Posterior Class VI Adhesive Tooth Repair
Glass ionomers and resin-based composites for durable and reliable cusp tip restoration
Dr. Greene Vardiman Black (1836-1915), the “father of modern dentistry,” classified dental caries lesions according to their anatomical locations (Table 1). His classification system became the diagnostic mainstay of infectious dental disease and has been used in the profession ever since.1
Another classification was added years later. Class VI cavities were described in W.J. Simon’s 1956 operative dentistry textbook: “To Black’s cavity classifications, a sixth category is occasionally added known as the Class VI cavities in the incisal edge or occlusal cusps due to either abrasion, erosion, or attrition.”2
The Class VI lesion is sometimes referred to as “Simon’s modification.” Simon’s textbook is the only “original” citation the authors were able to find for cusp tip/incisal edge lesions requiring tooth restoration. Although it is possible that Simon used an earlier source for this definition of Class VI cavities, extensive searches in the American Dental Association library and the library of the University of Pennsylvania School of Dental Medicine were unable to locate any earlier designations of such lesions.
Class VI enamel defects of incisors usually affect older, worn teeth in which the enamel layer has been lost, exposing dentin with a lower mineral content that is susceptible to wear, acidic content of saliva and foodstuffs, and caries. More mysterious is the etiology of Class VI cusp tip caries lesions. Because those anatomical sites do not have obvious patencies, such as the pits and fissures that commonly develop Class I caries lesions, or biofilm and dental plaque stasis associated with Class V smooth surface lesions, one wonders how cusp tip caries occurs.
One possibility is that these areas have microscopic porosities that develop naturally or form due to concentrated long-term stresses of occlusal and masticatory impact in the interstitial areas of enamel rod bundles in prominent cuspal and ridge regions. Such minute defects initially are not visible to the human eye, but are accessible to bacterial colonization. Once a caries lesion commences, the infection grows as surrounding enamel rods are demineralized, and the lesion expands in the usual caries process.
Repair of posterior teeth with Class VI defects resulting from caries, erosion, or wear has been accomplished with gold foil, silver amalgam, and resin-based composite.3-5 This clinical report describes three patients requiring Class VI tooth repair. One 18-month-old child had a maxillary primary molar restored using a “nano-ionomer” resin-modified glass-ionomer restorative material. An 11-year-old boy had a mandibular permanent molar restored using resin-based composite with a resin-modified glass-ionomer liner. In the third patient, a teenaged girl, a maxillary premolar with a Class VI caries lesion was restored using a combination of resin-based composite and resin-modified glass-ionomer. In addition, the adjacent occlusal groove was “super-sealed”” using the bonded resin-based composite.6
Case Presentations
Case 1
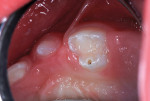
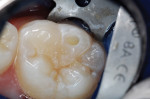
An 18-month-old girl was brought to the office for initial dental examination. The child’s mother’s chief complaint was “a black spot on her new baby molar.” Head and neck evaluation was unremarkable except for a Class VI caries lesion on the lingual cusp of the maxillary left primary first molar (Figure 1). Using a “hugging blanket”-type wrap7 for safety and comfort, placement of earphones that played pleasant children’s music, nitrous oxide/oxygen inhalation relaxation at a 20%/80% flow, and a Molt-type mouth prop, the tooth was restored as follows.
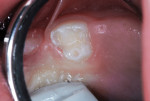
Using a 2 in x 2 in cotton gauze to protect the oropharynx, and no local anesthetic injections, carious tooth structure was removed using a slow speed #2 round bur. Undercuts were placed in the preparation using a #35 inverted cone bur at slow speed, assuring complete removal of the carious enamel and dentin, and providing for mechanical retention of the filling material (Figure 2).
A nano-ionomer resin-modified glass-ionomer restorative material (Ketac™ Nano, 3M ESPE, www.3mespe.com) was blended by spatula and placed into an orange AccuDose® Low Viscosity (small diameter lumen) syringe tip (Centrix, www.centrixdental.com). The filling material was then slowly injected into the preparation from the bottom up to avoid air entrapment. The visible light beam (1,100 mW/cm2) was applied for 20 seconds. A large round diamond rotary instrument was used at slow speed to trim the excess material and blunt the cusp tip. An additional 10-second light cure followed to assure through and through polymerization of the resin component of the cement.
