Full-Contour Zirconia Fixed Partial Dentures as Chairside Applications: A Case Report
Mike Skramstad, DDS; and Dennis J. Fasbinder, DDS, ABGD
Abstract: Clinical application of zirconia has been expanding due to the high strength properties it offers. Initial use of zirconia was as a coping or substructure material replacing cast metal. More recent formulations have been introduced for monolithic zirconia contour designs. New chairside computer-aided design and computer-aided manufacturing (CAD/CAM) technology has made it possible for dentists to deliver 3-unit bridges in a single appointment. This case report will present such a clinical application.
The dental community has expressed interest in having high-strength ceramic materials for use in restorative treatments. Metal-ceramic crowns are bilayer restorations relying on a strong metallic core or substructure veneered with a more esthetic porcelain. The introduction of zirconia as a restorative material has provided a strong tooth-colored coping material to replace metal copings. Initial zirconia crowns and fixed partial dentures (FPDs) have consisted of a strong, but generally opaque, core that was veneered with a more translucent, feldspathic porcelain.
Significant clinical research has been conducted on the use of bilayer zirconia restorations. One extensive systematic review of single-tooth crowns included 67 clinical studies reporting on 4663 porcelain-fused-to-metal (PFM) crowns and 9434 all-ceramic single crowns published between 2006 and 2013.1 The estimated survival rates after 5 years were 95.7% for PFM crowns, 96.6% for leucite-reinforced and lithium disilicate crowns, and 91.2% for veneered zirconia crowns. Chipping of the veneering porcelain was the most common technical problem for both PFM and veneered zirconia crowns with an estimated 5-year complication rate of 2.6%. However, the fracture of the zirconia core was rare at a rate of only 0.4% over 5 years. The loss of retention was greatest for veneered zirconia crowns at an estimated 5-year complication rate of 4.7%. Tooth fracture and loss of tooth vitality were more common for PFM crowns (1.2% to 1.8%) than for all-ceramic crowns. Biologically, all-ceramic single crowns performed better than metal-ceramic crowns. Significantly more loss of abutment tooth vitality and abutment tooth fracture was reported for metal-ceramic crowns.
The high strength of zirconia has generated considerable interest in using it as a substructure for FPDs. One systematic review included 40 clinical studies reporting on 1796 metal-ceramic and 1110 all-ceramic FPDs.2 Meta-analysis of the included studies indicated an estimated 5-year survival rate of 94.4% for the metal-ceramic FPDs and 90.4% for the densely sintered zirconia FPDs. No significant difference was observed between the survival rates. Significantly more framework fractures were reported for reinforced glass-ceramic FPDs (8.0%) and glass-infiltrated alumina FPDs (12.9%) compared with metal-ceramic FPDs (0.6%) and densely sintered zirconia FPDs (1.9%) after 5 years in function. The incidence of ceramic fractures and loss of retention was significantly higher for densely sintered zirconia FPDs. Clinical trials involving zirconia FPDs have shown that, despite a low frequency of core fracture, these restorations tend to have a significantly higher rate of porcelain veneer fracture than PFM FPDs.3
Continued development of zirconia materials improved the ability to provide desired coloring to the material and more esthetic translucent results. As computer-aided design/computer-aided manufacturing (CAD/CAM) processes similarly evolved, laboratories pursued monolithic restorations for the efficiency in fabrication and consistency in material properties by avoiding the veneered layer of weaker feldspathic porcelain.
Monolithic zirconia has become popular for use in posterior crowns and FPDs. Despite this preference, long-term clinical research on monolithic zirconia crowns is still scant. One recently published clinical study reported early results comparing a small number of CAD/CAM fabricated metal-ceramic and full-contour zirconia crowns.4 Twenty-two patients received 12 metal-ceramic, 10 lithium disilicate, and 10 zirconia crowns. An iTero® scanner (Align Technology, itero.com) was used to image the metal-ceramic and zirconia crowns for laboratory fabrication. An E4D scanner (Planmeca/E4D Technologies, e4d.com) and E4D milling unit (Planmeca/E4D Technologies) were used to fabricate the lithium-disilicate crowns. All crowns were reevaluated at 1 month and 6 months. No significant difference in gingival crevicular fluid volumes between any of the crowns and control teeth was observed. The average horizontal marginal discrepancy was significantly different with zirconia crowns having the least amount of horizontal margin discrepancy.
