Dental Operating Microscopes: Don’t Equip an Operatory Without One!
With the exception of dental chairs, units, handpieces, and other essential equipment needed in a dental office to treat patients, there is currently no other equipment or technology the author currently owns that is as invaluable as a microscope. Other technologies are useful, such as CAD/CAM systems and various lasers, but the fact of the matter is that the author could still practice dentistry without them. Crowns could still be fabricated by a dental laboratory, and patients with periodontal disease could still be referred to a periodontist. Technologies such as CAD/CAM and lasers offer another means or modality in the way treatment is performed. A microscope, however, does not change the means or modality; it simply enhances them pre-, intra-, and postoperatively regardless of the actual procedural methods used. When it comes to successfully integrating other technologies, microscopes can be an invaluable asset in not only streamlining the time required to successfully integrate such technologies, but also in enhancing the precision, efficiency, and effectiveness of numerous other procedures as well, including a simple oral examination.
The value of magnification is becoming more apparent. Many dentists have adopted and use some form of magnification, such as loupes, and more dental schools are now requiring that students use them as well. Magnification helps the user to see not only more, but to see better because of the improved illumination. The more one is able to see, the better able he or she is to diagnose problems more effectively and treat more precisely.
When one considers that the size of the structures dentists are trying to treat are most commonly measured in millimeters, and that the focus of treatment in all areas of surgery seems to be gravitating more and more toward doing more conservative procedures in order to preserve and protect healthy tissues, no surgeon (regardless of specialty) should be performing procedures without using some form of magnification. Therefore, in the author’s opinion, 2.5x to 3.5x telescopic loupes should be a minimum requirement for all dental practitioners, including hygienists.
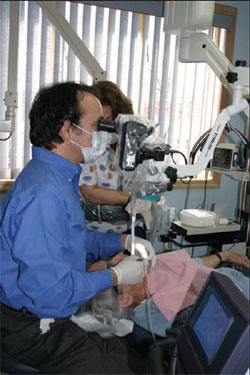
Microscopes, however, offer the user several distinct advantages over loupes, primarily in the area of ergonomics. Microscopes not only enable the user to see more and better than loupes, but do so in an extremely ergonomic fashion by forcing the user to sit in a comfortable, upright position (Figure 1). Improved ergonomics results in increased operator efficiency by enabling the operator to practice for longer periods of time, allowing for more dentistry to be completed in fewer visits. This is not only advantageous to the dentist from a productivity and profitability standpoint but, more importantly, to the patient from a convenience and benefit standpoint. In addition to ergonomics, microscopes offer three more advantages over loupes that, ultimately, also affect ergonomic factors: unobstructed coaxial illumination; multiple levels of magnification; and the ability to integrate video and digital devices.
UNOBSTRUCTED COAXIAL ILLUMINATION
Unobstructed coaxial illumination (UCI) means illumination without shadows. Dentists are all familiar with the shadows cast by various parts of our bodies and even hand instruments while using an overhead lamp. The reason why this occurs is because of the different paths of the operator’s vision in respect to the path of illumination.
Attaching a light source directly to a set of loupes or head gear makes illumination better in that its path can be better aligned with the visual path. However, unless the head and neck are adjusted to accommodate both the path of illumination and ocular focal length, which is set at a fixed distance, illumination may not always be unobstructed, especially when a mirror is introduced. The compensating anatomical positions the user must make to align the paths of vision and illumination while maintaining a fixed focal distance away from the target can sometimes be challenging and strenuous. One must also consider the additional strain that the weight of the equipment itself would exert on the musculoskeletal system. The light source from a microscope, however, is totally unobstructed because the light is emitted directly through the objective lens itself. This means that the operator’s visual path is traveling in the same exact direction as the path of illumination. With true UCI, even hard-to-access areas, such as the distals of terminal molars (Figure 2), can be easily visualized without any shadows while good posture is maintainted because no additional weight or wires are added to one’s head.
