A Six-Unit Anterior Makeover Case
Michael Gillis, DDS; Luke Kahng, CDT
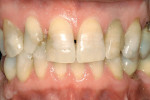
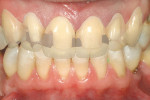
A healthy 44-year-old man presented for improvement of his smile. Clinical examination revealed a number of esthetic challenges. Specifically, this penicillin-allergic patient had substantial exposure to tetracycline as a child and consequent tooth discoloration. Additionally, the removal of a number of teeth as a child led to the drifting of his remaining dentition. At the time of examination, his midline was noted to be 4 mm left of midsagittal. It is worthy to note that the patient was unaware of the midline issue until it was pointed out. He was astonished he had not noticed himself. Nocturnal bruxism, coupled with the movement of his teeth, likely contributed to substantial wear on the palatal aspect of his maxillary anterior teeth (Figure 1). The patient reported that he no longer was a bruxer and the clinical examination did not show any increased muscle tone in the masticatory muscles. However, given his history of bruxism and his rather steep anterior guidance, the patient was instructed to wear an occlusal splint at night after the case was completed.
Periodontally, the patient was deemed to be stable and all remaining teeth showed good hard and soft tissue support. The patient’s temporomandibular joint (TMJ) status was unremarkable. A phased treatment plan was presented to the patient. It was the doctor’s preference that, initially, he would undergo preliminary orthodontic treatment to correct the midline. The patient declined and accepted that the final result would include a retained midline discrepancy.
Case Analysis
A diagnostic wax-up was prepared on models. Impressions for the models were taken with a polyvinyl material, then mounted on a semi-adjustable articulator. An additional set of mounted models was prepared and mounted to record the pretreatment condition.
During the model work, the functional and esthetic challenge of the maxillary anterior became more obvious. Given the dark shade of the teeth, substantial labial tooth structure would most likely have to be removed to allow room for adequate ceramic thickness. However, with the palatal wear, it was noted that any amount of preparation would leave too little tooth structure for support of the restorations. As a result, it was decided to recontour the lower anteriors to create room for palatal ceramic on the upper front teeth. Another concern was the potential for phonetic change. The proposed addition of a thickness of ceramic to the palatal aspect of the maxillary anterior teeth, albeit slight, carried an increased risk of change, especially the “s” sound.1 Although no substantial change in maxillary incisor length was intended, close attention to “f” and ‘v” sounds during the provisional stage was also warranted.
It was decided that a bleaching procedure might help to lighten the teeth before preparation, although whitening tetracycline-stained teeth can be challenging. Studies have shown, however, that a lasting improvement can sometimes be achieved.2,3 Nevertheless, the patient was cautioned that the degree of improvement could not be predicted. It was hoped that the lightened lowers could serve as an esthetic shade target for the maxillary anteriors.
The patient opted for in-office whitening (Illuminé™, DENTSPLY International, York, PA) supplemented by home-applied whitening gel in custom bleaching trays. A modest improvement in shade was achieved (A2 from A3-5). The patient proceeded with preparation 5 months after the whitening procedure and it was noted that the shade improvement remained stable over that time.
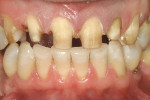
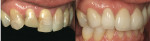
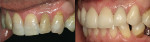
Under local anaesthesia, teeth Nos. 6 through 11 were prepared for ceramic restoration (Figure 2). A diode soft tissue laser (Diolase, American Medical Technologies, Irvine, CA) was used to judiciously correct minor irregularities in the gingival contour. Tissue retraction was achieved and both the final upper and opposing impressions were taken with Aquasil™ (DENTSPLY International). A maximum intercuspation bite registration was recorded (Blu-Bite™, Henry Schein, Melville, NY).
Provisional restorations were made directly with Structur® Premium B1 (VOCO America, Sunnyside, NY) in a PVS/silicone matrix (Figure 3). This matrix was fabricated using the approved esthetic wax-up. Once the material was set, excess was cleared from the margins with a sharp instrument. During the preparation appointment, the goal was to provide provisionalization that would suffice functionally and have reasonably good esthetics. Several days after the preparation appointment, the patient returned for provisional finalization. Occlusally, the provisionals showed no interferences with the envelope of function and the lower anteriors had a positive occlusal stop against the cingulum area of the upper anteriors. Phonetics were checked and all sounds were normal. The patient had good anterior guidance and no teeth were found to be in excursive interference. Esthetically, the patient was very satisfied. The provisionals were polished with Super-Snap® Disks (Shofu, San Marcos, CA) and a PVS impression was taken of the upper arch. An additional Blu-Mousse® (Parkell, Inc, Edgewood, NY) bite registration was obtained and a facebow record taken of the approved provisionals. This method of recording occlusal records would allow the upper preparation model to be fully interchangeable with the model of the provisionals.