Another study recorded the fracture rates of monolithic zirconia restorations based on data from two commercial dental laboratories.5 The number of restorations returned to the dental laboratories for remakes was recorded. A total of 39,827 restoration records were reviewed. The fracture rate was 0.99% over 5 years for posterior monolithic zirconia restorations and 2.06% for anterior monolithic zirconia restorations. However, the study design may have under-reported failures, as only those restorations dentists returned to the dental laboratories were included in the data.
Zirconia has been a laboratory-fabricated full-contour restoration due to the extended time required for processing and sintering. However, the recent introduction of an induction porcelain oven (CEREC® SpeedFire, Dentsply Sirona, dentsply.com) has opened clinical opportunities for chairside CAD/CAM applications never before thought possible. Not only can dentists take advantage of the physical properties of full-contour zirconia, but they can do it with more conservative preparations in a single patient visit. This case report will discuss such a clinical opportunity with a same-day 3-unit zirconia bridge.
Case Report
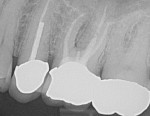
A 57-year-old male presented in October 2015 with an endodontically treated maxillary first molar (tooth No. 14) that had a vertical root fracture (Figure 1). The patient was about to begin chemotherapy and needed the tooth removed immediately due to pain and risk for infection. After he completed his chemotherapy in May 2016, he presented to the dentist for options to replace the missing tooth.
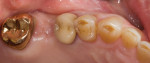
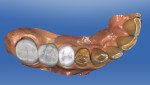
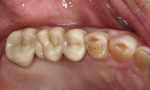
The patient previously had cast-gold bridges placed from teeth Nos. 18 through 20 and Nos. 29 through 31 to replace lost mandibular first molars. Although the dentist recommended an implant to replace the missing tooth No. 14, the patient did not want surgery, choosing instead to have another bridge placed on the upper left due to the success of his other FPDs. Because the teeth adjacent to the missing tooth already had full-coverage crowns (teeth Nos. 13 and 15) (Figure 2), the dentist agreed to perform the bridgework. Full-contour zirconia was chosen because of its high flexural strength and higher fracture toughness; it also provided the dentist with the ability to conventionally cement the bridge. Even though high-strength zirconia restorations are not as esthetic as some glass-ceramic restorations, the patient was more concerned with longevity than beauty. Although a veneered zirconia FPD may offer the opportunity to control the esthetic outcome of the FPD, it also has a significant risk for fracture of the veneering porcelain. Full-contour zirconia was elected because the patient expressed a concern with longevity and full-contour zirconia would significantly decrease the risk for fracture or chipping of the FPD.
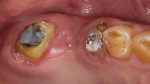
After removal of the existing restorations on teeth Nos. 13 and 15, no major structural damage or decay was observed on the existing tooth preparations (Figure 3). They were refined with a medium- and fine-chamfer bur (Meisinger USA, meisinger.de). Although zirconia can tolerate preparation reduction as small as 0.5 mm, a 1.0-mm axial reduction was performed on these preparations due to the previous amount of tooth reduction.
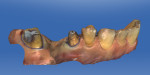
After proper retraction using size No. 1 Ultrapak® cord (Ultradent, ultradent.com), the bridge preparation was imaged (CEREC Omnicam, Dentsply Sirona) and the margins identified using the CEREC 4.4.3 chairside software (Dentsply Sirona) (Figure 4). Biojaw, the new biostatistical algorithm used by the CEREC software, is used to analyze the entire scanned digital model. This produces initial restoration proposals that need little manipulation and are virtually ready to mill (Figure 5).
The material chosen was CEREC Zirconia (Dentsply Sirona), which is a high-strength/precolored zirconia, and was dry milled with inLab MC X5 (Dentsply Sirona) and carbide burs (Shaper 25/Finisher 10 [Dentsply Sirona]). The dry-milling technique produces excellent marginal integrity and detail and allows for extremely fast sintering because no additional drying step is necessary (Figure 6). The overall mill time for this 3-unit bridge was 29 minutes.
The patient’s parafunctional habits that have caused attrition of the anterior teeth were not addressed in this particular case because they have remained consistent over several years and were not a primary concern for the patient. At the time of treatment, he was wearing a nightguard to prevent further damage and did not desire additional dentistry. Highly polished zirconia has excellent wear characteristics and should provide this patient an excellent long-term result.
