Challenging the Underuse of Composites in Support of Minimally Invasive Dentistry
Brian LeSage, DDS
In the late 1970’s within the dental community, cosmetic dentists were often looked at unfavorably for practicing “bondodontics” that was based on some science, but using a generation of materials and techniques that were not yet proven. Clinicians tended to have a poor understanding of and limited research about adhesive dentistry. From a material standpoint, there was not the level of enhanced materials that we have today, and the adhesive sciences were very weak. Dentists were using a third-generation adhesive system which, by today’s standards, is old adhesive dentistry. Equally important, the materials were more like epoxy-type composites that required mixing A and B components. Dentists only had so many seconds to apply this composite to the tooth and get it where they wanted it. Because these were small-particle composites, fractures occurred, as well as a lot of staining over time.
Yet, in those early years, dentists knew they could affect changes by adding material to existing tooth structure, without the need or desire to remove too much or prepare too aggressively. Although they worked with primitive resins and had not yet cultivated an understanding and ap-preciation of the material and optical properties of the resin, those dentists were pioneering cosmetic dentistry.
At the same time, dentists practicing cosmetic dentistry also were looked down on because they were practicing what many thought was unnecessary dentistry. Many members of the community thought it was unethical to treat a patient exclusively from an esthetic standpoint, a point of view that really stayed out of the realm of mainstream dentistry in the 1970s and into the 1980s.
It was in the early 1980s that Calamia1 and Horn introduced the innovative concept of bonding thin pieces of porcelain to teeth. Initially and understandably there were questions surrounding the long-term success of these restorations, and even into the 1990s many doubted this technique. When the public started to demand these procedures for a multitude of reasons, porcelain veneers captured and mesmerized the field of cosmetic dentistry, almost to the point that some thought direct composite bonding would be replaced.2
However, some clinicians did not feel comfortable bonding composite to enamel and especially to dentin, and many would excise tooth structure in the form of crown preparations to satisfy their patients’ esthetic demands. Based on the old thinking that porcelain needed to be a uniform 1-mm thickness to maximize its physical properties, dentists were taught to prepare teeth aggressively for veneer restorations. The author includes himself among those who taught that philosophy.
Now, dentistry seems removed from the additive ideology of the 1970s, and many clinicians find it easier to prepare sound tooth structure for indirect esthetic restorations than to devise a collaborative treatment plan with team members that is truly minimally invasive. The author suggests that the dental community’s relationship with porcelains and even the newer ceramics (such as zirconia) that require as much and maybe even more removal of tooth structure has become almost one of dependence.
Understanding the Consequences of Preparations
Ultimately, it is the clinician’s experience and professional knowledge that will determine the appropriate treatment plan based on each patient’s clinical situation and esthetic demands. However, asking patients what is important to them (eg, esthetics vs longevity of restorations), as well as how important conservation of natural tooth structure is to them, can help establish their understanding of what is required to provide them with the esthetic treatments they want and the prognosis of that option.
As a self-regulating profession, dentists owe it to their patients to think about the long-term consequences of removing sound tooth structure. In fact, dentists must ensure that their patients comprehend the risks associated with significant removal of circumferential tooth structure, as well as taking preparations into the sulcus for retention and resistance form. As part of ethically obtained informed consent, patients must understand that in the future, these preparation choices could lead to endodontic and periodontal problems. Additionally, they should be made fully aware—depending on their age—that they may need to replace their restorations for esthetic, restorative, periodontal, adhesive, or functional reasons multiple times during their lifetimes.3
Weighing the Restorative Options Against the Indication
Today, dentists understand that when it comes to treating patients, they have to treat the whole patient, which includes esthetic components. To be a comprehensive cosmetic dentist, esthetic concerns cannot be treated separately; they need to be fully integrated into the myriad of parameters and considerations that clinicians face when establishing a diagnosis and developing a treatment plan for a fully functioning dentition.4 Today, with cosmetic dentistry having become a valid form of dental treatment, the issue has become how to deliver the desired esthetic changes appropriately and ethically while doing no harm. There are no definitive guidelines in the dental profession to dictate how or when to perform more aggressive or less invasive techniques. Clinicians, therefore, must use their own judgment.
