A Clinical Investigation of the Rescue™ Internal Implant
Hoda Yousef, DMD, MS; Mark Khaimov, DMD; and Saul Weiner, DDS
Abstract
INTRODUCTION: Immediate implant placements in molar sites have been problematic. This report describes the use of a novel dental implant placed immediately in first and second molar sites. METHODS: Implants were inserted for 19 patients in molar sites immediately after tooth extraction. Patients were followed for 1 year post-insertion, with radiographs obtained and periodontal parameters recorded every 6 months. RESULTS: The implant success rate was 95.24%. Esthetics generally was acceptable in the posterior quadrants. Crestal bone die-back in most cases only extended to the crest of the implant. The periodontal parameters recorded at the 6- and 12-month recalls were consistent with periodontal health. CONCLUSIONS: Use of this novel implant system can be successful if the guidelines for its use are followed. It is best utilized by experienced implantologists.
Implants have become a standard approach to the rehabilitation of missing teeth. In addition, immediate placement of implants has also become a predictable approach that minimizes treatment time and facilitates patient management. However, this approach requires careful evaluation of bone quality and quantity as well as the soft-tissue biotype. Implants immediately placed into extraction sockets have been shown to have high survival rates, similar to those placed in healed sites. The immediate-placement implants provide significant advantages of fewer surgical procedures, shorter treatment time, and the facilitation of improved esthetics.1
A key to successful immediate surgical protocols is primary stability of the implant.2 Frequently, the walls of the tooth socket can provide support and stability to the implant.3 Most implant systems provide diameters ranging from 3 mm to 6 mm. For most anterior and premolar sites, available implant sizes allow the socket to contribute to primary stability of the implant. It is for this reason that immediate implants have principally been placed on anterior teeth and premolars. Molar tooth sizes exceed that of most current implant diameters and, therefore, immediate placements have been limited due to the difficulty of achieving primary stability with conventional implants.
The space between the implant and socket wall in the molar area has been an issue with regard to achieving osseointegration. Studies have shown that close adaptation of the implant to the socket wall promotes osseointegration.3,4 In those areas where a wide space of 3 mm or more exists from the implant to the socket wall, better bone healing has been achieved with some intervention, including the use of a bone graft to fill the gap and/or an occlusive membrane to prevent epithelial migration into the space between the implant and the socket wall.5 Typically, in a single-stage, immediate-placement protocol, the implant extends adjacent to the crestal bone, and a healing cap or custom-healing component provides support to the soft tissue adjacent to the socket.6 However, when a significant gap exists between the implant and the socket, there is concern regarding epithelial downgrowth along the side of the implant.
The placement of an implant of maximum length was especially significant when implants presented with a machined surface. The most common way to increase the surface area available was by placing a longer implant. Longer implants were associated with higher success rates,7 but the posterior region presents several complicating factors. These include interarch space considerations and structures such as the inferior alveolar nerve and a pneumatized maxillary sinus. Implants in these regions often require additional procedures such as sinus lifts and grafting. As a result of post-extraction resorption leading to extensive tissue loss over time, the treatment becomes more complex. However, today the use of shorter and wider implants with a higher crown-to-root ratio are an alternative approach for the posterior regions.8
The implant-supported restoration with long machined fixtures has maintained a crown-to-implant ratio of 1:1.8 However, in the posterior maxilla and mandible, natural resorption of the alveolar ridge, which occurs as a result of prolonged edentulism, can result in an enlarged interarch distance. With the consequent limited available bone, short implants become an option.9 This, however, can lead to a less desirable crown-to-implant ratio of 2:1 or greater. Improvements that have been made to surfaces and implant systems, along with prosthetic occlusal adjustments, make such restorations successful under certain circumstances.9-11 Tawil found no significant difference in marginal bone loss that could be correlated with the crown-to-implant ratio in short implants placed.12 He concluded that when the load distribution was favorable, increased crown-to-implant ratios were not a major risk factor. The study indicated that short implants are viable solutions in areas with reduced bone height. Even when prosthetic parameters exceeded the normal values, when the force orientation and load distribution were favorable—ie, in the long axis of the implant—and parafunction was controlled, short implants were successful.
