Overcoming Anterior Esthetic Challenges
Treating congenitally missing lateral incisors in less-than-ideal circumstances
The maxillary lateral incisor is the second most often congenitally missing adult tooth.1,2 Several treatment options can be considered depending on the patient’s age, the amount of space, the type of occlusion, and the condition of the adjacent teeth.3 Using a multi-interdisciplinary approach with consultation is paramount when replacing these teeth to achieve the most esthetic and functional result.
One of the challenges clinicians sometimes encounter when a new patient presents to the dental office is treatment that has already progressed through several phases without consultation with the restorative dentist. Depending on the severity of the problem and the location, these difficulties can limit the final restorative treatment, resulting in a less than optimal outcome for the patient. Whether it stems from a lack of treatment planning or other errors in handling the case, less than ideal previous treatment is a problem that must then be faced by the restorative dentist and the patient.
This article details the final phase of a clinical case of a patient with congenitally missing laterals who presented after being treated by a number of specialists without any previous consultation. Treatment options were further restricted by the dental clinic setting. Textbook-perfect treatment scenarios are rare in clinical practice for many reasons. Sometimes one encounters unexpected difficulties even with the most careful treatment planning and execution. In other cases, patient finances sometimes mean a more expensive but ideal treatment plan is not an option, so clinician and patient must agree upon a clinically acceptable and esthetic next-best alternative. All patients, regardless of prior circumstances, deserve the best possible outcome.
Treatment Options for Congenitally Missing Lateral Incisors
Among available treatment options for dealing with congenitally missing lateral incisors are restorative dentistry, implant replacement therapy, and orthodontics. Usually, a combination of some or all of these disciplines can be used to achieve the desired outcome.4 A solely orthodontic approach can, at times, be the most conservative choice, but it requires an appropriate malocclusion5 and, according to a formula by Chu,6 that the canines be of a specific size, shape, and color. This formula specifies that a canine is approximately 1 mm too wide to be substituted for a lateral incisor. In addition, the convexity of the canine is greater than that of a lateral and is visible in two planes mesiodistally instead of one. In addition, the lingual surface of the canine usually needs to be reshaped to achieve a proper overjet and overbite, and modifications are needed to flatten the canine cusp tip. All of this recontouring frequently requires significant reduction of enamel, leading to dental hypersensitivity. An additional problem with re-positioning canines into the lateral space is that the canine tooth tends to be two shades darker than central incisors.6 These challenges may be met with adjunctive restorative treatments.
Achieving esthetic outcomes in the anterior region with implant restorations is currently one of the most challenging areas of dentistry. It requires thoughtful treatment planning and may depend on a variety of factors, including patient expectations; bone quality; availability of appropriate restorative components; tissue health; occlusal load; operator skill, the position and size of adjacent teeth; occlusion; and inter-arch spacing.7 Unfavorably placed implants can be addressed in several ways, including removal and replacement, surgical repositioning, or the use of customized angle-corrected abutments; alternately, they can also be buried subgingivally and left unrestored.7
Case Presentation
A 61-year-old healthy woman presented to a university-affiliated dental clinic complaining chiefly of a desire to replace her missing teeth. Orthodontic treatment had been completed, and 4.0-mm platform implants had been previously placed in the area of No. 6 and No. 11, but were not yet uncovered. A clinical examination was completed, as were diagnostic study models and photographs.
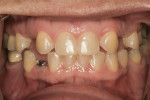
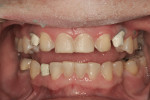
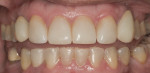
Before the patient began orthodontic treatment, she had presented with bilateral retained deciduous canine teeth, congenitally missing permanent maxillary lateral incisors, and permanent canine teeth anteriorly positioned toward the central incisors (Figure 1).
In developing a treatment plan, several concerns were noted. The mesial-distal widths in the maxillary right and left canine areas were 8.5 and 10 mm, respectively. The average mesial-distal width of a maxillary permanent canine is between 5.5 and 7.5 mm.8 The position of the canines in this case left spaces beyond the normal width of a maxillary canine. The implants placed by the periodontal specialist were placed in a more labial position, which increased the interproximal space between the adjacent teeth. Because a mock-up model was not created prior to the surgical intervention, ideal implant placement had not been considered for the restorative phase of treatment. In the anterior region, a slight deviation from an ideal position can have an enormous effect on the esthetic result of a case. Implant positioning is critical.19
The patient had expressed her dislike of the shade, shape, and size of her front four teeth and wanted to restore those teeth along with the implants and eliminate the interproximal spaces. Therefore, the treatment goals were to alter the shape of the canines to appear as lateral incisors and close the canine spaces without making the implant restorations appear too large. A diagnostic wax mock-up was created to determine the spatial relationships of the final restorations and to consider how to prepare the involved teeth (Figure 2).
