Using Minimally Invasive Veneers to Close Anterior Diastemas
New ceramic materials facilitate a more conservative approach that can produce stronger, highly esthetic restorations with minimal trauma to patients' teeth.
Since their development in the 1980s, porcelain veneers have undergone a major metamorphosis.1 From minimally prepared teeth utilizing feldspathic porcelain (0.3-mm to 0.5-mm preparation) to pressed ceramics (0.7 mm or more preparation) such as the IPS Empress® system (Ivoclar Vivadent, https://www.ivoclarvivadent.us), to the minimal- and no-preparation veneers of today, ceramics have evolved to meet the needs of practitioners and patients alike.
With the introduction of products made from lithium disilicate, such as IPS e.max® (Ivoclar Vivadent), today's no-preparation veneers are highly esthetic and extremely strong. A flexural strength of 400 MPa also allows the practitioner to make them very thin.2 IPS e.max restorations give dentists the ability to provide excellent esthetics and functionality, with minimal preparation and/or damage to the surrounding soft tissue and dentition.2
The preparation for these products is minimal compared to conventional full crowns, which significantly decreases the risk of pulpal damage.2 Also, there are less periodontal issues because the margins of the veneers are thin and usually end at or just above the free gingival margin.2 In procedures that involve porcelain veneers, the preparation should be kept in the enamel whenever possible.3 As the linguals of the anterior teeth are usually left intact, the occlusion and anterior guidance can also be more easily maintained.3 The final esthetic result, however, depends on the practitioner's communication with the laboratory technician and the laboratory technician's artistic ability.3
Case Study
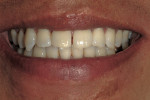
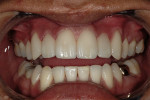
A 22-year-old man presented with the chief complaint of shifting dentition and spatial issues between his front teeth (Figure 1 and Figure 2). These issues developed upon completion of orthodontic treatment 5 years earlier, and he did not like the large diastema between his central incisors.
A comprehensive oral evaluation was completed, which included a temporomandibular joint disorder (TMJ) examination and a periodontal evaluation, including panoramic and full-mouth radiographs. A series of photographs, a bite registration, and impressions for study casts also were taken. His TMJ presented as asymptomatic, but there was evidence of parafunction. His lip-at-rest photograph also revealed that he did not display enough of his central incisors for someone his age. The patient's maxillary anterior teeth appeared esthetically displeasing due to a reverse smile line that resulted from the unusually short central incisors.
The patient's anterior teeth also diverged in different directions. Ideally, the axial alignment of his front teeth should have had a mesial inclination toward the midline, beginning from the central incisors and extending to the canines.4
Different options were discussed, such as orthodontics, direct bonding, and porcelain veneers. The patient previously had orthodontics and did not want to have that treatment again. Direct bonding was also a possibility, but it would be difficult and time-consuming to correct the problems. Porcelain veneers were part of his treatment plan for teeth Nos. 6 through 11.
Laboratory Procedure
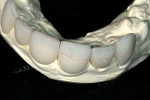
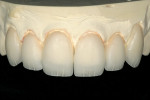
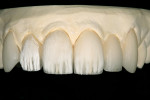
Initially, the study casts, bite registration, and photographs were sent to the dental laboratory for evaluation. A reduction guide was also made to prepare the teeth for movement into a more favorable alignment. Prior to completion of a diagnostic full-contour wax-up, the teeth on the cast were reduced to contour (Figure 3). A study cast, with mock preparations for the veneers, was also fabricated and used as a guide for the reduction of teeth Nos. 6 through 11.
Clinical Preparation
Preoperative shades were taken using a VITA shade guide (Vident™, https://www.vident.com), followed by digital photographs to communicate the correct shading to the laboratory. The patient was then anesthetized using lidocaine with epinephrine 1:100,000. The reduction guide was placed over the teeth and the facial surfaces of the central incisors. The cusp tip areas of the canines were then contoured using a high-speed NSK electric handpiece and a KS1 diamond bur (Brasseler USA, https://www.brasselerusa.com).
The putty matrix was then placed in the mouth to ensure a proper fit. It was filled with a bis-acryl resin (TurboTemp, Danville Materials, https://www.danvillematerials.com) and placed over the anterior teeth, then removed. Upon discussion with the patient, he was satisfied with the appearance of the mock-up. Using the mock-up as a guide, the teeth were prepared for the porcelain veneers.
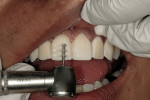
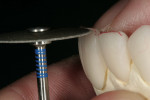
First, the incisal edges were reduced with a depth cut of 1.5 mm using the KS1 bur and connection of the depth cuts to produce a uniform incisal edge. Next, using an 834-016 bur (Brasseler USA) as a guide, depth cuts of 0.5 mm were made across the facial surfaces (Figure 4). The initial depth cuts were then connected using a KS1 bur to create a uniform facial surface without sharp internal angles. The interproximal margins were extended lingually with a KS0 bur (Brasseler USA).