Are porcelain veneers the most conservative, least invasive, and most predictable tooth-colored restorative option for returning teeth to normal form and function? When compared to a crown, absolutely. But when might they not be? What if the case involved only closing a small black triangle or medium black triangles? What if the patient presented with a less than 1-mm diastema? What if it were a less than 2-mm diastema? What if the patient had an existing class IV fracture that involved less than 40% of the tooth? What if less than 15% of the tooth was affected? What if the patient was your daughter or son? Would an indirect ceramic be your first treatment choice?
What would the appropriate restorative material be if the patient exhibited a slight amount of wear into the dentin on the incisal edge of a maxillary tooth? What if the tooth were a cuspid on a 16-year-old child? Is porcelain really the material of choice to treat these clinical scenarios?
Choosing between direct composite veneers and indirect porcelain alternatives involves understanding how many teeth are being treated and how many will be needed to enhance the smile in some fashion. As previously suggested, the amount of tooth structure already missing and in need of replacement also will direct the clinician toward the appropriate treatment option. If there is good sound enamel for bonding, which will facilitate the use of either composite or porcelain, the more conservative option is the author’s preference.
Occlusion and function should also be addressed. Bruxing, parafunctional habits, and occlusal pathology can be contraindications for direct composite restorations. When the indication suggests—or rather dictates—that a conservative and minimally invasive restorative technique is required, today’s composites should be considered. From a functional, esthetic, and long-term standpoint, today’s composites represent a significant evolution from 30 years ago and may represent the conservative, minimally invasive, and functionally/esthetically predictable options dentists need to offer their patients.
Today’s Composites
Today, after years of amassing tremendous, voluminous, and extensive research about adhesive dentistry, it may be time to reconsider preparation design and thought processes regarding esthetic dentistry. Within recent years, direct composites, and dentists’ mastery of techniques for their application, have reached sophisticated levels. Dentists know what they are doing and the consequences of their actions. Dentists can combine clinical and artistic skills with material science to produce direct resin restorations that are functionally sound, esthetically unrivalled, and minimally invasive.5
The advancements that have occurred over the past 30 years in composite technology have rendered this category of restorative material the perfect dentin replacement and an excellent enamel re placement. Composites can be divided into three classifications: microhybrids, microfills, and nanofillers.6
Microhybrid composites demonstrate a coefficient of thermal expansion (CTE) similar to dentin and are less water resorptive and optically closer to dentin.6 Their advantage is strength, and they are excellent replacements of enamel and dentin in functional areas. These advantages are because of the particle sizes that comprise their content, as well as the composites’ filler loading. Microhybrids’ disadvantage is their inability to hold a polish over the long term. This too is because of the size and loading of the particles and a phenomenon called plucking.6
Microfill composites perform marginally under heavy stress-bearing areas. They exhibit superb polishability and demonstrate low wear because of their particle size and loading.6 Microfills can be polished to any desired luster or finish, and will hold that shine for many years.
Nanofillers are relatively new, but show much promise. Having been introduced in the late 1990s, they do not have the 20+ year history of the other two classifications. They have a diverse particle size and filler loading that may prove to impart the advantages of both existing classifications while limiting their disadvantages.6 This would make for a composite that has strength under function, low wear, and exceptional polish over the long term. Although nanocomposites represent the next generation of direct restoratives, their performance in terms of wear resistance and strength requires evaluation.7 More in vitro and in vivo studies to fully substantiate the attributes of nanofilled composites are needed.
It is not the author’s suggestion that composite is the treatment option of choice for all clinical situations. Composites, as with porcelain and all restorative materials—be they gold or zirconia—perform best and provide predictable clinical/esthetic function when used for carefully selected indications. The most appropriate restorative option for a given indication must be determined with evidence-based literature and research, informed ethical and comprehensive consent, clinical experience, and know-how.
However, if direct composite restorations are indicated but the skill set required to create them is beyond the clinician’s comfort level, then a referral should be made. Referring the patient to someone who is well-trained in direct composites or cosmetic dentistry is no different than making a referral to a periodontist, endodontist, orthodontist, or prosthodontist.
