Cercon® Art: A New CAD/CAM System for Esthetic All-Ceramics
Stephen Poss, DDS
Many high-strength ceramic systems have recently emerged on the dental market. Of these, DENTSPLY Ceramco’s (York, PA) Cercon® zirconia has proven its durability and esthetics to the dental community since 1998.1 The recent launch of Cercon® Art has now made the predictability of a precision fit available to dental laboratories.2
Cercon, which is used for a wide variety of restorations—from single units to long-span bridges—has added Cercon Art, which is a new computer-aided design/computer-aided manufacturing (CAD/CAM) module for the Cercon system. Cercon Art delivers a consistently improved and predictable fit to dentists and their patients. To the clinician, this CAD/CAM system can also deliver excellent esthetics, as the case studies here will demonstrate.
Cercon Art CAD/CAM in Your Dental Laboratory
Cercon zirconia is an excellent material choice for metal-free restorations because of its biocompatibility, strength, and durability.3,4 It has been proven in clinical studies for more than 8 years. The news about the durability of this material is very promising. Research shows in vitro performance equivalent to porcelain-fused-to-metal (PFM) restorations.5 A new study of subcritical crack growth in Cercon zirconia predicts a possible 20-year lifetime for the material.6
The challenge with processing zirconia in a dental laboratory is controlling shrinkage. Until recently, dental technicians have had to create a wax model of a restoration to be scanned by the precision laser of the Cercon system. The general fit of the restorations was acceptable, and in the range of PFM restorations.7 However, this was still a labor issue for laboratories in a time of skilled labor shortages.
The recent development of Cercon Art CAD/CAM has brought automated and repeatable predictability and computer precision to the process. The Cercon Art program is intuitive and allows for the fabrication of copings customized for cement gaps, wall thickness, and occlusal geometry. This technology offers the dental laboratory a cost-effective means to fabricate single units without resorting to outsourcing. This also represents a significant time savings for the dental laboratory vs the hand-wax coping method because there are no interferences or tight fits that have to be hand-finished by the technician.
The fit of Cercon restorations is in the 40-µm ± 35-µm range.8 The CAD program reduces the effect of human variability, which allows for more consistency from the dental laboratory. What is of particular interest to this author is that the Cercon Art CAD will allow the cement gap to be adjusted to between 10 µm and 60 µm. A spacer parameter extends the cement gap up to 90% of the surface area. The cement gap is set to a default of 50 µm. You can now seat a relatively passive-fit restoration or a precision-tight restoration, depending on your choice. As always, communicating your preferences to your dental laboratory is indispensable in getting the results you want.
Case 1
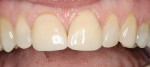
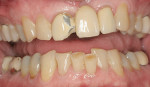
A 54-year-old woman presented with two failing crowns on her central incisors. She also thought her central incisors were too wide and was dissatisfied with proportions as well (Figure 1). There are a variety of esthetic materials that could have been used in this case, especially in a lower stress anterior situation. The author wanted to evaluate not only the fit but the esthetic potential of Cercon and the Ceramco® PFZ layering porcelain (DENTSPLY/Ceramco).
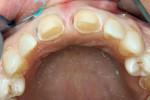
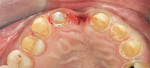
The older feldspathic material was removed from the two central incisors. A conservative 1-mm marginal and facial finish was prepared for the Cercon and the Ceramco PFZ layering porcelain (Figure 2 and Figure 3). A polyvinyl impression material, Aquasil (DENTSPLY/Caulk, Milford, DE), was used to take the impression. The bis-Acryl provisionals were made with Integrity™ (DENTSPLY/Caulk).
The Cercon Art CAD/CAM system was used to scan the die for both central incisors (Figure 4). This will ensure an adequate marginal fit with Cercon zirconia. The predetermined coping thickness of 0.4 mm appears to be an optimal balance between strength and translucency.
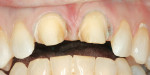
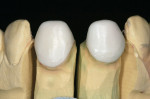
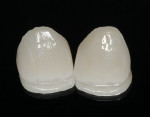
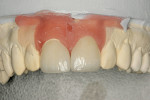
The completed restorations were inspected on the dies before placement. The patient was anesthetized and the provisionals were removed. The author prefers to evaluate the esthetics both on a neutral black background and on a die model incorporating gingival simulation (Figure 5 and Figure 6).
