Treatment Options for the Significant Dental Midline Diastema
Michael R. Sesemann, DDS
From the beginning of time people have noticed, and perhaps passed judgment on, people with prominent spaces in their dentitions. In France, the teeth on either side of a space or gap are called “dents du bonheur” or “lucky teeth.” In Nigeria, a dentition sporting gaps between teeth is considered an exceptionally attractive physical trait. In early English societies, the presence of a gapped-tooth presentation in a female smile was equated with lustful connotations.
In Western society, ambivalence exists as to whether a diastema is a favorable physical trait or not. A small midline diastema is usually not considered unattractive by any group of people.1 However, as the size of the gap increases to a more easily seen physical trait, the level of comfort someone has in personally possessing a “gapped-tooth appearance” may decrease to the point of creating a feeling of self-consciousness. If the condition develops an outward self-consciousness in relation to the way a person feels about a personal physical trait they possess, it can affect the way that person acts in life. This, in turn, could have a negative influence in certain career and social situations in which they are placed.
There can be wide variations of perception concerning the significance of a midline diastema when translated through different cultures, socioeconomic groups, and ethnic backgrounds.2 Indeed, unfair and ill-perceived judgments are leveled at people who possess certain physical traits. When testing the perceptions of subjects viewing anonymous faces with certain features, including dental midline diastemas, the subjects ranked the individuals in the images to be significantly less intelligent, beautiful, and sexually attractive. In addition, the anonymous faces were judged to belong to a lower socioeconomic class than the same faces with an ideal occlusal presentation.3 This finding illustrated that a social disadvantage was wrongly implied, simply on the appearance of one’s dentition—even if it was a healthy one.
The decision whether to live with one’s diastema or not is a personal one. Diastymata are prominently displayed in the mouths of many famous and successful people from all walks of life, including David Letterman, Elton John, Eddie Murphy, Madonna, Lauren Hutton, Michael Strahan, Arnold Schwarzenegger, and Condoleezza Rice, to name a few. However, there remain a significant number of people who do wish to eliminate a diastema if it is part of their dentition.
Because of the varying perceptions, a person may decide to make a dental midline diastema part of who they are or they may wish to eliminate it. If a person decides not to live with their diastema and they seek dental intervention, the task of finding a dental solution that eliminates the space in a responsible way is placed squarely on the dental professional.
Many clinical options exist that can be used for a given situation. The decisions that are ultimately made in rendering the appropriate treatment solution are ones that the patient will have to live with for the rest of their lives, particularly if the treatment solution chosen is one involving irreversible tooth preparation. Therefore, it is extremely important that the dentist and patient discuss all of the treatment options in detail to identify the pertinent and important ramifications that are associated with each particular choice.
A 42 year-old man in excellent physical health and no medical compromises presented to the dental office seeking information and possible treatment to eliminate his dental midline diastema. A comprehensive dental examination revealed excellent overall oral health. The only treatment recommendation, made for the purpose of maintenance, was for the replacement of a few older restorations that were showing signs of marginal deterioration.
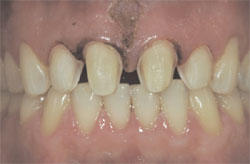
When asked to smile, the patient’s lip retraction capability was moderately dynamic, yet high enough to yield a clear view of a midline diastema measuring 1.79 mm at its most coronal aspect, widening to 2 mm at the height of the central papilla (Figure 1). When in repose, the patient’s maxillary incisors were hidden from view (Figure 2).
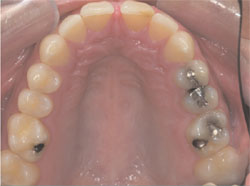
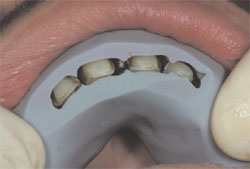
The maxillary incisors were diminutive in size with the central incisors measuring approximately 8.5 mm in height to 8 mm in width, giving a height-to-width ratio of 94%. The prevailing height-to-width ratio was significantly distanced from a visually pleasing range of 75% to 80%, with 78% being the ideal.4 All six maxillary anterior teeth had incurred slight wear over the patient’s lifetime, with the incisors exhibiting enough wear of the incisal enamel to expose dentin (Figure 3).