The model of the provisionals was poured and mounted with the opposing model on the articulator. All impressions and records were shipped by overnight delivery from Nova Scotia to LSK121 Oral Prosthetics, a dental laboratory in Naperville, IL.
Laboratory Procedures
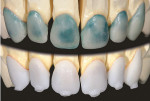
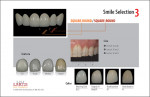
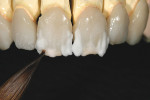
In the laboratory setting, the wax-up understructure for the GC Pure Press™ (GC America, Alsip, IL) investing procedure is shown on the model in Figure 4A. The interproximal contact and incisal edges were checked. After pressing, the copings were modified and prepared for porcelain build-up (Figure 4B). GC Initial™ dentin (GC America) was applied to the copings (Figure 5A), and after the first bake, chroma and incisal porcelain were layered onto the dentin (Figure 5B). When deciding on surface texture and color, the authors followed their smile selection chart (Figure 6).
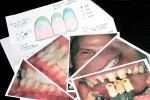
Dr. Gillis’ communication tools helped the technician’s overall progress by covering multiple aspects of the patient’s case: portrait photographs, shade tab communication, and illustrations of the tooth layers and color application (Figure 7). With such detailed information available, the technician can proceed with confidence that he is moving toward an approved finished product.
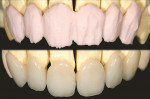
For maximum, brilliant color, a second porcelain build-up was applied (Figure 8). As a measure of the effectiveness to close the noticeable gaps in the patient’s dentition, the technician used a computer-generated program to demonstrate the corrected appearance in the patient’s smile (Figure 9).
Conclusion
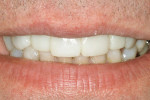
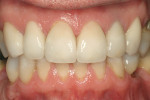
Three weeks later, the final restorations were seated under local anesthesia. Using rubber dam isolation, the provisionals were removed. Two percent chlorhexidine was scrubbed on the preparations for 30 seconds. Gluma® (Heraeus Kulzer, South Bend IN) was used before Optibond® Solo Plus (Kerr Corporation, Orange, CA) and translucent Calibra® (DENTSPLY International). The cement was light-cured and the excess material completely removed. Only minor occlusal adjustments were required. One week later, the patient returned for postoperative photographs and occlusal splint delivery (Figure 10; Figure 11; Figure 12).
Two main issues contributed to the complexity of this case: Moderate to heavy anterior wear, and a midline discrepancy. Addressing the wear introduced a third issue—phonetics. Placing crowns with a thicker palatal contour on the upper anteriors than was present in the heavily worn, untreated teeth introduced a real risk of phonetic change. Therefore, phonetics were checked and the possibilities discussed with the patient before treatment. If any sounds changed, the temporaries would have been modified to the point where phonetics normalized. In this case, no phonetic changes occurred.
The thicker palatal contour of the maxillary anteriors included a distinct occlusal stop that was idealized to the adjusted incisal edge of the lower anteriors. The semi-adjustable articulator and interchangeable provisional and preparation models were helpful to the laboratory in giving an excellent occlusal result.
The midline discrepancy posed a great esthetic challenge. Despite a recommendation to include an orthodontic phase of treatment, the patient declined. He was advised that complete correction would be impossible. Ker et al4 found that a majority of individuals found dento-facial midline discrepancies of up to 2.9 mm to be acceptable. The same study suggested that cants of up to 4% were esthetically acceptable by most. Restoratively, the laboratory was able to migrate the midline to a better position and the patient was satisfied. Great care was taken to not introduce a cant to the midline. Interchangeable models proved helpful in this regard.
References
1. Runte C, Lawerino M, Dirksen D, et al. The influence of maxillary central incisor position in complete dentures on /s/ sound production. J Prosthet Dent. 2001;85(5): 485-495.
2. Leonard RH Jr, Van Haywood B, Caplan DJ, Tart ND. Nightguard vital bleaching of tetracycline-stained teeth: 90 months post treatment. J Esthet Restor Dent. 2003; 15(3): 142-153.
3. Matis BA, Wang Y, Eckert GJ, et al. Extended bleaching of tetracycline-stained teeth: a 5-year study. Oper Dent. 2006; 31(6):643-651.
4. Ker AJ, Chan R, Fields HW, et al. Esthetics and smile characteristics from the layperson's perspective: a computer-based survey study. J Am Dent Assoc. 2008;139(10): 1318-1327.
About the Authors
Michael Gillis, DDS
Private Practice
Halifax, NS Canada
Luke Kahng, CDT
LSK121 Oral Prosthetics
Naperville, Illinois