Quality and Conservative Approach to Class I Resin Composite Restorations
Gildo C. Santos Jr., DDS, MSc, PhD; Len Boksman, DDS, BSc; and M. Jacinta Santos, DDS, MSc, PhD
Abstract
Advances in technology and adhesive dentistry have allowed practitioners to achieve long-term restorative results with minimal damage to tooth structures. The use of bonded restorations in restorative dentistry, including placement of resin composite restorations, has largely replaced the use of amalgam. The clinical case presented describes a technique utilizing minimal cavity preparation aimed at improving the quality and longevity of a Class I resin composite restoration. The procedure includes the use of an occlusal index to restore the tooth back to its original contour and anatomy. Other factors discussed are the use of matrix metalloproteinases inhibitors, new advances in bonding agents, proper light-curing technique, and minimal finishing and polishing of the restoration.
Minimally invasive dentistry has become a catchphrase in today’s practice, as clinicians are generally taking a more conservative approach to determining the best option to treat dental disease while preserving healthy tooth structure. A minimally invasive approach to treating dental caries encompasses detecting, diagnosing, intercepting, and treating the condition on a microscopical level.1 This approach utilizes fluoride and emphasizes the prevention of bacterial microleakage between the tooth and the restoration, deferring operative intervention for as long as possible. Standardized risk assessment can be used to identify the factors driving the patient’s disease so the clinician can address the cause of the disease. For any approach to be successful, clinicians must engage their patients in the management of their disease. Therefore, any restorative procedure must be conducted in conjunction with well-understood preventive techniques and patient education.2,3
Caries progression through enamel is very slow, especially in patients exposed to fluoride and in cases where treatment of lesions that are confined to half of the enamel is not indicated.4 Mejare5 noted that early dentin lesions in 12- to 15-year-old patients show annual progression rates from superficial to deep dentin in 32.5% of cases.
Advances in Adhesion
Advances in technology and adhesive dentistry have allowed practitioners to achieve long-term restorative results with minimal damage to tooth structures. Old cavity design preparations with preventive extension have been replaced by minimal cavity designs, and repair of defective restorations has supplanted replacement. Technological advances have increased the use of bonded restorations in restorative dentistry, including placement of resin composite restorations instead of amalgams.6
The literature has acknowledged that achieving perfect occlusion, anatomic details, and finishing and polishing with resin composite restorations is time-consuming.7 Dilley et al7 stated that a Class I composite resin restoration requires 35% more insertion and finishing time than an amalgam restoration. To address this challenge, a technique was disclosed in 1986 as US Patent #4,571,188 (Occlusal Matrix for Light-cured Composites), which is now in the public domain. This method utilized a transparent impression material to capture the occlusal anatomy of a tooth prior to preparation and restoration.
Later, several authors proposed methods to reduce finishing and polishing time. Some techniques involved employing the bite-form or functionally generated occlusion8,9; others proposed thermoplastic resin, transparent impression materials, and clear plastic wrap as a custom matrix material to substitute bite-form or functionally generated occlusion.10-12 The most promising technique utilized a clear custom occlusal matrix to place posterior composite restorations. This custom occlusal matrix technique significantly reduced placement and finishing time and improved surface smoothness of posterior composite restorations placed in vitro.10,11
Another factor to consider when placing resin-based composite restorations bonded to dentin substrate is the degradation of the collagen fibers, which affects the longevity of bonding to dentin. Collagen fibers are the only continuous structure between underlying mineralized dentin and overlying adhesive layer, and preserving the integrity of this tissue is vital for the longevity of esthetic restorations. According to Pashley,12 different strategies have been employed to neutralize the enzymes (ie, matrix metalloproteinases [MMPs]) responsible for collagen degradation and materials displaying antibacterial qualities. This includes the use of desensitizers containing glutaraldehyde (eg, G5™, Clinician’s Choice, clinicianschoice.com; MicroPrime™ B, Danville Materials, danvillematerials.com; GLUMA®, Kulzer, kulzer.com).
