Evaluating the Clinical Efficacy of Tooth Powder on Plaque-Induced Gingivitis: A Randomized Controlled Trial
Muhammad Khalil Khan, BDS, MPH, MCPS (Com), MCPS (Perio), PhD
Abstract
Toothpastes and tooth powders are common oral care products used to control plaque and other deposits from tooth surfaces, thereby reducing gingivitis. This study was conducted to evaluate the efficacy of tooth powder in controlling dental plaque and gingivitis. A double-blind, parallel-arm, randomized controlled trial was conducted on 154 participants, aged 33 to 40 years, having at least 20 teeth with a full-mouth gingival index (GI) score ≥ 1.04 and fulfilling other inclusion/exclusion criteria. The plaque index (PI) and GI scores were used as measures of oral hygiene. Outcome variables of gingivitis and dental plaque were evaluated in test and control groups randomized with 1:1 ratio at 4, 12, and 24 weeks of follow-up. Repeated measure analysis of variance (ANOVA), t test, and paired t test were used for statistical analysis with a significance level of ≤ 0.050. One hundred and thirty-seven (N = 137) participants completed the study. Demographic and oral clinical parameters showed no statistical difference between the test group and the control group at baseline. A statistically significant difference (P ≤ .033) between the test group and the control group was observed for dental PI and GI scores at follow-up examinations. The repeated measure ANOVA also revealed a significant group interaction (P ≤ .01) for a reduction in outcome variables. From the current study, it may be concluded that tooth powder has been shown to be statistically superior to toothpastes in controlling dental plaque and gingivitis.
Plaque-induced gingivitis is a common periodontal disease that affects more than 90% of the world’s population, regardless of age, sex, or race.1 A worldwide epidemic level of plaque-induced gingivitis has been reported,2,3 and deprived populations have demonstrated gingivitis in even greater proportions.4
Dental plaque is known as the primary etiological agent responsible for oral inflammatory diseases.5 Dental plaque accumulation on dental and gingival tissues for a certain time period with other contributing factors may lead to dental caries and/or periodontal diseases.6 Plaque pathogens produce toxins and enzymes that initiate an inflammatory response in the marginal gingiva.7 If not managed at early stages, dental plaque accumulation results in a cascade of events leading to the destruction of periodontal tissues and consequently tooth loss.8
Effective plaque control techniques have been suggested that maintain dental biofilms at levels compatible with oral health; indeed, teeth cleaning and plaque control remain the cornerstone for all preventive strategies for oral diseases, particularly gingivitis.9
The relevance of mild-to-moderate forms of gingivitis as a public health problem and the efforts to control this disease at a population level would be justifiable.10 Control of plaque by antimicrobial means has largely been ineffective, as plaque biofilms have proven to be remarkably resistant to them11; however, abrasive agents in dentifrices help to remove plaque and stained pellicle from the teeth, polish the surfaces, restore the natural luster, and enhance enamel whiteness.12,13
Significant prevalence of gingival inflammation in the general population suggests that most people practice inadequate oral hygiene and perform mechanical plaque removal unsatisfactorily.14 Antimicrobial and antiplaque agents in oral care products can augment mechanical plaque control by several direct and indirect mechanisms that not only involve reducing or removing dental biofilms, but also include inhibiting bacterial metabolism when these agents are still present at sublethal concentrations.15 The use of antiplaque agents in dental care products such as toothpaste, tooth powder, and mouthwash is recommended to supplement plaque control.16,17
There is limited research on the clinical efficacy of tooth powder on plaque and gingivitis. A search of the relevant scientific literature found only two clinical trials on the clinical efficacy of tooth powder.18,19 The present randomized clinical trial evaluated and compared the efficacy of a tooth powder and toothpaste in patients with plaque-induced gingivitis.
Materials and Methods
This study was designed as a double-blind, randomized controlled trial. Healthy subjects with plaque-induced gingivitis who fulfilled inclusion/exclusion criteria and gave written consent received mechanical periodontal therapy and were randomized to a test group and a control group at a 1:1 ratio. The test group was provided with tooth powder and the control group received toothpaste. This study was conducted at the outpatient Department of Periodontology, Fatima Jinnah Dental College (FJDC) Hospital, in Karachi, Pakistan.
Sample size (N = 129) was calculated by assuming 10% (P = .1) proportion of the population with the condition under observation, defining the probability of risk at > 90% and the margin of error at 0.05 (confidence interval, 95%). Assuming a 20% dropout rate, 154 subjects were recruited and randomized into the test group (n = 77) and the control group (n = 77), which would be sufficient to detect a significant effect of test material with > 90% power.
