A Case Study: A Custom Posterior Abutment Compared with a Prefabricated Stock Abutment
Larry R. Holt, DDS
A great deal has been written about peri-implant soft-tissue morphology.1,2 Much of the literature is focused on the critical esthetic zone.3-5 Contemporary implant–restorative techniques provide very natural esthetics with tissue architecture that rivals nature. Normal emergence profiles and clinical crown contours can be predictably delivered.6 It is the premise of this article that these same techniques can be used outside the esthetic zone to provide similar results, and that these same results are desirable. This article explores the value of custom posterior implant abutments and evaluates their ability to simulate natural esthetics and tooth morphology.7
Several manufacturers, such as Astra Tech (Waltham MA), Nobel Biocare USA, LLC (Yorba Linda, CA), and Biomet 3i (Palm Beach Gardens, FL), provide computer-aided design/computer-aided manufacture (CAD/CAM) custom implant abutments. Computer-aided optical scanning of models provides a virtual 3-dimensional model upon which an ideal abutment can be designed. After they are designed, these abutments are computer-milled from titanium or zirconia. These abutments are very accurate and provide ideal transmucosal anatomy. They have ideal retentive form and correct occlusal clearance. The clinical technique for placing these abutments is simple and straightforward.
Prefabricated abutments also are readily available from multiple manufacturers, including Astra Tech, Nobel Biocare USA, and Biomet 3i. They are available in various sizes, angulations, and materials. Some contemporary abutments are available with semi-anatomic emergence profiles. Many lecturers (and manufacturers) promote prefabricated abutments as a cost-saving, convenient approach to providing implant-borne restorations. These abutments can be inserted with an easily understood clinical technique that is similar to conventional crown-and-bridge treatment.7 These abutments can be modified chairside or by a laboratory technician.
The posterior region of the mouth is often treated with less emphasis on soft tissue profiles and esthetics. For this reason, prefabricated abutments are often used in the posterior. These abutments are typically non-anatomic with flat, cylindrical emergence profiles. They provide little lateral soft tissue support or tissue shaping (Figure 1). The overall shape of these abutments is similar to the natural anatomy of mandibular premolars.8 Unfortunately, these abutments share little similarity to the natural anatomy of any other posterior tooth, particularly molars.
Clinical Protocol
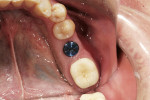
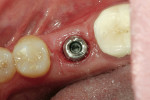
This simple study was designed to compare a stock abutment and its crown with a custom-fabricated abutment and its associated crown. The patient originally presented with a missing tooth, No. 19. The surrounding teeth were deemed healthy with good periodontal support. The edentulous ridge had an adequate volume of bone to support an implant. A Nobel-Replace® Select 5.0 implant (Nobel Biocare USA) was placed uneventfully. The implant was allowed to osseointegrate for 4 months (Figure 2).
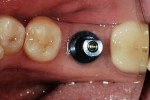
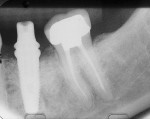
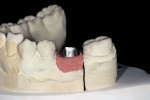
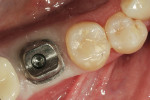
On the day of restorative treatment, the healing cap was removed and an impression coping was seated on the implant (Figure 3). A radiograph was taken to confirm seating of the impression coping (Figure 4). A polyether impression was made using a closed-tray technique. The impression was sent to the laboratory along with interocclusal bite records, an articulator-mounted opposing model, photographs, and a written prescription. This appointment was accomplished without local anesthesia and took approximately 30 minutes.
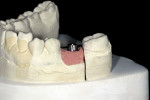
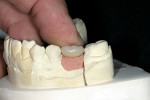
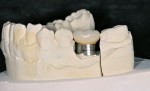
The laboratory developed an appropriate working model with a laboratory analogue and soft-tissue simulation. A stock 5-mm esthetic abutment with a 3-mm collar height (NobelReplace® Select Abut-ment, Nobel Biocare USA) was modified and fitted to the model (Figure 5). A porcelain-fused-to-metal (PFM) crown was then fabricated to fit the stock abutment (Figure 6). Although not done in this case, a practitioner could have easily fitted the abutment in the mouth and made a conventional impression.
The laboratory also developed a custom-abutment work order for an Atlantis™ abutment (Astra Tech). The work order specified an ideal emergence profile that would produce tissue blanching at delivery. The custom titanium abutment design included a 1-mm subgingival facial depth, 0.75-mm mesial and distal depths, and the lingual margin at the crest of tissue.9 The working model with mounted opposing model was sent along with the work order. Astra Tech, using CAD/CAM technology, designed and fabricated a custom titanium abutment (Figure 7). The abutment was returned to the laboratory (Figure 8), where an appropriate PFM crown was fabricated (Figure 9).