After the new patient examination and initial consultation, the patient returned for further data collection which included polyvinylsiloxane impressions, a maxillary arch registration with the Kois Dento- Facial Analyzer System (Panadent Corp, Colton, CA), and a bite registration taken with the condyles in centric relation (CR).5,6 Clinically, upon analysis of the patient’s occlusion, it was determined that maximum intercuspation (MI) of the patient’s dentition was different than the patient’s occlusion when his temporomandibular joints were placed in a CR position.
This discrepancy was meticulously carried over to the mounting of the patient’s study models in the laboratory. When the models were mounted using the CR bite registration from the data collection appointment, MI and CR occlusion were not coincident. When the mandibular study model was closed to occlude against the maxillary study model, early occlusal contact occurred on the mesial marginal ridges of the maxillary first bicuspids, mimicking the clinical presentation seen in the operatory.
A diagnostic laboratory equilibration of the CR-mounted study models demonstrated that very little tooth structure would need to be eliminated through selective odontoplasty to make MI and the patient’s CR occlusion coincident. Because of the necessity to have an optimally functioning occlusal scheme postoperatively, the decision was made that if any restorative treatment solution for the diastema was undertaken, it would have to include a clinical equilibration to achieve a similar clinical outcome for the patient’s postoperative occlusion. This would create a favorable synergy between esthetics and function that would enhance the potential to have increased longevity in the life of the restorations.7
An important determination needed to be made: would the patient’s natural cuspids provide the anterior guidance necessary to accommodate restorations on the incisors when the mandible went into lateral excursive movements? This was especially important because the restorations would be longer than the patient’s current incisors, which exhibited incisal wear. Those same cuspids would need to provide complete disclusion of the posterior teeth without balancing contacts during those same movements.
In addition to establishing occlusal stability from centric relation, a functional analysis would need to be done in the diagnostic wax-up, and eventually the provisional prototypes, to make sure that the new restorations would be compatible with habitual movements such as those that occur in mastication8 and speech.9 The steepness of the interarch relationship in the area of the cuspids (along with the type of food) determines to a large degree the path of closure during mastication.10,11
There was one important factor that would work in the restorative team’s favor to incorporate the natural cuspid morphology into an optimal anterior guidance, thereby reducing the number of restorative units necessary for treatment. Because of the diminutive size of the maxillary incisors, any restorative effort could be additive, not only adding incisal length to the incisors but also positioning the incisal edge of the maxillary incisors further facial. This would provide a greater distance for clearance between the maxillary and mandibular incisal edges when the patient was in function.
After determining that the cuspids could be viable guidance for disclusion of the posterior teeth in lateral and functional movements, it was time to fabricate a diagnostic wax-up to see what clinical dimensions the incisor restorations could be while using the natural maxillary cuspids for protection. Initially, the wax-up illustrated that the size of the central incisors could be increased to a dimension of 10.85 mm in height without contact in functional movement (Figure 4, Figure 5, Figure 6). This was important because the width of the central incisors would be increasing to compensate for the restorative elimination of the midline diastema. Any further increase in the width of the restorations, without an increase in their height, would not allow us to reach a desirable height-to-width ratio.
The last factor to work out in the diagnostic wax-up was the appropriate dimensions of the lateral incisors. Specifically, what dimensions would the lateral incisors have to be to complement the proposed new dimensions of the central incisors, and how far would they need to extend mesially to portray a favorable and harmonic dimensional change? This determination was critical because it would dictate the commensurate distal extension of the central incisor restorations. This in turn would decide whether orthodontics would be necessary to spatially arrange the incisors by moving the central incisors mesially for an optimal restorative solution. It would also affect the choice of material options available.
The completed laboratory analysis via the diagnostic equilibration and wax-up provided a great deal of information:
- The number of restorative units needed to optimally eliminate the patient’s dental midline diastema would equal four (on teeth Nos. 7 through 10).
- The wax-up illustrated how the individual restorations would appear dimensionally and whether an occlusal/ functional scheme could be worked out that would provide proper force management for longevity of the restorations.
- The wax-up would serve as the prototype design for the direct fabrication of the provisional restorations so that laboratory approximations could be adjusted and verified in vivo.
The only factor left to contemplate and decide on would be to determine what would be the best restorative material for this particular case, taking into account various elements of the patient’s personal life and career.
As a matter of record, this author believes that the practitioner who professes to possess a certain level of esthetic expertise should be able to competently use a variety of materials for a given situation. This particular case could be handled competently with two distinctly different classes of restorative materials and techniques: either direct composite or indirect porcelain veneers.
