Surgical and Prosthetic Management of Implants: Single and Full-Arch Reconstruction
Sergio Rubinstein, DDS; Barry P. Levin, DMD; and Toshiyuki Fujiki, RDT
Abstract: Whether it’s a single tooth or multiple teeth, tooth loss has esthetic, functional, and health implications. Replacing multiple teeth can be especially complicated due to the loss of surrounding structures, often making it necessary to use additional procedures—eg, bone grafting—to solve the problems that arise. Fortunately, modern techniques and materials in dentistry enable clinicians to replace and mimic lost teeth in a realistic, healthy, and functional way like no other field in medicine. This report discusses two cases that involve multiple subspecialties working synergistically to accomplish ideal tooth replacement and emphasizes the importance of proper diagnosis, treatment planning, and execution of surgical and restorative therapy to achieve optimal results.
Dental issues related to trauma, disease, genetics, developmental problems, decay, neglect, or even iatrogenic factors, can, in many circumstances, be reversed using multiple available treatment options and advanced, ever-evolving materials and techniques. The treating doctor(s) and the patient should always strive for the best possible treatment. Long-term health, stability, function, and esthetics are priorities when presenting patients with all available options, even when they appear to be extreme. It is the responsibility of the dental team to educate and properly guide the patient in order to achieve the expected results through proper diagnosis, detailed treatment planning, and meticulous execution.
The more complicated the case, the more all the doctors should be involved. However, the key to successful interdisciplinary treatment is clear communication within the team, as it is essential to define what is expected from each team member. Optimal results are required in each phase so each discipline can ultimately reach its intended goals without compromising the efforts of another. Success is determined not only by the initial and staged combination of tasks to be accomplished, but also by the longevity and optimal maintenance of the provided treatment.
Replacing Lost Structures
The loss of one or several teeth will inherently create a shrinkage of the surrounding bone and soft tissue, thus affecting not only esthetics but creating the dilemma of determining how the lost tooth/teeth and adjacent supporting structures should be reconstructed. Practitioners may tend to rely on one technique or discipline to compensate for a deficiency that another failed to resolve or correct. There may be limitations when managing osseous defects and, on a smaller scale, the proper regeneration of soft tissues, mostly in a vertical dimension, which can be extremely challenging. The results from bone regeneration techniques can sometimes fall short of expectations, or the developed soft-tissue biotype may not provide the ideal or anticipated outcome. While bone-grafting techniques can provide outstanding results,1-16 or if necessary, is done in conjunction with osteodistraction techniques,17-20 the expertise of the restorative dentist and ceramist is frequently required to maximize any deficiencies the surgical techniques were unable to ideally correct since there are some limitations to any surgical procedure. Using pink porcelain21-25 has its inherent challenges, but it is an example of an approach that can greatly enhance the esthetic outcome by creating a better esthetic proportion of the final restoration.
Whether it’s a single tooth replacement or a full-arch reconstruction, the goal is to create the best environment for a future restoration. This means excellent integration of the implant, abutment, and final restoration, surrounded by healthy bone and soft tissue that is able to withstand the function and maintenance to which the restoration will be subjected over the years. The goals for the restorative team are to create balance between healthy supportive bone in quantity and quality, with proper soft-tissue support of restorations. An implant that is properly placed in consideration of adjacent anatomical structures and preservation of a healthy buccal plate, and that will preserve the bone to the top threads of the titanium fixture, will enable the restorative dentist to achieve optimal esthetic outcomes.26
Case 1
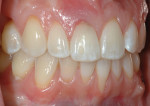
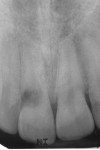
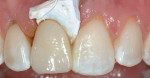
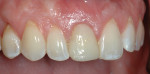
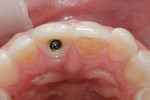
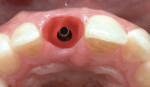
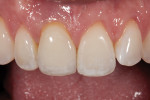
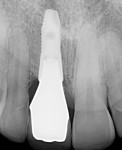
A 30-year-old patient presented with external resorption of a maxillary central incisor, tooth No. 8 (Figure 1). The patient understood that the tooth would be lost and looked forward to a replacement that would be esthetically pleasing, healthy, and functional. Multiple challenges included management of the extraction of the tooth in the least traumatic manner by proper manipulation of the soft tissues, and the best possible maintenance of the alveolar ridge and supporting interproximal papillae (Figure 2).
