Long-Term Provisional Bonded Composite Restorations Make Full-Mouth Rehabilitation Possible
Ronald G. Wilkins, DDS
Abstract: Full-mouth rehabilitation cases frequently require an extended period to complete. In this case involving a patient who presented with a significant amount of lost tooth structure, treatment featured laboratory-fabricated composite provisional restorations aimed at stabilizing the dentition and enabling definitive treatment to be completed in segments. The approach taken allowed occlusal and esthetic issues to be resolved through use of the provisionals while minimizing tooth preparation. The technique provided immediate improvement in esthetics, function, and comfort.
Full-mouth rehabilitation is a complex endeavor that can become even more complicated when treatment must be carried out over a protracted period. The reasons for extending treatment time are numerous and can include health issues, financial considerations, and scheduling conflicts. This case demonstrates a method of initiating restorative treatment using laboratory-fabricated composite provisional restorations that stabilize and protect the dentition, thus allowing definitive treatment to be completed in segments over an extended period.
Clinical Case Overview
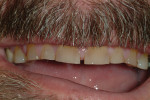
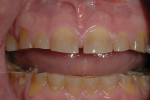
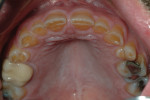
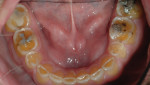
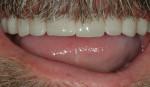
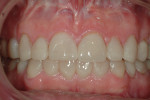
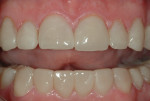
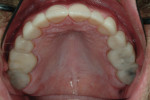
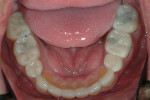
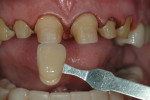
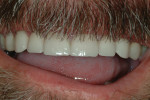
A 45-year-old man presented with the chief complaint of having “lost a filling.” On initial examination, it was apparent more serious issues were involved than just a lost filling (Figure 1 through Figure 6). The most obvious problem noted was the large amount of tooth structure that had been lost to erosion and attrition. The patient was aware of the tooth structure loss and was willing to explore the causes and potential treatment options for restoration.
Medical History
The medical history revealed hypertension, attention deficient disorder, seasonal allergies, and obstructive sleep apnea (OSA). He used a continuous positive airway pressure (CPAP) machine for OSA, and his hypertension was treated with medication. Because dental erosion was a major examination finding, the patient was asked if he had been given a diagnosis of gastroesophageal reflux disease (GERD), and he reported that he had never been tested for it. Based on his dentist’s urging that he be tested, the patient consulted with his physician about GERD testing. The findings from those tests revealed the presence of GERD, and treatment was initiated.
Because the dental findings fit the pattern of airway-related health issues,1,2 the dentist also strongly recommended he have a new sleep study performed to evaluate the efficacy of his current CPAP therapy. The patient contacted his sleep physician and had baseline and calibration studies performed to titrate CPAP therapy, so that the underlying medical issues were stable prior to the initiation of his dental treatment.
Dental History
The patient reported receiving orthodontic treatment with bicuspid extractions during his adolescence. The only other positive findings noted in the dental history were a history of broken teeth and restorations and an awareness of nocturnal bruxism.
Diagnostic Findings
The major diagnostic findings were consistent with nocturnal bruxism and acid erosion related to GERD, and included severe attrition and generalized dental erosion. One of the benefits of placing long-term provisionals in this case is that the patient’s sleep and airway issues could be evaluated and treated medically while his teeth were protected and restored to proper contour.
Diagnosis, Risk Assessment, and Prognosis
Periodontal: The examination revealed areas of light bleeding on probing. Most probing depths were less than 3 mm, with site-specific pocket depths of 4 mm to 5 mm noted in the lower molar areas. No areas of radiographic bone loss were greater than 2 mm. The findings were consistent with a diagnosis of AAP type II.
Risk: Low
Prognosis: Good
Biomechanical: Two carious lesions were noted around old amalgam restorations and along the crown margin of tooth No. 3. The most significant finding was severe generalized erosion. The biomechanical diagnosis needed to consider caries, severe erosion, defective restorations, and structural compromises due to the missing tooth structure.
