Staged Reconstruction for a Severely Worn Dentition
Christopher Wilson, DMD
Abstract:
When patients are constrained financially to receive dental work, a staged approach can be an effective way for enabling treatment to proceed. In this case, a patient who had been in the practice for about 10 years and had a severely worn and eroded dentition finally opted to receive treatment in stages. A systematic approach was used to determine the proper postoperative position of the teeth. The subsequent treatment plan included the use of porcelain onlays and full-coverage crowns in the mandibular posterior along with provisional direct composite restorations in the maxillary dentition; the composites would be transitioned to porcelain crowns as the patient’s finances would allow.
A long-time patient was finally in a better financial position to address his severely worn dentition, in which erosion and chipping and breaking of teeth were prevalent. However, despite his decision to accept treatment, economic constraints were still an issue, and, therefore, he required a staged approach to his treatment.
Clinical Case Review
A 54-year-old patient who had been in the practice since 2005 presented on re-care with a fractured tooth No. 10. He indicated he was ready to proceed with treatment that would improve his smile. Treatment options to restore his worn front teeth had been discussed several times in the past.
Medical and Dental History
The patient’s pertinent medical history included a heavy smoking habit, chronic obstructive pulmonary disease (COPD), gastric reflux disease, and an enlarged prostate. His medications included gabapentin and Spiriva® for COPD, pantoprazole for reflux disease, and Flomax® for prostate enlargement.
A review of the patient’s dental history revealed concerns with esthetics and tooth-structure loss. The patient said he was uncomfortable with his smile because he did not show any teeth when smiling. He noted his front teeth had become shorter in the past 5 years, indicating that the loss of tooth structure was active. He was aware of holes in his teeth and his teeth were chipping and breaking.
Diagnostic Findings
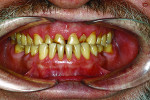
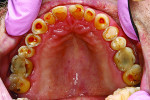
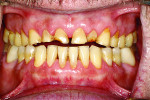
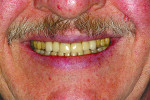
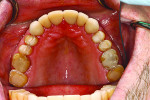
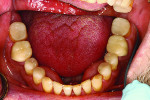
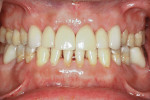
The examination revealed an extensively worn dentition (Figure 1 through Figure 3) with severe erosion affecting most of the posterior and the maxillary anterior teeth. The patient had lost his lower first molars when he was a teenager. The maxillary posterior teeth exhibited more damage than the mandibular posterior teeth. No decay was present. The teeth were only minimally restored with no defective restorations present, although some restorations, while not defective, had rough margins where further erosion was a risk. The patient showed no maxillary teeth in repose and had to strain to display them when he smiled (Figure 4 and Figure 5).
Diagnosis, Risk Assessment, and Prognosis Periodontal: The examination findings revealed light bleeding on probing with scattered 4-mm pocketing and no significant radiographic bone loss, consistent with an AAP type II diagnosis.
Risk: Low
Prognosis: Good
Biomechanical: Severe wear and erosion were noted on all the maxillary teeth and mandibular posterior teeth. Moderate wear and erosion was noted on the mandibular anterior teeth. Some restorations were in questionable condition, but no decay was present. Large erosion potholes in the posterior teeth were noted. The maxillary anterior teeth were extremely worn and fractured with the central incisors measuring 6.5 mm long.
Risk: High
Prognosis: Poor
Functional: The patient reported no discomfort in the temporomandibular joints, and had no noises in the joints. The range of opening was within normal limits, and the patient opened smoothly and easily without deviation.
Risk: Low
Prognosis: Good
Dentofacial: No tooth display was evident when the patient was speaking, and he had to strain to show any teeth at all when smiling. The canines measured –3 mm in repose.
Risk: Low
Prognosis: Good
Treatment Goals
Treatment goals in this case were threefold: (1) restore posterior teeth to cover eroded areas and protect them from further erosion; (2) restore maxillary anterior teeth to the correct length (10 mm to 10.5 mm) for esthetics; (3) create a plan that could accommodate the patient’s tight budget by providing treatment in stages.
Treatment Plan
The patient’s answers in the “Bite and Jaw Joint” section of the dental history form indicated an acceptable bite. However, given the amount of tooth structure loss, a Kois deprogrammer was used to confirm the centric-relation treatment position prior to commencing treatment to determine a stable and reproducible jaw position.1 A systematic approach (Kois Management Considerations: A 10-Step Approach©, Kois Center, www.koiscenter.com) was used to determine the proper postoperative position of the teeth. The desired maxillary incisal edge vertical position was determined by the maxillary cuspid position2 and the esthetic requirements driven by the patient’s lip mobility and gingival architecture. The central incisors needed to be 10 mm long. The maxillary occlusal plane was deemed acceptable, and the mandibular occlusal plane needed to be raised or increased. The mandibular incisal edge position was correct.
Thus, increasing the length of the mandibular posterior teeth using a combination of e.max® (Ivoclar Vivadent, www.ivoclarvivadent.com) onlays and full-coverage crowns would create the space needed for proper maxillary central incisor length while protecting those teeth from further damage. The maxillary posterior teeth would first be treated with composite to restore the eroded areas and to smooth the existing jagged occlusal plane. The maxillary anterior teeth would be restored to their proper length initially with direct composite, giving the patient a more esthetic smile. These provisional direct composites would then be transitioned to e.max full-coverage crowns as the patient’s finances would allow.
