Key Parameters of Hybrid Materials for CAD/CAM-Based Restorative Dentistry
Sebastian D. Horvath, Dr. med. dent.
Abstract: Hybrid materials are a recent addition to the dental armamentarium for computer-assisted design/computer-assisted manufacturing (CAD/CAM)-based restorative dentistry. They are intended to provide dentists with the capability of restoring single teeth in one appointment with a material that emulates the structure and physical properties of natural teeth. This article aims to provide an overview of currently available hybrid materials and offer the reader further understanding of their key clinical parameters and possible limitations.
The first dental computer-assisted design/computer-assisted manufacturing (CAD/CAM) system was developed with the goal of providing patients with long-lasting, esthetic restoration in a single appointment. Since the first such treatment was performed in 1985, this technology has revolutionized the way dentistry is performed. In the pioneering years, feldspar ceramic blocks were the restorative material of choice, as this materials class best matched the desired physical properties. Both the technology and the material performed well clinically, with survival rates of 90% after 10 years.1 Among failed ceramic restorations, materials fractures emerged as the biggest problem.1,2
While strong, ceramics are brittle with a low fracture toughness and a high susceptibility to failure in the presence of flaws.3 To overcome this problem, two diametrically opposed solutions were pursued. One was the development of tougher materials, such as lithium-disilicate glass-ceramics, which show higher clinical survival rates than feldspar ceramics.4 The enhanced toughness, however, makes it necessary to mill these materials in a presintered stage. The ensuing firing process, in turn, makes it difficult to complete the treatment in a single appointment. Furthermore, the manual nature of the processing can potentially lead to errors and reduce the quality of the final product.
The other solution to prevent fractures was to use a more flexible material. The developments in this direction were founded on polymer-based resin-composite materials’ ability to overcome the limitations of the aforementioned ceramic materials with regard to curing shrinkage, low mechanical properties, and poor wear resistance.5
Hybrid Materials
This breed of materials has been referred to by myriad names both by the manufacturers and in the dental literature.3,5 This is perhaps because of the different compositions and methods of manufacturing used, as well as the relative infancy of this product category. Due to their hybridity with regard to the combination of ceramic and polymer materials and the common goal to combine the positive effects of ceramics and resin-based materials, this article will refer to this materials family as “hybrid” materials. This materials family may be further subdivided into materials that are based on resins, which will be referred to as CAD/CAM composite resin, and those that are based on ceramics, which will be referred to as hybrid ceramic.
The first commercially available material considered a “hybrid” was Paradigm™ MZ100 (3M ESPE, 3mespe.com). Though initially not truly a result of a combination of materials, Paradigm MZ100 was achieved through industrialized polymerization of the Z100 (3M ESPE) direct composite. Combined light and heat polymerization under high pressure led to a significant improvement of the properties of composite resin.6,7 Consequently, Paradigm MZ100 demonstrated superior physical properties to Z100.3,7 The material was subsequently developed further, and Lava™ Ultimate (3M ESPE) emerged with slightly superior physical properties.8 Lava Ultimate and two other recent additions to the hybrid category, GC Cerasmart™ (GC Corp., gc-dental.com) and Shofu Block HC (Shofu Dental, shofu.com), are comprised of nanoceramic particles embedded in a highly cured resin matrix.9,10
Based on the knowledge of the glass-infiltrated ceramic systems it pioneered, the VITA company developed Vita Enamic® (VITA Zahnfabrik, vita-zahnfabrik.com), a resin composite that is obtained via the infiltration of a presintered ceramic network with a monomer mixture. In the true sense of the term hybrid, the processes for ceramic fabrication and composite resin fabrication were joined. Through this, a higher-volume fraction filler was achieved.11
Materials Properties and Their Respective Implications
Currently available hybrid materials are outlined in Table 1.12 Table 2 shows selected mechanical properties of hybrid materials, a feldspar ceramic, a lithium-disilicate glass-ceramic, adhesive luting cements, and human dentin and enamel.5,9,13-16 As seen in Table 2, the flexural modulus of Vita Enamic is closer to that of human dentin compared to the feldspar ceramic and lithium-disilicate glass-ceramic, which demonstrate a flexural modulus closer to that of enamel.