MULTIPLE LEVELS OF MAGNIFICATION AVAILABLE AT YOUR FINGERTIPS
Various procedures and even various steps of the same procedure often require different degrees of magnification at different times. For instance, higher levels of magnification may be useful in locating an accessory or calcified endodontic canal but may not be appropriate or even practical once the canal is located. Higher levels of magnification may be useful in refining the margins of crown preparations while causing minimal trauma to soft tissues but may not be useful in evaluating the overall taper of the preparations. Microscopes give the user the ability to instantly change levels of magnification without changing loupes or, in some cases, even having to reorient the light gear.
ABILITY TO INTEGRATE VIDEO AND DIGITAL DEVICES
Magnification can improve the operator's diagnostic capability (Figure 1), but this alone may not be sufficient to convince patients of the urgency and need to treat a problem in the earlier stages, especially if the patient is not experiencing any obvious symptoms. With a video-enabled microscope, limitations frequently encountered when trying to communicate and educate are virtually eliminated once the visual information obtained and observed by the operator can be shared with the patient. Having the ability to share such information with patients will have a significant impact on the rate of case acceptance. While increased case acceptance is good for the dentist, it is especially good for the patient because it may help to prevent an emergency situation as well as reduce overall treatment costs by eliminating the need for additional procedures that could result if the problem is left untreated until the patient develops symptoms. Furthermore, having the ability to easily and efficiently obtain images pre-, intra- and postoperatively is invaluable to the doctor from a medical-legal standpoint, as well as contributing to ease of documentation. This also results in improved ergonomics and greater efficiency for the operator.
OTHER ADVANTAGES
To a non-user, the most obvious disadvantages of microscopes may appear to be the cost and amount of time needed to fully integrate them, but the obstacles are not as high as many would think.
Figure 3 (View Figure)
By helping patients literally see the importance of treating things sooner than later (or many times not at all), and by providing treatment with greater efficiency and precision, it is easy to see how the microscope can be an excellent return on investment. Simply put, you cannot detect what you cannot see, and if the patient cannot see it, they often will not allow you to treat it. And if they do allow you to treat something, and a complication should arise during treatment, some patients will be quick to place blame on the operator for convincing them to treat something that, from an asymptomatic patient’s perspective, would have been better off left untreated.
Although the time required to properly integrate microscopes into the practice can take up to 3 to 6 months for some users, this time period can be significantly reduced to a matter of weeks with formal training. But when one truly considers all of the advantages and benefits that microscopes offer to the doctor and patient, the author firmly believes that no operatory should be equipped without one. You really need to use them to discover and “see” all the advantages for yourself.
This article was written by Donato Napoletano, DMD, who owns a private practice in Middletown, New York. He is also a technology integration consultant for Donato Dental Systems, also in Middletown.
For more information, contact:
Global Surgical Corporation
Phone: 636-861-3388
Web: www.globalsurgical.com/dental
DISCLAIMER
The preceding material was provided by the manufacturer. The statements and opinions contained therein are solely those of the manufacturer and not of the editors, publisher, or the Editorial Board of Inside Dentistry. The preceding is not a warranty, endorsement, or approval for the aforementioned products or services or their effectiveness, quality, or safety on the part of Inside Dentistry or AEGIS Communications. The publisher disclaims responsibility for any injury to persons or property resulting from any ideas or products referred to in the preceding material.
 | 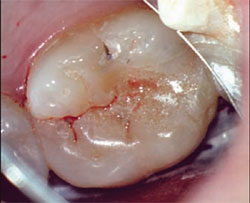 | |
| Figure 2 Distal to mesial fracture. | ||
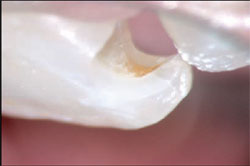 | ||
| Figure 1 The author sits comfortably comfortably at his microscope in Middletown, NY. | Figure 3 Decay hiding in an area difficult to visualize; inspection also revealed microfractures in the enamel toward the incisal edge. |



