Principles of Replacement Dentistry
Complex restorative challenges require advanced materials and techniques
The practice of dentistry has changed significantly in recent years. Gone is the “Golden Age,” when the dentist was the primary source of patient education and knowledge and practice was less constrained by the bureaucracy of insurance companies. During that time, the introduction of more esthetic, metal-free direct restorative options outpaced concomitant technique advancements, making material selection more challenging, as was the case with early attempts at Class II direct composite restorations.
In the past several years, a new era has emerged. With the help of the Internet, dental consumers have access to more dental information than ever before and may be actively seeking services for replacement of failing and mismatched dentistry. Today, in what might be called “The Age of Replacement Dentistry,” practitioners have access to advanced restorative materials and techniques that can meet the needs and desires of their patients. Replacement dentistry is a multi-billion dollar business and should be considered an opportunity for both patients and providers.1
The leading causes of failed composite resin dentistry are secondary decay and fracture.2,3 As a result, Class II restorations are becoming larger buccally and lingually, and interproximal boxes are becoming deeper apically. The successful clinician manages these risks with an armamentarium of cutting-edge materials and techniques to mitigate factors that may compromise the success of the restoration. No longer can the clinician expect traditional circumferential matrices, previous-generation adhesives, or older composite technology to solve complex restorative challenges. Dentists’ choice of replacement materials and techniques must continue to improve and be based on best practices established by leading experts and product manufacturers. This article explores five material strategies clinicians can employ to maximize restorative success to enhance the longevity and predictability of direct restorations.
Matrices
Historically, the most commonly used approach for obtaining proximal contacts has been the application of thin, dead-soft stainless steel matrix bands that circumferentially fit around the tooth. These bands are available for use in a Tofflemire-type matrix retainer (HO Bands™, Young Dental, www.youngdental.com, are 0.001-inch dead-soft stainless steel bands); as conventional Tofflemire-type matrix bands machined to be ultrathin in the contact area (Microbands, Dental Innovations; or as circumferential retainerless matrices (AutoMatrix™ DENTSPLY Caulk, www.caulk.com; SuperMat™, Kerr Dental, https://intl.kerrdental.com). These circumferential-type matrix systems have been used with Class II MO/MOD/MODL(B) preparations. The biggest drawback in using these systems include the time needed to prepare the matrix band and inconsistent interproximal contact creation.
Another class of matrix system is the sectional matrix in combination with a ring. Traditionally these systems have been limited to two-surface Class II preparations for restoring only a single proximal surface. The “weak link” in these systems is the design of the ring. Either metal or plastic, the thin and often poorly shaped ring-tines that fit between two teeth on the buccal and lingual surfaces slip off easily, making them inappropriate for use on shorter clinical crowns and more extensive tooth preparation into either the buccal or lingual cusps. Examples include Contact Matrix™ (Danville, www.danvillematerials.com) and the ComposiTight® matrix with G-Ring® (Garrison Dental Solutions, www.garrisondental.com).
Entirely redesigned, the Palodent Plus Sectional Matrix System™, (DENTSPLY Caulk) incorporates some unique features, using an ultrathin dead-soft stainless steel sectional matrix in combination with a nickel-titanium ring. When placed, the Palodent Plus Sectional Matrix ring is designed to achieve additional tooth separation, which together with the super-curved sectional matrix, results in anatomically correct contact with the adjacent tooth.
The Palodent Plus Sectional Matrix System can be used with virtually all types of interproximal restorations, including MOD and MODL(B). The system allows practitioners to place the Palodent Plus wave wedges before or after placing the ring. The wedges comes in three different sizes and are designed to help seal the matrix band against the cervical portion of the box, while not impinging on the interdental papilla. The rings, sectional matrices, and wedges are uniquely designed for easy handling, pick-up, and control during placement and removal; the wedges and matrices are created with built-in holes to accommodate specially designed pin tweezers.