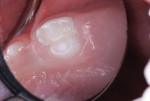
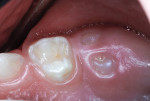
The nano-ionomer restoration was photographed immediately after treatment (Figure 3) and 8 months postoperatively (Figure 4).
Case 2
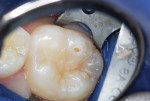
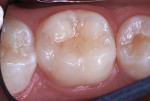
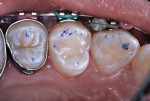
A Class VI caries lesion was diagnosed in a buccal cusp of mandibular first molar in an 11-year-old boy (Figure 5). After routine local anesthetic injection and placement of a rubber dam, the tooth was restored as follows.
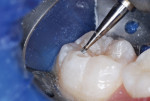
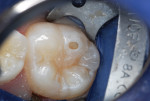
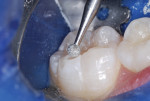
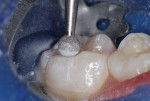
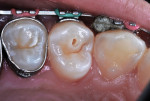
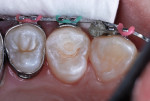
An inverted cone bur at slow speed was used to remove carious tooth structure and to create a slightly undercut preparation design (Figure 6 and Figure 7). A large diamond rotary instrument at slow speed slightly blunted the peak of the cusp tip to distribute future forces of impact from occlusion and mastication and to roughen the enamel for improved acid-etching (Figure 8).
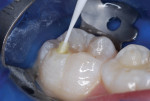
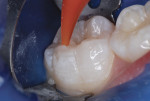
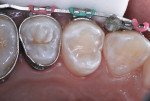
Because the depth of the lesion included dentin, a resin-modified glass-ionomer liner (Vitrebond™ Plus, 3M ESPE) was injected and trimmed to replace dentin lost to caries and preparation (Figure 9). A strongly acidic self-etching adhesive (Adper™ Prompt™ L-Pop™, 3M ESPE) was liberally applied internally and over the enamel around the preparation (Figure 10). The bonding agent was agitated with the brush applicator for 20 seconds. Resin-based composite was then injected to excess, with care to avoid air incorporation. Only one increment of resin-based composite was required in this case (Figure 11) and it was light activated for 20 seconds.
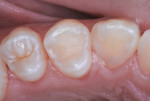
Final trimming was completed with a large round diamond bur at slow speed (Figure 12). The bonding agent was then painted over the resin-based composite and peripheral enamel and a final exposure of the light beam assured complete resin polymerization. The restored cusp is shown 31 months after treatment (Figure 13).
Case 3
A 14-year-old girl in orthodontic appliances had a Class VI caries lesion of the maxillary right first premolar (Figure 14). In addition, the occlusal groove of that tooth was stained. The cusp of the premolar was restored in the identical manner as depicted in case 2. However, this tooth required additional treatment (Figures 15 through Figure 18). The occlusal groove was cleared of debris using a mid-sized Micro NTF Fissurotomy® Bur (SS White, www.sswhitedental.com). Once assured that no caries infection was hidden underneath, the groove was sealed using a self-etching adhesive and resin-based composite material, as described by Croll and colleagues.”6 Such “reinforced sealants” have given excellent service over the decades. The restored and sealed tooth was photographed 24 months after treatment (Figure 19).
Discussion
Some practitioners might question the use of a resin-modified glass-ionomer dentin replacement prior to placement of the resin-based composite. That step does require a bit more time. However, in consideration of the biomimetic approach to tooth repair using adhesively bonded materials,8,9 there is concern about eventual hydrolysis of resin-dentin bonds and differences in biocompatibility of the respective materials. In addition, some pulp horns can extend pulp spaces well up into a cusp so that a caries lesion and tooth preparation might be much closer to exposing the pulp than expected. Ruiz and Mitra succinctly outlined the value and advantages of resin-modified glass-ionomer dentin replacement in resin-based composite tooth repair.10
The nano-ionomer alone was used for the primary molar, rather than stratifying a glass-ionomer base with resin-based composite as shown in cases 2 and 3. Since 2007, Ketac Nano has been used extensively for repair of primary anterior and posterior teeth and has proven itself remarkably durable and reliable over a 6-year period.11,12 The material has all the advantages of other glass polyalkenoate (ionomer) systems and, in addition, the nanofiller technology has improved its physical properties. Although the nano-ionomer does not have the potential for decades of wear resistance in a cusp tip restoration, it does not require that much potential in a tooth that will exfoliate at 10 or 11 years of age.
