Options for the Esthetic Zone Using the Immediate Restoration Procedure: Observational Data of 15 Years and 5000 Implants
Paul S. Petrungaro, DDS, MS
Abstract
Dental implants have become a suitable treatment option for patients experiencing tooth loss and a popular choice among clinicians for immediate tooth replacement. Because of modifications in implant designs and development in immediate restoration and loading protocols, dental implant treatment can be reduced to a single procedure instead of multiple processes, hence providing the patient with a streamlined treatment that is typically much less invasive with immediate-tooth replacement. The purpose of this paper is to review the immediate restoration of dental implant(s) procedure and validate its position in treatment protocols by presenting success rates documented for more than 15 years and with 5000 implants. Also, recommendations for the management of different alveolar contours and defects will be presented, which have been encountered by the author when performing the immediate restoration procedure throughout this 15-year period.
As implantology continues to develop, the literature has seen an increase in the topic of immediate provisionalization of dental implants at placement; the procedure provides a suitable solution to tooth replacement in the esthetic zone, while maintaining soft-tissue emergence profiles throughout the entire placement process.1-5 Several authors4-6 have expanded the discussion to describe soft-tissue changes in relation to specific classifications of pretreatment soft-tissue parameters, and the necessity to enhance the process by the addition of a connective tissue or acellular dermal matrix graft to the procedure for single-tooth replacement in the esthetic zone. While minor differences in the immediate restoration process presented by various authors exist,1-5 the success rates show positive short-term intermediate results for the parameters of tissue maintenance, crestal-bone maintenance, and success of the implant fixture itself. The literature presents various success rates noted from 2 to 8 years7-11 in the aforementioned procedure. Also, many of these authors have previously advocated the procedure for implant sites that were free of presurgical residual infection, or sites that had not consisted of vertical/horizontal dimensional loss of the preexisting buccal plate.12-16 The reestablishment of the alveolar structures and elimination of any residual periodontal infection or granulation tissue in these types of cases were previously thought to be more critical than maintenance of the soft-tissue contours.12-16
Immediate provisionalization has continued to gain popularity for many clinicians replacing teeth in the esthetic zone. The procedure described below and its clinical success allow the clinician to perform an easy, efficient, and predictable technique.10,11,17,18
As the clinician approaches the manipulation of the buccal tissues in the immediate provisionalization in the pretreatment planning phase, it is important to realize that successful management of the various clinical situations encountered determine not only the esthetic success of the case, but also the long-term maintenance of the bone and peri-implant structures at the emergence profile/implant platform region of the implant.11,19,20 For the surgical clinician, understanding when to bone-graft the buccal plate structures, initially regenerate the alveolar structures prior to implant placement, and enhance the soft-tissue volume and knowing when additional bone replacement procedures will not be required is paramount to the long-term success of the case. This is important not only for esthetics, but also for maintaining the peri-implant environment.
The dental literature has established that for a dental implant to maintain a buccal plate environment and sound peri-implant tissues, 2 mm of bone is required around a dental implant.21 In the esthetic zone, even though this minimum of bone is required, increased zones of connective tissue/keratinized tissue are more critical to the success of peri-implant esthetics than increased amounts of bone thickness.4,5,20 The clinician should have a wide area of attached soft tissue, and this is as equally important as having a minimal thickness of the alveolar bone. Therefore, when a tooth in the esthetic zone is removed by minimally invasive (flapless) means and the extraction socket debrided, the existing buccal plate, or lack thereof, can be managed in various ways. Sanz et al22 demonstrated the labial thickness of the buccal plate is ≤1 mm or less for approximately 90% of patients,23 which generally is cortical bone. Hence, not only is this bone plate thin and consisting of fenestrations or dehiscences, but it also lacks the ability for rapid remodeling of grafted bone placed into this area for increasing bone volume on the facial aspect of the plate, inferior to the residual periosteum, or the palatal/lingual aspect of the “pouch” initially described by the author.11 For this reason, conventional thought has supported a multistep approach to replacement of the deficient buccal tissues prior to implant placement in the esthetic zone.
