The Direct-Indirect Technique for Composite Restorations Revisited
André V. Ritter, DDS, MS, MBA; Newton Fahl, Jr., DDS, MS; Marcos Vargas, DDS, MS; and Rodrigo R. Maia, DDS, MS, PhD
Abstract
In the direct-indirect composite technique, composite is applied to a nonretentive tooth preparation (eg, a noncarious cervical lesion or a veneer/inlay/onlay preparation) without any bonding agent, sculpted to a primary anatomic form, and light-cured. The partially polymerized restoration is then removed from the preparation and finished and tempered extraorally chairside. The finished inlay is bonded to the preparation using a resin-based luting agent. Advantages of this technique include enhanced physical and mechanical properties afforded by the extraoral chairside tempering process because of increased monomer conversion, and greater operator control over the final marginal adaptation, surface finishing and polishing, and anatomy of the restoration, given that these elements are defined outside of the patient’s mouth. The direct-indirect approach also affords enhanced gingival health and patient comfort. This article presents a clinical case in which the direct-indirect composite technique was used to restore three noncarious cervical lesions on the same quadrant on an adult patient. Clinical steps and tips for success are offered. The authors also present scanning electron microscope and atomic force microscope images showing the excellent marginal fit obtained with the direct-indirect composite technique.
Since their introduction in the early 1960s,1 resin-based composites have been extensively used for the restoration of both anterior and posterior teeth. When used correctly, composites have many advantages over other restorative materials. For example, composites can be used in very conservative preparations with no minimal thickness requirements. They can be bonded to the tooth structure and can esthetically reproduce the optical characteristics of the natural tooth. Composites can be cured on demand, offering virtually unlimited working time. Conversely, composites also present challenges that have been difficult to overcome. In particular, the adhesion to the tooth can deteriorate over time, compromising bonding2; composites have a limited degree of conversion,3 which can affect physical and mechanical properties; they undergo polymerization shrinkage4; and they can be difficult to apply in certain areas of the mouth.
The annual failure rate for direct composites can be as high as 4.1% and survival rates as low as 53%, depending on the location and size of the restoration.5 Multisurfaced and posterior restorations tend to have higher annual failure rates and lower survival rates over time.6 Not all factors affecting longevity of composite restorations are material-related; however, it has long been established that direct composite restorations fail primarily because of either material fracture or secondary caries.7 Many of the factors related to failure of direct composite restorations are linked to the challenges mentioned previously.
The direct-indirect composite technique was introduced in the early 1990s, primarily as a means to heat-temper composites in partial and full composite veneer applications.8-11 More recently, the technique has been revisited and its application expanded to include Class V noncarious cervical lesion (NCCL) restorations.12,13 When using a direct-indirect composite technique, the clinician applies a light-cured composite material to a nonretentive tooth preparation (eg, an NCCL area or a veneer/inlay/onlay preparation) without previous application of an adhesive resin, sculpts the composite to a primary anatomic form, and light-cures the partially finished restoration. The partially polymerized restoration is then carefully removed from the nonretentive, nonbonded preparation, finished, and tempered extraorally chairside. After try-in, the finished inlay is bonded to the preparation using a resin-based flowable composite or cement.8,9,11-13
From a material standpoint, the main advantage of this approach over a directly placed composite restoration is the enhanced physical and mechanical properties afforded by the extraoral chairside tempering process because of increased monomer conversion.14-17 From an operator standpoint, the technique affords greater operator control over the final marginal adaptation, surface finishing and polishing, and anatomy of the restoration, given that these elements are defined outside of the patient’s mouth.12 Finally, patients overwhelmingly indicate that the direct-indirect technique is more comfortable to them because many of the restorative steps involving rotary instrumentation, particularly subgingival margin finishing in NCCL restorations, occurs extraorally.12
This article presents a clinical case in which the direct-indirect composite technique was used to restore three NCCLs on the same quadrant on an adult patient. Clinical steps and tips for success are offered.
Clinical Technique
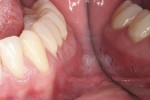
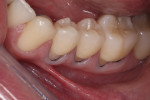
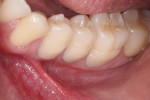
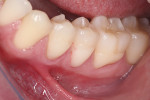
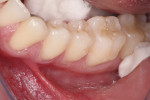
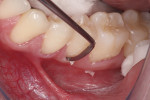
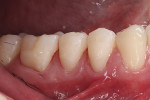
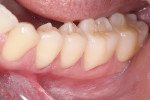
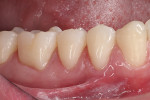
A young adult patient presented complaining of hypersensitivity in the cervical areas of teeth Nos. 19 through 21. Figure 1 and Figure 2 show buccal and profile views, respectively, of NCCLs on these teeth. The hypersensitivity was an indication for the management of these areas. A direct-indirect approach was recommended because of the advantages presented previously.