Study Sample
At FJDC Hospital, 481 subjects were screened for the study. Based on general and medical exclusion criteria, 180 subjects were excluded. Thirteen subjects declined to participate in the study. The oral and/or periodontal criteria were not met by 116 subjects. Eighteen subjects failed to complete periodontal therapy. Of the remainder, 154 subjects were randomized to the test and control groups, with 77 subjects assigned to each group. By the end of the study, 137 subjects had completed the study, and their data was analyzed using per-protocol analysis. Details of all participants at each stage of examination is provided in the study flowchart (Figure 1).
Inclusion and Exclusion Criteria
General and medical inclusion criteria were male or female, aged 33 to 40 years, in good general health, available for the duration of the study, and able and willing to both follow study protocol and sign approved informed consent.
Subjects were excluded based on the following general and medical criteria: chronic systemic illness, currently smoked or used tobacco, pregnant or lactating woman, allergic to the ingredients of the products to be tested, had used an antibiotic in the past 3 months, or had routinely used any anticoagulant medication, anti-inflammatory medication, or any medications known to have effects on the gingiva.
The orodental inclusion criteria were as follows: at least 20 natural teeth (excluding third molars, grossly carious teeth, fully crowned/restored teeth, and abutment teeth) suitable for evaluation and a full-mouth gingival index (GI) score ≥ 1.04.
Orodental exclusion criteria included the following: routine use of any mouth rinse or interdental cleaning device, use of any removable appliance or fixed orthodontic appliance, having a probing depth ≥ 4 mm at any site, having had active periodontal therapy during the past 6 months or periodontal prophylaxis or periodontal maintenance therapy in the past 3 months, or having more than three carious lesions requiring immediate care. The exit criteria for the study were as follows: subjects who were no longer willing or able to continue participation, who did not comply with study procedures and/or appointments, who developed or experienced adverse reactions to assigned study products and/or devices, or subjects who due to a change in status subsequently met the above-listed exclusion criteria during the study.
Randomization
Random number tables were used for randomization, and subjects were provided sealed opaque envelopes for their allocation to either the test or the control group. Record of allocation was maintained for recall visits for oral/periodontal examinations, masking the allocation from the examiners.
Clinical Parameters
Parameters of the study were recorded at four examinations: the first examination (E1), considered the baseline; the second examination (E2), which took place 4 weeks after periodontal treatment; the third examination (E3), at 8 weeks after E2; and the last examination (E4), at 12 weeks after E3. Oral clinical examination was scored using two indices, GI20 score and plaque index (PI) 21,22 score.
For the GI score, the following criteria were used: 0 = normal gingiva, 1= mild inflammation (slight change in color and slight edema, but no bleeding on probing), 2 = moderate inflammation (redness, edema and glazing, bleeding on probing), and 3 = severe inflammation (marked redness and edema, ulceration with a tendency toward spontaneous bleeding).
For the PI score, the following criteria were noted: 0 = no plaque, 1 = separate flecks of plaque, 2 = a continuous band of plaque of 1 mm, 3 = a band of plaque > 1 mm but covering less than one third of the tooth surface, 4 = plaque covering more than one third but less than two thirds of tooth surface, and 5 = plaque covering more than two thirds of tooth surface.
Clinical Calibration
Examiners were trained and calibrated for inter-examiner and intra-examiner repeatability of measurements of clinical parameters of GI and PI scores. Intra-examiner reliability was 0.91, whereas the inter-examiner reliability was 0.88, as calculated by Kappa scores. The ethical committee of the FJDC Hospital approved the study conducted in the outpatient Department of Periodontology.
Statistical Analysis
Data was presented as mean ± SD and percentages or proportions. Independent t test was applied to see the significant difference in the mean GI and PI scores in the control group and in the test group. Repeated measure analysis of variance (ANOVA) was used to ascertain the significance mean change in GI and PI scores at follow-up examinations. To delineate the equality of variances, Levene’s test for independent samples and Mauchly’s test for repeated measurement ANOVA were used. P value ≤ .05 was taken as significant, and the Shapiro-Wilk test was used to determine the normality of the data distribution.