A strongly acidic self-etching bonding agent was used in cases 2 and 3 rather than a total-etch approach. Because dentin has already been replaced with the chemically bonded resin-modified glass-ionomer “internal” filling material, there is a need to etch only the enamel. The self-etching material simplifies the etching process by eliminating the rinsing and tooth surface drying steps, without compromising etch quality.13
Slight blunting of the treated cusp tip helps to distribute impact forces on the enamel and repair material. Without affecting occlusal relationships, the authors believe that eliminating “jack hammer–like” contacts simply creates minor wear patterns that would have existed eventually as the patient ages, along with relieving pinpoint regional stress concentrations.
Conclusion
Adhesive dental restorative materials have given dentists attractive alternatives to silver amalgam and gold foil for restoring teeth with Class VI caries lesions. Glass ionomer materials can reliably replace lost dentin, and most resin-based composites now have sufficient physical strength and wear resistance for enamel repair, such that long-term durability in Class VI tooth repair can be achieved.
References
1. Black GV. Excavation of cavities by classes. In: Operative Dentistry: Technical Procedures in Filling Teeth. 2nd ed. Chicago, IL: Medico-Dental Publishing Co.; 1914:117.
2. Simon WJ. Clinical Operative Dentistry. Philadelphia, PA: W.B. Saunders Company; 1956:9.
3. Ritter AV, Walter R, Roberson TM. Class I, II, and VI composite restorations and other tooth-colored restorations. In: Heymann HO, Swift EJ, Ritter AV. Sturdevant’s Art & Science of Operative Dentistry. 6th ed. St. Louis, MO: Mosby Elsevier; 2013:254-279.
4. Boushell LW, Roberson TM, Wilder AD. Class I, II, and VI amalgam restorations. In: Heymann HO, Swift EJ, Ritter AV. Sturdevant’s Art & Science of Operative Dentistry. 6th ed. St. Louis, MO: Mosby Elsevier; 2013:353-409.
5. St Germain HA Jr, Rusz JE Jr. Restoring Class 6 abrasion/erosion lesions with direct gold. Oper Dent. 1996;21(2):49-52.
6. Croll TP, Sundfeld RH, Berg JH. A pit-and-fissure clinical protocol. Compend Contin Educ Dent. 2005;26(12):862-868.
7. Croll TP. ASDC Kids Mouth Book. Chicago, IL: American Society of Dentistry for Children; 1999:91.
8. Croll TP, Cavanaugh RR. Posterior resin-based composite restorations: a second opinion. J Esthet Restor Dent. 2002;14(5):303-312.
9. Croll TP, Swift EJ Jr. Tissue-specific, biomimetic, direct-application tooth repair. J Esthet Restor Dent. 2013;25(3):156-158.
10. Ruiz JL, Mitra S. Using cavity liners with direct posterior composite restorations. Compend Contin Educ Dent. 2006;27(6):347-351; quiz 352.
11. Croll TP, Berg JH. Nano-ionomer restorative cement: Observations after 2 years of use. Inside Dentistry. 2009;5(1):60-67.
12. Killian CM, Croll TP. Nano-ionomer tooth repair in pediatric dentistry. Pediatr Dent. 2010;32(7):530-535.
13. Ernst CP. Options for dentin bonding. J Esthet Restor Dent. 2006;18(2):61-67.
About the Authors
Theodore P. Croll, DDS
Private Practice
Doylestown, Pennsylvania
Affiliate Professor
Department of Pediatric Dentistry University of Washington School of Dentistry
Seattle, Washington
Adjunct Professor
Department of Pediatric Dentistry, University of Texas Health Science Center at San Antonio
San Antonio, Texas
Edward J. Swift, Jr., DMD, MS
Professor
Department of Operative Dentistry
Interim Associate Dean for Education
University of North Carolina School of Dentistry
Chapel Hill, North Carolina