The following cases demonstrate the use of composites to assist in delivering minimally invasive dentistry while meeting the patient’s demanding esthetic expectations.
Case 1
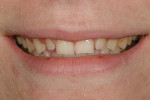
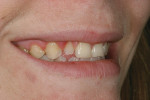
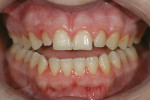
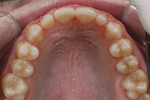
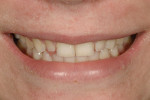
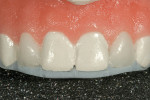
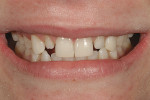
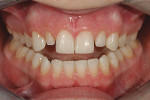
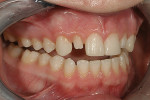
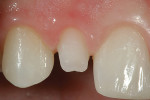
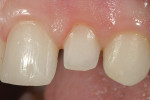
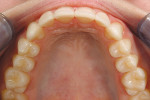
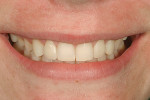
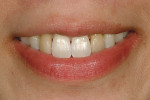
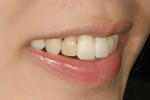
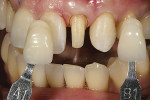
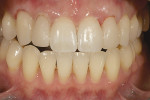
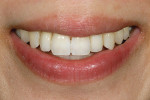
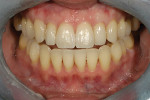
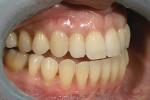
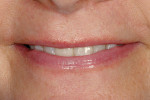
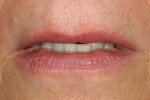
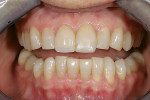
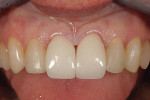
A 15-year-old girl who completed orthodontic treatment 1 year prior presented to address remaining esthetic concerns about her smile. Originally, it was determined that she had a tooth-size discrepancy, and the laterals were positioned to accommodate future restorations (Figure 1; Figure 2; Figure 3).
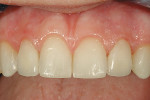
The esthetic issues that needed to be addressed were the display of tooth structure in the repose and pleasing smile, minor wear on the cuspids, and the diastemas on the mesial and distal aspects of the laterals caused by their pegged shape (Figure 4 and Figure 5). A whiter smile also was desired.
The patient and her parents indicated that they wanted the best treatment possible, but preferred that no tooth structure be removed. A comprehensive discussion followed about the advantages, disadvantages, and long-term maintenance of direct composite veneers and porcelain veneers. Her parents appreciated the conservative approach and concern regarding the future dental needs of their daughter. They understood that with a 15-year-old, these restorations would need to be replaced multiple times in her lifetime, regardless of the material chosen. They selected the most conservative and least invasive technique available, with cost being the least determining factor: direct composite veneers on teeth Nos. 6, 8, 9, and 11, and indirect “prepless” porcelain veneers on teeth Nos. 7 and 10. Note that “prepless” veneers are rarely done completely without any preparation. In this case the author used a very minor finishing line, just enough to aid the ceramist in determining where to put the finish line. The amount of composite in three dimensions will aid in the decision-making process. For example, small peg laterals will require a significant amount of composite to be added interproximally, facially, lingually, and incisally. Obtaining ideal emergence profiles circumferentially is very challenging, and if the author can do a “no-prep” porcelain veneer that is fabricated indirectly, he feels that he can better manage the tissue response, interproximal contacts and connectors, seamlessness, and polychromicity more effectively and efficiently for the long-term.
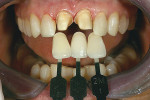
Tray bleaching using a take-home whitening kit (16% carbamide peroxide NiteWhite®, Discus Dental, Culver City, CA) for 10 days after prophylaxis treatment initiated the smile makeover. The teeth were taken from a 1.5R2 shade—as determined using the VITA Easyshade® (Vident, Brea, CA) spectrophotometer—to a 1M1. This was a pleasing shade for the patient and her parents and would be used for the definitive restorations after a 10-day period to allow for minor shade relapse and normal tooth hydration.
