Digital Dentures: Efficient, Well-fitting Solutions for Edentulous Patients—A Case Report
Jean G. Furuyama, DDS, FAGD
Abstract:
Despite overall better health trends, edentulism remains a serious health issue, and not every patient with edentulism is a candidate for implants. Digitally designed and manufactured dentures provide well-fitting, comfortable prostheses with improved occlusion. In addition, with the use of new innovative impression trays, final impressions and vertical dimension and centric relation records can be taken on the first visit. This results in the denture being able to be delivered in only two or three visits, thus drastically cutting down on chairtime and improving efficiency. This case report describes the record-taking and delivery of a digitally designed and milled full upper denture.
Dental-licensure examinations in the United States no longer require students to set denture teeth or even take denture impressions, according to the Council of Interstate Testing Agencies. Dental schools now have so many other subjects to teach that little time is devoted to providing instruction on dentures. Theoretically, because more people are keeping their natural teeth longer, fewer people have edentulism and those who have edentulism will probably be best served with implants.1
Edentulism rates have decreased, with the most recent Centers for Disease Control and Prevention survey showing a decline from 18% of the general dental population in 1958 to 4% in 2010.2 Nonetheless, according to the American College of Prosthodontists, more than 35 million people are fully edentulous.3 Among the various reasons for edentulism is patients with lower incomes being unable to afford needed restorative treatment, which often leads to extraction as the solution of choice. Living in a rural environment is another predictor of edentulism because patients often have to travel far for dental treatment.4
In addition, even among patients with edentulism who have greater disposable income, not all are candidates for implants. These include patients with uncontrolled diabetes, heavy smoking habits, alcohol abuse, immune deficiency issues, or a history of intravenous bisphosphonate treatment.5
The 65-and-older demographic represents the highest percentage of denture wearers6,7 with 23 million being completely edentulous.3 As the baby-boomer generation swells, so will the actual number of patients needing dentures.8 With only 3372 prosthodontists in the United States, an inadequate amount of specialists will be available to meet the need.9 General dentists will also have to serve the edentulous community.
In academia, the challenge regarding full dentures is that dental schools are faced with the dilemma of needing to teach students a procedure that has been deprioritized. A CAD/CAM solution may help dental students once they’re out in the “real world” in which fewer laboratory technicians are proficient at fabricating dentures.10,11 A modern, digitized, simplified method to produce dentures at least as good as conventionally fabricated dentures could be worthwhile for engaging students and re-engaging experienced general dentists.
A New Solution for Dentures
In 2007, Tae Kim, DDS, Chair of Removal Prosthodontics at Herman Ostrow School of Dentistry, University of Southern California, worked with six of his colleagues to both simplify the denture-making process and produce a better-fitting and better-functioning denture. They engineered a unique impression tray that enabled even beginning students to take excellent impressions and records in one visit. In addition, they developed the software to design a denture based on a 3-dimensional (3D) scan of the impression. Kim and his colleagues patented the system and formed DENTCA Inc. (dentca.com). Recognizing the potential of DENTCA’s trays and software, Mitsui Chemicals, Inc. (of Japan) (www.mitsuichem.com/index.htm) acquired DENTCA in 2013 and in 2015 established Whole You, Inc. (wholeyou.com), a subsidiary to market and manufacture CAD/CAM dentures, bringing together DENTCA’s technology and Mitsui Chemicals’ materials expertise.
Four features of the Whole You DENTCA impression trays make them unique. First, the trays are underextended at the borders, which allows dentists to take accurate functional impressions on the first visit. Second, the upper and lower trays can be separated at the distal aspect of the impression, which allows free movement of the lower jaw when the impressions are put back in the mouth for determining vertical dimension (VD) and centric relation (CR). Third, the upper tray has a flat platform, called a registration plate, on the palate that is used to take an intraoral Gothic arch tracing on the first visit, thus eliminating the need for taking facebows or wax bite records. Fourth, the lower trays have an attachable dual-purpose pin that rotates up and down to determine VD and then CR as the patient moves back and forth to scribe the Gothic arch tracing on the upper registration plate. If the denture is a single arch, this pin is attached to a single-arch attachment instead of an impression tray and the attachment is placed on the opposing arch and held in place with polyvinyl bite material.
Case Report
A 66-year-old Caucasian woman presented to receive a new full upper denture. On the lower jaw, she had implants on her right and left molars and natural teeth anterior to the implants. Her medical history was noncontributory, and she was in good general health. Her mucosa was pink and firm.