Risk: High
Prognosis: Hopeless
Functional: Severe attrition, likely resulting from a combination of nocturnal bruxism (parafunction) and acid erosion (GERD), was noted. The patient believed the amount of bruxing had decreased since CPAP therapy was initiated. There were no signs or symptoms of temporomandibular joint pathology, and the joint accepted loading. A functional diagnosis of occlusal dysfunction (referring to his OSA) and parafunction (nocturnal bruxism) was determined.
Risk: High
Prognosis: Hopeless
Dentofacial: The patient presented with a moderate display of tooth structure on smiling, which was the result of a lack of lip mobility caused by an accident that had damaged his facial muscles and nerves.
Risk: Moderate
Prognosis: Fair
Treatment Goals
The following treatment goals were established:
• Assure that GERD and OSA were being managed successfully.
• Establish proper occlusal vertical dimension (OVD) and a repeatable treatment position (centric relation [CR]). Because all the teeth were severely damaged and the joints were healthy, a leaf gauge would be used to efficiently establish treatment position.
• Treat the caries, then restore the teeth using long-term bonded provisionalization to protect them from further destruction.
• Place the final restorations in sextants as the patient’s circumstances would permit.
Treatment Plan
The treatment plan would be carried out as follows:
• Remove caries and restore teeth Nos. 2 and 14 with direct composite resin.
• Fabricate study models and mount casts on a Panadent™ (Panadent, www.panadent.com) articulator with a Kois Dento-Facial Analyzer™ (Panadent). Use a leaf gauge to determine CR, and employ esthetic determinants to establish the proper OVD, which would facilitate restoring proper form and function of the teeth in the provisional restorations.
• Take final impressions for provisionals using polyvinylsiloxane (PVS) followed by a laboratory-fabricated diagnostic wax-up at the newly established OVD and CR. Have the laboratory construct the provisional restorations (Radica™, DENTSPLY, www.dentsply.com) using the wax-up as a guide.
• Place provisional restorations on all teeth using microabrasion, acid-etch, bonding agent, and flowable composite as cement. At this time, prior to cementing the provisionals, the crown and caries on tooth No. 3 would be removed. Analyze and equilibrate the provisionals as needed to assure equal bilateral posterior contacts, using the leaf gauge to establish the CR treatment position.
• Complete final restorations in sextants as the patient’s circumstances allow.
Treatment Phases
Phase 1: Disease Control and Records
At the initial diagnostic visit, a comprehensive examination was done, and full-mouth radiographs and clinical photographs were taken. A consult was scheduled for 1 week later, at which treatment options were discussed and a treatment plan was accepted.
Following case acceptance, the patient arrived for the initial clinical appointment. At that time, teeth Nos. 2 and 14 were restored with a hybrid composite resin (Estelite®, Tokuyama, www.tokuyama-us.com) and resin-based adhesive (Clearfil™ SE Bond, Kuraray, www.kuraraydental.com) using standard bonding protocols after the excavation of caries. At this same appointment, alginate impressions were taken for study models, a facebow record was taken using a Kois Dento-Facial Analyzer, and occlusal records were taken using a leaf gauge. Full-arch PVS impressions were also taken.
Phase 2: Laboratory Phase
The mounted study models, PVS impressions, photographs, and a detailed laboratory slip were all sent to the laboratory for fabrication of the wax-up and provisionals. The maxillary incisal edge position was determined first, using established norms3 and the clinical photographs. Then the proper position of the maxillary occlusal plane was chosen, followed by determination of the mandibular incisal edge position and mandibular occlusal plane. A full-mouth wax-up was created in the laboratory at the prescribed OVD. The Panadent adjustable occlusal platform makes this an accurate process that gives the laboratory technician an easily visualized occlusal plane and enables changing the OVD by raising or lowering the occlusal platform on the articulator.