It is an incredible advantage for the esthetic-minded practitioner to possess the skills necessary to competently use composite restorative material with direct resin bonding for composite veneers, especially for a “no-preparation” option. Composite resin could certainly work for this case; however, the composite restorations would have to be placed over prepared teeth or orthodontic movement would need to take place before any restorative work to attain the sought-after dimensions for the anterior restorations.
There was acute attention paid to understanding the proportionate balance of the incisors in the work-up of this case. Therefore, it was known that in order for the case to be dimensionally optimum, either orthodontic movement of the central incisors mesially or a compensatory preparation of the distal contour of the central incisors would have to be completed to perceptively move the central incisors closer to the midline. Because the nature of the restorations would be additive, it was determined that the extent of the preparation would not remove significant tooth structure that would compromise the biologic properties of the tooth when compared to its non-prepared state.
Essentially, the preparation would leave enamel over 90% of the bondable surface, therefore leaving an optimum tooth surface for bonding the restoration.12 In addition, the structural component of the dentino-enamel junction (DEJ) would be saved, conserving the tooth’s ability to resist structural deformity upon being stressed.13 In a number of studies, when the structural integrity of the DEJ is conserved and an appropriate restorative modality is carried out, the complete biomimetic properties of the natural tooth can be retained in the restored tooth.14,15
Because either composite or porcelain material could work for this case, a description of the pros and cons of each material and its longevity was reviewed with the patient. Images of previously treated cases were shown to the patient so he could make an informed decision. The patient chose the porcelain option.
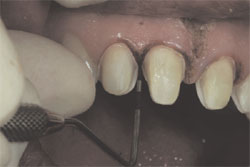
To compensate for the central incisor restorations and to make the centrals appear to be in a more mesial position, the periodontal tissues needed to be altered to make that mirage appear real (Figure 7). After the administration of local anesthesia, sounding of the gingival complex surrounding the maxillary incisors was carried out to determine if the gingival treatment would include crown lengthening of the alveolar crest or soft tissue changes only via gingivoplasty.16 Because the gingival complex was in a low-crest relationship around the incisors, it was determined that a simple gingivoplasty would be all that was needed to place the free gingival margin in harmony with the intended restorations and in a very stable normal crest relationship, as described by Kois.
The gingivoplasty was completed using a soft tissue diode laser at the preparation appointment. Particular attention was given to making the gingival zenith in harmony with the future restorations, not the prevailing tooth position (Figure 8). A labial frenectomy was subsequently completed, as well as papillary re-shaping.
Silicone putty (Sil-tec Putty; Ivoclar Vivadent, Amherst, NY) preparation guides formed over the diagnostic wax-up would serve as a reference during preparation (Figure 9). They would prove particularly useful in helping to guide the preparation depth on the distal surfaces of the maxillary central incisors to accurately provide the correct space for the intended restoration thickness (Figure 10). Because of the changing position of the interproximal contacts between the central and lateral incisors, the preparation had to be carried through the contact between those teeth to provide the room for natural emergence contours. The natural interproximal contacts between the lateral incisors and the cuspids were preserved (Figure 11). Margin placement was verified after preparation through sounding to the alveolar crest (Figure 12).
As stated previously, stringent objectives concerning preparation design were put forth for enamel and DEJ preservation.11-14 The list of manuscripts and research documents supporting conservative preparation are well represented in the literature.17-19
Provisionalization was accomplished using a bis-acryl temporization material (Luxatemp®; Zenith/DMG Brand Division, Foremost Dental LLC, Englewood, NJ) that had been formed directly in the mouth, removed, finished in the laboratory, characterized with resin tints for a polychromatic appearance and sealed with a composite sealer (LuxaGlaze®; Zenith/ DMG). After fabrication, the provisionals were seated by using a spot-etch procedure by etching a 2-mm area on the tooth’s prepared facial surface and using low-viscosity resin as a temporary cement. The patient was seen in 48 hours to verify the appearance and functionality of the provisionals (Figure 13 and Figure 14). Images and impressions were then taken to be used as 3-dimensional communication with the dental laboratory.
