Composite Resin as a Viable Alternative to Porcelain
No longer considered a radical new technique for posterior restorations, composite resin proves to be both predictable and profitable when used with the proper protocol.
Jaimee’ Morgan, DDS; Stan Presley, DDS
In this challenging economy, more clinicians will be looking for ways to decrease overhead. While decreasing expenses may be at the forefront of concern, maintaining unquestionable and uncompromising dental services carries equal consideration. While porcelain restorations increase production, they also increase overhead because of the laboratory fees incurred. The porcelain restoration usually involves at least two appointments, one for preparing the tooth, the second to deliver the restoration. These multiple appointments should also be figured into overhead as time invested affects production and income. In some situations, a viable alternative to the porcelain restoration is the direct composite resin restoration. Composite restorations, when performed using a proper protocol, in a time-efficient manner, and with high-quality materials, are esthetic, predictable, long lasting, and profitable.
Composite resin for posterior restorations is no longer considered a new technique, nor is it considered radical or unpredictable. Durability, function, comfort, and esthetics can be achieved when a proper protocol is used in conjunction with rubber dam isolation and high-quality materials. Proper protocol can vastly minimize past problems associated with direct placement, such as postoperative sensitivity, open interproximal contacts, poor anatomy, and questionable longevity. Microhybrid resin systems (eg, ENA HRI, Micerium, www.micerium.com Vit~l~escence®, Ultradent Products, www.ultradent.com) provide both strength and beauty, and can be used for anterior, posterior, direct, and indirect restorations.1 Composite systems that provide this kind of versatility eliminate the need to have area-specific restoratives in the dental office. Paring down the number of products required simplifies inventory control and may decrease overhead because it is easier to keep track of stock and decreases the potential of a product reaching its expiration date. Additionally, the laboratory expense is eliminated as well as the time needed for the laboratory to fabricate the restorations. Patient satisfaction also is improved when procedures can be completed in a single visit.2
The following clinical case demonstrates the proper use of direct composite resin placement protocol combined with the use of a microhybrid resin material (ENA HRi). A simplified and practical approach of using only one shade of composite for posterior restorations was used, thereby saving time without compromising esthetics. The optical depth and dimension required for anterior restorations is rarely if ever appreciated by the patient in posterior restorations. Because there is a certain amount of translucency in the dentin shades, they allow optical integration between the resin and the tooth even when only one shade is used.
Clinical Case
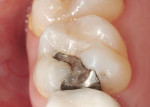
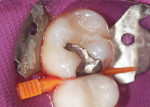
A 36-year-old patient presented with a failing mesio-occlusal amalgam restoration in tooth No. 3 (Figure 1). After the patient was anesthetized, a rubber dam was placed to isolate the area of treatment. A wedge (G-Wedge, Garrison Dental Solutions, www.garrisondental.com) was placed between teeth Nos. 3 and 4 before preparing the tooth (Figure 2 ). This pre-wedging allows more time for the teeth to separate before placement of the restoration, and it also serves to protect the dental papilla from bur trauma. After removal of the amalgam material and recurring decay, the wedge was removed. A Composi-Tight Silver Plus molar sectional matrix (Garrison Dental Solutions) was positioned and the original G-Wedge was re-inserted. If the original wedge failed to offer resistance at reinsertion, the next larger wedge would have been used to continue the separation process. A standard G-Ring (Garrison Dental Solutions) was placed and the interior of the matrix was burnished against the adjacent tooth.
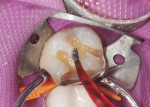
The prepared tooth, both dentin and enamel, was etched for 15 seconds using a 35% phosphoric acid (UltraEtch®, Ultradent Products), rinsed, and excess moisture removed. An antimicrobial agent (Consepsis®, Ultradent Products) was then placed on the etched surfaces and gently air-dried. A single-component dentin bonding agent (PQ1®, Ultradent Products) was applied to the tooth, air-thinned and light-cured for 10 seconds. A flowable composite in shade clear (UltraSeal XT®, Ultradent Products) was brushed onto the prepared tooth as well as the margins as the initial super-adaptive layer (Figure 3). This flowable liner was light-cured for 10 seconds. The microhybrid resin (ENA-HRi) in shade UD2 (universal dentin 2), the equivalent of A2, was placed in 2-mm increments. Each increment was light-cured for 10 seconds. After the complete placement of the resin, the G-Ring, G-Wedge, and segmental matrix band were removed.
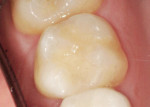
Trimming and shaping were performed using a football-shaped diamond bur (Brasseler 379, Brasseler USA, www.brasselerusa.com) to provide occlusal anatomy, and a flame-shaped carbide finishing bur (Brasseler ETS, Brasseler USA) for the shaping of the embrasures. The rubber dam was removed and the occlusion adjusted using Accufilm I Ribbon (Parkell Inc, www.parkell.com). Occlusal polishing was performed with a carbide finishing bur (Brasseler 274, Brasseler USA), white Jiffy Polisher and Jiffy Brush (Ultradent Products). To enhance marginal integrity and wear resistance, the tooth was re-etched for 5 seconds, rinsed, and air-dried, followed by a thin layer of composite sealer.3,4 The sealer was then air-thinned and light-cured for 10 seconds. Dental floss was used to remove any resin debris from the interproximal contact. The finished restoration exhibited the warmth in the center of the tooth as one would see in a natural, unrestored healthy tooth, as well as a high shine, and imperceptible transition between composite and tooth (Figure 4).
Successfully placing direct posterior resin restorations is simply a matter of combining a quality material with sound clinical protocol. The selection of a resin that not only provides strength, wear resistance, and longevity, but also an esthetically pleasing restoration, creates peace of mind for the clinician. Knowing the proper protocol of resin placement allows the traditional posttreatment issues such as temperature and pressure sensitivity, interproximal food impactions, and resin fracture or debonding to no longer be of concern. With the convenience, low overhead, durability, and esthetics of directly placed resin restorations, it is obvious that this is a viable alternative to porcelain restorations.
References
1. Presley S, Morgan J. Take advantage of improved materials: a rapid and effective posterior resin placement protocol. Inside Dentistry . 2007;3(7):100-102.
2. Jones LA. Elegant esthetics: restoring the natural beauty of teeth with composite. Inside Dentistry . 2007;3(10):102.
3. Kawai K, Leinfelder KF. Effect of surface penetrating sealant on composite wear. Dent Mater. 1993;9(2):108-113.
4. Dickinson GL, Leinfelder KF. Assessing the long-term effects of a surface penetrating sealant. J Am Dent Assoc.1993;124(7):68-72.
About the Author
Stan Presley, DDS
Private Practice
Salt Lake City, Utah
Jaimee’ Morgan, DDS
Private Practice
Salt Lake City, Utah