Adhesives
Very little evolution in bonding systems took place between 1960 and 1980; however, from the early 1990s to 2000, there was an explosion in adhesive technology. Differences in the number of agents used and their mechanisms of bonding have defined each “generation” of adhesive system. The seventh-generation bonding systems combine the acid, primer, and resin in one bottle. These materials require a single step, which eliminates separate etching, rinsing, and mixing for the light-cured products.4,5
A variation on the seventh-generation adhesive system is Prime&Bond Elect® (DENTSPLY Caulk), a universal dental adhesive that delivers high bond strengths to enamel and dentin, with virtually no postoperative sensitivity. It can be used in any direct restorative procedure and can be combined with DENTSPLY Caulk’s Cure Activator in situations where light curing is difficult. This product enables the practitioner to decide how best to use phosphoric acid as part of a total-etch, self-etch, or selective-etch approach.
Bulk Fill
Until recently, the incremental layering technique has been recommended when placing a composite restoration. However, the introduction of bulk-fill composite materials makes fewer placement steps possible by allowing placement of larger increments of composite material. The characteristics of bulk-fill materials that allow this change in technique involve greater depth of cure and reduced polymerization stresses, which help minimize cuspal deflection.6,7
There are several bulk fill composite materials on the market today. Among them is SureFil® SDR® flow (DENTSPLY Caulk). SureFil SDR gives the clinician an advantage in deeper interproximal boxes of Class II restorations for several reasons: there is increased marginal adaptation in the gingival area because the material has a low viscosity and flows easily; it can be placed in 4-mm increments (Universal shade); and it has a self-leveling characteristic for improved placement in any clinical situation.7 Using a bulk-fill strategy in deep interproximal boxes of Class II restorations can improve the success and efficiency of larger or complex restorations.
Composite Technology
With the advent of nano particles, monomer chemistries, optical enhancements, and photo initiator technologies, the composites placed today are truly advanced biomaterials.8 Yet when clinicians are asked why they prefer one composite material over another, references to these modern characteristics are rarely cited; they are instead more likely to mention feel and handling as major factors for their preference. Dentists assume the composite manufacturer has incorporated the latest technology.
The TPH family of composites has been evolving for over 20 years. TPH Spectra® Universal Composite (DENTSPLY Caulk) is the latest and most advanced formulation. Together with other composite improvements, TPH Spectra has improved the optical qualities and blending capability and has dramatically simplified the shading process. Dentists need only two or three shades chairside to handle color matching of approximately 90% of restorations. Handling has also been dramatically improved with a choice of two viscosities: HV (High Viscosity) for clinicians who prefers a firmer, more tactile composite; and LV (Low Viscosity) for practitioners who favor a creamy yet responsive composite. Using the latest in composite technology gives practitioners more freedom to select the materials best suited for a particular clinical situation and to potentially increase the overall quality of restorations produced.
Polish
Finishing and polishing composite restorations requires several subtle steps that contribute to the final result and longevity of the restoration, including gross finishing, contouring, fine finishing, and polishing.9-11 In Class II restorations, practitioners must pay special attention to fine finishing and polishing.
The Enhance® Finishing System (DENTSPLY Caulk) includes single-use aluminum oxide cups, discs, and points. It is designed as a one-step polishing system that simplifies the process because it can be used to contour, finish, and polish composite restorations.
Case Presentation
A patient presented with an existing Class II amalgam restoration on her upper right second premolar bicuspid (tooth No. 4). She complained that food was becoming stuck between this tooth and the tooth immediately distal (tooth No. 3). Upon radiographic examination, it was noted that secondary caries was associated with the disto-occlusal of tooth No. 4. The clinical exam revealed a slight fracture of the interproximal amalgam and an open interproximal contact. The patient complained of occasional gingival tenderness but not tooth pain.
Clinical Protocol
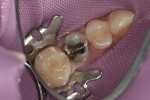
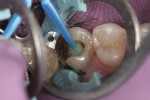
The treatment plan included removal of the existing amalgam filling and replacement with a direct composite restoration. The patient was anesthetized with one carpule of 2% lidocaine containing 1:100,000 concentration epinephrine. Isolation with a rubber dam was achieved (Figure 1), and the clinical protocol described below was completed.