Adopting an immediate restoration protocol can achieve the same results as the multistep process, in respect to implant survival rate, esthetic outcomes, and most importantly, patient satisfaction, and has shown to provide more predictable soft-tissue esthetics in the smile zone than previous multistep surgical methods, over the 15-year period observed by the author in this paper.24
Allowing the implant surgeon to be more successful in the immediate restoration procedure are enhanced design features of implants commonly used in the contemporary implant practice. Recent developments in the surface coating of implant fixtures, implant-body design features of a tapered screw design, replacement of the polished titanium or surface-treated collar by implant surface coatings to the top aspect of the implant itself, and an internal hex design for improved esthetics and enhanced stability has enabled the implant surgeon to maximize the immediate restoration procedure in different classifications of bone density and quality, should the surgeon elect to perform the immediate restoration.
When performing this technique, management options for tooth replacement following extraction, or a previously edentulous site, can be described and managed by four criteria, based on residual bone present on the labial aspect of a dental implant once the implant is placed in an ideal position for emergence-profile formation. Based on these criteria, the author advocates this procedure for the management of various clinical situations in the esthetic zone, and provides a recommendation on the management of deficient contours present at the buccal surface of an implant placed into an immediate extraction socket, or residual edentulous site in the esthetic zone.
Type 1 Residual Alveolar Contour
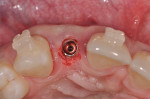
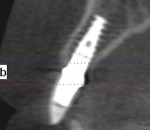
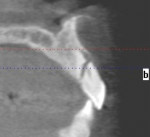
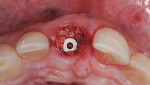
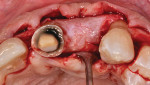
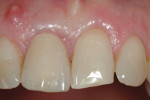
Buccal plate thickness remaining on the facial aspect of the implant placed in the correct position for proper emergence profile formation24 is ≥2 mm.21 No additional bone grafting or incision is required (based on adequate zones of keratinized attached tissue 2 mm to 3 mm in width), and soft-tissue contours may be enhanced20 (Figure 1 and Figure 2).
Type 2 Residual Alveolar Contour
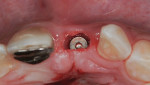
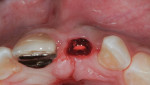
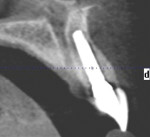
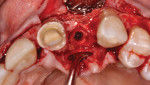
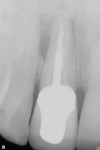
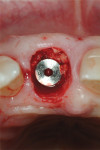
Buccal plate thickness remaining on the facial aspect of the implant placed in the correct position for proper emergence profile formation24 is 1 mm to 2 mm. A bone graft procedure is recommended, a connective-tissue replacement graft may be required,20 and membrane is recommended.11,25 The procedure can be accomplished with an incision or by minimally invasive means (flapless) and, if the technique adopted incorporates the “pouch,”3,11 created on the facial of the buccal plate, inferior to the periosteum; the residual periosteum has been observed by the author to serve as a membrane for containment of the graft complex. A membrane (resorbable collagen), connective-tissue graft, acellular dermal matrix graft, or allogenic grafting material may also be placed in the pouch space to increase the connective tissue facial to the existing buccal plate (Figure 3 and Figure 4).
Type 3 Residual Alveolar Contour
A preexisting dehiscence or fenestration is present, and/or the existing buccal plate thickness remaining on the facial aspect of the implant placed into the correct position for proper emergence profile formation24 is ≤1 mm. A bone graft/replacement procedure is recommended, a connective tissue graft may be required,20 and a membrane is recommended.14,26,27 The procedure may be accomplished by minimally invasive means; however, depending on the skill of the surgeon, it may also be accomplished by traditional flap methods. Similar to the type 2 residual alveolar defect, the pouch, if minimally invasive protocol is adopted, can serve as a contained space to place an additional bone graft, connective tissue graft, acellular dermal matrix graft, or resorbable membrane. The author also advocates, if an incision protocol is adopted, a resorbable collagen membrane can be used superior to the graft complex filling the space from the facial of the implant to the palatal aspect of the extraction socket, and over the residual facial plate present (Figure 5 through Figure 7).
Type 4 Residual Alveolar Defect
A preexisting defect is present in which both vertical and horizontal bone volume are deficient, and an implant cannot be placed into the residual ridge in the proper position to support an esthetic emergence profile.24 This procedure requires a separate bone replacement/graft procedure prior to implant placement.28-30 In addition, the author advocates an incision technique, a nonabsorbable titanium-reinforced membrane, and, when possible, an amniotic/chorionic membrane.31 This is to support rapid soft-tissue healing and maturation by providing different types of collagen and cell adhesion bioactive factors and aiding in proper alveolar reconstruction of the grafted ridge (Table 1; Figure 8 and Figure 9).