Some published laboratory data indicate zirconia may be abrasive to the opposing dentition.6-8 Studies using natural teeth have shown that zirconia may cause excessive wear of the tooth structure.9 This is particularly true if an as-milled surface of the zirconia is simply glazed. The process of milling zirconia results in a rough surface. Applying a glaze to the rough milled surface merely fills in the valleys of the surface roughness. The weaker glaze wears rather rapidly, exposing a rougher zirconia surface that then accelerates opposing tooth wear. Alternatively, if the milled zirconia is polished to a smooth surface, significantly less wear of the opposing antagonist is likely. Laboratory studies have shown polished zirconia causes the least amount of opposing enamel wear, glazed zirconia the most amount of antagonist wear, and polished-then-reglazed zirconia was intermediate.10 A systematic review of in vitro research on zirconia wear of opposing enamel included 62 studies for review. Regardless of test mechanism, enamel wear rates were lower against polished zirconia.11 One suggested explanation for the reduced amount of wear is that the glazing surface is quickly worn away to expose the rough surface of the unpolished underlying ceramic.12,13 Therefore, polishing ceramics prior to glazing may help minimize opposing enamel wear.
After removing the sprue (Universal White Polisher 9613V-220 [Meisinger]), a light contour at low RPMs (<5000) with a fine diamond (863-016 [Meisinger]) and pink twist polisher (9771F-170 [Meisinger]) was performed to accentuate overall anatomy and polish on the occlusal surface. This was also done to help create a smoother surface after sintering to make polishing easier and overall reduce the wear to opposing enamel (Figure 7). Even though a light prepolish helps smooth the initial sinter surface, polishing post-sintering is also necessary to maximize flexural strength advancing and opposing wear.14
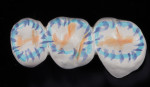
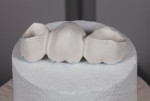
Because high-strength zirconia can be a little opaque and high in value, water-based infiltration liquids can be added to internalize color and help with overall esthetics. For this case, Incisal Blue and Violet Colour Liquids Prettau® Aquarell (Zirkonzahn, zirkonzahn.com) and Okklusal Amber shade effect (Whitepeaks Dental Solution, white-peaks-dental.com) were used for the infiltration (Figure 8). The bridge was then ready to be sintered and placed occlusal surface down in the CEREC SpeedFire oven (Dentsply Sirona) (Figure 9). The use of ceramic beads is not necessary with this furnace because it uses patented induction technology that allows energy-efficient heating cycles based on ceramic volume and shade. Single-unit restorations can often be sintered in less than 15 minutes and bridges (as in this report) in less than 30 minutes.
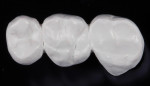
Once the material is sintered and cooled (Figure 10), the restoration must be hand polished to a “mirror finish” (Figure 11). This author’s preferable method of polishing is with Meisinger Twist polishers (Green, Blue, and Pink) with an RPM less than 11K. This efficient polishing system produces an excellent finish that has been shown to wear enamel less than feldspathic porcelain15 and similar to gold alloy.16 After the zirconia is properly polished, stains and glazes can be applied to better enhance esthetics and match other characteristics of existing teeth.
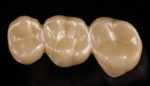
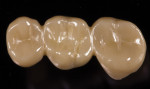
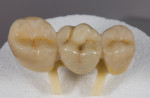
Dentsply Sirona manufactures specialized glazing pins for the CEREC SpeedFire (Figure 12) that properly support the restoration in a second 7-minute glazing cycle (Figure 13). The stains and glazes used in this case were a combination of GC Initial IQTM Lustre Pastes (GC America, gcamerica.com) and IPS Ivocolor (Ivoclar Vivadent, ivoclarvivadent.us). CEREC SpeedFire is the first furnace that both sinters and glazes zirconia and other glass-ceramics. The final restoration was ready for cementation (Figure 14).
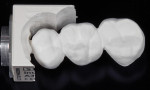
An advantage of monolithic zirconia is its ability to be conventionally cemented or bonded in place dependent on the preparation. In this case, conventional cementation with a resin-modified glass-ionomer cement was chosen due to the retentive properties of the preparations (FujiCEMTM 2 [GC America]). A high-strength zirconia was chosen for this case to maximize the flexural strength and connector dimension properties of the bridge (Figure 15). In doing so, the restoration can appear a little higher in shade value, or brighter, compared to the existing teeth. More translucent zirconia is available and being developed that will help this optical discrepancy, but currently only can be sintered with longer (8-hour) sintering cycles. Full-contour zirconia does not have the translucency of tooth structure and has a tendency to appear higher in shade value than the adjacent tooth structure.