The margins for the veneers were carried to the free gingival margins with the KS1 diamond bur, using a Zykra retractor, to protect the gingival area from being abraded. The margins were then finished with a 661-420 white stone (Brasseler USA). A 0053 brown rubber point (Brasseler USA) was used on the highest speed setting to leave a smooth finish on the enamel surfaces.
Stumpf shades of the prepared teeth were taken with the VITA shade guide and photographed. An initial polyvinyl impression (Aquasil, DENTSPLY Caulk, https://www.caulk.com) was taken and poured in stone (Denstone, Heraeus, https://www.heraeus-dental-us.com) to fabricate the provisional restorations. A final impression was then made of the maxillary arch using the PVS materials.
Using a duplicated model of the diagnostic wax-up, a provisional vacuum-formed matrix was made (Copyplast®, Scheu-Dental GmbH, https://www.scheu-dental.com) using a positive-pressure thermal-forming machine (Biostar®/MiniSTAR®, Scheu-Dental GmbH). The matrix was then filled with shade A1 TurboTemp and placed over the preparations.
The provisional restorations were removed from the cast in one piece and then trimmed to fit the teeth. Once the provisional was completed, it was tried in to verify fit, esthetics, and phonetics. Upon patient approval, the provisional was taken back to the laboratory and coated with Palalseal (Heraeus) to give it the smooth appearance of the surrounding dentition.
Teeth Nos. 6 through 11 were then etched for 15 seconds with 37% phosphoric acid (Ultradent Products Inc, https://www.ultradent.com), followed by rinsing. Gluma (Heraeus) was then applied to all of the teeth to kill bacteria and desensitize them. The provisionals were then filled with a flowable composite (Accolade, Danville Materials) in shade A1 and seated on the teeth.
The excess resin was removed with a No. 3 synthetic brush (Cosmedent Inc, https://www.cosmedent.com) and then light-cured. Care was taken to remove any residual composite, and then the occlusion was checked with articulating paper (AccuFilm, Parkell Inc, https://www.parkell.com). The provisionals were adjusted and polished. Photographs of the provisionals and an alginate impression were taken to communicate specifications to the laboratory (Figure 5).
Laboratory Fabrication
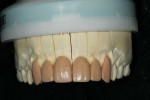
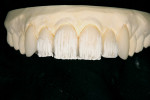
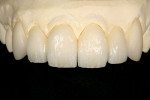
The first step of the laboratory fabrication process was to inject the matrix from the approved provisional model onto the prepared master dies (Figure 6). Once completed, a medium translucency lithium disilicate ingot (IPS e.max Impulse Value 1, Ivoclar Vivadent) was pressed to a thickness of 0.5 mm (Figure 7). The restorations were marked for a 0.5-mm reduction on the facial (Figure 8). A 9001 contour stone (Komet USA, https://www.kometusa.com) was utilized at a low setting to reduce 0.5 mm of the incisal facial area and to taper the face of the restorations. Next, a K6974 cintered diamond disc (Komet USA) was used to undercut the restorations (Figure 9). It was also necessary at this time to cut a deep mesio-incisal and disto-incisal trough to create a natural low-value effect (Figure 10).
High and low internal staining effects were then utilized, with gray stain added to the mesio-incisal and disto-incisal troughs (Figure 11). After staining, IPS e.max Light MM powder (Ivoclar Vivadent) was used, with a single segment of Salmon MM in the middle lobe to compensate for the internal mamelons (Figure 12).
A white dentin powder (IPS e.max, shade 0E3, Ivoclar Vidadent) was then feathered over the mamelons and the cervical middle. The internal powder effects were finished with the addition of IPS e.max Light MM to the incisal edge (Figure 13). Once all internal effects were completed, they were fired in preparation for the enameling process (Figure 14).
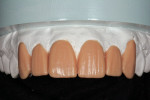
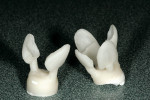
A low-value opal and a high-value tagged blue enamel powder (IPS e.max shades 0E1 and TI1, respectively) were layered in segments until the restoration appeared esthetically correct (Figure 15). Upon completion, the segmental enamel was fired (Figure 16). A medium diamond 842 disc (Komet USA) was used to smooth the surface, create line angles, and establish the heights of the contour (Figure 17). The 842R disc was then used to define the surface lobes and morphology. Once the restorations were glazed and polished, they were sent to the practitioner's office for final placement (Figure 18 and Figure 19).