At the bonding appointment, the tooth shade was taken again and recorded to be a 1M1 (Figure 6). The teeth were pumiced, and a small bevel was placed to smooth out any pointed areas that existed and to help create a seamless restoration. Build-up of the restoration began using a new microhybrid composite system (3D®-Direct™, Vident).
A preliminary model was taken and a composite mock-up was made (Figure 7). The mock-up, including the matrix, was completed in the laboratory prior to the bonding appointment. The putty matrix was made to help guide the lingual and incisal contours. The proprietary layering color guide for shade 1M1 and 3D-Direct composite shade OP 0M2 were used. The initial composite layer filled the lingual contour, creating a shelf into which the remaining restoration would be blended. While all of the direct restorations could either be built simultaneously or done individually, the author usually chooses to do one or two at a time to maintain control and allow for revisions throughout the appointment. This first layer, being of highest opacity, was carried onto the incisal facial line angle to match the optical properties of the existing enamel. Space was left on the facial for incisal effects and halo. The second composite layer, shade 1M2, started to develop the dentinal lobes and help to create zones of higher chroma deep within the incisal third. The third composite layer, shade EN2, was used to build translucency between the dentinal lobes. An outer composite layer of shade T4 (translucent) established a clear filter on top, imparting depth and balance to the tooth’s color.
Initial outline form was produced using coarse diamonds and discs (Finishing Disc, Bisco, Inc, Schaumburg, IL). The remaining primary anatomy and finishing were created using a propriety bur kit (UCLA LeSage Anterior Aesthetic Restorative System, Brasseler USA). Electric hand pieces (NSK, Brasseler USA) and a coarse diamond were used at varying speeds to blend the texture with the existing tooth structure. Next, medium finishing discs were used to finish the composite restorations and complete the first appointment. A low-viscosity, light-cured resin sealant (BisCover™ LV, Bisco, Inc) was placed to protect the composite for the first 72 hours, while the “dark cure” occurred (ie, cross-linking continues to occur in the composite despite the removal of the curing light).8 Photographs were taken for self-evaluation and laboratory communication (Figure 8; Figure 9; Figure 10).
The veneer preparations for teeth Nos. 7 and 10 involved only placing a very minor finishing line. This was done to aid the ceramist in knowing where the margin should begin (Figure 11A and Figure 11B). Restoring peg laterals equates to a diastema closing situation, in which instance an interproximal subgingival margin is preferred. After placing the margin using a coarse diamond (6869-L), two final impressions were taken using a reversible hydrocolloid material (Slade, Van R Dental Products, Oxnard, CA). One impression was used to fabricate the porcelain veneers and the other was used to confirm their fit and ability to close the gingival areas.
The laboratory was asked to fabricate layered pressed ceramic veneers (IPS Empress®, Ivoclar Vivadent, Inc, Amherst, NY) for teeth Nos. 7 and 10 using shades provided from the spectrophotometer. Photographs of the post-whitening preoperative condition and close-ups of the direct bonded teeth and the prepared teeth would aid the ceramist in fabricating veneers that achieve harmony and balance with the rest of the smile.
At the delivery appointment, the original bonded restorations were evaluated, and only minor modifications were indicated. A high, final polish was then completed. The pressed ceramic veneers were tried in and confirmed to fit, and the patient and her parents gave full approval.
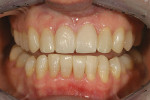
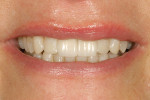
Cementation was accomplished using a total-etch, three-step adhesive and a light-cured luting cement (All-Bond™ 3/Choice™ 2, Bisco, Inc) (Figure 12 and Figure 13). Because the best adhesive bond strengths are attained with three-step, total-etch systems, the author is always striving for the best possible bond strength with enamel or dentin as the substrate. The final outcome was one that delighted both the patient and her parents, while being minimally invasive (Figure 14 and Figure 15).