Results
Study Parameters at Baseline
The age of the study participants ranged from 33 to 40 years; mean age was 37.3 ± 0.17 years. In the study, 72% of the participants were men, 82% had secondary or higher education, and 29% were from a low income group (≤ US $100 per month). Statistically (P ≥ .47), there was no difference in demographic parameters (age, gender, education, and income) between the test group and the control group at baseline. All clinical variables (GI and PI scores) also showed no significant (P ≥ .104) difference between the groups. All the subjects included in this study experienced a moderate level of gingivitis (range, 2 to 2.5 GI score) (study candidates with a GI score < 1 were not included in the study) and moderate-to-severe plaque accumulation on the surfaces of all teeth.
Comparison of Study Parameters at Baseline and Follow-up Examinations
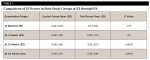
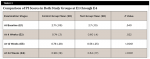
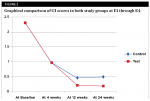
GI scores showed no statistically significant difference at E1 and E2, whereas a significant difference was noted at E3 and E4 (P < .0001) (Table 1). The repeated measures ANOVA revealed a significant group interaction (P = .001). PI scores showed no difference at E1, whereas a statistically significant difference was noted at E2 (P < .022), E3 (P < .0001), and E4 (P < .001) (Table 2). The repeated measures ANOVA revealed a significant group interaction (P < .0001). The change in clinical oral parameters (GI and PI scores) is presented graphically in both study groups at E1 through E4 (Figure 2 and Figure 3).
Discussion
The current clinical trial offers scientific evidence for the efficacy of tooth powder in controlling plaque and gingivitis compared with toothpaste. This information may fill a gap in the existing literature, caused by inconsistent reporting and subjectivity of studies on dentifrices in reducing plaque-induced gingivitis.
Dental plaque is the principal etiological agent responsible for periodontal diseases, including gingivitis. Plaque-induced gingivitis is the result of an interaction between microorganisms found in dental plaque biofilm and the tissues and inflammatory cells of the host.23 Control of dental plaque biofilm, which involves various mechanical and chemical techniques, is the primary step in the prevention of periodontal disease.24 Control of plaque by antimicrobial means, however, has been largely ineffective in that plaque biofilms have proved remarkably resistant to antimicrobial action. The process of bacterial attachment to the tooth surface involves a variety of physiochemical interactions.25
The present study was conducted on patients with gingivitis, defined as having a full-mouth GI score ≥ 1.04. At the end of this study, 70 subjects in the test group and 67 subjects in the control group had complied with the study protocol and completed the 6-month trial with a lost-to-follow-up rate of 11%. Subjects of both the test and the control group were observed to have an insignificant difference in all study parameters at baseline. All subjects received nonsurgical mechanical periodontal therapy before randomization and concealed allocation to the test and control group. None of the patients disclosed any unpleasant experience during the study. The oral clinical variables in the present study were comparable with another contemporary study26 for the baseline levels of GI and PI scores.
Another study compared the users and nonusers of tooth powder that contained calcium carbonate and essential oils as the active ingredients, which are used as antimicrobial agents in reducing plaque and, by extension, gingivitis.27 These tooth powders, which are chemotherapeutic agents, are useful in patients who cannot manage mechanical dental cleaning. As noted by Alves and colleagues,28 mouthwash and toothpaste coupled with mechanical oral hygiene play a major role in oral health. Essential oil–based tooth powders reach their target without being substantially diluted by saliva and remain at such concentrations that they are not washed away by gingival crevicular fluid.29 This is a major requirement of a chemotherapeutic or antimicrobial agent to be effective in eliminating and controlling micro-organisms that cause subgingival plaque.30
The abrasiveness of dentifrices is a concern of oral healthcare professionals.31 The relative dentin abrasivity (RDA) level of tooth powder used by the test group in the present study was 157,32 which is well below RDA limits recommended by International Order for Standarization (ISO) standard No. 11609, which is 250; the US Food and Drug Administration, which is 200; and the American Dental Association, also 250.31 Research from the Pakistan Council of Scientific and Industrial Research Laboratories (Karachi, Pakistan) was conducted that tested 20 dentifrices, including the tooth powder used in the study for the test group, which was found to be free from steroid.33
In the current study, the GI score continued to decline in the test group during the follow-up periods; however, it increased in the control group. This indicates that the tooth powder played a more significant role in controlling gingivitis than did the toothpaste. Claydon and coworkers34 observed that when toothpaste is used, most of the cleaning is achieved by the mechanical action of the toothbrush and not by the toothpaste. Nonetheless, a toothpaste formulation containing 0.13% calcium glycerophosphate in a natural calcium carbonate has proved to be significantly more effective in reducing plaque and gingivitis than other toothpaste formulations under study, thus strengthening the role of calcium carbonate in control of plaque and gingivitis.4 In another study by Li and colleagues,35 subjects of the test group exhibited a significant difference from baseline at the 3-month and 6-month examinations after using toothpaste containing 8% arginine, 1450 ppm sodium monofluorophosphate, and calcium carbonate.