This article will discuss the success rates of more than 5000 implants placed into extraction, edentulous, and sinus-grafted sites, based on earlier reports presented by the author.3,11 These cases follow the management protocols outlined for the 4 types of residual alveolar defects remaining on the facial of an implant placed in the proper spatial arrangement in the tooth positions to be replaced with dental implants, in the esthetic zone and both the maxillary and mandibular arches. For a 15-year period, observation has been documented, in regard to implant fixture stability and long-term integration, and the success rates observed can be seen in Table 2 through Table 4.
The following case reports will demonstrate a review of the procedure for the immediate restoration of dental implants at placement originally presented by the author3,11 in three representative cases: a single-tooth immediate implant procedure in a failing/active endodontic site, with 15-year success; post-traumatic multiple tooth replacement in the esthetic zone with 4.5-year follow-up; and full-mouth immediate implant rehabilitation and loading in a “terminal dentition” with 7-year follow-up.
Case 1: Single-Tooth Replacement: Type 3 Residual Alveolar Contour
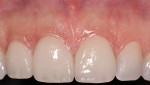
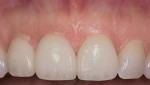
A 39-year-old nonsmoking male presented with a failing endodontically treated, fractured maxillary right central incisor. A draining sinus track was noticed at the mucogingival junction distal to the right central incisor (Figure 10). A pretreatment periapical radiograph demonstrated the large alveolar defect distal-apically (Figure 11). Clinically, the site registered a 12-mm probing depth at the distal line angle of the right central incisor. Following the technique previously outlined by the author, a preoperative administration of moxicillin and clavulanate potassium 875 mg 20 1 q 12 hours was started 1 day before the procedure. The patient was given the appropriate local anesthetic, the tooth removed, and the extraction site debrided by mechanical (curettage) and rotary instrumentation using high-speed handpiece with a round No. 6 diamond until all remnants of the periodontal ligament and granulation tissue were removed. A Tapered Screw Vent® implant (Zimmer Biomet Dental, zimmerbiometdental.com) measuring 4.7 mm x 13 mm was placed to the appropriate depth and achieved initial stabilization in the alveolar bone apical to the extraction site. An allogenic, mineralized cancellous, 1-mm to 2-mm-particle-size graft (Tutogen Medical GmbH, rtix.com) was placed into the remaining peri-implant defect, and condensed to completely fill the osseous defects and void in the preexisting buccal plate (Figure 12). A plastic provisional abutment was seated, and the preexisting full-coverage porcelain restoration was retrofitted to the plastic provisional abutment and served as the immediate provisional restoration. After a 3-month healing and maturation phase of the implant placed, the graft was inserted and the tissue was sculpted and held in place by the immediate provisional restoration, which allowed for a stable, mature soft-tissue emergence profile. The restorative clinician completed the final implant abutment and crown for the right central incisor. The patient followed regularly scheduled implant maintenance visits biannually. Figure 13 shows the 15-year post-treatment clinical view, and a 15-year post-treatment clinical view can be seen in Figure 14.
Case 2: Multiple-Tooth Replacement: Type 3 Residual Alveolar Defect
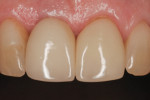
A 30-year-old, nonsmoking female presented with trauma to the anterior maxillae, avulsing both central incisors and traumatizing the right lateral incisor. The patient presented to the referring clinician and was given the options of root canal treatment, splinting and long-term stabilization, and the option of being more definitive in the treatment, removing the traumatized teeth, reconstruction of the fractured buccal plate in the premaxillae region (Figure 15), and implant placement. The patient opted for the definitive treatment, and reconstruction with dental implants. In addition, esthetics was the patient’s primary concern, as she exhibited a high smile line and excessive gingival display, which she declined to have corrected. The patient also chose the minimally invasive immediate restoration protocol and a stable, immediate provisional restoration for teeth Nos. 7 through 9.