Case 2
A 30-year-old woman presented with 10-year-old veneers on teeth Nos. 7 and 10 and wanted a new look. She expressed a desire for whiter teeth, with no black triangles between them in her new smile (Figure 16 and Figure 17).
To meet the patient’s expectations conservatively, direct composite “veneers” would be placed on the mesial gingival areas of teeth Nos. 6 and 11 and on the mesial and distal gingival areas of teeth Nos. 8 and 9. After bleaching her dentition, in the same manner as described in Case 1, restorative treatment was begun. The teeth were pumiced to remove the pellicle layer and allow for ideal enamel bonding. A total-etch, one-bottle adhesive system (OptiBond Solo™ plus, Kerr Corp, Orange, CA) was used. A nanofilled composite that, in the author’s opinion, has demonstrated esthetic chroma and opacity characteristics (lite™ Aesthetic Enamel, Bisco, Inc) was layered to replicate the natural tooth structure. Layering of composite accomplished a seamless restoration. When a seamless margin is the goal, the clinician should consider placing a proper bevel when indicated, etching past the bevel, and rolling the outer layer with clean, gloved hands for sculptability and to prevent inclusions or voids. Also, the finishing armamentarium should be rotated from restoration to tooth.9,10
The veneers on teeth Nos. 7 and 10 were removed, and minor preparation modifications were indicated (Figure 18). Impressions, bite registration, photographic images, and a laboratory prescription were sent to the laboratory technician. The ceramist transformed ceramic into an enamel and dentin replacement. Prototype veneers were fabricated using bis-Acrylic (Integrity™, DENTSPLY Caulk, Milford, DE) using a putty matrix from the diagnostic wax-up (Figure 19).
Try-in and cementation occurred as described in Case 1. The final outcome, accomplished with a conservative and minimally invasive approach, mimicked natural tooth structure (Figure 20) and produced a dramatic smile enhancement (Figure 21; Figure 22a; h Figure 22b).
Case 3
A 56-year-old woman presented with 13-year-old veneers on teeth Nos. 8 and 9, as well as an aged, worn dentition (Figure 23 and Figure 24). At the initial appointment, the fractured veneer on tooth No. 9 was patched, which enabled the patient to consider all of her options before making a decision about her comprehensive treatment plan (Figure 25). After discussing the patient’s goal, considering the number of teeth to be treated, analyzing the patient’s occlusal pathology, and taking into account clinical experience and the long-term prognosis of composite veneers vs porcelain veneers, a final decision was made.
The treatment plan consisted of bonding teeth Nos. 6, 7, 10, and 11. Free-hand bonding with a life-like composite (Vit-l-escence®, Ultradent Products, Inc, South Jordan, UT) was initiated using the fractured veneers as a rough guide. The spectrophotometer (VITA Easyshade) confirmed visual and photographic shade taking. The spectrophotometer recorded the canines to be 3M2, the laterals to be 3M1, and the centrals to be 2M1. The laterals were layered using shade A-3, Iri-descence Blue composite, and Shade A-2. This would allow the laterals to be slightly lower in value than the centrals; in general, this is a good guide to follow. The cuspids were built with shade A-3, which would give them the highest chroma. Outline form, embrasure progression, and axial inclination were obtained at the first appointment, along with an initial polish.
The veneers on teeth Nos. 8 and 9 were removed, revealing “aggressive” veneer preparations. Approximately 50% of the preparation was in dentin but an enamel periphery was present. In the past, it was common to put 1-mm depth-cutting grooves directly into the tooth and hope to have an enamel periphery. Today, it is taught differently. By using bis-Acrylic with the putty matrix before touching the tooth, putting the depth-cutting grooves in the bis-Acrylic will guide the clinician on how much tooth preparation needs to be done. Usually, teeth are being built more to the facial and so they are prepared very minimally.
Refinement of the preparations and two final impressions were taken. As in the other cases, a bis-Acrylic prototype was fabricated in coordination with the newly bonded teeth.
After communication with and fabrication of the restorations by the ceramist, the veneers were tried in (Figure 26). Some minor margin and shade discrepancies were noted at 1:1 magnification. Further instructions and photographs helped guide the ceramist to create veneers that would blend with the newly designed dentition (Figure 27 and Figure 28).