Because the elastic modulus of hybrid materials is more similar to the elastic modulus of dentin and adhesive luting cements, a more uniform stress distribution in the system during loading may be anticipated for hybrid-materials restorations.17,18 The flexural strength of hybrid materials CAD/CAM blocks is higher than that of recently developed nanofilled composite resins.19 This can be attributed to the factory polymerization involving heat and pressure, as well as the high filler load.
An investigation of the hardness of Vita Enamic also demonstrated values closer to dentin than the higher hardness values of enamel and traditional veneering ceramics.11 Thus, no excessive antagonist wear can be observed,20 which is a concern using conventional ceramics.21
Wedge-shaped Vita Enamic specimens milled with a Sirona MC XL milling unit (Dentsply Sirona, dentsplysirona.com) showed a better marginal fit and less avulsions than specimens of conventional CAD/CAM materials.22 This can be ascribed to the polymer component and is important for the clinical fit of restorations, including those that are minimally invasive. Furthermore, the reduced hardness leads to more rapid machining and less wear of CAD/CAM instruments.5
Vita Enamic shows an indentation deformation ability similar to human enamel, though it lacks enamel’s ability to recover after unloading. Traditional ceramic materials do not deform at all. This implies a better stress redistribution ability under use when compared with traditional ceramic materials.5
CAD/CAM machining, clinical adjustments, and normal use can lead to cracks in restorations. In an investigation on the milling-induced strength reduction of CAD/CAM materials, Vita Enamic demonstrated a lower loss of strength than feldspar ceramics and lithium-disilicate glass ceramics.23 A scanning electron microscopy (SEM) evaluation of cracks induced in Vita Enamic revealed that cracks run through the ceramic parts but are deflected at the polymer–ceramic interfaces. This behavior results in a damage tolerance of the material, which suggests local damage will be less likely to result in a chipping-induced failure of the restoration.11
Adequate polishing of restorations is critical to remove surface defects caused by machining and to establish high gloss and low surface roughness. Hybrid materials, especially CAD/CAM composite resin, can be polished more easily than traditional ceramic.24
In the author’s experience, similar to glass-ceramics, hybrid materials adapt to the color of the underlying tooth substance, which typically leads to a good esthetic integration. However, because the materials are monolithic, the esthetic result is inferior to laboratory-produced restorations. While a customization of the materials is possible using composite resin or painting techniques, it should be noted that the restorations then lose their monolithic composition and the advantages associated with it.
Unlike some partially sintered CAD/CAM materials that require additional firing, hybrid materials are milled in the final stage. This makes the materials good candidates for single-tooth restorations that are to be concluded in a single appointment. To date, manufacturers have provided the range of indications for hybrid materials for use in inlays, onlays, laminate veneers, full-crown restorations, and implant-supported restorations. However, in 2015 3M ESPE chose to remove the crown indication for Lava Ultimate due to a reported heightened debonding rate of said restorations.25 Suffice it to say that clinicians must be careful with full-coverage crown restorations using resin materials.