Using the wax-up and the models of the teeth, the laboratory fabricated the Radica composite resin onlays at the proper tooth length and position. The onlays were made in sextants to facilitate easy chairside placement.
Phase 3: Onlay Placement
Once the laboratory-fabricated onlays were completed, the patient returned to continue the treatment. At this time, tooth No. 3 was anesthetized, and the crown and all caries were removed. Provisional bonding proceeded in a similar manner to that used with the teeth in Phase 1.
All teeth were micro-abraded with 27-µm aluminum oxide at 40 psi (PrepStart™, Danville, www.danvillematerials.com), etched with phosphoric acid, rinsed, and coated with a dual-cure bonding agent (Clearfil™ Photo Bond, Kuraray). The internal surfaces of the onlays were also micro-abraded chairside, acid etched, and coated with the bonding agent. They were then bonded to the teeth with a light-cured flowable composite, Estelite flow (Tokuyama).
After light-curing, the contacts were cleared using an interproximal finishing tool (CeriSaw™, Denmat, www.denmat.com), and the excess composite was removed from the margins of the restorations using a curette. The occlusion was then evaluated and adjusted to establish equal bilateral occlusal contacts. Anesthetic was not needed to place, clean, or adjust occlusion of the onlays, except for tooth No. 3. The entire mouth was restored with the provisionals in less than 6 hours of chairtime with only three visits necessary: (1) examination and diagnosis; (2) records and impressions; and (3) delivery of the provisionals.
One of the great joys for a dental practitioner is witnessing patients seeing their new smiles for the first time. This patient smiled wider than he had in years and was overwhelmed with his new life-changing smile (Figure 7). Both he and the treating dentist were extremely pleased with not only the new smile but also that it had been created so quickly and affordably.
Phase 4: Follow-Up
Approximately 1 week following placement of the onlays, the patient returned for a postoperative evaluation and photographs (Figure 8 through Figure 12). Minor occlusal adjustments were made at this appointment. Three months following placement of the interim restorations, teeth Nos. 6 through 11 were prepared for final restorations (Figure 13). Because all the teeth were stabilized and the correct occlusion had been both established and maintained with the Radica restorations, executing the impression procedures, bite registration, and provisionalization of the six anterior teeth was routine (Figure 14).
The provisional restorations performed well over the 4 months between temporary placement and cementation of the final restorations on the upper anterior teeth. The final layered zirconia crowns were cemented following Kois Center (www.koiscenter.com) protocols, using microabrasion, Z-Prime™ priming agent (Bisco, www.bisco.com), and RelyX™ Unicem resin cement (3M ESPE, www.3m.com) (Figure 15 and Figure 16).
There are many ways to accomplish full-mouth rehabilitation. This case presentation outlines the steps used to provide this care over an extended period. The method has several benefits. First, all occlusal and esthetic issues can be worked out in the provisionals before any porcelain restorations are placed. Next, the cost of the Radica provisional restorations is relatively reasonable. Finally, because the onlays require little or no tooth preparation and are bonded primarily to enamel, the teeth are better protected and sealed than with traditionally cemented provisional restorations.
Perhaps the greatest benefit of this technique is that the patient is able to realize the improvements in esthetics, function, and comfort of the treatment immediately. In this case, these benefits motivated the patient to complete final treatment.
Acknowledgments
The wax-up and onlays were made by Swiss Dental and Technical Art Laboratory, Seattle, Washington, owned by Claudio Bucceri, CDT, master technician; the final layered zirconia crowns were made by LeBeau Dental Laboratory, Renton, Washington.
About the Author
Ronald G. Wilkins, DDS
Private Practice
Salt Lake City, Utah
References
1. Rouse JS. Sleep prosthodontics: a new vision for dentistry. Inside Dentistry. 2013;9(7):60-73.
2. Rouse JS. Sleep prosthodontics: analyzing myofascial pain. Inside Dentistry. 2013;9(12):35-39.
3. Misch CE. Guidelines for maxillary incisal edge positions-a pilot study: the key is the canine. J Prosthodont. 2008;17(2):130-134.