Whenever immediate placement of the implant is considered—whether loaded for soft-tissue support but without function, or unloaded—it is a decision that should be made with an understanding of what is best in each individual case. The availability of a facial cortical plate is crucial, not only for long-term esthetics but also for the implant to function for years to come.
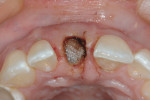
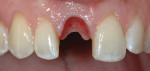
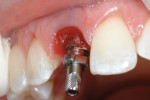
When the tooth is extracted, the maintenance of papillae height is a major challenge. It must be managed by proper surgical technique along with an interim restoration that will provide acceptable esthetics and stability. The purpose of the described procedure is to maintain maximum horizontal and vertical ridge dimensions, thus facilitating prosthetically driven implant placement. There is substantial clinical efficacy of socket grafting, as it facilitates optimal implant placement by preserving hard- and soft-tissue dimensions superior to physiologic modeling and remodeling after extraction.27 As shown in Figure 3, ridge preservation using a mineralized allograft (Puros®, Zimmer Dental, www.zimmerdental.com) and a bioresorbable membrane was performed without reflection of a mucoperiosteal flap. Immediate implant placement was not indicated at this point, and the graft was allowed to heal for 6 months.
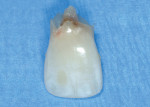
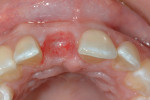
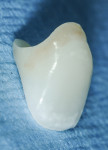
In this case, the same tooth (No. 8) was modified using composite material, creating an ovate shape for proper gingival healing, tissue height, and interproximal support (Figure 4 through Figure 6). The extraction site and the tissue response must be closely evaluated in order to determine if additional bonding needs to be added or removed based on the tissue response. Among the advantages of this technique is that the patient avoids any period of edentulism following extraction (in this case, the same tooth, but modified), but just as important, the tooth is fixed instead of being a removable appliance. Other important benefits are that the restorative procedure is cost-effective and excellent support is provided for the surrounding healing tissues.
Healing after 3 weeks from the tooth being extracted can be seen in Figure 6. Gingival height was actually coronal to the adjacent tooth and was more favorable compared to prior to the extraction. The tooth was slightly shorter to avoid any contact in a protrusive movement during the healing phase.
Once healing has occurred, the bonded tooth is removed and an implant is placed. It is extremely beneficial for the surgeon to have a clear understanding of the prosthetic plan at this point, since implant position for a cemented or screw-retained crown can be significant as it relates to the final contours and materials to be used for the provisional and final restoration (Figure 7 and Figure 8). This typically should result in an implant placed in a palatal position, relative to the horizontal implant location buccal-palatally. The depth of the implant platform also must be placed approximately 3 mm to 4 mm apical to the anticipated gingival zenith of the final restoration. This is best achieved with a surgical template accurately representing the contours of the final restoration. When this cannot be performed due to anatomic considerations, communication between the surgeon and restorative dentist is critical prior to surgery so adequate planning regarding provisionalization can occur. A preoperative cone-beam computed tomography (CBCT) scan with a radiopaque template allows the team to anticipate the eventual implant position and plan accordingly moving forward.
Provisional And Final Restorations
After the implant has osseointegrated, a provisional utilizing the implant is created to reproduce the anatomical contours of the extracted tooth in addition to the emergence tissue profile27-29 (Figure 9 and Figure 10), which must be created prior to taking a final impression. While there is documentation about the use of different impression materials and techniques, whenever possible it is best to take a final impression with the pick-up–open-tray technique,30,34 thus eliminating the need to transfer the impression post from the mouth onto the impression, as shown in Figure 11. Since the screw access was slightly buccal, complicating fabrication of a screw-retained crown, and there was concern about a lack of support at the incisal third for the substructure, a screw-retained zirconia abutment and cementable crown were designed as the final restoration (Figure 12 and Figure 13).
Although ideal dentistry is not always achievable—eg, in this case, the patient did not agree to have connective tissue grafting done to cover the exposed roots—it is important for the final restoration to reproduce the anatomical contours of the adjacent teeth and roots (Figure 14 and Figure 15).