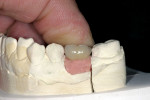
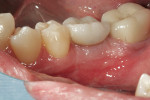
Both sets of restorations and abutments were returned to the dental office. All laboratory work was documented with pre-insertion photography. The stock pre-fabricated abutment was tried in first (Figure 10). The crown was fitted to the abutment in the mouth after slight adjustment of interproximal contacts. The occlusion was modified slightly. The crown was “tacked” in place with a small amount of temporary cement (Figure 11). The patient was allowed 20 minutes to evaluate the crown. She was encouraged to “explore” the new crown visually and by tactile sensation to her tongue. Patient comments were recorded. The prefabricated abutment was then removed.
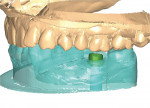
Next, the custom abutment was placed (Figure 12). After a 10-minute period for tissue blanching to resolve, the PFM crown was tried in and modified slightly to accommodate interproximal contacts and occlusion. The patient was again given the opportunity to “explore” the restoration. Patient comments were recorded. The patient was then given the choice as to which restoration she would prefer to have placed in her mouth.
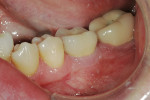
The patient preferred the custom abutment and crown. “It looks and feels more natural in my mouth,” was her statement. The Atlantis abutment was torqued to place (35 Ncm), and the crown was seated with temporary cement. Care was taken to en-sure removal of all excess cement. Occlusion was evaluated and adjusted slightly. The patient was asked to return for a 1-month post-delivery evaluation. Final seated photographs were taken (Figure 13).
Clinical Observations
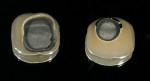
Inspection of the laboratory work revealed the custom abutment and crown to be more consistent with natural anatomy. On direct comparison of the intaglio surface of each crown (Figure 14), the stock abutment lacked natural contours. The narrow, cylindrical shape of the stock abutment forces the crown to appear like a mushroom cap on its stem (Figure 15). Clinically, this relationship creates an undercut area in the embrasures that resembles a pontic. In fact, the crown has artificially created facial and lingual embrasures. These areas can certainly be maintained, but not with the ease of simple flossing.
Discussion
Under the simple, anecdotal nature of this case study, it was observed that the custom abutment and its final restoration were more “anatomically correct.” The patient enthusiastically chose the custom crown and abutment over the stock abutment with crown. Her decision was based on the fact that the custom restoration felt more natural to her tongue. Dentists often forget this critical parameter for treatment success. On subsequent follow-up visits, the patient reported her continuing satisfaction: “It feels just like my other teeth.” This is the ultimate compliment to the laboratory and to the dentist. She has reported no difficulty in performing appropriate hygiene techniques. No food trapping or other problems were reported. It is readily apparent that the custom abutment provides normal papillary architecture with no open gingival embrasures.
Based on this case study, it is the conclusion of this author that a custom abutment is a desirable choice in the posterior region of the mouth, particularly for molar replacement. Normal anatomic morphology can be re-created, which provides a more satisfying patient experience. The clinical protocol for this technique is simple and easily implemented.10
Acknowledgment
Special thanks to Mark Stueck, CDT, of Drake Precision Dental Laboratory whose meticulous attention to detail allowed this case to be a success.
References
1. Salama H, Salama M, Garber D, et al. The interproximal height of bone: a guidepost to predictable aesthetic strategies and soft tissue contours in anterior tooth replacement. Pract Periodontics Aesthet Dent. 1998;10(9):1131-1142.
2. Lindhe J, Berglundh T. The interface between the mucosa and the implant. Periodontol 2000. 1998;17:47-54.
3. Sadan A, Blatz M, Bellerino M, et al. Prosthetic design considerations for anterior single-implant restorations. J Esthet Restor Dent. 2004;16(3):165-175.
4. Zetu L, Wang HL. Management of inter-dental/inter-implant papilla. J Clin Periodontol. 2005;32(7):831-839.
5. Potashnick SR. Soft tissue modeling for the esthetic single-tooth implant restoration. J Esth Dent. 1998;10(3):121-131.
6. Smuckler H, Castellucci F, Capri D. The role of the implant housing in obtaining aesthetics: part 2. Customizing the peri-implant soft tissue. Pract Proced Aesthet Dent. 2003;15(6):487-492.
7. Kerstein RB, Castellucci F, Osorio J. Ideal gingival form with computer-generated permanent healing abutments. Compend Contin Educ Dent. 2000;21(10): 793-802.
8. The permanent mandibular premolars. In: Wheeler RC. Dental Anatomy, Physiology and Occlusion. 5th ed. Philadelphia, PA: W.B. Saunders Company; 1974:216-236.
9. Chee W, Jivraj S. Designing abutments for cement retained implant supported restorations. Br Dent J. 2006;201(9):559-563.
10. Garg AK. The Atlantis Components Abutment: simplifying the tooth implant procedure. Dental Implantol Update. 2003;13(9):65-70.
About the Author
Larry R. Holt, DDS
Private Practice
Hickory, North Carolina
Adjunct Associate Professor, University of North Carolina
School of Dentistry
Chapel Hill, North Carolina