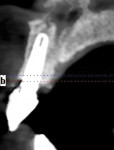
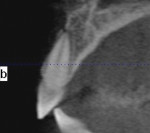
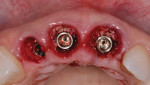
Following the technique for immediate extraction, immediate implant placement and provisionalization procedures outlined previously, the patient had teeth Nos. 7 through 9 removed by atraumatic, minimally invasive means, debridement was accomplished, and 3 implants were placed: a NobelActive implant (Nobel Biocare, nobelbiocare.com) measuring 3.5 mm x 11.5 mm at No. 7; and 2 NobelActive implants measuring 3.5 mm x 13.5 mm placed at Nos. 8 and 9 respectively, with each implant obtaining an ISQ of 50 Ncm at placement. Implant placement was accomplished by a minimally invasive (flapless) protocol. Reconstruction of the missing buccal plate in the region of teeth Nos. 7 through 9 was accomplished once again by an allogenic, mineralized, cancellous 1-mm to 2-mm-particle-size bone graft (LifeNet Health, lifenethealth.org) condensed into the peri-implant defects, to the level of the crest of the bone-level NobelActive implant (Figure 16). Provisional QuickTemp Abutment Conical Connection (Nobel Biocare) were screwed into place, and an immediate provisional restoration constructed from the retrofitted TempStent II surgical guide32 provisionalization system. The provisional restoration was cemented with Temp-Bond™ Clear (Kerr, kerrdental.com), and the excess cement was removed. The patient was allowed to follow a 3-month healing and observation period after which fixture-level impressions were obtained and computer-aided design and computer-aided manufacturing custom-milled zirconia abutments were constructed. This was followed by a second set of provisional restorations the patient utilized for an additional 2 months. Final impressions were taken of the zirconia abutments, and final all-ceramic restorations were constructed and cemented into place. The case’s complete clinical view can be seen in Figure 17. Figure 18 shows the 4.5-year post-treatment clinical view, while Figure 19 shows the 4.5-year post treatment computed tomography (CT) scan serial view. Please note that the total reconstruction of the buccal bone structures achieved by the minimally invasive bone graft procedure was accomplished following the technique previously outlined.
Case 3 Multiple Tooth Replacement:Extraction Sockets Type 2 and 3 Residual Alveolar Defects: Edentulous Sites, Type 1 Residual Alveolar Defects
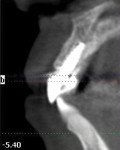
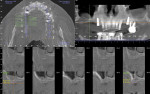
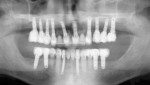
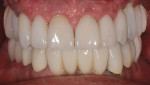
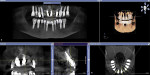
A 49-year-old nonsmoking male presented for treatment of his advanced tooth loss, terminal dentition, residual infection after dental treatment, and recurrent sinus infections. His dental history consisted of multiple attempts at conventional treatment approaches to prolong tooth longevity, several implant procedures to replace failing endodontically treated teeth and edentulous sites (all resulting in repeated failure of treatment), compromised esthetics, and various secondary infectious diseases related to previous failures of dental treatment. The pretreatment CT scan view of the maxillae and several serial views (Figure 20) demonstrated multiple edentulous sites, residual sinus infections, failing implant procedures with large alveolar defects, and the remaining dentition, which can be classified as a “terminal dentition.” After reviewing multiple treatment options with the patient ranging from conventional fixed and removable options, to partial implant reconstruction with extensive bone replacement procedures recommended, the patient opted for removal of most of the remaining dentition, correction of sinus pathology, multiple implant placement, and immediate provisionalization procedures, most accomplished by a conservative, minimally invasive protocol (except for the sinus regions, which required flap access and a lateral-wall osteotomy), and immediate loading of the implants at the initial and only surgical procedure planned. After extensive medical and dental histories were taken, medical clearance for the preexisting sinus infections was obtained, and a complete dental workup consisting of a facebow transfer, mounted maxillary and mandibular pretreatment models, a complete diagnostic waxup of both the hard and soft tissues required to be replaced, and construction of the TempStent II surgical guide and provisionalization system, the patient was given an appointment for the complex surgical visit. During this surgery, remaining dentition and implants were removed, ten implants in the maxillary arch were inserted, and bilateral sinus elevations and alveolar reconstruction was performed along with peri-implant bone grafting and immediate provisionalization. In the mandibular arch, removal of the remaining dentition was done, except for teeth Nos. 21, 22, 27, and 28, and six implants were placed and immediately provisionalized, keeping the patient in the planned first-molar occlusion scheme. The immediate post-treatment panoramic view can be seen in Figure 21. After an uneventful healing for 4.5 months, the patient then initiated the final reconstructive phase of his treatment. A 7-year post-treatment clinical view can be seen in Figure 22, with the 7-year post-treatment CT panoramic scan, axial and serial views of the maxillary central incisor seen in Figure 23.