Clinical reports have employed a number of strategies to manage implants in molar sites.9 These include grafting, placement of two smaller-diameter implants, or selection of one regular implant, which can be placed to restore the site. The placement of one implant, however, may result in a restoration that does not fill the complete edentulous space or may be cantilevered. A more recent approach is the use of wide-diameter implants that approximate the size of the tooth socket. However, because of their taper, many of the wide-body implants currently available do not adapt well after insertion into the extracted socket, resulting in a lack of primary stability, a key to the success of osseointegration. Primary stability is obtained from frictional adaptation of the implant to the walls of the tooth socket.13 Traditionally, extraction sites have been grafted and subsequently implanted. This two-stage process can take anywhere from 3 to 6 months time. Immediate placement reduces the treatment time. However, there is no definitive data reporting the degree of implant survival in immediate grafted sites.14
The purpose of this clinical trial was to evaluate the use of a novel implant system that is immediately placed in an extracted molar tooth socket.
Methods
The study was a case series. Patients were treated between September 2008 and November 2010 at University of Medicine and Dentistry of New Jersey in Newark, New Jersey. The protocol for this study was approved by the Institutional Review Board, Newark Campus of the University of Medicine and Dentistry of New Jersey. Twenty patients were to be selected for this study in whom a molar with a nonrestorable prognosis was to be extracted, followed by immediate placement of a MegaGen Rescue™ implant (MegaGen International, www.megagen.us) as a one-stage procedure.
Patients for the study were selected based on the following series of criteria. They were required to be free of systemic disease for which medication was used. Smokers of more than 10 cigarettes a day, pregnant women, and children under 18 were excluded, as were individuals above 75 years of age. Teeth adjacent to the implant site could not have more than 20% attachment loss or defective restorations. Teeth with Class II or Class III furcations, teeth with loss of buccal osseous plate, and teeth with caries extending below the alveolar crest were not selected as sites for implant placement.
Teeth identified for extractions were evaluated radiographically and examined with a periodontal probe. Teeth with pocket depths greater than 5 mm, periapical radiolucencies greater than 5 mm in size, Class II or Class III furcations, and active suppuration were excluded, as were patients in acute pain.
Implant Design
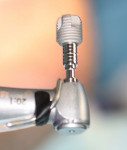
The MegaGen Rescue is a parallel-walled implant with threads to the crest of the implant. It has a resorbable blast medium (RBM) hydroxylapatite treated surface. The thread pitch (0.8 mm) is narrowed to compensate for its reduced dimension; heights range from 5 mm to 11.5 mm and diameters range from 6 mm to 8 mm. It is designed to engage the walls of the edentulous socket for primary stability. The prosthetic design is platform-switched. The neck of the abutment is 4 mm in diameter, and the screw is quite robust, with a diameter of 2.5 mm. The torque value for tightening the screw is 45 Ncm.
Implant Surgery, Restoration, and Loading
Implant placement for all study participants was performed by the same surgeon. Implants were inserted in a one-stage procedure with placement of a healing abutment. The molar tooth was decoronated and the roots were separated and removed individually with periotomes and elevators. Following extraction, a trephine was used in the center of the socket to remove the interradicular septum to the depth of the osteotomy. The osseous core was removed and the osteotomy was enlarged to the size of the implant at 900 RPM and then thoroughly curetted.
The implant was inserted with a hand torque wrench. If dehiscense or perforation of the buccal plate occurred, the procedure was halted and the site socket preserved. After implant placement, the areas around the implant were filled with a combination autogenous bone (from the septal bone trephined from the socket) and alloplastic tricalcium phosphate (TCP) material, a healing abutment was placed, and, if needed, interproximal sutures were placed. No attempt was made to raise either buccal or lingual flaps.
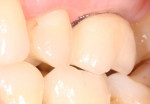
Four months after placement, the healing abutment was removed and a closed-tray impression obtained. A screw-retained metal ceramic crown using a 50% gold alloy was made, evaluated intraorally in the bisque stage, contoured, and the occlusion adjusted. After glazing and polishing, the crown was inserted.
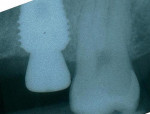
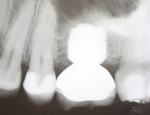
Radiographs using a standardized holder were taken at the time of implant insertion, at the time of crown insertion, 6 months after crown insertion, and 1 year after crown insertion.