The bond of the restoration to the tooth is essential for the survival of all restorations. Due to the relative novelty of hybrid materials, the author has found no clear bonding protocols in the dental literature. With the evidence available thus far, it may be recommended to subject resin to air-particle abrasion and silane treatment prior to bonding, whereas hybrid ceramics can be pretreated through hydrofluoric-acid etching and silane application because of their ceramic substructure.26
Case Presentation
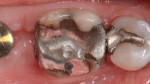
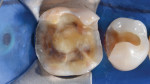
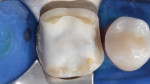
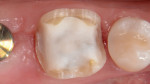
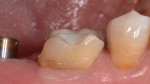
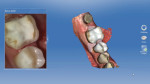
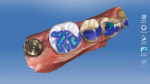
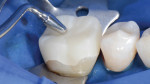
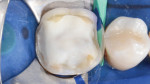
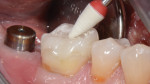
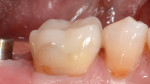
A 47-year-old woman presented with occasional pain and hypersensitivity of her lower right first molar. Findings from the clinical examination revealed insufficient amalgam restorations on her lower right first molar and second premolar (Figure 1). Both teeth were vital. The lower right quadrant was isolated (OptraDam, Ivoclar Vivadent, ivoclarvivadent.com) and the old restorations were removed (Figure 2). The tooth surfaces were cleaned with an air-polishing unit. To achieve a good esthetic integration of the final restoration, discolored dentin areas were covered with an opaque build-up restoration (LuxaCore®, DMG, dmg-dental.com) (Figure 3). The adjacent second premolar was restored using a direct resin composite (Filtek™ Supreme XTE, 3M ESPE). Subsequently, the first molar was prepared according to the guidelines for all-ceramic CAD/CAM restorations27 (Figure 4 and Figure 5). A digital impression was performed (CEREC Omnicam, Dentsply Sirona) (Figure 6), and the final restoration was planned (CEREC Software 4.3.1, Dentsply Sirona) (Figure 7).
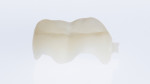
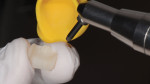
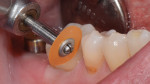
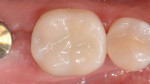
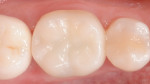
For a restorative material, the CAD/CAM composite resin Lava Ultimate was selected (Figure 8). The milled restoration was checked for fit (Figure 9) and subsequently prepared for bonding. To roughen the surface, the part of the restoration facing the tooth was air abraded with aluminum-oxide particles with a particle size of 50 μm (Figure 10). The restoration was cleaned using alcohol and a silane (GC Ceramic Primer, GC Corp.) applied to the bonding surface. Subsequently, the abutment tooth was prepared for bonding (Figure 11). The enamel was selectively conditioned. The tooth was rinsed and dried, and a desensitizer (Telio CS Desensitizer, Ivoclar Vivadent) was applied to the dentin areas. An adhesive (Scotchbond™ Universal Adhesive, 3M ESPE) was applied to the restoration and the tooth surfaces, and the restoration was cemented using a resin cement (RelyX™ Ultimate, 3M ESPE). The restoration was checked for occlusal and proximal contacts and subsequently polished (Figure 12 and Figure 13). Figure 14 and Figure 15 show the final restoration on the day of bonding, and Figure 16 demonstrates the restoration 1 year later.
Performance of Hybrid Materials
Due to the relative novelty of this product family, both in vitro and in vivo data on their performance are scarce, much like other CAD/CAM materials that are in their infancy. The promising material properties, however, should lead to an increased clinical use of these materials in dental offices. Thus, independent studies on the clinical performance of these materials are urgently needed.
The studies cited in this article are focused on hybrid materials for CAD/CAM use. Results on the performance of manually fabricated indirect composites were omitted because these materials significantly differ from the new CAD/CAM materials.
In in vitro studies, CAD/CAM composite resin occlusal veneers (Paradigm MZ100) showed a significantly increased survival rate when compared with those made of reinforced ceramics (IPS Empress and e.max® CAD, Ivoclar Vivadent)28,29 and an increased fatigue resistance in endodontically treated teeth when compared with teeth restored with a feldspar porcelain (Vita Mark II).30 The maximal loads at fracture for CAD/CAM composite resin restorations (Lava Ultimate) were found to exceed human masticatory forces, even at a thickness of 0.3 mm.8
In a study, 7-day water storage and thermocycling negatively affected the mechanical properties of CAD/CAM composite resin blocks and e.max, whereas the hybrid ceramic material and the feldspar ceramic material were not affected (Table 2).9 Water penetrated the resin matrix of the resin blocks, which, in turn, led to a softening of the polymer.31,32 Furthermore, the absorbed water may have caused hydrolysis of the silane coupling agent.33 The effect was highest in the materials using zirconium silicate as filler particle. This may be attributed to the fact that zirconium silicate cannot be effectively silanized due to the high crystalline content.33
Abrasive tooth brushing was found to significantly reduce the gloss and intensify the surface roughness of enamel and restorative materials. Hybrid materials show less gloss retention and more surface roughness than traditional ceramics. However, values were still better than those of human enamel.20
In an ongoing clinical evaluation, 103 teeth were restored with hybrid ceramic (Vita Enamic) minimally invasive restorations. After an observation time of 1 year, the survival rate was 100%. Marginal adaptation and marginal discoloration of all restorations were clinically satisfying.34
Conclusions
Within the limitation of the available data on hybrid materials, it may be concluded that this novel product family represents a successful step toward the goal of restoring single teeth in a single appointment using a material with similar mechanical behavior to that of human enamel and dentin. However, independent long-term studies on the clinical performance of these materials are urgently needed.
