Implant Treatment in Maxillary Posterior: Determining the Path to Success
Barry Levin, DMD, PC; Barry Wagenberg, DMD; and Samuel Lee, DDS, DMSc
Sinus grafting vs. short dental implant: What approach would you take?
Dr. Levin
When considering “sinus graft versus short dental implant,” there is no clear, singular solution, as both approaches are substantiated in the scientific literature. The question could be posed as, “Which technique are surgeons more comfortable with in maxillary posterior sites?”
With the majority of occlusal forces on implants concentrated in crestal bone, short implants should be acceptable in most situations. This concept is mainly supported in finite-element models. In patients with meticulous oral hygiene, physiologically restored occlusions, favorable bone trabecular patterns, and adequate maintenance, short implants serve a purpose.
In patients with pre-existing periodontal diseases, excessive occlusal forces, poor bone density, and less-than-optimal hygiene, peri-implant bone loss can occur. Also, implant design may predispose patients to crestal bone modeling. Most implants are placed level to crestal bone. In posterior sites, the cortical bone at the crest is thin and is lost after functional loading in many situations, particularly those cases without platform-switched connections. In posterior edentulous sites, the length of clinical crowns can be significantly greater than natural teeth prior to tooth loss and alveolar bone resorption. Unfavorable crown-to-implant ratios may compromise prognoses of these implants.
What is often overlooked with short implants is the potential for peri-implantitis. When several millimeters of bone is lost around a 6-mm to 8-mm implant, the overall percentage of loss of osseous support can be significant, whereas with 10-mm or longer implants, the loss of 1 mm to 2 mm of bone may not significantly impact the long-term prognosis of the implant(s) and restorations. With short implants, 20% to 50% bone loss and unfavorable crown-to-implant ratios are cause for concern.
Sinus grafting is normally predictable, safe, and not associated with significant morbidity. For experienced surgeons, sinus lift surgery is typically a short, minimally traumatic procedure. No longer is there a need to harvest autogenous bone, which is often from mandibular sites. Numerous studies1,2 support various “out of the bottle” bone grafting materials for sinus elevations, and recombinant growth factors increase bone formation and shorten treatment time significantly. However, with a staged approach, treatment time, the number of procedures, and costs are increased. This is the main reason why shorter implants have grown in popularity.
Offering patients expedient, more economical options of posterior tooth replacement, such as short implants, frequently results in greater case acceptance. Also, more extensive surgical therapy requires stable systemic and localized sinus health, occasionally necessitating otolaryngologic therapy to treat antral polyps, chronic inflammation, etc., prior to sinus grafting. Additionally, patients on anticoagulant therapy often need to temporarily discontinue their medication prior to dental surgery, and minimizing the number of procedures reduces cardiovascular risks.
Evidence supports the use of short and wide-diameter implants as viable alternatives to sinus graft surgery and delayed placement of longer implants.3,4 Bone-to-implant contact with newer implant surfaces is substantially greater compared to older implant surfaces. Also, wide-diameter implants not only provide more appropriate restorative platforms, but they also increase the overall bone-to-implant contact compared to standard-diameter implants.
There are many variables that must be appreciated for each patient’s situation; therefore, one uniform approach is not realistic. After evaluating the patient’s systemic and periodontal condition, then diagnosing the occlusal and parafunctional situation, both options have a place in the treatment of posterior edentulous maxilla.
Dr. Wagenberg
In cases in which the maxillary sinus extension leaves minimal bone available for dental implant placement, the clinician faces at least four choices in deciding how to restore the posterior dentition. The four options for consideration are: a fixed bridge, if there are both mesial and distal potential abutments; a maxillary sinus lift (window approach); an internal sinus lift, if there is adequate bone available to lift; and short dental implants, if at least 4 mm of bone is available.
Most patients do not wish to have their existing dentition altered for a fixed bridge. This option is also dependent on the potential strength and viability of both abutments. However, because this approach is likely the least invasive and costly for the patient, it is an option that must be considered.
In the past, I frequently used maxillary sinus lifts with a window approach to increase the amount of bone available to support an implant of at least 10 mm in length. This is a more invasive method that increases the length of time to final restoration and is more costly than other approaches. I have avoided placing the implant at the time of the lift due to its relatively low 82% success rate in my practice and because it requires 6 months of healing prior to implant placement, at which time additional bone is added after osteotome creation of the osteotomy. Today, I reserve this approach for patients with less than 3 mm of crestal bone, performing fewer than 10 of these procedures each year.
Short implants have certain potential risks. Their design is often wide and tapered significantly. To place a 5-mm-wide implant requires a ridge of at least 7 mm, and preferably 9 mm, to have sufficient bone on the buccal and palatal to support the implant; otherwise, augmentation would be necessary to widen the ridge further. The posterior dentition receives the greatest amount of force in mastication. Some of this may be counteracted by increasing the number of implants, however this raises costs. If there is any crestal bone loss in the future, the tapered nature of this implant could place both the implants and restoration in jeopardy.
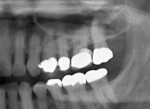
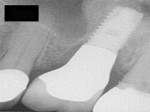
My first choice in areas with a low sinus but at least 2 mm to 3 mm of bone remaining is an internal sinus lift with osteotomes, a procedure I have performed more than 1,000 times in edentulous sites, with immediate implant placement at the time of extraction (Figure 1 and Figure 2). Careful use of osteotomes allows the clinician to create an entrance to lift the sinus internally and augment the area with bone material to help support the implant. An implant designed for soft bone is recommended. This procedure allows the clinician to place an implant of at least 10 mm in length with minimal trauma and little increased cost. It also decreases the amount of time needed for a final restoration from 1 year to 6 months.