Protocol
The implants were inserted 1.5 mm below the level of the crestal bone, as per the MegaGen Rescue recommended protocol. In most circumstances, this was achieved; but because clinically the crestal bone was not uniform around the tooth, there were areas where this was not possible. It is not surprising that under these circumstances, die-back of the bone occurred. Significantly, in most circumstances, this die-back was greatest in the cases that were most subcrestal. When the 1.5-mm placement could not be achieved, in most circumstances, the die-back was less. The stability of the crestal bone may also have been influenced by the ease of removal of the tooth. While in most circumstances, the teeth were readily removed, at times it was difficult to remove the residual root structure. The difficulty of extraction varied depending upon the status of the tooth. Some endodontically involved teeth were difficult to remove. Nevertheless, because these were immediate placements and the teeth had a hopeless prognosis, the extractions may have had some negative effects on the peri-implant bone, which may have affected the healing of the sites.
Post-insertion, patients were prescribed amoxicillin 500 mg, three times daily, for 1 week starting the day of surgery. Chlorhexidine 0.12% rinses were prescribed twice daily for 2 weeks. The patient was seen at 1 week and 2 weeks postsurgery, with suture removal if needed. In the event of a problem, patients were seen immediately.
After the crowns were inserted, patients were subsequently seen at 1 and 2 weeks. At these visits, occlusion was checked, the stability of the abutment was confirmed, and a standardized periapical radiograph was obtained. Each patient was seen again at 6 months and 12 months post-insertion, at which time the standardized periapical radiograph was repeated. Periodontal parameters of pocket depth, gingival index, and plaque index were recorded at these time intervals.15
Data Collection and Statistical Analysis
The periapical radiographs were scanned and digitized. A software package was used to measure changes in crestal bone height. The top of the implant was used as the reference point for all bony crest measurements, which were made of the crestal bone height relative to the top of the implant. The mesial and distal surfaces were treated separately but were then combined for a larger sample size because their mean values did not differ significantly. The periodontal parameters were recorded at 6 months and at 12 months after crown insertion.
For the crestal bone analysis, means and standard deviations were calculated separately for all 20 implants for the mesial and distal surfaces during patient visits at each of the four time intervals—implant insertion, restoration, 6 months post-restorations, and 12 months post-restorations.
Results
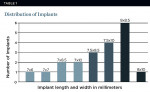
Nineteen patients were accepted into the study, and 21 implants were inserted and restored. One implant failed 2 weeks after insertion in a patient who was not compliant with the postoperative instructions. This left 20 implants in 18 patients among the sample population, making the success rate 95.24%. There were seven male patients and 11 female patients. The average age of the male patients was 52.7 years, and that of the female patients was 46.7 years. Four implants were inserted in the maxilla and 16 in the mandible. Thirteen implants were placed in first molar sites with proximal teeth both mesial and distal. Seven were placed in second molar sites without any distal adjacent tooth. Eight of the implants had an 8-mm diameter and 12 had a 7-mm or 7.5-mm diameter. The length of the implants varied from 6 mm to 10 mm (Table 1).
Crestal Bone Levels
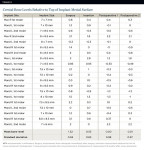
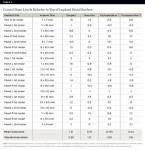
The implants were inserted immediately after extraction of the tooth and thorough curettage of the socket. As per the protocol, the implants were placed approximately 1.5 mm below the crestal bone. The mean subcrestal depth was 1.3 mm on the mesial and 1.4 mm on the distal. Bone remodeling did occur, and at the time of the second evaluation, the mean bony crestal levels were essentially at the level of the top of the implant. At the 12-month interval the mean die-back for the mesial surface was 1.31 mm. The die-back along the distal surface was 1.17 mm (Table 2 and Table 3).
Periodontal Parameters
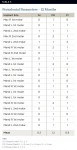
The gingival index, plaque index, and pocket depths were calculated for both the first and second recalls. They were stable and consistent with gingival health (Table 4 and Table 5).
Discussion
The purpose of the study was to observe the survival rate, experiences, and complication rates of a novel implant system that has been said to be effective in the immediate replacement of nonrestorable molars with an implant.
There has been significant discussion in the literature of the relative importance of implant diameter versus length to implant survival and the maintenance of crestal bone. The more recent reports—particularly finite element analyses—have suggested that an increased implant diameter reduces stress on the adjacent crestal bone and is more significant in providing initial stability,16,17 which is necessary to allow bone to osseointegrate adjacent to the implant.18 From a practical perspective, it permits stability for the implant without threatening vital structures such as the mandibular nerve and the maxillary sinus.