Sadek et al13 noted that, because there is no covalent bonding between chlorhexidine (CHX) and collagen fibers, it is likely that the CHX leaches from the hybrid layer over a period of 1 to 2 years, leaving the collagen to degrade. This observation provided the rationale for chemically grafting CHX to resin monomers to create CHX–methacrylates and incorporating these resin monomers with anti-MMP potential into dentin adhesives to increase long-term bond stability (eg, MPa™ MAX, Clinician’s Choice; Peak® Universal, Ultradent Products, ultradent.com). Another example of an MMP inhibitor grafted into a bonding agent is 12-methacryloyloxydodecyl-pyridinium bromide (MDPB), an antibacterial monomer used in two-step self-etching primer adhesives (eg, Clearfill™ SE Protect, Kuraray, kuraraydental.com).12
Light-Curing
The polymerization of resin composites can be influenced by light intensity and exposure time.14 The effectiveness of a light-curing procedure depends on the light’s output power, its light spectrum, and tip design. Other important factors include the curing exposure time, resin chemistry, type of photoinitiators, location and orientation of the restoration, any materials that partially block the light, distance between the restorative material and light source, and the clinician’s ability to aim and maintain the light on or at the target at 90 degrees.15 The principles of light-curing are important for clinicians to understand because unbound monomers are cytotoxic, and undercuring can also cause flex with pumping of the restoration, resulting in postoperative sensitivity.14
Minimally Invasive Approach
The following clinical case depicts and discusses minimal cavity preparation and the science behind each product/technique selected in order to improve the quality and longevity of a Class I resin composite restoration. The case report describes the use of an occlusal index to restore the tooth back to its original contour and anatomy, the use of MMP inhibitors, new advances in bonding agents, proper light-curing technique, and minimal finishing and polishing of the restoration.
Clinical Case
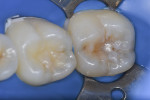
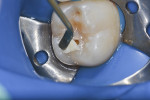
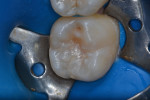
A 15-year-old female patient presented to the authors’ clinic with a small cavity lesion at the distal occlusal pit that had affected enamel and dentin (Figure 1). After intraoral and radiographic examination it was decided to use a lesion orientation approach, which means to first access the dentin caries, remove infected dentin, and then minimally modify the cavity to receive the filling material, combined with an occlusal index technique.9-11
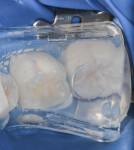
A clear silicone (Template Clear, Clinician’s Choice) was selected due to its physical and mechanical properties. This water-clear material is designed especially to be used as a matrix for the fabrication of temporary restorations, and, in the authors’ experience, offers excellent flow properties, capturing precise morphology. Regardless of what kind of bite registration material is used, it should have good flow adaptation, not be too rigid, and should set within a reasonable amount of time, eg, 45 seconds to 1 minute. A clear impression tray was modified (Figure 2 and Figure 3), and the material was injected into the tray and placed onto the occlusal surface of the tooth prior to cavity preparation (Figure 4 and Figure 5).
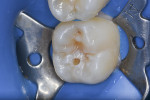
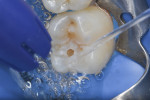
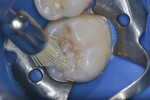
A conservative cavity preparation was performed to enable access to the affected dentin (Figure 6). After removal of the caries, both the enamel and dentin were etched (MAX Etch, Clinician’s Choice) for 20 seconds (Figure 7). The etchant agent was rinsed for 10 seconds (Figure 8) and lightly dried.
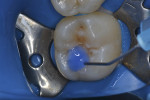
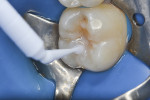
Although it was a small preparation with 2-mm depth into dentin, a desensitizing agent (G5) was used with a twofold purpose. The first reason was to desensitize the dentin because of the case involving a young patient with a large pulp chamber. The agent used desensitizes the dentin by coagulating the plasma proteins contained within the dentinal tubule fluid.16 The second reason was to stabilize the collagen fibers to prevent their degradation due to activation of MMPs.12,17 The desensitizer was applied with a microbrush for 10 seconds (Figure 9) and the excess removed, leaving a glistening appearance.
As mentioned previously, when applied by itself, it is likely that the CHX leaches from the hybrid layer over a period of 1 to 2 years, leaving the collagen to degrade. However, when the CHX is combined with or grafted into a bonding agent, the copolymerization with other dimethacrylate resin monomers prevents CHX from debinding and diffusing out of the incompletely resin-infiltrated hybrid layers.12
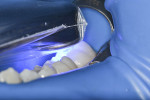
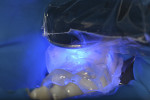
Applying the combination of concepts for MMP inhibition, CHX plus HEMA (G5), and “therapeutic adhesive systems,”12 a bonding agent containing CHX was selected (MPa MAX). After application of the G5 desensitizer, a puddle of MPa MAX was applied and scrubbed for 10 seconds, then air-dried with a half air pressure for another 10 seconds, and light-cured for 10 seconds using a curing light with an output of 1000 mW/cm2 (Figure 10 and Figure 11).
After curing the bonding agent, a nanofilled hybrid composite (Renamel Nano, Cosmedent, cosmedent.com) was selected due to its mechanical and physical properties. Nanofilled composites, also known as universal composites, present improved strength, wear resistance, improved polishability, and enhanced esthetics.18 Such materials can be used to create predictable, esthetic restorations in posterior stress-bearing areas that exhibit long-term durability and a high degree of surface anatomy and luster.