Restorative Treatment Phases
Phase 1
A Kois deprogrammer was fabricated, and the patient wore it for 2 weeks. No change in jaw position was noted after deprogramming, confirming the diagnosis of acceptable function. Alginate impressions and a facebow were used for fabrication of a diagnostic wax-up. The locations of the new vertical dimension, maxillary incisal edge position, and mandibular posterior occlusal plane were communicated to the laboratory. A putty stent was fabricated to facilitate direct composite placement on the maxillary anterior teeth.
The patient returned for the preparation of the mandibular posterior teeth. Teeth Nos. 18 and 31 were prepared for e.max crowns, and the remaining mandibular posterior teeth received minimal preparation (a seating dimple only) for e.max onlays, thus preserving as much tooth structure as possible. The crowns and onlays were fabricated to match the wax-up.
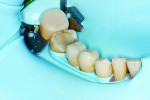
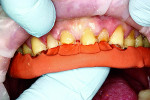
At the next visit, the mandibular onlays and crowns were delivered. The restorations were placed using local anesthesia under rubber dam isolation (Figure 6). The prepared teeth were microabraded (PrepStart™ Air Abrasion System, Danville Materials, www.danvillematerials.com) and then etched and bonded (All-Bond Universal™, Bisco, www.bisco.com). The e.max crowns were cemented with self-adhesive resin cement (RelyX™ Unicem 2, 3M ESPE, www.3MESPE.com), and the onlays were cemented using RelyX™ Veneer Cement (3M ESPE). Gross cleanup of the cement was accomplished with a sharp scaler, and then the margins were finished with ultra-fine diamonds and Enhance® cups (DENTSPLY, www.dentsply.com) (Figure 7 and Figure 8).
At the same appointment, the maxillary anterior teeth were restored with direct composite (Filtek™ Supreme Ultra, 3M ESPE) using the putty stent as a guide (Figure 9) to be in harmony with the newly corrected occlusion provided by the mandibular restorations. The teeth were microabraded and the dentin covered with a thin coat of Unicem 2, which was cured for 10 seconds. The layer of Unicem 2 was intended to seal the dentin, thereby decreasing microleakage and minimizing postoperative sensitivity. The teeth were then etched and bonded (All-Bond Universal). Because the dentin was sealed, etch could then be applied to the entire preparation without risk to the dentin. The teeth were then restored using Filtek Supreme Ultra composite. The shaping and finishing was done with ultra-fine diamonds and abrasive discs, followed by final shaping and polishing with Enhance cups.
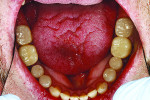
The maxillary posterior teeth were restored minimally with composite to cover the eroded areas and even out the jagged occlusal surfaces to allow a proper occlusion with the mandibular e.max restorations. The teeth were restored with the composite protocol outlined above using Filtek Supreme Ultra material. The increased occlusal vertical dimension change was created with mandibular restorations only (Figure 10 and Figure 11).
Phase 2
As the patient’s finances allowed, the maxillary anterior teeth were restored with e.max crowns, two at a time for a 2-year period. The central incisors were restored first, followed by the lateral incisors and, finally, the cuspid teeth (Figure 12).
At this time, the maxillary posterior teeth are restored only with composite. The patient will receive e.max crowns as his finances allow.
Conclusion
All the maxillary composite restorations remained trouble free, with no chipping or breakage, for 2 years following the first restorative phase, during which time the patient transitioned to the definitive restorations with the placement of the 6 maxillary anterior e.max crowns. Two of the maxillary posterior composites were recently repaired after sustaining small fractures. This confirms the diagnosis of acceptable occlusal function and the correct treatment position of the mandible. The Kois deprogrammer was a useful tool in confirming the diagnosis, recording centric relation, and designing a treatment strategy to minimize the risk for future problems while staging the definitive treatment.3
The extent and pattern of wear on the teeth before treatment was consistent with erosion from acid reflux. Although he may have also initially had an occlusal problem, he had acceptable function when he presented for treatment. Although he may have also initially had an occlusal problem, he had acceptable function when he presented for treatment.
The patient has been pleased with the esthetic result (Figure 13 through Figure 15), even though the direct composite restorations did show extrinsic staining at replacement, which was likely due to his heavy smoking habit. The maxillary posterior teeth have been maintaining well in composite until the patient is ready financially for completion of the treatment.
Acknowledgment
The author would like to acknowledge the excellent porcelain work of Schell Dental Ceramics in Kelowna, British Columbia, Canada.
About the Author
Christopher Wilson, DMD
Mentor
Kois Center
Seattle, Washington
Private Practice
Kamloops, British Columbia, Canada
References
1. Jayne D. A deprogrammer for occlusal analysis and simplified accurate case mounting. Journal of Cosmetic Dentistry. 2006;21(4):96-102.
2. Misch CE. Guidelines for maxillary incisal edge position—a pilot study: the key is the canine. J Prosthodont. 2008;17(2):130-134.
3. Kois JC, Hartrick N. Functional occlusion: science-driven management. Journal of Cosmetic Dentistry. 2007;23(3):54-57.