Treatment Planning
A review of the literature for cases of canine substitution suggests that an esthetic approach to transforming yellow or dark canines to an optimal lateral incisor shade is to use porcelain veneers.3,5 Zachrisson and colleagues5 suggest that clinical evaluation of the central incisors is indicated because frequently they are also smaller in size in patients with missing laterals. Using porcelain veneers to widen and lengthen the incisors may allow patients a more optimal display of dentition during speech and smiling. In the laboratory phase of treatment, the contours of the restorations can be manipulated to create optical illusions to disguise space discrepancies. Additional consideration should be given the soft tissue changes that would be visible through different types of implant abutment materials. In the anterior region, there is a choice between titanium and zirconia abutments. A milled zirconia custom abutment demonstrates fewer soft-tissue color changes than titanium abutments in patients presenting with a thin gingival biotype.10 A recent systematic review of ceramic implant abutments demonstrated that their survival rates resembled those of metal abutments, even in the posterior.11 Although these studies seem promising, they included a limited number of ceramic abutments with a limited 5-year follow-up at this time. The case presented here was treated in an academic environment, where further evidence-based research supporting the longevity of ceramic abutments is required to deem their use acceptable.
Whatever abutment is chosen, the use of all-ceramic crowns for anterior restorations requiring optimal esthetics is a widely accepted application among dentists. One of the esthetic benefits of all-ceramic crowns is their semi-translucent properties, which enable light transmission. This influences the shade of the final restoration. Studies have shown that dark abutment teeth, cement shade, metal posts, metal abutments, and ceramic thickness all have an influence on the final esthetic outcome.12-15 Because in this case a titanium abutment was the only available option, a technique was used to mask the metal color and ensure that the all-ceramic, implant-supported crowns were esthetically acceptable to the patient.
Considerations for Masking Abutments
The color of the composite luting cement and the opacity of the restoration are key factors affecting the final treatment outcome. Composite luting cements are used for several reasons: to improve mechanical retention by making the crown and the tooth one unit; to mask the underlying color of the tooth; and to modify the final restoration color. Clinicians must consider the type of composite cement used, because studies have shown the properties of different types of opaque cements can vary dramatically from one manufacturer to the next.13 It may be necessary to mix different cement shades to achieve the desired optical properties and esthetic outcome.
In addition, various all-ceramic crowns have demonstrated different esthetic outcomes based on their levels of translucency.13 The attribute that makes the most perceptible difference when masking the underlying abutment color is the thickness of the ceramic layer. A thickness of 2.0 mm was found to be ideal; however, a luting cement can make a difference as long as the ceramic’s thickness was not greater than 1.0 mm.14
It is also important to evaluate the patient’s tissue. A study examining soft tissue height and thickness found that at a sulcus depth of 2.2 mm, the most apical tissue has a thickness of 3 mm. This study found that when the buccal mucosa is 2.1 mm thick, no perceivable difference between a zirconia and titanium implant abutment can be observed.15
Tooth Preparations
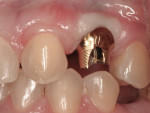
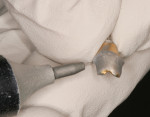
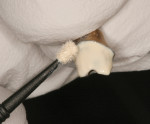
To begin treatment, Stage II implant uncovering was performed and healing abutments were placed. The patient returned 4 weeks later for implant-level impressions and occlusal records. At the preparation appointment, the custom abutments were tried in to evaluate the position and occlusal clearance (Figure 3). The abutments were removed and placed on the working model, where the labial and incisal aspect were reduced (Figure 4). Using a micro-abrasion unit, silicatization of the metal abutments was performed using the CoJet™ system (3M ESPE, www.3mespe.com) (Figure 5). This technique uses specially developed silica sand (30 µm) that is tribochemically embedded into the surface of the metal, creating a ceramic coating. According to the manufacturer, tribochemistry is the creation of a chemical bond by the use of mechanical energy. The silicatization of a metal surface improves the bond strength to composite resin.16 After the coating was completed, a ceramic primer containing the phosphate monomer 10-MDP (10-methacryloyloxydecyl dihydrogen phosphate) was applied to the surface and then air dried to evaporate the solvent. A filled bonding adhesive was applied to the treated metal surface and light polymerized. Several thin coats of an opaque resin (Kolor + Plus®, Kerr Corporation, www.kerrdental.com) that matched the shade of the prepped teeth were applied and light polymerized (Figure 6). This step was repeated until the metal color was masked. The abutments were then placed in the mouth and torqued to 35 Ncm. The four anterior teeth were then prepared for porcelain laminate veneers. The labial surface of the canine teeth (in the lateral incisor position) was reduced more than the central incisor to flatten the mid-facial bulge characteristic of the canine tooth (Figure 7). Impressions, a bite registration, and a facebow transfer were then made. Using a vacuum stent from the mock-up, provisional restorations were then placed.