Conclusion
The immediate restoration, and/or loading of dental implants at the initial placement procedure, has been shown to streamline the implant treatment process, decrease healing and maturation times, and allows patients to have immediate, stable, and esthetic provisional restorations. When compared with the success rates of the conventional multistep implant process,33,34 this technique provides favorable and consistent success rates over long-term post-treatment timeframes.7-11 Conventional treatment procedures recommending conservative approaches to tooth removal and active peri-tooth infections provide for assurance in the debridement and reconstruction of the void remaining in the alveolar housing of the extraction socket. Allowing for extended healing times, multiple surgical visits, and commonly compromised soft-tissue esthetics due to the multiple incision and suturing procedures has shown to be successful long term in regard to the implant fixture itself. However, the implant team may also consider more contemporary protocols of immediate restoration, minimally invasive surgical techniques, and immediate loading protocols that can produce highly successful results in shorter treatment times and fewer surgical/prosthetic appointments. The author has advocated the surgical procedure outlined in this paper over a 15-year-plus time frame, which has demonstrated highly successful results. He proposes the outlined method for the management of deficient buccal plate thickness for type 1, 2, and/or 3 classifications as outlined in the text, at the labial aspect of dental implants not only in the esthetic zone, but in all areas requiring tooth replacement with implants.
About The Author
Paul S. Petrungaro, DDS, MS
Private Practice
Periodontics and Implantology
Chicago, Illinois
Founder and Director
The Implant Learning Center
Chicago, Illinois
References
1. Saadoun AP, Le Gall MG. Periodontal implications in implant treatment planning for aesthetic results. Pract Periodontics Aesthet Dent. 1998;10(5):655-664.
2. Petrungaro PS. Immediate restoration of dental implants in the aesthetic zone. Dent Implantol Update. 2001;12(12):89-95.
3. Petrungaro PS. Implant placement and provisionalization in extraction, edentulous, and sinus grafted sites: a clinical report on 1500 sites. Compend Contin Educ Dent. 2005;26(132):879-890.
4. Kan JY, Rungcharassaeng K, Morimoto T, Lozada JL. Facial gingival tissue stability after connective tissue graft with single immediate tooth replacement in the esthetic zone: consecutive case report. J Oral Maxillofac Surg. 2009;67(suppl 11):40-48.
5. Kan JY, Rungcharassaeng K, Lozada J. Bilaminar subepithelial connective tissue grafts for immediate implant placement and provisionalization in the esthetic zone. J Calif Dent Assoc. 2005;33(11):865-871.
6. Kan JY, Morimoto T, Rungcharassaeng K, et al. Gingival biotype assessment in the esthetic zone: visual versus direct measurement. Int J Periodontics Restorative Dent. 2010;30(3):237-243.
7. Roe P, Kan JY, Rungcharassaeng K, et al. Horizontal and vertical dimensional changes of peri-implant facial bone following immediate placement and provisionalization of maxillary anterior single implants: a 1 year cone beam computed tomography study. Int J Oral Maxillofac Implants. 2012;27(2):393-400.
8. Kan JY, Rungcharassaeng K. Lozada J. Immediate placement and provisionalization of maxillary anterior single implants: 1 year prospective study. Int J Oral Maxillofac Implants. 2003;18(1):31-39.
9. Tortamano P, Camargo LO, Bello-Silva MS, Kanashiro LH. Immediate implant placement and restoration in the esthetic zone: a prospective study with 18 months of follow-up. Int J Oral Maxillofac Implants. 2010;25(2):345-350.
10. Wohrle PS. Single-tooth replacement in the aesthetic zone with immediate provisionalization: fourteen consecutive case reports. Pract Periodontics Aesthet Dent. 1998;10(9):1107-1114.
11. Petrungaro PS. An update on implant placement and provisionalization in extraction, edentulous and sinus grafted sites: a clinical report on 3200 sites over 8 years. Compend Contin Educ Dent. 2008;29(5):288-294, 296, 298-300.
12. Araujo MG, Lindhe J. Ridge alterations following tooth extraction with and without flap elevation: an experimental study in the dog. Clin Oral Implants Res. 2009;20(6):545-549.
13. Becker W, Goldstein M. Immediate implant placement: treatment planning and surgical steps for successful outcome. Periodontol 2000. 2008;47:78-89.