The restorations were fabricated and returned to the dental office for seating (Figure 15). Though their composition was leucite-reinforced material (IPS Empress®; Ivoclar Vivadent), the restorations were only 0.65 mm in thickness in some areas (Figure 16). Although not advocated to be used at that thickness by the manufacturer, the restorative team of the author and Lee Culp, CDT, has repeatedly used IPS Empress at that thickness successfully throughout their working relationship of 12 years. The thinness of the restoration and the additive nature of the technique allowed for the retention of etched enamel for bonding and conservation of the DEJ for deformation resistance, resulting in a conservation of the tooth’s natural biomimetic behavior (Figure 17).13-15
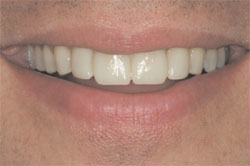
The dental midline diastema is present in a significant portion of the world’s population. People in western civilizations vary as to their views on whether to retain a diastema or whether to eliminate it through cosmetic dentistry when they personally possess one. When a patient presents to a dentist wishing to eliminate a diastema, the situation requires a systematic evaluation that can determine all of the esthetic, functional, and biologic implications that apply to the particular case. The dentist and patient need to work together to analyze all of the options and identify a proper course of treatment for the individual and their circumstances. When a proper course of action is taken, an optimal result with favorable esthetic, functional, and biologic consequences can be provided (Figure 18, Figure 19, Figure 20).
References
1. Kokich VO, Kokich VG, Kiyak HA. Perceptions of dental professionals and laypersons to altered dental esthetic: asymmetric and symmetric situations. Am J Orthod Dentofacial Orthop. 2006;130(2): 141-151.
2. Reichmuth M, Greene KA, Orsini MF, et al. Occlusal perceptions of children seeking orthodontic treatment: impact of ethnicity and socioeconomic status. Am J Orthod Dentofacial Orthop. 2005;128(5):575-582.
3. Kerosuo H, Hausen H, Laine T, Shaw WC. The influence of incisal malocclusion on the social attractiveness of young adults in Finland. Euro J Orthod. 1995;17(6):505-512.
4. Chiche G, Pinault A. Esthetics of Anterior Fixed Prosthodontics. Chicago, IL: Quintessence Publishing Co, 1994.
5. Dawson PE. Evaluation, Diagnosis, and Treatment of Occlusal Problems. 2nd ed. St. Louis, MO: CV Mosby Co, 28-55.
6. Dawson PE. Optimum TMJ condyle position in clinical practice. Int J Perio Rest Dent. 1985;3:11-31.
7. Miller L. Symbiosis of esthetics and occlusion: Thoughts and opinions of a master of esthetic dentistry. J Esthet Dent. 1999; 11(3):155-165.
8. Pameijer JHN, Glickman I, Roeber FW. Intraoral occlusal telemetry III. Tooth contacts in chewing, swallowing and bruxism. J Periodont. 1969;40: 253-258.
9. Howell CT. Incisal relationships during speech. J Prosthet Dent. 1986;56: 93-98.
10. Nishagawa K, Nakano M, Bando E. Study of jaw movement and masticatory activity during unilateral chewing with and without balancing side molar contacts. J Oral Rehab. 1997;24:691-696.
11. Hiiemae K, Heath MR, Heath G, et al. Natural bites, food consistency and feeding behavior in man. Arch Oral Biol. 1996;41: 175-189.
12. Anusavice KJ. Structure of matter and principles of adhesion. Phillip’s Science of Dental Materials. 10th ed, Philadelphia, PA; WB Saunders; 1996.
13. Magne P, Belser U. Bonded Porcelain Restorations in the Anterior Dentition: A Biomimetic Approach. Carol Stream, IL: Quintessence Publishing Co, Inc; 2003;23-54.
14. Magne P, Douglas WH. Porcelain veneers: dentin bonding optimization and biomimetic recovery of the crown. Int J Prosthodont. 1999;12:111-121.
15. Magne P, Douglas WH. Cumulative effect of successive restorative procedures on anterior crown flexure: Intact vs veneered incisors. Quintessence Int. 2000;31:5-18.
16. Kois JC. Altering gingival levels: The restorative connection Part I: Biologic variables. J Esthet Dent. 1994;6(1):3-9.
17. Magne P, Douglas WH. Rationalization of esthetic restorative dentistry based on biomimetics. J Esthet Dent. 1999;1:5-15.
18. Castelnuovo J, Tjan AHL, Phillips K, et al. Fracture load and mode of failure of ceramic veneers with different preparations. J Prosthet Dent. 2000;83:171-180.