Acknowledgments
The author would like to express his sincere appreciation to Petra Gierthmüehlen, DDS, PhD, and Markus B. Blatz, DMD, PhD, for their editorial and professional guidance and support in the production of this manuscript.
About The Author
Sebastian D. Horvath, Dr. med. dent.
Department of Preventive and Restorative Sciences
University of Pennsylvania
Philadelphia, Pennsylvania
Department of Prosthodontics
School of Dentistry
Albert-Ludwigs University
Freiburg, Germany
Private Practice
Jestetten, Germany
References
1. Reiss B, Walther W. Clinical long-term results and 10-year Kaplan-Meier analysis of Cerec restorations. Int J Comput Dent. 2000;3(1):9-23.
2. Donovan TE. Factors essential for successful all-ceramic restorations. J Am Dent Assoc. 2008;139 suppl:14S-18S.
3. Ruse ND, Sadoun MJ. Resin-composite blocks for dental CAD/CAM applications. J Dent Res. 2014;93(12):1232-1234.
4. Guess PC, Selz CF, Steinhart YN, et al. Prospective clinical split-mouth study of pressed and CAD/CAM all-ceramic partial-coverage restorations: 7-year results. Int J Prosthodont. 2013;26(1):21-25.
5. He LH, Swain M. A novel polymer infiltrated ceramic dental material. Dent Mater. 2011;27(6):527-534.
6. Suh BI. New concepts and technology for processing of indirect composites. Compend Contin Educ Dent. 2003;24(8 suppl):40-42.
7. Nguyen JF, Migonney V, Ruse ND, Sadoun M. Resin composite blocks via high-pressure high-temperature polymerization. Dent Mater. 2012;28(5):529-534.
8. Johnson AC, Versluis A, Tantbirojn D, Ahuja S. Fracture strength of CAD/CAM composite and composite-ceramic occlusal veneers. J Prosthodont Res. 2014;58(2):107-114.
9. Lauvahutanon S, Takahashi H, Shiozawa M, et al. Mechanical properties of composite resin blocks for CAD/CAM. Dent Mater J. 2014;33(5):705-710.
10. Koller M, Arnetzl GV, Holly L, Arnetzl G. Lava ultimate resin nano ceramic for CAD/CAM: customization case study. Int J Comput Dent. 2012;15(2):159-164.
11. Coldea A, Swain MV, Thiel N. Mechanical properties of polymer-infiltrated-ceramic-network materials. Dent Mater. 2013;29(4):419-426
12. Lauvahutanon S, Takahashi H, Oki M, et al. In vitro evaluation of the wear resistance of composite resin blocks for CAD/CAM. Dent Mater J. 2015;34(4):495-502.
13. Thornton I, Ruse ND. Characterization of nanoceramic resin composite and lithiumdisilicate blocks for CAD/CAM [abstract]. J Dent Res. 2014;93(spec iss B): Abstract 151.
14. Kinney JH, Balooch M, Marshall SJ, et al. Hardness and Young’s modulus of human peritubular and intertubular dentine. Arch Oral Biol. 1996;41(1):9-13.
15. Habelitz S, Marshall SJ, Marshall GW Jr, Balooch M. Mechanical properties of human dental enamel on the nanometre scale. Arch Oral Biol. 2001;46(2):173-183.