At the delivery appointment, after the patient approved the veneers for contour and color, cementation began. The veneers were completely seated, using a total-etch technique (All-Bond 3) and A3 shade composite (Herculite®, Kerr Corp). Porcelain veneer cement is composite resin cement—just a very thinned version of the microhybrid system most of the time. The author uses a thick version of it, which is the original format. Some clinicians like to warm the cement and others thin it with a very small amount of flowable composite or unfilled resin. The one limitation is seating and while one needs to use caution, the author has never had an issue getting them fully seated.
The occlusion was checked in protrusive and right and left working movements. After all occlusal issues were addressed, a high polish was accomplished. Despite living in Hollywood, the patient liked the natural esthetics that were attained for her with the replacement of her 13-year-old cosmetic dentistry and an add-on technique to enhance her smile to the fullest (Figure 29 and Figure 30).
Conclusion
It is time for the dental profession to come to terms with the need to be minimally invasive in its approaches to cosmetic dentistry and restorative treatments. Today’s dentist could learn much from where the profession was in the 1970s. It was a time of additive dentistry, despite very little science to support the techniques and their obvious initial benefits of improved esthetics and conservation of tooth structure. Those early esthetic materials and protocols were not well understood. Now, 30 years later, dentists have an enormous amount of research, material improvements, science, and clinical performance to support and heighten the use of composites and adhesive dentistry wherever and whenever possible.
Composites should be an integral part of every esthetic practice. To cut teeth down for minor tooth shape and size changes to accommodate a ceramic veneer or crown would be gross overtreatment in many instances by today’s more conservative standards. Exceptionally esthetic direct composite restorations require additional clinical, technical, visual, and artistic skills; mastering them enables clinicians to take ownership of the esthetic procedures they perform. Minimally invasive dentistry should not just be words discussed in the literature, but a guiding philosophy for practicing modern esthetic dentists. Giving patients the most conservative, least invasive, and predictable restoration of teeth to normal form and function needs to be every dentist’s goal.
Acknowledgment
The author wishes to thank Hermanson’s/ DTI Dental Laboratories for fabricating the ceramic restorations featured in Case 1, Micro Dental/DTI Laboratory for fabricating the restorations featured in Case 2, and Frontier Dental Laboratory for fabricating the restorations featured in Cases 2 and 3.
References
1. Calamia JR. Clinical evaluation of etched porcelain veneers. Am J Dent. 1989;2(1):9-15.
2. Garber DA. Direct composite veneers versus etched porcelain laminate veneers. Dent Clin North Am. 1989;33(2):301-304.
3. DiMatteo A. Dissecting the debate over the ethics of esthetic dentistry. Inside Dentistry. 2007;3(8):52-64.
4. Maruyama T. Esthetics: occlusion and function. J Esthet Dent. 1994;6(6):295-299.
5. Gresnigt MM, Ozcan M. Fracture strength of direct versus indirect laminates with and without fiber application at the cementation interface. Dent Mater. 2007;23(8): 927-933.
6. LeSage BP. Aesthetic anterior composite restorations: a guide to direct placement. Dent Clin North Am. 2007;51(2):359-378.
7. Yesil ZD, Alapati S, Johnston W, et al. Evaluation of the wear resistance of new nanocomposite resin restorative. J Prosthet Dent. 2008;99(6):435-443.
8. Albers HF. Tooth Colored Restorations: Principles and Techniques. 9th ed. BC Decker Publishing; 2001.
9. Peyton JH. Finishing and polishing techniques: direct composite resin restorations. Pract Proced Aesthet Dent. 2004; 16(4):293-298.
10. Eubank J, LeSage B. Data presented at the UCLA Aesthetic Continuum (composite lecture and hands-on workshops). 19972008; UCLA Dental School, Los Angeles, CA.
About the Author
Brian LeSage, DDS
Private Practice
Beverly Hills, California
Director
UCLA Aesthetic Continuum
Los Angeles, California
Director
Beverly Hills Institute of Dental Esthetics
Beverly Hills, California