Clinical Procedure
Using a medium-value try-in gel (Vario link Veneer MVO, Ivoclar Vivadent), each veneer was tried in to verify the fit and path of insertion. Clinical photographs were taken to check the appearance of the veneers. The try-in paste was removed from the veneers, and each veneer was steam-cleaned to remove contaminants.
The veneers for the central incisors were first treated with a conditioner (Clearfil™ porcelain bond activator, Kuraray Dental, https://www.kuraraydental.com) for 20 seconds and lightly cleansed with air. A bonding agent (Clearfil™ Photobond, Kuraray Dental) was then placed in the veneers and lightly air-blown to remove the volatile monomers. After Variolink Veneer was placed in the veneers, they were set in a Resin Keeper (Cosmedent).
The prepared teeth were isolated with the cheek and lip retracted, using OptraDam (Ivoclar Vivadent) and cotton rolls were placed in the buccal vestibule. The veneers were cemented in pairs, the central incisors, teeth Nos. 10 and 11 and teeth Nos. 6 and 7. The central incisors were etched with 37% phosphoric acid for 15 seconds and rinsed. Gluma was then applied to the central incisors. Photobond was dispensed, mixed, and placed with a micro-brush on teeth Nos. 8 and 9. The teeth were then dried with an air dryer (A-dec Inc, https://www.a-dec.com).
Next, the veneers on Nos. 8 and 9 were placed and seated in their final position. The gingival margins of the veneers were then light-cured for 5 seconds to tack them into place. Using a No. 6 sable brush (Cat's Tongue, Princeton Art and Brush Co, https://www.princetonartandbrush.com), the excess resin was removed facially, lingually, and interproximally. The veneers were cured for 20 seconds on the facial and lingual. DeOx® (Ultradent Products) was placed around the margins of the veneers, which were light-cured for 40 seconds, facially and lingually. The DeOx was rinsed-off, and residual cement was removed from the distal.
The veneers for teeth Nos. 6 and 7 were tried on as a pair to ensure that they would fit. The veneers for teeth Nos. 10 and 11 were tried on as well. However, once the first two veneers were cemented, the lateral incisors and canine did not fit completely in place. This was the case with tooth No. 7 as well. Using a 952 Vision Flex diamond disk (Brasseler USA), the distal of tooth No. 8 was lightly buffed until the veneer for tooth No. 7 seated completely.
The veneers were cleaned with the steamer and treated with silane and Photobond. The veneers were then filled with Variolink Veneer and placed in the Resin Keeper. Teeth Nos. 10 and 11 were etched with 37% phosphoric acid, and the veneers were seated. This procedure was repeated with teeth Nos. 6 and 7.
Very little resin needed to be cleaned up, and residual cement was removed with a No. 12 scalpel. Floss was used to remove any cement left interproximally and to administer a final check of the contacts. Accufilm was then used to mark the occlusal contacts, and any occlusal discrepancies were adjusted.
During a follow-up visit, periapical radiographs were taken to check for any cement that may have been under the gingiva. Occlusion was then marked and adjusted once again. An upper alginate impression was taken for use in fabricating a maxillary occlusal appliance to help protect the veneers and the rest of the teeth from parafunction.
There were several areas where the gingiva was still slightly inflamed, and the contour of the gingiva around tooth No. 8 did not match that of tooth No. 9. Topical anesthetic was placed on the gingival of tooth No. 8, and a single wire-tipped electro-surgery unit (Parkell) was used to sculpt the gingiva slightly on the distal half.
Conclusion
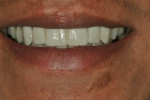
Advances in new ceramic materials such as IPS e.max lithium disilicate allow clinicians and laboratory technicians to take a more conservative approach when removing tooth structure to ensure that as little is removed as possible. With new material innovations, it is now possible to provide highly esthetic restorations that are stronger and procedures that are less invasive, causing minimal trauma to teeth.
References
1. Rufenacht CR. Fundamentals of Esthetics. Hanover Park, Ill: Quintessence Publishing; 1990:329-332.
2. Terry DA. Leinfelder KF, Geller W. Aesthetic & Restorative Dentistry: Material Selection & Technique. Hanover Park, Ill: Quintessence Publishing; 2009:152-153.
3. Chiche GJ, Pinault A. Esthetics of Anterior Fixed Prosthodontics. Hanover Park, Ill: Quintessence Publishing; 1994:42-48.
4. Rufenacht CR. Fundamentals of Esthetics. Hanover Park, Ill: Quintessence Publishing; 1990:85-109.
About the Authors
Brian Dennis, DDS
Private Practice
Albuquerque, New Mexico
Bradley L. Jones, FAACD
Private Practice
Boise, Idaho