Conclusion
With the introduction of the CEREC SpeedFire and dry-milling capabilities, chairside fabrication of monolithic crowns, abutments, and 3-unit bridges is now a reality. Also, these procedures can be accomplished in a single visit, thus expanding the indications of same-day CAD/CAM applications.
Disclosure
Dr. Fasbinder has received research support from Dentsply Sirona.
About The Authors
Mike Skramstad, DDS
Resident faculty member
Spear Education and CERECdoctors.com
Private Practice
Orono, Minnesota
Dennis J. Fasbinder, DDS, ABGD
Clinical Professor
Director of the Computerized Dentistry Program
University of Michigan
School of Dentistry
Private Practice
Ann Arbor, Michigan
References
1. Sailer I, Makarov NA, Thoma DS, et al. All-ceramic or metal-ceramic tooth-supported fixed dental prostheses (FDPs)? A systematic review of the survival and complication rates. Part I: single crowns (SCs). Dent Mater. 2015;31(6):603-623.
2. Pjetursson BE, Sailer I, Makarov NA, et al. All-ceramic or metal-ceramic tooth-supported fixed dental prostheses (FDPs)? A systematic review of the survival and complication rates. Part II: multiple-unit FDPs. Dent Mater. 2015;31(6):624-639.
3. Heintze SD, Rousson V. Survival of zirconia and metal-supported fixed dental prostheses: a systematic review. Int J Prosthodont. 2010;23(6):493-502.
4. Batson ER, Cooper LF, Duqum I, Mendonça G. Clinical outcomes of three different crown systems with CAD/CAM technology. J Prosthet Dent. 2014;112(4):770-777.
5. Sulaiman TA, Abdulmajeed AA, Donovan TE, et al. Fracture rate of monolithic zirconia restorations up to 5 years: a dental laboratory survey [published online ahead of print May 10, 2016. J Prosthet Dent. doi: 10.1016/j.prosdent.2016.01.033.
6. Suputtamongkol K, Anusavice KJ, Suchatlampong C, et al. Clinical performance and wear characteristics of veneered lithia-disilicate-based ceramic crowns. Dent Mater. 2008;24(5):667-673.
7. Oh WS, Delong R, Anusavice KJ. Factors affecting enamel and ceramic wear: a literature review. J Prosthet Dent. 2002:87(4):451-459.
8. Metzler KT, Woody RD, Miller AW 3rd, Miller BH. In vitro investigation of the wear of human enamel by dental porcelain. J Prosthet Dent. 1999;81(3):356-364.
9. Shah S, Michelson C, Beck P, et al. Wear of enamel on polished and glazed zirconia [abstract]. J Dent Res. 2010;89(spec iss A). Abstract 227.
10. Janyavula S, Lawson N, Cakir D, et al. The wear of polished and glazed zirconia against enamel. J Prosthet Dent. 2013;109(1):22-29.
11. Passos SP, Torrealba Y, Major P, et al. In vitro wear behavior of zirconia opposing enamel: a systematic review. J Prosthodont. 2014;23(8):593-601.
12. Heintze SD, Cavalleri A, Forjanic M, et al. Wear of ceramic and antagonist—a systematic evaluation of influencing factors in vitro. Dent Mater. 2008;24(4):433-449.
13. Etman MK. Confocal examination of subsurface cracking in ceramic materials. J Prosthodont. 2009;18(7):550-559.
14. Schatz C, Strickstrock M, Roos M, et al. Influence of specimen preparation and test methods on the flexural strength results of monolithic zirconia materials. Materials. 2016;9(3):180.
15. Albashaireh ZS, Ghazal M, Kern M. Two-body wear of different ceramic materials opposed to zirconia ceramic. J Prosthet Dent. 2010;104(2):105-113.
16. Sorensen JA, Sultan EA, Sorensen PN. Three-body wear of enamel against full crown ceramics [abstract]. J Dent Res. 2011;90(spec iss A):Abstract 1652.
Not only can dentists take advantage of the physical properties of full-contour zirconia, but they can do it with more conservative preparations in a single patient visit