The severity of gingivitis is influenced by host factors,29 and as Hasturk and coworkers27 noted, with effective oral biofilm disruption gingivitis can be reversed because it does not have adverse effects on the tissues. Thus, the present study is consistent with this observation in that tooth powder had a curative effect on gingivitis. After 6 months, the GI scores had dropped to very low levels and appeared to be declining further.
In the present study, the PI scores lowered in the test group over 3- and 6-month follow-up, but increased in the control group over the same period. The dental plaque reduction was substantial at the 4-week examination but declined over the following months in both groups. However, the plaque score was declined significantly in the test group. Such short-term studies have helped in determining the efficacy of tooth powders in reducing dental plaque and gingivitis as observed by Chapple and colleagues.36 Physically removing dental plaque or rinsing it off completely is difficult,37 which is why, in the present study, a decline in the dental PI scores was noted, though good control cannot be ensured for a longer period.
Conclusion
The current study revealed that tooth powder and toothpaste were equally effective in both the test group and the control group from a clinical perspective; however, tooth powder showed a statistically significant effectiveness as compared with toothpaste. However, another randomized controlled trial, to be conducted on a larger scale or at a multicenter, is needed to realize the efficacy of tooth powder in regard to cost effectiveness.
Acknowledgment
The authors would like to acknowledge Asif Hanif, Assistant Professor and Head of the Bio-Statistics Department, Gulab Devi Post Graduate Medical Institute, for helping with statistical analysis.
About the Author
Muhammad Khalil Khan, BDS, MPH, MCPS (Com), MCPS (Perio), PhD
Associate Professor, Department of Periodontology/Oral Medicine, Quassim University College of Dentistry, Saudi Arabia
References
1. de Oliveira SM, Torres TC, Pereira SL, et al. Effect of a dentifrice containing aloe vera on plaque and gingivitis control. A double-blind clinical study in humans. J Appl Oral Sci. 2008;16(4):293-296.
2. Bhat M. Periodontal health of 14-17-year-old US school children. J Public Health Dent. 1991;51(1):5-11.
3. Botelho MA, Bezerra Filho JG, Correa LL, et al. Effect of a novel essential oil mouthrinse without alcohol on gingivitis: a double-blinded randomized controlled trial. J Appl Oral Sci. 2007;15(3):175-180.
4. Peter S, Nayak DG, Philip P, Bijlani NS. Antiplaque and antigingivitis efficacy of toothpastes containing Triclosan and fluoride. Int Dent J. 2004;54(5 suppl 1):299-303.
5. Guthmiller JM, Novak KF. Periodontal diseases. In: Brogden KA, Guthmiller JM, eds. Polymicrobial Diseases. Washington, DC: ASM Press; 2002:chap 8.
6. Juan SP. Dental caries and periodontal disease (prevention and control methods). J Philipp Dent Assoc. 1999;51(1):29-36.
7. Darveau RP, Tanner A, Page RC. The microbial challenge in periodontitis. Periodontol 2000. 1997;14:12-32.
8. Pihlstrom BL, Michalowicz BS, Johnson NW. Periodontal diseases. Lancet. 2005;366(9499):1809-1820.
9. Sgan-Cohen HD, Adut R. Promotion of gingival and periodontal health from childhood. In: Birnstein E, Needleman HL, Karimbux N, Van Dyke TE, eds. Periodontal and Gingival Health and Diseases: Children, Adolescents, and Young Adults. London, England: Martin Dunitz; 2001.
10. Baelum V, Luan WM, Chen X, Fejerskov O. Predictors of tooth loss over 10 years in adult and elderly Chinese. Community Dent Oral Epidemiol. 1997;25(3):204-210.
11. Wade WG, Slayne MA. Controlling plaque by disrupting the process of plaque formation. Periodontol 2000. 1997;15:25-31.
12. Baxter PM, Davis WB, Jackson J. Toothpaste abrasive requirements to control naturally stained pellicle. The relation of cleaning power to toothpaste abrasivity. J Oral Rehabil. 1981;8(1):19-26.
13. Schemehorn BR, Moore MH, Putt MS. Abrasion, polishing, and stain removal characteristics of various commercial dentifrices in vitro. J Clin Dent. 2011;22(1):11-18.