Case 2
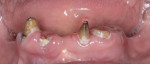
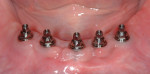
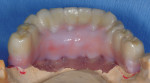
Depending on the specific problem(s) of a tooth or teeth, there will likely be multiple treatment options available. If the tooth or teeth have a hopeless prognosis, diagnosis is quite simple since extraction(s) is the solution (Figure 16 and Figure 17). When all remaining teeth require extraction, treatment options are numerous, with the high predictability of osseointegration and various designs available with dental implants.
Periapical radiographs, as seen in Figure 16, in addition to computerized tomograms and planning, provide excellent diagnostic information and are extremely valuable for the surgical planning and help serve to reduce unforeseen surprises during the surgical procedure. Evaluation of quality and quantity of bone, in addition to mandibular nerve location before the actual procedure, are in line with standard of care in modern implant practice. The accuracy of compact and microfocus CT scans have made identification of vital structures a practical and safe procedure prior to surgery.35-41
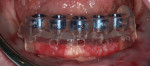
Computer-generated guides (Figure 18) not only simplify the surgical procedure, they also ultimately provide the restorative dentist and laboratory technician the ability to create the best possible restoration for bone preservation and optimal oral hygiene (Figure 19).
Provisional and Final Restoration Considerations
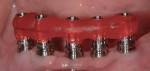
When multiple implants are present, a final impression is taken with an open-tray technique for best accuracy, since impression posts do not require to be transferred.34 On the final stone model, a jig is fabricated to verify that the impression is accurate and the final prosthesis will have a passive fit.42-45 In the mouth, the index is tried and either visual or radiographic passive fit must be confirmed before proceeding with the design of the final prosthesis (Figure 20).
A provisional is delivered to the patient verifying a passive fit, comfort, esthetics, function, and ability to perform oral hygiene. Any corrections must be addressed during this phase of treatment, and once the patient has given approval, the provisional is duplicated to reproduce proper contours for the construction of the final prosthesis (Figure 21 and Figure 22).
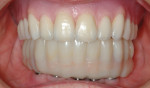
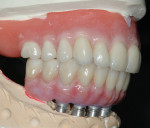
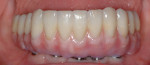
Material and technique selection must be based on the needs of each individual patient. In this instance, a full-zirconia bridge was fabricated (Figure 23). For this particular technique, it is essential to have an accurate model to verify a passive fit before the creation of the final prosthesis, because it is not possible to section, solder, or reconnect the bridge (Figure 24).
Conclusions
Implant therapy involves multiple subspecialties working synergistically to accomplish ideal tooth replacement. Surgeons and restorative dentists may collaborate to provide long-term solutions for patients of various ages and with multiple conditions. Surgical management of hard and soft tissues can accomplish goals thought to be unrealistic at the inception of implantology. Despite the importance of surgical management, the ultimate goals of tooth/teeth replacement with implants are often in the hands of the prosthodontist and laboratory technicians. The rapid evolution of ceramics—both substructures and prostheses—has greatly enhanced esthetic outcomes. The proper diagnosis, treatment planning, and execution of surgical and restorative therapy often leads to results thought unattainable just a few years ago.
Technology continues to improve at a rapid pace. It is the clinician’s responsibility to utilize scientifically proven modalities to complement the time-tested arts of diagnostics and treatment planning to help patients achieve hygienic and esthetic outcomes that offer long-term stable function.
About the Authors
Sergio Rubinstein, DDS
Private Practice
Dental Reconstruction Center
Skokie, Illinois
Barry P. Levin, DMD
Clinical Associate Professor of Periodontics
University of Pennsylvania School of Dental Medicine
Philadelphia, Pennsylvania
Private Practice
Jenkintown, Pennsylvania
Toshiyuki Fujiki, RDT
Master Laboratory Technician
Dental Reconstruction Center
Skokie, Illinois
References
1. Summers RB. A new concept in maxillary implant surgery: the osteotome technique. Compend Cont Educ Dent. 1994;15(2):152-158.
2. Hahn J. Clinical uses of osteotomes. J Oral Implantol. 1999;25(1):23-29.
3. Al-Maseeh J, Levin B, Symeonides E. The osteotome technique: a classification for technique approach and clinical case reports. Compend Contin Educ Dent. 2005;26(8):551-556.
4. Lazzara, RJ. Immediate implant placement into extraction sites: surgical and restorative advantages. Int J Periodontics Restorative Dent. 1989;9(5):333-342.
5. Ashman A. An immediate tooth root replacement: an implant cylinder and synthetic bone combination. J Oral Implantol. 1990;16(1):28-38.