16. Boschian Pest L, Cavalli G, Bertani P, Gagliani M. Adhesive post-endodontic restorations with fiber posts: push-out tests and SEM observations. Dent Mater. 2002;18(8):596-602.
17. Ausiello P, Rengo S, Davidson CL, Watts DC. Stress distributions in adhesively cemented ceramic and resin-composite Class II inlay restorations: a 3D-FEA study. Dent Mater. 2004;20(9):862-872.
18. Coldea A, Swain MV, Thiel N. In-vitro strength degradation of dental ceramics and novel PICN material by sharp indentation. J Mech Behav Biomed Mater. 2013;26:34-42.
19. Takahashi H, Finger WJ, Endo T, et al. Comparative evaluation of mechanical characteristics of nanofiller containing resin composites. Am J Dent. 2011;24(5):264-270.
20. Mörmann WH, Stawarczyk B, Ender A, et al. Wear characteristics of current aesthetic dental restorative CAD/CAM materials: two-body wear, gloss retention, roughness and Martens hardness. J Mech Behav Biomed Mater. 2013;20:113-125.
21. Heintze SD, Cavalleri A, Forjanic M, et al. Wear of ceramic and antagonist—a systematic evaluation of influencing factors in vitro. Dent Mater. 2008;24(4):433-449.
22. Vita Zahnfabrik. Vita Enamic - Technical and scientific documentation. December 2012:26. https://www.vita-zahnfabrik.com/de/VITA-ENAMIC-27588,27568,85233.html. Accessed September 13, 2015.
23. Coldea A, Fischer J, Swain MV, Thiel N. Damage tolerance of indirect restorative materials (including PICN) after simulated bur adjustments. Dent Mater. 2015;31(6):684-694.
24. Fasbinder DJ, Neiva GF. Surface evaluation of polishing techniques for new resilient CAD/CAM restorative materials. J Esthet Restor Dent. 2016;28(1):56-66.
25. 3M ESPE. Lava™ Ultimate CAD/CAM Restorative. https://www.3m.com/3M/en_US/Dental/Products/Lava-Ultimate/. Accessed September 13, 2015.
26. Spitznagel FA, Horvath SD, Guess PC, Blatz MB. Resin bond to indirect composite and new ceramic/polymer materials: a review of the literature. J Esthet Restor Dent. 2014;26(6):382-393.
27. Ahlers MO, Mörig G, Blunck U, et al. Guidelines for the preparation of CAD/CAM ceramic inlays and partial crowns. Int J Comput Dent. 2009;12(4):309-325.
28. Magne P, Schlichting LH, Maia HP, Baratieri LN. In vitro fatigue resistance of CAD/CAM composite resin and ceramic posterior occlusal veneers. J Prosthet Dent. 2010;104(3):149-157..
29. Schlichting LH, Maia HP, Baratieri LN, Magne P. Novel-design ultra-thin CAD/CAM composite resin and ceramic occlusal veneers for the treatment of severe dental erosion. J Prosthet Dent. 2011;105(4):217-226.
30. Magne P, Knezevic A. Simulated fatigue resistance of composite resin versus porcelain CAD/CAM overlay restorations on endodontically treated molars. Quintessence Int. 2009;40(2):125-133.
31. Ferracane JL, Berge HX, Condon JR. In vitro aging of dental composites in water—effect of degree of conversion, filler volume, and filler/matrix coupling. J Biomed Mater Res. 1998;42(3):465-472.
32. Nambu T, Watanabe C, Tani Y. Influence of water on the transverse strength of posterior composite resins. Dent Mater J. 1991;10(2):138-148.
33. Druck CC, Pozzobon JL, Callegari GL, et al. Adhesion to Y-TZP ceramic: study of silica nanofilm coating on the surface of Y-TZP. J Biomed Mater Res B Appl Biomater. 2015;103(1):143-150.
34. Vuck A, Strub JR, Guess PC. Minimal invasive CAD/CAM hybrid-ceramic restorations. XXXIII International AIOP Congress. November 2014:1-1.