Use of the surgical protocol recommended by the manufacturer—a trephine followed by a drill—allowed the establishment of primary stability for the implant. Furthermore, while this system does not have a collar at the top of the implant, this does not appear to pose a problem with regard to bone healing around the implant. With the exception of one implant, all of the implants osseointegrated, with a survival rate of 95.24%.
It has previously been perceived that placement of implants at sites where periapical infections were previously present is contraindicated.19 Recently, it has been reported that careful management of these sites with removal of active infection can allow predictable osseointegration.20 This study confirms these results; the implants healed without any radiolucence or pathology.
Implant stability resulted from engagement of the buccal and lingual residual walls of the socket. Frequently, there were gaps between the mesial and distal walls of the tooth socket and the threads of the implants. When these were larger than 3 mm, they were filled with the previously mentioned combination autogenous and alloplastic TCP material. Based upon the probing depth recorded at the time of the recall visit, osseointegration occurred and the bone healed up against the implant surfaces. A number of case series and clinical reports have reported this observation, which was seen in the authors' case series.21
Replacement of a molar with an immediate implant has been a subject of some debate. If the tooth is removed and the site socket is preserved with an implant subsequently inserted, it is possible to place a larger-diameter implant centered in the edentulous site. Centering the implant provides the most appropriate force transfer and allows development of symmetrical mesial and distal embrasures.22 If, however, an immediate-placement strategy is employed, it is technically very difficult to center an implant in the socket, particularly for replacement of mandibular molars. Balshi recommends cementing two narrow-diameter implants, while others recommend employing one of the root sockets and cantilevering the restoration.23 The use of a trephine to initially create the osteotomy through the septum permits insertion of the implant in a more axial position. While the procedure is technically more difficult in that the trephine must be stabilized during the initial cuts, it positions the implant ideally, enabling forces in the long axis of the implant.
The design of the implant system used in this study provides a strong implant-abutment connection. The neck of the implant is 4 mm in diameter, which provides stability to the connection. In addition, the dimensions of the screw, 2.5 mm, affords sufficient strength to allow torquing the screw to 45 Ncm. This is significantly higher than the 32 Ncm to 35 Ncm recommended by other implant systems and, thus, may be more resistant to occlusal forces, which are greatest in the molar area.24 Screw loosening was less of a problem in this trial.
The design of the connector provides a platform-switched configuration that varies from 1 mm to 3 mm depending upon the diameter of the implant. The RBM surface extends slightly onto the top of the implant, allowing for bone growth along the crest of the implant. Platform-switching transfers the microgap between the implant and abutment inward, away from the crestal bone. Platform-switching has been demonstrated to reduce the crestal die-back by moving the inflammatory infiltrate associated with the microgap away from the crestal bone.25
Summary and Conclusions
A clinical trial of a novel implant system for immediate placement in molar sites demonstrated implant success in the non-esthetic zone of 95.24% of participants. Use of the system requires non-traumatic removal of the tooth and the presence of adequate buccal and lingual alveolar bone height for primary stability. While implant placement can be done in areas of previous infection, this should be done with caution. This system is best used by an experienced implantologist.
References
1. Morton D, Jaffin R, Weber HP. Immediate restoration and loading of dental implants. Int J Oral Maxillofac Implants. 2004;19 suppl:103-108.
2. Esposito M, Grusovin MG, Willings M, et al. The effectiveness of immediate, early, and conventional loading of dental implants: a Cochrane systematic review of randomized controlled clinical trials. Int J Oral Maxillofac Implants. 2007;22(6):893-904.
3. Wilson TG, Schenk R, Buser D, Cochran D. Implants placed in immediate extraction sites: a report of histologic and histometric analyses of human biopsies. Int J Oral Maxillofac Implants. 1998;13(3):333-341.
4. Lundgren D, Rylander H, Andersson M, et al. Healing-in of root analogue titanium implants placed in extraction sockets: an experimental study in the beagle dogs. Clin Oral Implants Res. 1992;3(3):136-143.
5. Todescan R Jr, Pilliar RM, Melcher AH. A small animal model for investigating endosseous dental implants: effect of graft materials on healing endosseous, porous-surfaced implants placed in a fresh extraction socket. Int J Oral Maxillofac Implants. 1987;2(4):217-223.
6. Cooper LF, Rahman A, Moriarty J, et al. Immediate mandibular rehabilitation with endosseous implants: simultaneous extraction, implant placement, and loading. Int J Oral Maxillofac Implants.. 2002;17(4):517-525.