6. Becker W, Becker BE. Guided tissue regeneration for implants placed into extraction sockets and for implant dehiscences: surgical techniques and case reports. Int J Periodontics Restorative Dent. 1990;10(5):377-391.
7. Barzilay I, Graser GN, Iranpour B, Natiella JR. Immediate implantation of a pure titanium implant into an extraction socket: report of a pilot procedure. J Oral Maxillofac Implants. 1991;6(3):277-284.
8. Caudill RF, Meffert RM. Histologic analysis of the osseointegration of endosseous implants in simulated extraction sockets with and without e-PTFE barriers. 1. Preliminary findings. Int J Periodontics Restorative Dent. 1991;11(3):207-215.
9. Seibert J, Nyman S. Localized ridge augmentation in dogs: a pilot study using membranes and hydroxyapatite. J Periodontol. 1990;61(3):157-165.
10. Becker W, Becker BE, Handlesman M, et al. Bone formation at dehisced dental implant sites treated with implant augmentation material: a pilot study in dogs. Int J Periodontics Restorative Dent. 1990;10(2):92-101.
11. Nyman S, Lang NP, Buser D, Bragger U. Bone regeneration adjacent to titanium dental implants using guided tissue regeneration: a report of two cases. Int J Oral Maxillofac Implants. 1990;5(1):9-14.
12. Wachtel HC, Langford A, Bernimoulin JP, Reichert P. Guided bone regeneration next to osseointegrated implants in humans. Int J Oral Maxillofac Implants. 1991;6(2):127-135.
13. Jensen OT, Brownd C, Delorimier J. Esthetic maxillary arch vertical location for the osseointegrated cylinder implant. J Am Dent Assoc. 1989;119(6):735-736.
14. Boyne PJ, James RA. Grafting of the maxillary sinus floor with autogenous marrow and bone. J Oral Surg. 1980;38(8):613-616.
15. Wallace SS, Froum SJ. Effect of maxillary sinus augmentation on the survival of endosseous dental implants. A systematic review. Ann Periodontol. 2003;8(1):328-343.
16. Del Fabbro M, Testori T, Francetti L, Weinstein R. Systematic review of survival rates for implants placed in the grafted maxillary sinus. Int J Periodontics Restorative Dent. 2004;24(6):565-577.
17. Samchukov ML, Cope JB, Cherkashin AM. Craniofacial Distraction Osteogenesis. St. Louis, MO: Mosby; XIX 2001.
18. Dessner S, Razdolsky Y, el-Bialy T. Surgical and orthodontic considerations for distraction osteogenesis with ROD appliances. Atlas Oral Maxillofac Surg Clin North Am. 2001;9(1):111-139.
19. El-Bialy TH, Razdolsky Y, Kravitz ND, et al. Long- term results of bilateral mandibular distraction osteogenesis using an intraoral tooth-borne device in adult Class II patients. Int J Oral Maxillofac Surg. 2013;42(11):1446-1453.
20. Rubinstein S, Nidetz AJ, Heffez LB, Fujiki T. Prosthetic management of implants with different osseous levels. Quintessence of Dental Technology. 2006;29:147-156.
21. Coachman C, Salama M, Garber D, et al. Prosthetic gingival reconstruction in fixed partial restorations. Part 1: introduction to artificial gingiva as an alternative therapy. Int J Periodontics Restorative Dent. 2009;29(5):471-477.
22. Salama M, Coachman C, Garber D, et al. Prosthetic gingival reconstruction in the fixed partial restoration. Part 2: diagnosis and treatment planning. Int J Periodontics Restorative Dent. 2009;29(6)573-581.
23. Coachman C, Salama M, Garber D, et al. Prosthetic gingival reconstruction in fixed partial restorations. Part 3: laboratory procedures and maintenance. Int J Periodontics Restorative Dent. 2010;30(1):19-29.
24. Coachman C, Van Dooren E, Gurel G, et al. Minimally invasive reconstruction in implant therapy: the prosthetic gingival restoration. Quintessence of Dental Technology. 2010;33:61-75.
25. Coachman C, Garber D, Salama M, et al. The incorporation of tissue colored composite and a zirconium abutment to solve an esthetic soft tissue asymmetry. Inside Dentistry. 2008;4(9)82-87.