Laboratory Phase
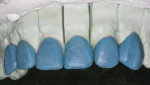
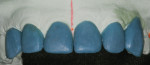
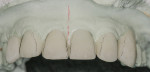
In the laboratory, a multiple-die working model and a solid working model were fabricated. Using the wax injection technique,17 the restorations were created in wax. At this point, the proximal contours of teeth No. 7 and No. 10 were altered to create the optical illusion of a narrower tooth, reflecting the shape of a lateral incisor on the body of a canine (Figure 8 and Figure 9). The wax restorations were then invested for ceramic pressing using lithium disilicate ingots (IPS e.max®, Ivoclar Vivadent, www.ivoclarvivadent.com).
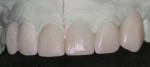
After completion of the pressing cycle, the restorations were divested and separated, and the incisal one third of each restoration was cut back and then layered with a number of enamel porcelains. The mesial contour ridge of the lateral incisors was highlighted to enhance the optical illusion transforming a canine tooth into a lateral incisor. The contours of the restorations were seen more readily by using pencil lines (Figure 10). The cervical width of the canine teeth was still greater than a lateral incisor. To offset the greater width of the prepared canine, the distal-facial contour ridge was brought more towards the mesial to reduce the width of the reflective surface of the restoration. The reduction in the amount of light reflection helped create the illusion of a lateral incisor. Normally, the incisal embrasure between the distal aspect of the lateral incisor and the mesial aspect of the canine is very open and broad, creating an obtuse angle. The incisal embrasure between the lateral incisor and central incisor is the second smallest angle in the anterior region, which creates an acute angle where the angle between the two central incisors is the smallest. It was necessary to add incisal porcelain to the lingual aspect to close the incisal embrasure (Figure 11).18
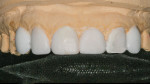
At the insertion appointment, the provisional restorations were removed and the prepared teeth were cleaned. The final restorations were tried in and approved by the patient (Figure 12). The intaglio surfaces were etched using 5% hydrofluoric acid for 20 seconds. The restorations were then rinsed, ultrasonically cleaned for 5 minutes, and then air dried. A 10-MDP monomer–containing ceramic primer was applied to the bonding surfaces and air dried to evaporate the solvent. A light-cure-only bonding adhesive was applied to the bonding surface and then air thinned. A highly filled (80%) flowable composite was then applied to each of the restorations and placed in a CALSET™ Warmer (AdDent, Inc., www.addent.com) and then covered.19
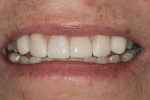
The prepared teeth were etched using 35% phosphoric acid, rinsed with water, and then dried with an air-water syringe. The same adhesive bonding agent was then applied to the teeth and air thinned. The overhead unit light was turned off. The preloaded warmed veneers were placed, starting with the central incisors, followed by the lateral incisors, and then the crowns on the canines. Excess composite resin was removed. Both central incisor veneers were secured in place, using simultaneous light pressure in an incisal direction with the index fingers, and labial pressure with the thumbs. An LED curing light with a 2-mm light guide was placed at the center of each veneer and activated for 1 second on the facial side. The same procedure of securing and tacking down the restoration was repeated for the lateral incisors, followed by the canines. The light guide tip was then changed to a larger diameter. Holding the light tip 1 inch from the labial surface, further light activation was completed, using a waving motion for an additional 4 seconds on the labial side and then on the lingual side. The remaining excess flowable composite was then removed with a 12-b surgical blade mounted in a round handle instrument. Dental floss was passed through each interproximal contact. A clear water-soluble gel was used to cover all margins to prevent the formation of an oxygen-inhibited layer during the final light-curing step. Using two curing lights—one placed on the facial and the other placed on the lingual—the veneers were light-cured for 60 seconds, divided into 20-second increments, to prevent overheating of the tooth. The margins were checked and finished using ultra-fine diamond burs. Any remaining resin on the veneer surface was removed with the 12-b surgical blade; the restorations were then polished with a soft bristle brush and Zircon-Brite (Dental Ventures, https://dentalventures.com) polishing paste (Figure 13).
