangular ridges. After the elimination of occlusal interferences and adjustment of the static and dynamic occlusion (Figure 18), the accessible proximal areas were contoured and prepolished with abrasive disks. The use of diamond-impregnated composite polishers (Dimanto, VOCO) achieved a satin matte, lustrous finish on the surface of the restoration. Subsequent high-gloss polishing was completed using the same Dimanto polishers with reduced pressure to optimize the luster of the restoration material.
Figures 19 and 20 show the finished direct restoration with the composite x-tra fil in a maxillary first molar, reconstructing the tooth with an anatomically functional occlusal surface and a physiologically formed proximal contact area. Finally, a foam pellet was used to apply the fluoride varnish Bifluorid 12 (VOCO) to the affected tooth.
Conclusion
Direct composite restorative materials are scientifically proven, high-quality permanent restorations for the load-bearing posterior region; their reliability has been documented in literature and their use is likely to increase in the future. The results of a comprehensive review have shown that the annual failure rates are not statistically different from those of amalgam restorations.13 Minimally invasive treatment protocols, in combination with the ability to detect carious lesions ever earlier, also have a positive effect on the longevity of such restorations. However, to ensure a high-quality direct composite restoration with good marginal adaptation, a careful matrix technique (in cases with proximal involvement), an effective adhesive system, the correct processing of the restorative material, and sufficient polymerization of the composite continue to be basic prerequisites.
To maintain practice profitability despite increasing financial pressure in the health care system and, in many cases, the limited financial means of patients who require time-consuming high-end restorations, practitioners benefit from a simpler, faster-to-complete, and therefore more economical basic treatment.10 Composite-based basic treatment cannot be offered entirely without some additional cost to the patient; however, the time advantage associated with the bulk-fill technique can reduce these costs.
References
1. Kelsey WP, Latta MA, Shaddy RS, Stanislav CM. Physical properties of three packable resin-composite restorative materials. Operative Dentistry. 2000;25(4):331-335.
2. Lambrechts P, Braem M, Vanherle G. Klinische Erfahrungen mit Composites und Dentin-Adhäsiven im Seitenzahnbereich I: Klinische Beurteilung von Composites. Phillip J. 1988;1:12-28.
3. Leinfelder KF, Sluder TB, Santos JFF, Wall JT. Five-year clinical evaluation of anterior and posterior restorations of composite resin. Oper Dent. 1980;5:57-65.
4. Lutz F, Phillips RW, Roulet JF, Setcos JC. In vivo and in vitro wear of potential posterior composites. J Dent Res. 1984;63(6):914-920.
5. Roulet JF. The problems associated with substituting composite resins for amalgam: a status report on posterior composites. J Dent. 1988;16(3):101-113.
6. Manhart J. Charakterisierung direkter zahnärztlicher Füllungsmaterialien für den Seitenzahnbereich. Alternativen zum Amalgam? Quintessenz. 2006;57:465-481.
7. Manhart J, Kunzelmann KH, Chen HY, Hickel R. Mechanical properties and wear behavior of light-cured packable composite resins. Dent Mater. 2000;16(1):33-40.
8. Manhart J. Praxistaugliche Schichttechnik für die Anwendung von plastischen Kompositrestaurationen im Seitenzahnbereich. Quintessenz. 2008;59:1337-1342.
9. Manhart J. Muss es immer Kaviar sein? – Die Frage nach dem Aufwand für Komposite im Seitenzahnbereich. ZMK. 2011;27:10-15.
10. Margeas R. New bulk-fill material simplifies restorations to one step. Inside Dentistry. 2014;10(10):86-90.
11. Manhart J. Seitenzahnversorgung - Adhäsiv befestigte indirekte Kompositinlays und -onlays im Seitenzahnbereich. Teamwork Interdiszipl J Restaurat Zahnheilk. 2006;9:394-402.
12. Noack M. Stirbt der Goldstandard aus? Quintessenz. 2008;59:1017.
13. Manhart J, Chen H, Hamm G, Hickel R. Buonocore Memorial Lecture. Review of the clinical survival of direct and indirect restorations in posterior teeth of the permanent dentition. Oper Dent. 2004;29(5):481-508.