14. Elian N, Cho SC, Froum S, et al. A simplified socket classification and repair technique. Pract Proced Aesthet Dent. 2007;19(2):99-104.
15. Block MS, Mercante DE, Lirette D, et al. Prospective evaluation of immediate and delayed provisional single tooth restorations. J Oral Maxillofac Surg. 2009;67(suppl 11):89-107.
16. Jung RE, Zaugg B, Philipp AO, et al. A prospective, controlled clinical trial evaluating the clinical radiological and aesthetic outcome after 5 years of immediately placed implants in sockets exhibiting periapical pathology. Clin Oral Implants Res. 2013;24(8):839-846.
17. Petrungaro PS. Immediate implant placement and provisionalization in edentulous, extraction and sinus grafted sites. Compend Contin Educ Dent. 2003;24(2):95-113.
18. De Rouck T, Collys K, Wyn I, Cosyn J. Instant provisionalization of immediate single-tooth implants is essential to optimize esthetic treatment outcome. Clin Oral Implants Res. 2009;20(6):566-570.
19. Tarnow DP, Chu SJ, Salama MA, et al. Flapless postextraction socket implant placement in the esthetic zone: part 1. The effect of bone grafting and/or provisional restoration on facial-palatal ridge dimension change-a retrospective cohort study. Int J Periodontics Restorative Dent. 2014;34(3):323-331.
20. Rungcharassaeng K, Kan JY, Yoshino S, et al. Immediate implant placement and provisionalization with and without a connective tissue graft: an analysis of facial gingival tissue thickness. Int J Periodontics Restorative Dent. 2012;32(6):657-663.
21. Merheb J, Quirynen M, Teughels W. Critical buccal bone dimensions along implants. Periodontol 2000. 2014;66(1):97-105.
22. Sanz M, Cecchinato D, Ferrus J, et al. A prospective, randomized-controlled clinical trial to evaluate bone preservation using implants with different geometry placed into extraction sockets in the maxilla. Clin Oral Implants Res. 2010;21(1):13-21.
23. Petrungaro PS. Immediate restoration of dental implant sin the aethsetic zone utilizing a flapless approach to preserve interdental contours. Pract Periodon Aesthet Dent. 2005;17(2):151-158.
24. Petrungaro PS. Maintaining and creating natural soft tissue contours and emergence profiles around dental implants. J Cosmetic Dent. 2012;28:142-152.
25. Petrungaro PS. Recreating balance, harmony, and symmetry in the gingival complex in conjunction with immediate implant placement and restoration. J Cosmetic Dent. 2010;26(2):97-106.
26. Petrungaro PS. The formation of interdental bone contours and tissue emergence profiles in aesthetic implant cases. Contemp Esthet Rest Pract. 2000;4(5)20-28.
27. Petrungaro PS. Bone grafting at the time of extraction: a new technique for achieving natural bone and tissue contours in esthetic tooth replacement. J Cosmetic Dent. 2000;16(2)30-43.
28. Buser D, Ingimarsson S, Dula K, et al. Long-term stability of osseointegrated implants in augmented bone: A 5 year prospective study in partially edentulous patients. Int J Periodontics Restorative Dent. 2002;22(2)109-117.
29. Degidi M, Scaran A, Piattelli A. Regeneration of the alveolar crest using titanium micromesh with autologous bone and a resorbable membrane. J Oral Implantol. 2003;29(2):86-90.
30. Simion M, Jovanovic SA, Benfenati SP. Long-term of osseointegrated implants inserted at the time or after vertical ridge augmentation. A retrospective study on 123 implants with 1-5 year follow-up. Clin Oral Implants Res. 2001;12(1)35-45.
31. Petrungaro PS. Stem cell block grafts. Implant Practice. 2013;6(6):22-24.
32. Petrungaro PS. The TempStent™ surgical guide provisionalization method for immediate restoration for dental implants. Contemp Esthet Rest Pract. 2002;6(5)84-90.
33. Adell R, Lekholm U, Rockler B, Brånemark PI. A 15-year study of osseointegrated implants in the treatment of the edentulous jaw. Int J Oral Surg. 1981;10(6):387-416.
34. Adell R, Eriksson B, Lekholm U, et al. Long-term follow-up study of osseointegrated implants in the treatment of totally edentulous jaws. Int J Oral Maxillofac Implants. 1990;5(4):347-359.