Impression-Taking
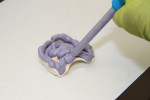
Initially, a medium-sized Whole You DENTCA impression tray was selected. When the preliminary heavy-bodied impression was taken, the lateral borders of the tray were too far away from the ridge, so a new heavy-bodied impression was taken with a small tray. In taking the impression, care was given to putting adequate impression material in the posterior portion of the tray because the hamular notches are critical for retention (Figure 1).
With the heavy-bodied polyvinyl siloxane (PVS) applied to the entire tray, border molding was performed. To achieve this, the patient was instructed to: open her mouth as wide as possible, move her lower jaw from side to side, purse her lips as though she was sucking on a straw, smile as wide as possible, and relax her cheeks so they could be pulled out and down. Border molding was repeated about three times.
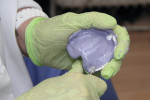
Even with the underextended DENTCA tray, the tray was visible in some areas of the impression (Figure 2). These areas were relieved using an acrylic bur (Figure 3). A thin layer of light-bodied PVS was then evenly spread over the impression while the assistant dried off the palatal tissue. The tray was reinserted and the patient instructed to repeat the border molding three or four times. If the wash had not been completely satisfactory, a second wash could have been taken as long as the tray was completely seated and the border molding repeated.
A counter impression was taken in alginate and poured up immediately (which is required for single-arch cases). A single-arch attachment with the aforementioned pin was then seated on the lower teeth using bite material to stabilize the platform.
Recording Vertical Dimension and Centric Relation
To remove interferences and ensure free range of motion while recording VD and CR, the distal part of the upper impression was sectioned and removed. As a guide, a Thompson stick was used to draw a line across the PVS approximately where the tray separates (Figure 4). This made it easier to cut in one clean swipe across the impression (Figure 5). The distal segment was then set aside. When scanned at Whole You, the anterior of the impression would be reconnected.
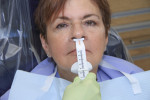
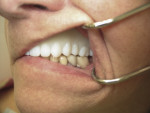
The preliminary VD was established by inserting the old denture into the mouth and measuring with the Whole You Jaw Gauge (Figure 6). Because the jaw gauge measures from the base of the nose to the chin, the VD measurement is reproducible between visits and the process is easier than using dots on the nose and chin. The upper impression that was sectioned and the lower platform with the pin were reseated in the patient’s mouth. When the patient closed, the pin rested against the tray’s registration plate. At proper vertical, relaxed lips should touch comfortably; to achieve this, the pin can be rotated up or down. After adjustments, visually observing the lip drape confirmed the correct VD was achieved and the patient was comfortable. The gauge was then used to recheck the VD from the previous denture. If the VD needed to be increased because of wear on the old denture, the gauge would have shown how many millimeters the bite was opened when the patient was resting comfortably.
Next, CR was determined by taking a Gothic arch tracing using the pin on the lower arch to scribe an arrow on the registration plate. In this case, Occlude® (Pascal International, Inc., pascalinternational.net) was applied to the registration plate to record the tracing (Figure 7). The patient was instructed to move her lower jaw back and forth several times and to stop at the retruded position before making lateral excursions. A No. 6 bur was used to place a divot at the apex of the arrow. The patient was then instructed to close and find the divot but not to bite too hard. Polyvinyl siloxane bite material was injected bilaterally to join the upper and lower elements, which were then removed and sterilized along with the distal segment prior to sending them to Whole You.
To conclude the first appointment, a lip measurement was taken and recorded using the Whole You Lip Ruler with the lips at rest. This measurement helps the software determine where to place the incisal edges of anterior teeth.
Try-In Evaluation and Prosthesis Delivery
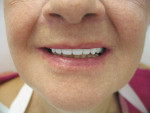
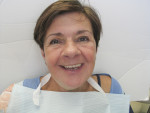
The second visit was to evaluate the try-in (Figure 8). Because the try-in was a 3D-printed version of the final denture, it fit exactly as the final denture would, making it possible to test phonetics, fit, and function far better than could have been accomplished with wax base plates. If the fit needed any correction, a wash could have been taken directly in the denture and any occlusal or minor border adjustments could have been done on the printed try-in. Articulation paper was used to check the occlusal contact points, and the jaw gauge was used to check that the VD was the same as originally measured. Finally, the patient was given a mirror to verify that she was pleased with the esthetics (Figure 9 and Figure 10).