Composite Selection
For NCCLs with minor or no root exposure, a single shade of high opacity and high chroma composite imparts the blending effect for an optimal outcome. Examples of this type of composite include Estelite Omega® (Tokuyama Dental America Inc., tokuyama-us.com), Renamel Microfill (Cosmedent, cosmedent.com), and Filtek™ Supreme Ultra Body (3M ESPE, 3m.com).
Tooth Preparation
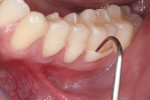
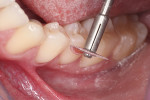
Non-impregnated retraction cords (eg, Ultrapack®, Ultradent, ultradent.com) are selected according to sulcus depth and packed to reveal the gingival margin of the lesion (Figure 3). Using a flame-shaped diamond bur, the sharp enamel edges of the lesion are beveled and brought to a feather-edge infinity line at the coronal (occlusal) margin. This step assists in producing a seamless tooth–composite transition. Any irregular gingival margins are smoothed with round diamond burs to ensure an accurate marginal imprint with the composite.
Composite Application and Sculpting
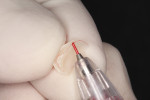
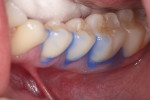
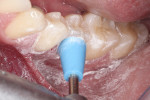
A sufficiently large increment of composite is shaped into a ball and carried onto the preparation. When more than one tooth is being treated on the same quadrant, they should be restored at the same time to optimize restorative time. With gentle fingertip strokes, the composite is molded to the shape of the cervical emergence profile and carried past the bevel until it assumes a gross anatomical configuration. Gentle tapping of the composite assures an accurate imprint of the gingival margins, especially when they are slightly subgingival. Further anatomical refinement is performed with hand instruments and artist brushes to warrant proper interproximal marginal adaptation. Establishing an ideal marginal fit requires extending the composite increment beyond the cervical preparation margin onto the free gingival margin (Figure 4). This enables a precise and visible finish line to be obtained on the intaglio surface of the composite inlay, which facilitates extraoral finishing and polishing.
Inlay Light Activation and Removal
A high-intensity curing unit (eg, VALO®, Ultradent; BluePhase G2®, Ivoclar Vivadent, ivoclarvivadent.us; Elipar™ DeepCure-S, 3M ESPE) is used for initial curing of the composite. An exposure of 1400 mW/cm2 for 8 to 12 seconds should suffice for this purpose. After light-curing, the inlays are flaked off with a curette and organized sequentially on a pad (Figure 5).
Inlay Finishing and Polishing
As noted previously, one of the main advantages of the direct-indirect composite technique is its extraoral finishing and polishing protocol. After outlining the margin finish line of the inlay (Figure 6), aluminum-oxide finishing discs (eg, Sof-Lex™ XT Pop-On, 3M ESPE) are used sequentially to bring the margins to a knife-edge finish and to polish. The optimal smoothness and gloss produced by the use of discs have been reported to promote enhanced gingival health compared with other finishing and polishing techniques.18,19 The prefinished composite inlays are then tried intraorally; additional finishing can be accomplished extraorally until the desired marginal fit is obtained because the inlays can easily be inserted and lifted from the tooth preparation (Figure 7 through Figure 9).
Inlay Treatment for Bonding
Next, each inlay is submitted to supplemental extraoral light-curing by using a chairside high-intensity curing unit for at least 30 seconds (Figure 10). If a high-energy curing light is used, this extraoral curing step will not only provide adequate polymerization for the composite material, but also heat similar to heat-tempering, which has been reported to induce an increase in monomer conversion and subsequent improvement of the physical properties.14,15 Adhesion to the intaglio surface can be enhanced by airborne particle abrasion. The inlays are then cleaned with 35% phosphoric acid for 5 seconds, rinsed, and dried. After silane treatment, a thin coat of a hydrophobic adhesive is applied, and the inlays are coated with a thin, even layer of a flowable composite of matching shade and saved under a protective shield.