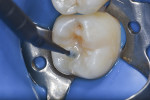
Although the preparation was small the restorative material was placed in two increments. In the first increment (Figure 12) the composite was accommodated inside the cavity preparation up to the dentin–enamel junction and light-cured for 10 seconds. The second and final increment was placed to the level of the cavity preparation, and the clear matrix was pressed against it. With the matrix in position, the resin composite was light-cured for another 10 seconds (Figure 13) with a light-curing unit (VALO®, Ultradent, ultradent.com) at a power of 1000 mW/cm2.
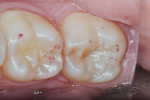
As discussed previously, this restorative technique, which employs a clear matrix, results in a restoration with a smooth surface, free from the oxygen-inhibited layer, and, thus, minimal finishing and polishing is required (Figure 14). The surface was quickly finished with a diamond impregnated bristle brush (Groovy Diamond, Clinician’s Choice), and the final restoration was a precise replica of the original occlusal anatomy (Figure 15 and Figure 16). The final restoration was obtained in a time-effective manner and no occlusal adjustment was needed after finishing and polishing.
Conclusion
In conclusion, applying the combined current concepts in restorative dentistry can result in minimally invasive restorations that replicate natural occlusion with highly polished surfaces that resist staining and plaque accumulation, leading to an esthetic, durable, and functional result that will further increase patient satisfaction and the longevity of the restoration.
About the Authors
Gildo C. Santos Jr., DDS, MSc, PhD
Associate Professor
Restorative Dentistry
Schulich School of Medicine & Dentistry
Western University
London, Ontario, Canada
Len Boksman, DDS, BSc
Former Associate Professor in Operative Dentistry
Schulich School of Medicine & Dentistry, of Western University
London, Ontario, Canada
Dr. Boksman is retired from private practice.
M. Jacinta Santos, DDS, MSc, PhD
Associate Professor
Schulich School of Medicine & Dentistry
Western University
London, Ontario, Canada
References
1. Rainey JT. Air abrasion: an emerging standard of care in conservative operative dentistry. Dent Clin North Am. 2002;46(2):185-209.
2. Peters MC, McLean ME. Minimally invasive operative care, I: minimal intervention and concepts of minimally invasive cavity preparations. J Adhes Dent. 2001;3(1):7-16.
3. Peters MC, McLean ME. Minimally invasive operative care, II: contemporary techniques and materials—an overview. J Adhes Dent. 2001;3(1):17-31.
4. Murdoch-Kinch CA, McLean ME. Minimally invasive dentistry. J Am Dent Assoc. 2003;134(1):87-95.
5. Mejàre I, Stenlund H, Zelezny-Holmlund C. Caries incidence and lesion progression from adolescence to young adulthood: a prospective 15-year cohort study in Sweden. Caries Res. 2004;38(2):130-141.
6. Eklund SA. Trends in dental treatment, 1992 to 2007. J Am Dent Assoc. 2010;141(4):391-399.
7. Dilley DC, Vann WF Jr, Oldenburg TR, Crisp RM. Time required for placement of composite versus amalgam restorations. J Dent Child. 1990;57(3):177-183.
8. Terry DA. Finishing and polishing tooth-colored adhesive restorations: Part I. Pract Proced Aesthet Dent. 2005;17(7):477-478.
9. Bertolotti RL, Laamanen H. Bite-formed posterior resin composite restorations, placed with a self-etching primer and a novel matrix. Quintessence Int. 1999;30(6):419-422.
10. Hamilton JC. Posterior Class II composite restorations utilizing a custom occlusal matrix. Pract Periodontics Aesthet Dent. 1999;11(3):371-374.
11. Hamilton JC, Krestik KE, Dennison JB. Evaluation of custom occlusal matrix technique for posterior light-cured composites. Oper Dent. 1998;23(6):303-307.
12. Pashley DH, Tay FR, Imazato S. How to increase the durability of resin-dentin bonds. Compend Contin Educ Dent. 2011;32(7):60-66.
13. Sadek FT, Braga RR, Muench A, et al. Ethanol wet-bonding challenges current anti-degradation strategy. J Dent Res. 2010;89(12):1499-1504.
14. ADA Professional Product Review. Curing lights. 2009;4(4).
15. Mahn E. Light polymerization. Inside Dentistry. 2011;7(2):66-71.
16. Boksman L, Tousignant G, Boushell LW, Santos Jr GC. Adhesives: newer is not always better—Part 2. Inside Dentistry. 2012;8(3):70-74.
17. Pashley DH, Tay FR, Yiu C, et al. Collagen degradation by host-derived enzymes during aging. J Dent Res. 2004;83(3):216-221.
18. Morgan M. Finishing and polishing of direct posterior resin restorations Pract Proced Aesthet Dent. 2004;16(3):211-216.