Conclusion
Treatment planning is essential to produce predictable restorative results. The restorative clinician should always be involved in the treatment decisions from the very beginning of the patient’s care. Whether the case is simple or complex, the restorative phase is usually the last step completed and is critical in meeting the patient’s expectations. The ultimate treatment goal should be determined first; then the necessary steps to achieve that goal should be formulated through collaboration with the various specialists involved throughout treatment.
When this ideal is not met, steps can nevertheless be taken to provide an excellent and satisfying result for the patient. Communication between the restorative dentist and the laboratory, for example, can lead to solutions that meet patient expectations.
References
1. Graber LW. Congenital absence of teeth: a review with emphasis on inheritance patterns. J Am Dent Assoc. 1978;96(2):266-275.
2. Dermaut LR, Goeffers KR, De Smit AA. Prevalence of tooth agenesis correlated with jaw relationship and dental crowding. Am J Orthod Dentofacial Orthop. 1986;90(3):204-210.
3. Kokich VO Jr, Kinzer GA. Managing congenitally missing lateral incisors. Part I: Canine substitution. J Esthet Restor Dent. 2005;17(1):5-10.
4. Krassnig M, Fickl S. Congenitally missing lateral incisors--a comparison between restorative, implant, and orthodontic approaches. Dent Clin North Am. 2011;55(2):283-299, viii.
5. Zachrisson BU, Rosa M, Toreskog S. Congenitally missing maxillary lateral incisors: canine substitution. Point. Am J Orthod Dentofacial Orthop. 2011;139(4):434-438.
6. Chu SJ. Range and mean distribution frequency of individual tooth width of the maxillary anterior dentition. Pract Proced Aesthet Dent. 2007;19(4):209-215.
7. Rumfola JL, Andreana S, Colucci L, Tsay Y. Restoring unfavorably positioned implants in anterior maxilla: case report. N Y State Dent J. 2013;79(5):40-44.
8. Shah AA, Elcock C, Brook AH. Posterior tooth morphology and lower incisor crowding. Dental Anthropology. 2005;18(2):37-42.
9. Margeas RC. Clinical case report: treatment of anterior teeth with an implant, veneers, and full-coverage restorations. Compend Contin Educ Dent. 2009;30(3):156-160.
10. Sailer I, Zembic A, Jung RE, et al. Single-tooth implant reconstructions: esthetic factors influencing the decision between titanium and zirconia abutments in anterior regions. Eur J Esthet Dent. 2007;2(3):296-310.
11. Dede DÖ, Armaganci A, Ceylan G, et al. Influence of abutment material and luting cements color on the final color of all ceramics. Acta Odontol Scand. 2013;71(6):1570-1578.
12. Chang J, Da Silva JD, Sakai M, et al. The optical effect of composite luting cement on all ceramic crowns. J Dent. 2009;37(12):937-943.
13. van Brakel R, Noordmans HJ, Frenken J, et al. The effect of zirconia and titanium implant abutments on light reflection of the supporting soft tissues. Clin Oral Implants Res. 2011;22(10):1172-1178.
14. Sailer I, Philipp A, Zembic A, et al. A systematic review of the performance of ceramic and metal implant abutments supporting fixed implant reconstructions. Clin Oral Implants Res. 2009;20 (suppl 4):4-31.
15. Martinez-Rus F, Ferreiroa A, Ozcan M, Pradies G. Marginal discrepancy of monolithic and veneered all-ceramic crowns on titanium and zirconia implant abutments before and after adhesive cementation: a scanning electron microscopy analysis. Int J Oral Maxillofac Implants. 2013;28(2):480-487.
16. Della Bona A, Borba M, Benetti P, Cecchetti D. Effect of surface treatments on the bond strength of a zirconia-reinforced ceramic to composite resin. Braz Oral Res. 2007;21(1):10-15.
17. Helvey GA. Press-to-zirconia: a case study utilizing cad/cam technology and the wax injection method. Pract Proced Aesthet Dent. 2006;18(9):547-554.
18. Rosa M, Zachrisson BU. Integrating esthetic dentistry and space closure in patients with missing maxillary lateral incisors. J Clin Orthod. 2001;35(4):221-234.
19. Helvey GA. Creating super dentin: using flowable composites as luting agents to help prevent secondary caries. Compend Contin Educ Dent. 2013;34(4):288-300.
About the Authors
Cheyanne E. Warren, DDS, MS
FQHC
Private Practice
Plainfield, Vermont
Gregg A. Helvey, DDS, MAGD
Adjunct Associate Professor
Virginia Commonwealth University School of Dentistry
Richmond, Virginia
Private Practice
Middleburg, Virginia