Tooth Preparation for Bonding
If the retraction cords have been removed with the inlays, fresh ones are packed into the sulci. Airborne particle abrasion with either 27 µm or 50 µm of aluminum oxide is performed on the lesions to optimize adhesion.20,21 The choice of adhesion protocol, either etch-and-rinse or self-etch, may vary from case to case and according to tooth substrate type. Etch-and-rinse three-step adhesives are the most common and are highly indicated when no gingival inflammation is present, taking into consideration that phosphoric acid can cause bleeding on contact with an inflamed gingiva. This adhesive, examples of which include All-Bond 3® (BISCO, bisco.com), Optibond™ FL (Kerr Corp., kerrdental.com), and Adper™ Scotchbond™ Multi-Purpose Adhesive (3M ESPE), may also be beneficial in the absence of sclerotic dentin. Self-etch adhesives are less irritating to soft tissues than phosphoric acid and also have a favorable bonding mechanism to sclerotic dentin. Examples include All-Bond Universal™ (BISCO) and Clearfil™ SE Bond 2 (Kuraray, kuraraydental.com). When self-etch adhesives are used, the enamel can be etched selectively for enhanced adhesion and marginal seal.22,23
When using an etch-and-rinse adhesive, enamel is etched with 35% phosphoric acid for 15 seconds and dentin for 5 to 10 seconds (Figure 11). After rinsing, excess water is suctioned to leave the dentin surface moist. The primer is applied, per the manufacturer’s instructions, followed by the application of the adhesive. After gentle suctioning to control the thickness, the adhesive is light-activated. Care must be taken when using highly filled adhesives, such as All-Bond 3 and Optibond FL, to avoid pooling because this might prevent full seating of the inlay.
Seating the Inlay
The inlays are positioned into the preparations one at a time; each is lightly pressed so that excess luting composite oozes off, and the gross excess is removed with a brush. The inlays are spot-cured for 1 to 2 seconds, using a 2-mm to 4-mm–diameter light guide (eg, VALO; or DEMI™ Plus, Kerr Corp.) to secure the restorations in position (Figure 12). Because of the low light energy provided, the flowable composite reaches a gel stage, which can then be thoroughly cleaned with a sickle or a similar instrument (Figure 13). After thorough cleaning of the excess luting composite, an air-inhibiting gel is applied over the restorations and they are further light-cured for 20 seconds.
Finishing and Polishing
Although the gingival margins of the inlays exhibit superior fit, finish, and polish, the occlusal and interproximal areas tend to present margins that are slightly irregular because they cannot be finished to a seamless transition extraorally (Figure 14). Final finishing and polishing of such margins is performed with the sequential use of flexible aluminum-oxide discs until an inconspicuous transition from tooth to composite is rendered (Figure 15). Rubber finishing and polishing cups (eg, FlexiCup, Cosmedent; Astropol, Ivoclar Vivadent) used alone or associated with polishing pastes (eg, Diamond Polish Mint, Ultradent) enhance the ability to finesse the polish and remove any subgingival residue (Figure 16). Felt discs are used with polishing pastes, such as FlexiBuff and Enamelize™ (Cosmedent), respectively, as a final step to highlight the luster of the inlays (Figure 17 through Figure 19).
Discussion and Conclusion
Although the direct-indirect composite technique is not new, recent advances in materials, instrumentation, and chairside light-curing have generated renewed interest in this restorative approach given its advantages over directly placed composites. Modern composites, when effectively used, can achieve esthetics, including surface texture, shade matching, and characterization, that are similar to ceramics in many cases. Additionally, newer-generation curing lights afford energy that approximates that of laboratory-based composite processing devices. All of these advances make it possible for clinicians to obtain chairside composite inlays that are an excellent restoration choice for many cases that would otherwise be highly challenging to complete using a direct composite technique. The superior marginal finish obtained with the direct-indirect technique was confirmed by scanning electron microscopy and atomic force microscopy studies (Figure 20 through Figure 22).
The direct-indirect composite technique represents a different—and, admittedly, perhaps initially challenging—paradigm for the management of certain clinical situations. This approach is not a solution for all problems related to composite resins and certainly has its limitations, such as in situations when the tooth preparation is retentive, in which case a direct restorative technique would allow more tooth conservation. When the direct-indirect technique is used to restore small volumes of lost tooth structure, another challenge is the extraoral manipulation of the small-sized composite inlays. Nevertheless, with practice, determination, and attention to detail, clinicians may find this technique to be a worthy addition to their armamentarium.
As with any evolving clinical technique, further research is needed to determine optimal adhesive protocols for the direct-indirect composite technique and to more properly compare its marginal adaptation and clinical performance with the more traditional direct composite technique.