Dr. Lee
According to Felice et al5 in a recent short-term 5-year randomized controlled trial, the survival rate of short dental implants is similar to that of long implants placed with sinus grafting. Many key opinion leaders like Beaumer6 and Misch7 suggest a minimum implant length of 10 mm to 12 mm should be used.
When discussing this topic, it is important to note that the definition of “short implants” has changed over the years from 8 mm to 5-6 mm due to enhanced surface treatments.5 But perhaps a more critical factor for osseointegration is surface area rather than the length of dental implants. As the diameter of an implant increases, it has more effect on surface area than the length of the implant. Therefore, the diameter of short dental implants plays a more critical role in a short implant’s long-term survival (in the posterior region only). As a result, short and wide dental implants (5 mm to 7 mm in diameter) have demonstrated excellent survival rates.
For the purposes of this article, I will address regular-diameter (4 mm) short implants (5 mm to 8 mm in length) compared to regular-diameter long implants (10 mm to 15 mm) in grafted sinus.
Whether crown-to-root ratio is critical when it comes to dental implants is debatable; a more relevant topic regarding implant integration and survivability is the crown to surface area. Moreover, many clinical studies that compare implants in grafted sites versus short implants fail to address biting force, lateral excursion, and parafunctional habits of the patient. Biting force is a critical factor in determining the length of dental implants in the anterior region and the diameter of implants in the posterior. Since “form follows function,” patients with heavy biting force present with a mandibular plane angle (GoGn-SN) of less than 27 degrees (brachy-facial) with a heavy antegonial notch. This heavy bite presents with deep bite, limited interocclusal spaces, exostosis, flat cusps, and group function. Therefore, it is crucial to have long dental implants in the anterior to resist lateral force and wide-diameter implants in the posterior region.
These heavy biters often present with both a wide and denser quality of bone. Presence of canine guidance is critical for the survival of short implants, as they do not handle lateral excursive forces well. Reduction of cusp angles and flattening of both curves of Spee and Wilson allow the clinician control over the occlusal scheme. Finally, parafunctional habits of the patient should be considered. Shorts implants will not perform well in lateral bruxers. Protective occlusal schemes and nightguards are highly indicated for these patients.
In summary, I am not against wide-diameter (5 mm to 7 mm) short-length (5 mm to 6 mm) dental implants. Regular-diameter (4 mm) short-length (5 mm to 6 mm) implants need to show longer survival data in studies. A minimum 10-year success rate rather than survival rate should be guaranteed in private practice to satisfy patients. Short implants are a minimally invasive approach for patients with a compromised health status who have a favorable occlusal scheme (ie, canine guidance, flat cusp angles, GoGn-SN >37 degrees, and no parafunction). However, sinus lifts can now be performed relatively easily due to new, innovative sinus tools, resulting in decreased morbidity. Today’s sinus lift/augmentation techniques are minimally invasive and highly predictable, and can be learned easily (through educational organizations such as International Academy of Dental Implantology, www.ce4dentist.com).
About the Authors
Barry Levin, DMD, PC
Diplomate
American Board of Periodontology
Clinical Associate Professor
Department of Periodontics
University of Pennsylvania School of Dental Medicine
Philadelphia, Pennsylvania
Private Practice limited to Periodontics and Implant Surgery
Jenkintown, Pennsylvania
Barry Wagenberg, DMD
Director of Dental Education and Periodontics
Newark Beth Israel Department of Dentistry
Associate Clinical Professor Department of Periodontics and Implant Dentistry
New York University School of Dentistry
Private Practice
Livingston and Roselle Park, New Jersey
Samuel Lee, DDS, DMSc
Diplomate
International Academy of Dental Implantology
Diplomate
American Board of Oral Implantology/Implant Dentistry
Private Practice limited to Periodontics and Implant Dentistry
San Diego, California
Inventor of the crestal window sinus grafting technique
References
1. Valentini P, Abensur DJ. Maxillary sinus grafting with anorganic bovine bone: a clinical report of long-term results. Int J Oral Maxillofac Implants. 2003;18(4):556-560.
2. Yildirim M, Spiekermann H, Biesterfeld S, Edelhoff D. Maxillary sinus augmentation using xenogenic bone substitute material Bio-Oss in combination with venous blood. A histologic and histomorphometric study in humans. Clin Oral Implants Res. 2000;11(3):217-229.
3. Schincaglia GP, Thoma DS, Haas R, et al. Randomized controlled multicenter study comparing short dental implants (6 mm) versus longer dental implants (11-15 mm) in combination with sinus floor elevation procedures. Part 2: clinical and radiographic outcomes at 1 year of loading. J Clin Periodontol. 2015;42(11):1042-1051.
4. Renouard F, Nisand D. Short implants in the severely resorbed maxilla: a 2-year retrospective clinical study. Clin Implant Dent Relat Res. 2005; 7 suppl 1:S104-S110.
5. Felice P, Cannizzaro G, Barausse C, et al. Short implants versus longer im-plants in vertically augmented posterior mandibles: a randomised controlled trial with 5-year after loading follow-up. Eur J Oral Implantol. 2014;7(4):359-369.
6. Beumer J III, Faulkner RF, Shah KC, Moy PK. Fundamentals of Implant Dentistry, Volume 1: Prosthodontic Principles. Hanover Park, IL: Quintessence Publishing Co., Inc.; 2015.
7. Misch CE. Contemporary Implant Dentistry. 3rd ed. St. Louis, MO: Mosby Elsevier; 2008.