Long-Term Results with Connective Tissue Grafting Using an ADM
A case demonstrating 15 years of stable root coverage with esthetic results
Gingival recession occurs when the gingival margin is located apical to the cementoenamel junction (CEJ) with oral exposure of the root surface.1 It has been reported that 50% of individuals 18 to 64 years of age and 88% of persons 65 years of age and older have one or more sites with gingival recession.2 Gingival recession can lead to root surface sensitivity, root caries, esthetic problems, and tooth loss.
The goal of treatment to correct gingival recession has been to re-establish a gingival architecture that covers the root surface that looks natural in appearance and is stable. The subepithelial connective tissue graft technique has been considered the gold standard in the treatment of gingival recession.3,4 However, it requires a palatal surgical site from which the connective tissue graft is harvested. The acellular dermal matrix (ADM) is a connective tissue matrix derived from the skin of an organ donor.5 Its use eliminates the need for a palatal donor site.
It has been more than 10 years since researchers have begun reporting the successful use of ADMs in the treatment of gingival recession defects.6-9 Many of these studies had a relatively short follow-up of less than 18 months. In 2005, Hirsch and colleagues published a report describing long-term results of connective tissue grafting using ADMs.10 They concluded that connective tissue grafting using ADMs to achieve root coverage was predictable and stable over 2 years. The purpose of this report is to describe a case in which a Miller Class I gingival recession defect11 was successfully treated using an ADM and complete root coverage remained stable for 15 years.
Case Presentation
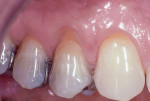
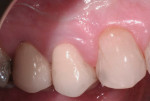
A 62-year-old male patient was referred in 1999 with a chief concern of progressive gingival recession. The patient reported that he noticed the recession defect had deteriorated over the past couple of years (Figure 1). He delayed treatment because he was very concerned about the discomfort he had heard was associated with palatal donor site. Tooth No. 5 was found to have a 3-mm facial gingival recession defect. A narrow facial cervical composite was present adjacent to the enamel. The straight facial probing depth was 3 mm. There was approximately a 1 mm zone of attached keratinized gingiva (AKG). After discussing my findings, treatment options, and risks, we agreed to treat tooth No. 5 with connective tissue grafting using an ADM.
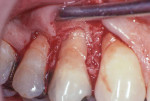
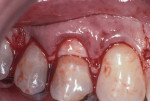
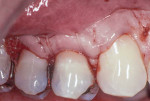
Profound local anesthesia was obtained using 2% lidocaine with 1:100,000 epinephrine. A Bard Parker #15 scapel blade was used to make intrasulcular incisions. A full thickness flap from tooth No. 4 to No. 6 was raised (Figure 2). Using hand curettes and a rotary football-shaped diamond bur, the facial composite was removed and the root surfaces were planed until they were smooth and flattened. An ADM was trimmed to approximately 10 mm x 6 mm. It was placed over the root surface and under the gingival flap (Figure 3). The basement membrane side of the ADM was placed against the root surface. The gingival flap was secured completely over the ADM and root surface using a continuous 4.0 plain gut suture (Figure 4).
At the 6-week re-evaluation, the site was found to have healed well with thicker gingiva and complete root coverage (Figure 5). The straight facial probing depth was 2 mm. The facial gingiva appeared thicker than prior to treatment. A small of amount of the enamel that was recontoured to remove the composite and reduce the tooth eminences can be seen. Residual incision line defects in the adjacent interdental papille are also present.
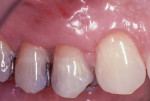
At the 1-year re-evaluation, tooth No. 5 continued to have complete root coverage and natural gingival contours (Figure 6). The straight facial probing depth was 2 mm. The facial zone of AKG was approximately 2 mm. The incision line defects, present at 6 weeks, were no longer present. Tooth No. 5 also had been restored with a crown.
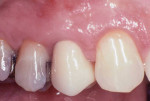
At the 15-year re-evaluation, tooth No. 5 maintained its complete root coverage (Figure 7). The straight facial probing depth was 2 mm. The facial zone of AKG was continued to be approximately 2 mm. The soft tissue architecture of the facial gingiva and interdental papillae appeared healthy and natural in appearance. Tooth No. 4 had also received a crown restoration.
During the 15-year period, the patient maintained 3- to 4-month periodontal recall and supportive therapy appointments alternating between the offices of the general dentist and periodontist. His oral hygiene varied, but was typically fair with mild to moderate plaque accumulations. The patient infrequently smoked cigarettes.
Discussion
Early studies documenting the success of connective tissue grafting using ADMs were very encouraging.6-9 As previously mentioned, Hirsch and colleagues published a report comparing the 2-year follow-up of connective tissue grafting using ADMs with subepithelial connective tissue grafts.10 Both treatments had greater than 98% average root coverage. They found no significant difference in the two treatment methods in final recession or root coverage.