About the Authors
André V. Ritter, DDS, MS, MBA
Professor and Chair, Department of Operative Dentistry, University of North Carolina School of Dentistry, Chapel Hill, North Carolina
Newton Fahl, Jr., DDS, MS
Clinical and Scientific Director, Fahl Center, Curitiba, PR, Brazil; Private Practice, Curitiba, PR, Brazil
Marcos Vargas, DDS, MS
Professor, Department of Family Dentistry, University of Iowa College of Dentistry, Iowa City, Iowa
Rodrigo R. Maia, DDS, MS, PhD
Assistant Professor, Department of Operative Dentistry, University of Iowa College of Dentistry, Iowa City, Iowa
References
1. Bowen RL, inventor; Bowen RL, assignee. Dental filling material comprising vinyl silane treated fused silica and a binder consisting of the reaction product of bis phenol and glycidyl acrylate. US patent 3 066 112. November 27, 1962.
2. Cardoso MV, de Almeida Neves A, Mine A, et al. Current aspects on bonding effectiveness and stability in adhesive dentistry. Aust Dent J. 2011;56(suppl 1):31-44.
3. Fronza BM, Rueggeberg FA, Braga RR, et al. Monomer conversion, microhardness, internal marginal adaptation, and shrinkage stress of bulk-fill resin composites. Dent Mater. 2015;31(12):1542-1551.
4. Mantri SP, Mantri SS. Management of shrinkage stresses in direct restorative light-cured composites: a review. J Esthet Restor Dent. 2013;25(5):305-313.
5. Demarco FF, Collares K, Coelho-de-Souza FH, et al. Anterior composite restorations: A systematic review on long-term survival and reasons for failure. Dent Mater. 2015;31(10):1214-1224.
6. Demarco FF, Corrêa MB, Cenci MS, et al. Longevity of posterior composite restorations: not only a matter of materials. Dent Mater. 2012;28(1):87-101.
7. Carvalho RM, Manso AP, Geraldeli S, et al. Durability of bonds and clinical success of adhesive restorations. Dent Mater. 2012;28(1):72-86.
8. Birnbaum NS. Direct oven-tempered hybrid composite-resin laminate veneers. Pract Periodontics Aesthet Dent. 1992;4(5):23-31.
9. Birnbaum NS. Heat-tempered composite resin laminate veneers. Curr Opin Cosmet Dent. 1994:52-57.
10. Covey DA. Composite resin inlays. VA Dent J. 1992;69(2):30-36.
11. Fahl N Jr. The direct/indirect composite resin veneers: a case report. Pract Periodontics Aesthet Dent. 1996;8(7):627-638.
12. Fahl N Jr. Direct-indirect class V restorations: a novel approach for treating noncarious cervical lesions. J Esthet Restor Dent. 2015;27(5):267-284.
13. Dietschi D, Spreafico R. Adhesive Metal-Free Restorations: Current Concepts for the Esthetic Treatment of Posterior Teeth. Chicago, IL: Quintessence Publishing; 1997.
14. Covey DA, Tahaney SR, Davenport JM. Mechanical properties of heat-treated composite resin restorative materials. J Prosthet Dent. 1992;68(3):458-461.
15. Ferracane JL, Condon JR. Post-cure heat treatments for composites: properties and fractography. Dent Mater. 1992;8(5):290-295.
16. Ferracane JL, Mitchem JC, Condon JR, Todd R. Wear and marginal breakdown of composites with various degrees of cure. J Dent Res. 1997;76(8):1508-1516.
17. Wassell RW, McCabe JF, Walls AW. Wear rates of regular and tempered composites. J Dent. 1997;25(1):49-52.
18. Paolantonio M, D'Ercole S, Perinetti G, et al. Clinical and microbiological effects of different restorative materials on the periodontal tissues adjacent to subgingival class V restorations. J Clin Periodontol. 2004;31(3):200-207.
19. Gedik R, Hürmüzlü F, Coskun A, et al. Surface roughness of new microhybrid resin-based composites. J Am Dent Assoc. 2005;136(8):1106-1112.
20. Roeder LB, Berry EA 3rd, You C, Powers JM. Bond strength of composite to air-abraded enamel and dentin. Oper Dent. 1995;20(5):186-190.
21. Freeman R, Varanasi S, Meyers IA, Symons AL. Effect of air abrasion and thermocycling on resin adaptation and shear bond strength to dentin for an etch-and-rinse and self-etch resin adhesive. Dent Mater J. 2012;31(2):180-188.
22. Szesz A, Parreiras S, Reis A, Loguercio A. Selective enamel etching in cervical lesions for self-etch adhesives: a systematic review and meta-analysis. J Dent. 2016;53:1-11.
23. Van Meerbeek B, Kanumilli P, De Munck J, et al. A randomized controlled study evaluating the effectiveness of a two-step self-etch adhesive with and without selective phosphoric-acid etching of enamel. Dent Mater. 2005;21(4):375-383.