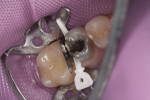
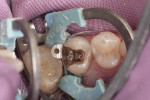
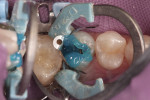
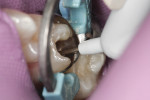
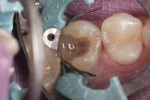
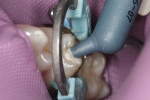
Initial removal of existing amalgam was accomplished with a 558 carbide bur. Prior to removal, a Palodent Plus wedge guard had been placed to ensure that no damage to the adjacent tooth occurred (Figure 2). The preparation was completed by shaping axial/cavosurface walls and removing secondary caries with a round end diamond bur. To ensure proper anatomical form and a tight interproximal contact, both a Palodent Plus matrix band and wedge were placed (Figure 3). Burnishing of the contact area was accomplished with the round end of a composite instrument and the end of the Palodent Plus pin tweezers (Figure 4).
The enamel was prepared with a selective-etch technique using UNI-ETCH® 32% phosphoric acid (BISCO, www.bisco.com) for 15 seconds (Figure 5), followed by rinsing with water. The enamel was left moist. Prime&Bond Elect was placed on both dentin and enamel and scrubbed vigorously for 20 seconds (Figure 6). The excess was blown off, and the preparation was light cured for 20 seconds. SureFil SDR flow (Figure 7) was placed in the base of the proximal box up to the pulpal floor of the preparation (Figure 8), followed by light curing for 20 seconds. TPH Spectra (Figure 9) shade A2 HV was placed as the final occlusal layer over the SureFil SDR flow and cured for another 20 seconds. Shaping and polishing was accomplished with Enhance cups and discs. After the rubber dam was removed, the occlusion and interproximal contacts were check and the patient was released with the completed restoration (Figure 10 and Figure 11).
Conclusion
Because a large number of restorations being done today are performed on previously restored teeth, it is important for the clinician to have a good understanding of the necessary materials to ensure success. Working knowledge of sectional matrix systems will enhance the Class II restoration with anatomically correct, tight contact points, whether doing one or multiple teeth in a quadrant. Having the latest universal bonding system will ensure that large complex Class II restorations are filled and sealed with confidence. When placing composite, whether anterior or posterior, clinicians need to take advantage of the superior technology built into composites today that provides unique handling and optical properties. Finally, to round out the restorative process, the operator needs to have a trusted polishing system that will enhance the restoration without harming the substrate or surrounding teeth. When restorations are managed with the materials and techniques mentioned above, long-term success, longevity, and peace of mind for both the patient and dentist are sure to follow.
Disclosure
Dr. Simos received an honorarium from DENTSPLY.
References
1. Dental amalgam benefits analysis. Health.gov website. https://web.health.gov/environment/amalgam1/appendixI-sectionIV.htm. Accessed March 27, 2014.
2. Christensen JJ. Duplicating the form and function of posterior teeth with Class II resin-based composite. Gen Dent. 2012;60(2):104-108; quiz 109-110.
3. Kopperud SE, Tveit AB, Gaarden T, et al. Longevity of posterior dental restorations and reasons for failure. Eur J Oral Sci. 2012. 2012;120(6):539-548.
4. Lopes GC1, Marson FC, Vieira LC, et al. Composite bond strength to enamel with self-etching primers. Oper Dent, 2004;29(4):424-429.
5. Ozer F, Blatz MB. Self-etch and etch-and-rinse adhesive systems in clinical dentistry. Compend Contin Educ Dent. 2013;34(1):12-14, 16,18; quiz 20,30.
6. Lowe RA. The search for a low-shrinkage direct composite. Oral Health Journal. March 2010.
7. Van Ende A, De Munck J, Mine A, et al. Does a low-shrinking composite induce less stress at the adhesive interface? Dent Mater. 2010;26(3):215-222.
8. Cramer NB1, Stansbury JW, Bowman CN. Recent advances and developments in composite dental restorative materials. J Dent Res. 2011;90(4):402-416.
9. Lutz F, Setcos JC, Phillips RW. New finishing instruments for composite resins. J Am Dent Assoc. 1983.107(4):575-580.
10. Da Costa J, Ferracane J, Paravina RD, et al. The effect of different polishing systems on surface roughness and gloss of various resin composites. J Esthet Restor Dent. 2007;19(4):214-224; discussion 225-226.
11. Peyton JH. Finishing and polishing techniques: direct composite resin restorations. Pract Proced Aesthet Dent. 2004;16(4):293-298; quiz 300.e
About the Authors
Sam Simos, DDS
Private Practice
Bolingbrook and Ottawa, Illinois