19. Stappert CFJ, Ozden U, Strub JR. Longevity and failure load of ceramic veneers with different preparation designs after exposure to masticatory stimuli. J Prosthet Dent. 2005;94:132-139.
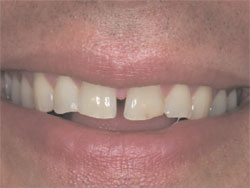 |  | ||||
| Figure 1 Patient’s smile appearance exhibiting a dental midline diastema of 1.79 mm to 2 mm. | Figure 2 Patient’s oral presentation when lips were in repose. | ||||
 | 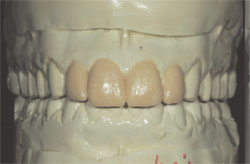 Figure 4 | ||||
| Figure 3 Occlusal view of the maxillary arch showing wear of the incisors through to dentin. | |||||
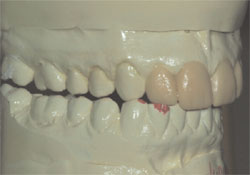 Figure 5 | 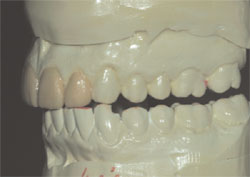 Figure 6 | ||||
| Figure 4 through Figure 6 The diagnostic wax-up showing possible dimensions of the proposed incisor restorations and their interplay with the mandibular teeth when the mandible is in lateral excursive movements. | |||||
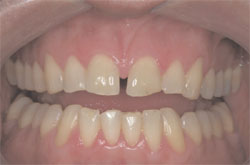 | 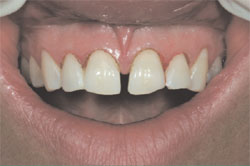 | ||||
| Figure 7 The patient’s gingival levels before gingivoplasty procedures. | Figure 8 Gingivoplasty procedures carried out with consideration of the future restoration size and intended gingival zenith location. | ||||
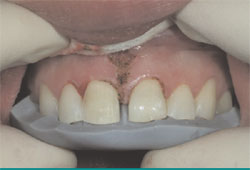 |  | ||||
| Figure 9 Palatal silicone putty preparation guide tried in before tooth preparation. | Figure 10 Labial silicone putty preparation guide allowing visualization of critical interproximal contact location. | ||||
 |  | ||||
| Figure 11 Preparations finalized after periodontal gingivoplasty and frenectomy. | Figure 12 Margin placement on the prepared tooth relative to interproximal alveolar crest verified through “sounding” procedure. | ||||
 | 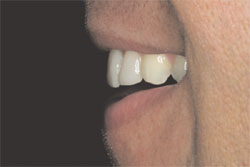 | ||||
| Figure 13 Patient displays natural smile for visualization of prototypes and satisfaction of smile design principles. | Figure 14 Profile view of provisionals shared with laboratory to convey the importance of the exact incisal edge position for phonetics and lip closure. | ||||
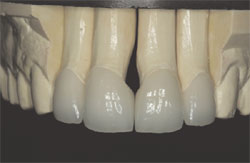 | 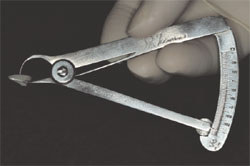 | ||||
| Figure 15 The leucite-reinforced porcelain restorations. Note the extensive over-contour necessary to eliminate a 2-mm midline diastema. | Figure 16 Boley gauge showing the thickness of the restoration to be 0.65 mm. | ||||
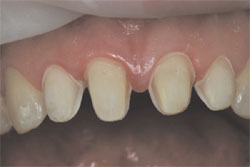 | 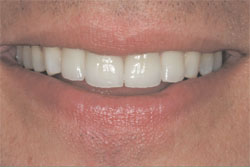 | ||||
| Figure 17 Prepared teeth after acid-etching for bonding illustrate the enamel surface that was meticulously preserved. | Figure 18 The patient’s natural smile with leucite-reinforced porcelain veneer restoration on teeth Nos. 7 through 10. | ||||
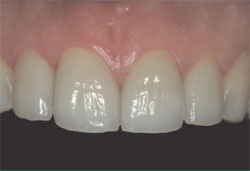 |  | ||||
| Figure 19 A close-up view of the restoration. | Figure 20 A confident patient, at ease with his decision to eliminate the midline dental diastema. | ||||
| |||||