In contrast, Harris reported a difference in results between the two treatment modalities after more than 3 years.12 Only 32% of the patients maintained complete root coverage with an ADM as compared to 84% with a subepithelial graft. It should be noted that the increase in recession of the ADM cases from the short-term (mean 12.3 to 13.2 weeks) evaluation to the long-term (mean 48.1 to 49.2 months) evaluation was only 0.2 to 1.1 mm. Despite this deterioration, the average recession site had improved from 3.2 mm of root exposure at the pretreatment measurement to 1.1 mm of root exposure at the long-term evaluation.
The ultimate goal of all dental procedures is to provide a healthy, functional, esthetic, and stable result. Connective tissue grafting using a palatal connective tissue has satisfied these goals.4,10 It is also beneficial to achieve these results while causing the patient a minimum of discomfort and anxiety. When determining which graft material to use, the patients concerns of discomfort versus long-term results must be considered. In this case, the patient may not have had any treatment if a palatal donor site was required.
Cummings and colleagues compared the histology of sites treated with ADMs and autogenous connective tissue.13 Histologically, both treatment modalities were found to be well incorporated within the recipient tissues. The ADM had new fibroblasts, vascular elements, and collagen, as well as transplanted elastic fibers. Attachment to root surfaces in the ADM and autogenous connective tissue cases was similar.
P.D. Miller Jr. published a classification for marginal tissue recession defects.1 Four categories of gingival recession defects were described. The limiting factor guiding the amount of root coverage that could be expected from any grafting procedure was the height of the adjacent papilla. In Miller Class I defects, marginal gingival recession does not extend to the mucogingival junction and interproximal attachment is intact. These defects tend to have the best results when treated.
In 1999, the availability of ADMs was relatively recent. The patient was very concerned about the possibility of pain associated with the palatal donor site. Given this concern and the likelihood of achieving a good result grafting a Miller Class I gingival recession defect, the patient elected to use an ADM. Complete root coverage and a natural appearance were achieved. In 2014, the site demonstrated long-term (15-year) stable results.
Conclusion
Long-term success in the treatment of gingival recession using connective tissue grafting techniques and an ADM is possible. Controlled studies to confirm the long-term predictability of these results would be useful.
References
1. Wennström JL. Mucogingival therapy. Ann Periodontol. 1996;1(1):671-701.
2. Kassab MM, Cohen RE. The etiology and prevalence of gingival recession. J Am Dent Assoc. 2003;134(2):220-225.
3. Langer B, Langer L. Subepithelial connective tissue graft technique for root coverage. J Periodontol. 1985;56(12):715-720.
4. Chambrone L, Chambrone D, Pustiglioni FE, et al. Can subepithelial connective tissue grafts be considered the gold standard procedure in the treatment of Miller Class I and II recession-type defects? J Dent. 2008;36(9):659-671.
5. Livesey SA, Herndon DN, Hollyoak MA, et al. Transplanted acellular allograft dermal matrix. Potential as a template for the reconstruction of viable dermis. Transplantation. 1995;60(1):1-9.
6. Harris RJ. A comparative study of root coverage obtained with an acellular dermal matrix versus a connective tissue graft: results of 107 recession defects in 50 consecutively treated patients. Int J Periodontics Restorative Dent. 2000;20(1):51-59.
7. Henderson RD, Greenwell H, Drisko C, et al. Predictable multiple site root coverage using an acellular dermal matrix allograft. J Periodontol. 2001;72(5):571-582.
8. Aichelmann-Reidy ME, Yukna RA, Evans GH, et al. Clinical evaluation of acellular allograft dermis for the treatment of human gingival recession. J Periodontol. 2001;72(8):998-1005.
9. Tal H, Moses O, Zohar R, et al. Root coverage of advanced gingival recession: a comparative study between acellular dermal matrix allograft and subepithelial connective tissue grafts. J Periodontol. 2002;73(12):1405-1411.
10. Hirsch A, Goldstein M, Goultschin J, et al. A 2-year follow-up of root coverage using sub-pedicle acellular dermal matrix allografts and subepithelial connective tissue autografts. J Periodontol. 2005;76(8):1323-1328.
11. Miller PD Jr. A classification of marginal tissue recession. Int J Periodontics Restorative Dent. 1985;5(2):8-13.
12. Harris RJ. A short-term and long-term comparison of root coverage with an acellular dermal matrix and a subepithelial graft. J Periodontol. 2004;75(5):734-743.
13. Cummings LC, Kaldahl WB, Allen EP. Histologic evaluation of autogenous connective tissue and acellular dermal matrix grafts in humans. J Periodontol. 2005;76(2):178-186.
About the Author
Douglas H. Mahn, DDS
Private Practice
Manassas, Virginia