14. Al-Kholani AI. Comparison between the efficacy of herbal and conventional dentifrices on established gingivitis. Dent Res J (Isfahan). 2011;8(2):57-63.
15 Marsh PD. Contemporary perspective on plaque control. Br Dent J. 2012;212(12):601-606.
16. Charles CH, Mostler KM, Bartels LL, Mankodi SM. Comparative antiplaque and antigingivitis effectiveness of a chlorhexidine and an essential oil mouthrinse: 6-month clinical trial. J Clin Periodontol. 2004;31(10):878-884.
17. Paraskevas S. Randomized controlled clinical trials on agents used for chemical plaque control. Int J Dent Hyg. 2005;3(4):162-178.
18. Davies GN, King RM. The effectiveness of an ammonium ion tooth powder in the control of dental caries. J Dent Res. 1951;30(5):645-655.
19. West TL, King WJ. Toothbrushing with hydrogen peroxide-sodium bicarbonate compared to tooth powder and water in reducing periodontal pocket suppuration and darkfield bacterial counts. J Periodontol. 1983;54(6):339-346.
20. Loe H, Silness J. Periodontal disease in pregnancy. I. Prevalence and severity. Acta Odontol Scand. 1963;21:533-551.
21. Quigley GA, Hein JW. Comparative cleansing efficiency of manual and power brushing. J Am Dent Assoc. 1962;65:26-29.
22. Turesky S, Gilmore ND, Glickman I. Reduced plaque formation by the chloromethyl analogue of victamine C. J Periodontol. 1970;41(1):41-43.
23. Novak MJ, Donley TG. Using host response modifiers in the treatment of periodontal disease. Pract Proced Aesthet Dent. 2002;14(9 suppl):3-10.
24. Drisko CH. Nonsurgical periodontal therapy. Periodontol 2000. 2001;25:77-88.
25. Ohrn K, Sanz M. Prevention and therapeutic approaches to gingival inflammation. J Clin Periodontol. 2009;36(suppl 10):20-26.
26. Zhang J, Xuan D, Fan W, et al. Severity and prevalence of plaque-induced gingivitis in the Chinese population. Compend Contin Educ Dent. 2010;31(8):624-629.
27. Hasturk H, Kantarci A, Van Dyke TE. Paradigm shift in the pharmacological management of periodontal diseases. Front Oral Biol. 2012;15:160-176.
28. Alves KM, Goursand D, Zenobio EG, Cruz RA. Effectiveness of procedures for the chemical-mechanical control of dental biofilm in orthodontic patients. J Contemp Dent Pract. 2010;11(2):041-048.
29. Chapple IL, Milward MR, Ling-Mountford N, et al. Adjunctive daily supplementation with encapsulated fruit, vegetable and berry juice powder concentrates and clinical periodontal outcomes: a double-blind RCT. J Clin Periodontol. 2012;39(1):62-72.
30. Walker CB, Karpinia K, Baehni P. Chemotherapeutics: antibiotics and other antimicrobials. Periodontol 2000. 2004;36:146-165.
31. Stamm JW. Multi‐function toothpastes for better oral health: a behavioural perspective. Int Dent J. 2007;57(S5):351-363.
32. Khan M, Khan A, Hosein T, et al. Comparison of the plaque-removing efficacy of toothpaste and tooth powder. J Int Acad Periodontol. 2009;11(1):147-150.
33. Farooqui O, Hosein T, Hosein M. Addition of steroids in medicated dentrifices marketed in Pakistan: a possible serious health hazard. J Pak Med Assoc. 2003;53(8):332-334.
34. Claydon N, Yates R, Labello R, et al. A methodology using subjective and objective measures to compare plaque inhibition by toothpastes. J Clin Peridontal. 2004;31(12):1106-1109.
35. Li Y, Lee S, Stephens J, et al. Comparison of efficacy of an arginine-calcium carbonate-MFP toothpaste to a calcium carbonate-MFP toothpaste in controlling supragingival calculus formation and gingivitis: a 6-month clinical study. Am J Dent. 2012;25(1):21-25.
36. Chapple IL, Milward MR, Dietrich T. The prevalence of inflammatory periodontitis is negatively associated with serum antioxidant concentrations. J Nutr. 2007;137(3):657-664.
37. Silva MF, dos Santos NB, Stewart B, et al. A clinical investigation of the efficacy of a commercial mouthrinse containing 0.05% cetylpyridinium chloride to control established dental plaque and gingivitis. J Clin Dent. 2009;20(2):55-61.