7. Winkler, S, Morris HF, Ochi S. Implant survival to 36 months as related to length and diameter. Ann Periodontol. 2000;5(1):22-31.
8. Morand M, Irinakis T. The challenge of implant therapy in the posterior maxilla: providing a rationale for the use of short implants. J Oral Implantol. 2007;33(5):257-266.
9. Fugazzotto, PA, Beagle JR, Ganeles J, et al. Success and failure rates of 9 mm or shorter implants in the replacement of missing maxillary molars when restored with individual crowns: preliminary results 0 to 84 months in function. A retrospective study. J Periodontol. 2004;75(2):327-332.
10. Rangert, BR, Sullivan RM, Jemt TM. Load factor control for implants in the posterior partially edentulous segment. Int J Oral Maxillofac Implants. 1997;12(3):360-370.
11. Langer B, Langer L, Herrmann I, Jorneus J. The wide fixture: a solution for special bone situations and a rescue for the compromised implant. Part 1. Int J Oral Maxillofac Implants. 1993;8(4):400-408.
12. Tawil, G, Aboujaoude N, Younan R. Influence of prosthetic parameters on the survival and complication rates of short implants. Int J Oral Maxillofac Implants. 2006;21(2):275-282.
13. Petrie C, Williams JL. Comparative evaluation of implant designs: influence of diameter, length, and taper on strains in the alveolar crest. A three-dimensional finite-element analysis. Clin Oral Implants Res. 2005;16(4):486-494.
14. Nelson K, Ozyuvaci H, Bilgic B, et al. Histomorphometric evaluation and clinical assessment of endosseous implants in iliac bone grafts with shortened healing periods. Int J Oral Maxillofac Implants. 2006;21(3):392-398.
15. Löe H. The gingival index, the plaque index, and the retention index systems. J Periodontol. 1967;38(6):suppl:610-616.
16. Himmlová L, Dostalová T, Kácovský A, Konvicková S. Influence of implant length and diameter on stress distribution: A finite element analysis. J Prosthet Dent. 2004;91(1):20-25.
17. Iplikçioğlu H, Akça K. Comparative evaluation of the effect of diameter, length, and number of implants supporting three-unit fixed partial prostheses on stress distribution in the bone. J Dent. 2002;30(1):41-46.
18. Ersanli S, Karabuda C, Beck F, Leblebiciogl UB. Resonance frequency analysis of one-stage dental implant stability during the osseointegration period. J Periodontol. 2005;76(7):1066-1071.
19. Schwartz-Arad D, Chausku G. The ways and wherefores of immediate placement of implants into fresh extraction sites: A literature review. J Periodontol. 1997;68(10):915-923.
20. Minichetti JC, D'Amore JC, Hong AY. Three-year analysis of tapered screw-vent implants placed into extraction sites grafted with mineralized bone allograft. J Oral Implantol. 2005;31(6):283-293.
21. Fugazzotto PA. Treatment options following single tooth removal: A literature review and proposed hierarchy of treatment selection. J Periodontal. 2005;76(5):821-831.
22. Eskitascioglu G, Usumez A, Sevimay M, et al. The influence of occlusal loading location on stresses transferred to implant-supported prostheses and supporting bone: A three-dimensional finite element study. J Prosthet Dent. 2004;91(2):144-150.
23. Balshi T, Hernandez RE, Pryszlak MC, Rangert B. A comparative study of one implant versus two replacing a single molar. Int J Oral Maxillofac Implants. 1996;11(3):372-378.
24. Lavrentiades G, Yousef H, Luke A, Flinton R. Changes in abutment screw dimensions after off-axis loading of implant-supported crowns: A pilot study. Implant Dent. 2009;18(5):447-453.
25. Herman F, Lerner H, Palti A. Factors influencing the preservation of the implant marginal bone. Implant Dent. 2007;16(2):165-175.
About the Authors
Hoda Yousef, DMD, MS
Associate Professor
Department of Restorative Dentistry
University of Medicine and Dentistry of New Jersey
Newark, New Jersey
Mark Khaimov, DMD
Adjunct Assistant Professor
Department of Periodontics
University of Medicine and Dentistry of New Jersey
Newark, New Jersey
Saul Weiner, DDS
Professor
Department of Restorative Dentistry
University of Medicine and Dentistry of New Jersey
Newark, New Jersey