After verifying the fit, the interior aspect of the Cercon was microetched by the laboratory with 50-µm aluminum oxide at 2 to 3 bars. This creates micro-mechanical retention for the luting cement. The teeth were scrubbed with chlorhexidine and rinsed. The teeth were then treated with phosphoric acid for 15 seconds and rinsed. A generous coat of Prime & Bond® NT™ (DENTSPLY/Caulk) was placed on the prepared teeth, lightly air-dried, and cured for 10 seconds.
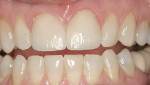
Calibra® Luting Cement (DENTSPLY/Caulk) was placed in each crown and placed firmly on the teeth. The gingival margins of each crown were tacked to place for approximately 3 seconds. The teeth were carefully flossed followed by a complete cure of 40 seconds on the facial and 40 seconds on the lingual. The excess cement was cleaned off with a scaler and the margins were polished with an Enhance® cup (DENTSPLY/Caulk) (Figure 7). The patient was instructed in home care and dismissed.
Case 2
A 48-year-old man presented with a PFM bridge on teeth Nos. 8 through 10 with a broken abutment on tooth No. 8. Part of the veneering porcelain had sheared away, exposing the metal core. There was interproximal decay on teeth Nos. 5, 6, and 11 with extensive wear on the opposing dentition because of a poorly fitted bridge (Figure 8).
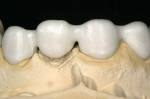
Cercon zirconia is a good choice for an anterior bridge because the connector size required is significantly smaller (3 mm x 3 mm) than that of competing lithium disilicate options (5 mm x 4 mm). The reduced connector size allows for a more natural-looking bridge. Teeth Nos. 5 through 12 were prepared with the bridge extending from teeth Nos. 8 through 11. Teeth Nos. 5 through 7 and 12 were single units (Figure 9). Tooth reductions were about 1 mm axial and 1.6 mm occlusal, comparable to those in the first case.
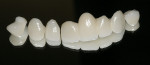
Cercon Art was used to achieve a more accurate fit (Figure 10) for the single units. The patient requested a lighter shade for his restoration with plans to restore the worn lower teeth after the upper Cercon bridge was complete. Ceramco’s PFZ porcelain was veneered to the Cercon copings to achieve a lighter (B2) but still natural shade (Figure 11).
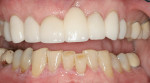
After removing the provisionals, the fit and esthetics were verified. The internal aspects of the Cercon restorations were blasted with aluminum oxide and the cementation protocol was the same as in Case 1 (Figure 12).
Discussion
The Cercon zirconia system has opened up new avenues of restorative possibilities for the clinician. This system provides extraordinary strength and beauty with the capability of providing long-span, metal-free bridges as well as single crowns. The addition of Cercon Art, with its consistency of fit, has reduced some of the stresses associated with fabrication and fit issues for the dental technician.
References
1. Sturzenegger B, Feher A, Luthy H, et al. Clinical study of zirconium oxide bridges in the posterior segments fabricated with the DCM system. Schweiz Monatsschr Zahnmed. 2000;110(12): 131-139.
2. von Schroeter P, Jurgensen B, Zollner M. Cercon move—a navigation aid for dental CAD applications. Int J Comput Dent. 2004;7(4): 371-377.
3. Piconi C, Maccauro G. Zirconia as a ceramic biomaterial. Biomaterials. 1999;20(1):1-25.
4. Filser F, Kocher P, Weibel F, et al. Reliability and strength of all-ceramic dental restorations fabricated by direct ceramic machining (DCM). Int J Comput Dent. 2001;4(2):89-106.
5. Kilicarslan MA, Kedici PS, Kucukesmen HC, et al. In vitro fracture resistance of posterior metal-ceramic and all-ceramic inlay-retained resin-bonded fixed partial dentures. J Prosthet Dent. 2004;92(4):365-370.
6. Studart AR, Filser F, Kocher P, et al. Cyclic fatigue in water of veneer-framework composites for all-ceramic dental bridges. Dent Mater. 2006;8(3):653-678.
7. Ariko K. Evaluation of the marginal fitness of tetragonal zirconia polycrystal all-ceramic restorations. Kokubyo Gakkai Zasshi. 2003;70(2):114-123.
8. Piwowarczyk A, Lauer HC. Determining the marginal fit of CAD/CAM bridge frameworks. Proc PEF. 2006; Abstract #254.
About the Author
Stephen Poss, DDS
Clinical Director
Center for Exceptional Practices
Garfield Heights, Ohio