26. Barone A, Ricci M, Tonelli P, et al. Tissue changes of extraction sockets in humans: a comparison of spontaneous healing vs. ridge preservation with secondary soft tissue healing. Clin Oral Implants Res. 2013;24(11):1231-1237.
27. Rubinstein S, Salama MA, Garber DA, Salama H. The reverse pathway: parameters for the integration of function and aesthetics with implants. Journal of Implant & Advanced Clinical Dentistry. 2010;2(4):19-29.
28. Saadoun AP, LeGall M, Touati B. Selection and ideal tridimensional implant position for soft tissue aesthetics. Pract Periodontics Aesthet Dent. 1999;11(9):1063-1072.
29. Saadoun AP. Multifactorial parameters in peri-implant soft tissue management. In: Romano R. The Art of Treatment Planning: Dental and Medical Approaches to the Face and Smile. London: Quintessence Publishing; 2009:75-153.
30. Lee H, So JS, Hochstedler JL, Ercoli C. The accuracy of implant impressions: a systematic review. J Prosthet Dent. 2008;100(4):285-291.
31. Daoudi MF, Setchell DJ, Searson LJ. A laboratory investigation of the accuracy of two impression techniques for single-tooth implants. Int J Prosthodont. 2001;14(2):152-158.
32. Walker MP, Petrie CS, Haj-Ali R, et al. Moisture effect on polyether and polyvinylsiloxane dimensional accuracy and detail reproduction. J Prosthodont. 2005;14(3):158-16.
33. Bambini F, Ginetti L, Memĕ L, et al. Comparative analysis of direct and indirect impression techniques: An in vitro study. Minerva Stomatol. 2005;54(6):395-402.
34. Prithviraj DR, Pujari ML, Garg P, Shruthi DP. Accuracy of the implant impression obtained from different impression materials and techniques: review. J Clin Exp Dent. 2011;3(2):e106-e111.
35. McGivney GP, Houghton V, Strandt JA, et al. A comparison of computer-assisted and data-gathering modalities in prosthodontics. Int J Oral Maxillofac Implants. 1986;1(1):55-68.
36. Schwarz MS, Rothman SL, Rhodes ML, Chafetz N. Computed tomography: Part I. Preoperative assessment of the mandible for endosseous implant surgery. Int J Oral Maxillofac Implants. 1987;2(3):137-141.
37. Schwarz MS, Rothman SL, Rhodes ML, Chafetz N. Computed tomography: Part II. Preoperative assessment of the maxilla for endosseous implant surgery. Int J Oral Maxillofac Implants. 1987;2(3):143-148.
38. Lindh C, Petersson A. Radiographic examination for location of the mandibular canal: a comparison between panoramic radiography and conventional tomography. J Oral Maxillofac Implants. 1989;4(3):249-253.
39. Clark DE, Danforth RA, Barnes RW, Burtch ML. Radiation absorbed from dental implant radiography: a comparison of linear tomography, CT scan and panoramic and intraoral techniques. J Oral Implantol. 1990;16(3):156-164.
40. Naitoh M, Katsumata A, Mitsuya S, et al. Measurement of mandibles with microfocus x-ray computerized tomography and compact computerized tomography for dental use. Int J Oral Maxillofac Implants. 2004;19(2):239-246.
41. Pyun JH, Lim YJ, Kim MJ, et al. Position of the mental foramen on panoramic radiographs and its relation to the horizontal course of the mandibular canal: a computed tomographic analysis. Clin Oral Implants Res. 2013;24(8):890-895.
42. Duyck J, Van Oosterwyck H, Vander Sloten J, et al. Pre-load on oral implants after screw tightening fixed full prostheses: an in vivo study. J Oral Rehabil. 2001;28(3):226-233.
43. Natali AN, Gasparetto A, Carniel EL, et al. Interaction phenomena between oral implants and bone tissue in single and multiple implant frames under occlusal loads and misfit conditions: A numerical approach. J Biomed Mater Res B Appl Biomater. 2007;83(2):332-339.
44. de Sousa SA, de Arruda Nobilo MA, Henriques GE, Mesquita MF. Passive fit of frameworks in titanium and palladium-silver alloy submitted the laser welding. J Oral Rehabil. 2008;35(2):123-127.
45. de Torres EM, Rodrigues RC, de Mattos Mda G, Ribeiro RF. The effect of commercially pure titanium and alternative dental alloys on the marginal fit of one-piece cast implant frameworks. J Dent. 2007;35(10):800-805.