The third visit was for the delivery of the prosthesis. Only slight occlusal adjustments were needed, and no adjustments were made on the borders or the intaglio of the denture. When the patient returned for a postinsertion follow-up, she had no sore spots and no additional adjustments were needed. This was presumably due to the lack of polymerization shrinkage, which is a distinct advantage of milled dentures. The patient was happy with the esthetics and fit (Figure 11).
Discussion
Providing traditional dentures requires five visits and at least 4 hours of chairtime for fabrication, with each step having the potential to introduce some measure of inaccuracy. Rudd12 listed 243 opportunities for errors in the fabrication of a removable partial denture. With digital dentures, all records are taken in the first visit. Theoretically, fewer steps mean fewer risks for mistakes and a shorter treatment time. The first visit typically requires approximately 45 to 90 minutes. The second visit is short; because of the accuracy of the fit of the try-in, speech, esthetics, and function can be easily verified, and any changes can usually be corrected relatively easily. In addition, the delivery visit is typically briefer than with traditional dentures. Overall, less chairtime is beneficial for the patient, dentist, and practice.
Even with partially automated systems on the market—for example, the base is 3D printed and the denture teeth are digitally placed in wax—more accurate results can be achieved, with reports of reset rates being less than half compared with those of conventional dentures.13
Conclusion
Digital methods have revolutionized denture delivery. Not only are the procedures easier for the dentist, but they produce more accurate results. Also, less chairtime translates into higher productivity. Without having to resort to the tedious methods learned in dental school, younger dentists will be able to provide dentures for more patients, and established dentists will find offering dentures to be more profitable and enjoyable.
Disclosure:
Dr. Furuyama is a consultant for and has received honorarium from Whole You, Inc.
About The Author:
Jean G. Furuyama, DDS, FAGD
Private Practice
New York, New York
References
1. Alfano MC. Hedge our bet or trim our hedge: the need to reform the dental education process. New York University College of Dentistry Global Health Nexus. 2004;6(2):16-21.
2. Centers for Disease Control and Prevention. Summary Health Statistics for U.S. Adults: National Health Interview Survey, 2010. https://www.cdc.gov/nchs/data/series/sr_10/sr10_252.pdf. January 2012. Accessed July 15, 2016.
3. Facts & Figures. Prosthodontists. American College of Prosthodontists website. https://www.gotoapro.org/facts-figures/. Accessed September 26, 2016.
4. Samen DM, Lemieux A, Arevalo O, Lutfiyya MN. A population-based study of edentulism in the US: does depression and rural residency matter after controlling for potential confounders? BMC Public Health. 2014;14:65 doi: 10.1186/1471-2458-14-65.
5. Hwang D, Wang HL. Medical contraindications to implant therapy: part I: absolute contradictions. Implant Dent. 2006;15(4):353-360.
6. Dye B, Li X, Beltrán-Aguilar ED. Selected Oral Health Indicators in the United States, 2005–2008. Hyattsville, MD: US Dept of Health and Human Services, Centers for Disease Control; May 2012. NCHS Data Brief, No. 96.
7. Dye B, Thornton-Evans G, Li X, Iafolla TJ. Dental Caries and Tooth Loss in Adults in the United States, 2011–2012. Hyattsville, MD: US Dept of Health and Human Services, Centers for Disease Control; May 2015. NCHS Data Brief, No. 197.
8. Douglass CW, Shih A, Ostry L. Will there be a need for complete dentures in the United States in 2020? J Prosthet Dent. 2002;87(1):5-8.
9. Waldman HB, Perlman SP, Xu L. Should the teaching of full denture prosthetics be maintained in schools of dentistry? J Dent Educ. 2007;71(4):463-466.
10. Haden NK, Morr KE, Valachovic RW. Trends in allied dental education: an analysis of the past and a look to the future. J Dent Educ. 2001;65(5):480-495.
11. Zamanian K, Wong J. New technologies guide paradigm shifts in dental prosthetics industry. Dental Tribune website. January 30, 2012. www.dental-tribune.com/articles/business/usa/7335_new_technologies_guide_paradigm_shifts_in_dental_prosthetics_industries.html. Accessed September 26, 2016.
12. Rudd RW, Rudd, KD. A review of 243 errors possible during fabrication of a removable partial denture: part I. J Prosthet Dent. 2001;86(3):251-261.
13. Morales D, Truong N. A digital spin on traditional dentures. Chairside Magazine website. 2016;11(1).Document16 https://glidewelldental.com/education/chairside-dental-magazine/volume-11-issue-1/digital-spin-traditional-dentures/. Accessed September 26, 2016.