14. Frankenberger R. Die adhäsive Seitenzahnversorgung. Komposit oder Keramik? ZWR. 2009;118(4):187-190.
15. Frankenberger R, Reinelt C, Petschelt A, Kramer N. Operator vs. material influence on clinical outcome of bonded ceramic inlays. Dent Mater. 2009;25(8):960-968.
16. Frankenberger R, Garcia-Godoy F, Kramer N. Clinical performance of viscous glass ionomer cement in posterior cavities over two years. Int J Dent. 2009; doi:10.1155/2009/781462.
17. Hickel R, Ernst CP, Haller B, et al. Direkte Kompositrestaurationen im Seitenzahnbereich - Indikation und Lebensdauer. Gemeinsame Stellungnahme der Deutschen Gesellschaft für Zahnerhaltung (DGZ) und der Deutschen Gesellschaft für Zahn-, Mund- und Kieferheilkunde (DGZMK) aus dem Jahr 2005. Deutsche Zahnärztliche Zeitschrift. 2005;60:543-545.
18. Lohbauer U. Dental glass ionomer cements as permanent filling materials? - Properties, limitations and future trends. Materials. 2010;3(1):76-96.
19. Haller B. Moderne Füllungstechniken und ihre Langzeitbewährung. ZNN Zahnärztliche Nachrichten Niedersachsen. 2003;4:10-11.
20. Hellwig E, Klimek J, Attin T. Einführung in die Zahnerhaltung. Köln: Deutscher Ärzte Verlag; 2009.
21. Manhart J, Hickel R. "Bulk Fill"-Komposite. Neuartige Einsatztechnik von Kompositen im Seitenzahnbereich. Swiss Dental Journal. 2014;124:19-28.
22. Kluschke A. SDR - die Zukunft in der Adhäsivtechnik? ZP Zahnarzt & Praxis. 2010;13(2):86-95.
23. Haberkorn KE. Randschluss von Fast-Track-Kompositfüllungen im Vergleich zu Amalgam- und Glasionomerzementfüllungen [dissertation]. Ulm, Germany: Universität Ulm; 2006.
24. Fleming GJ, Awan M, Cooper PR, Sloan AJ. The potential of a resin-composite to be cured to a 4mm depth. Dental Materials. 2008;24:522-529.
25. Arhun N, Celik C, Yamanel K. Clinical evaluation of resin-based composites in posterior restorations: two-year results. Oper Dent. 2010;35:397-404.
26. Celik C, Arhun N, Yamanel K. Clinical evaluation of resin-based composites in posterior restorations: 12-month results. Eur J Dent. 2010;4:57-65.
27. Manhart J, Chen HY, Hickel R. Three-year results of a randomized controlled clinical trial of the posterior composite QuiXfil in class I and II cavities. Clin Oral Investig. 2009;13(3):301-307.
28. Manhart J, Chen HY, Hickel R. Clinical evaluation of the posterior composite Quixfil in class I and II cavities: 4-year follow-up of a randomized controlled trial. J Adhes Dent. 2010;12(3):237-243.
29. Manhart J, Neuerer P, Hickel R. 10-Jahresergebnisse von QuiXfil und Tetric Ceram in einer kontrollierten klinischen Studie. Publication in preparation.
30. Peschke A. Ein neues Bulk-Fill-Material in der klinischen Anwendung. DZW Die Zahnarzt Woche. 2013;45(13):10-11.
31. Ferracane J, Alex G, Margeas R. Question: Are bulk-fill composites a good idea? Inside Dentistry. 2014;10(10):42-44.
32. Kunzelmann KH, Hickel R. Klinische Aspekte der Adhäsivtechnik mit plastischen Werkstoffen. In: Die Adhäsivtechnologie. Ein Leitfaden für Theorie und Praxis. Seefeld, Germany: 3M ESPE; 2001:46-67.
33. Manhart J. Eine Alternative zu Amalgam? Hochvisköse stopfbare Komposite: Überblick, Eigenschaften und Verarbeitungshinweise. KONS-Journal. 2001;3:21-26.
About the Author
Jürgen Manhart, DDS, MS, PhD
Professor, Department of Restorative Dentistry
Dental School of the Ludwig-Maximilians-Universität
Munich, Germany