Intraoral Digital Impressioning for Dental Implant Restorations Versus Traditional Implant Impression Techniques
Brian L. Wilk, DMD
Abstract: Over the course of the past two to three decades, intraoral digital impression systems have gained acceptance due to high accuracy and ease of use as they have been incorporated into the fabrication of dental implant restorations. The use of intraoral digital impressions enables the clinician to produce accurate restorations without the unpleasant aspects of traditional impression materials and techniques. This article discusses the various types of digital impression systems and their accuracy compared to traditional impression techniques. The cost, time, and patient satisfaction components of both techniques will also be reviewed.
Intraoral digital impression systems have been commercially available for more than 25 years.1 The first scannable implant was introduced in 2004 (BIOMET 3i); it utilized a coded implant healing abutment. This abutment provided all the 3-dimensional information of the location of the dental implant in relation to the adjacent and opposing teeth. As with a traditional impression the exact position of the dental implant was captured, including the internal orientation of the implant’s anti-rotational properties such as internal hex and anti-rotational grooves. Most of these scans were done after a traditional dental impression was taken, and the resultant model was then scanned by the dental laboratory. This technique still subjected patients to dental impression materials, and no time or cost savings were associated with it.1
In 2010 unique scannable impression copings (scan bodies) were introduced, which could be placed on the implant and scanned intraorally using a parallel confocal imaging system. Although this now eliminated the traditional impression technique, this approach was limited to only one implant system and one intraoral scanning device.2 In the past few years a number of scanning systems have come to market that are capable of scanning multiple implant systems and multiple implant platforms.3,4 There are two basic types of scanners available today: either a blue LED (light emitting diode) type, which is considered an optical scanner that usually requires the use of a powder, or scanners that use lasers to scan and record distances from the tooth surface to capture the image and build the digital model. More recently, most scanners utilize the laser technology to eliminate the use of powder, considered to be one of the early drawbacks encountered by dentists.
Dental Implant Scanning Procedure
With the dental implant scanning procedure, as is the case in any crown and bridge impression, including those supported by dental implants, an impression must be made and a model must be fabricated. In traditional crown and bridge restorations, typically a polyether or polyvinylsiloxane (PVS) impression is taken and then poured in stone to create a master model. Once that model is poured, the corresponding dies are ditched and indexed. This process can be time-consuming. Joda and Brigger reported that a digital intraoral implant impression procedure from the time of removal of the healing cap to the replacement of the healing cap was approximately 3 minutes less than its traditional polyether impression counterpart.5 Once the impression is made a model must be fabricated. The traditional impression must be disinfected and sent to the dental laboratory, and, in most cases, the technician does not even look at the physical model for 48 to 72 hours.6 In the digital workflow, using an intraoral scanner, all the critical data is transferred via the Internet as digital files enabling work to commence on designing the abutment and crown the day the digital impression is taken without ever having to manufacture models for either abutment or crown.6
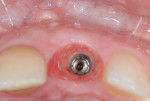
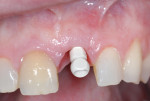
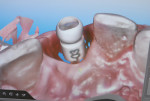
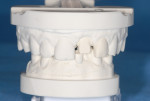
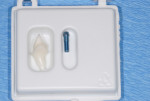
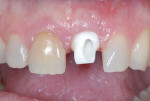
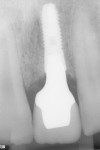
Although there are a number of intraoral impression systems on the market today they all have a similar workflow. The first step involved, once implant integration and tissue maturation is complete, is to appoint the patient for a digital implant transfer scan. This scan is analogous to a traditional implant transfer impression. Instead of a traditional implant transfer coping a scannable coping is used (Figure 1). Once the scannable coping is placed into the implant (Figure 2 and Figure 3), proper seating is confirmed with a radiograph, which is critical because the case will be going to completion with a final abutment and crown. The clinician does not want to incur the expense of a second restoration if the abutment is not seated properly.
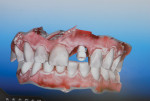
Next, the scanning is performed and a 3-dimensional (3-D) model of the region is visualized on the screen evaluating that all necessary surfaces of the scannable impression coping are present for the manufacture of the abutment and crown. These areas include the impression coping, the contact areas of all adjacent teeth, gingival tissue, opposing arch, and bite registration6 (Figure 4 and Figure 5).
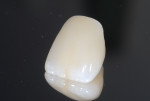
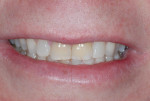
After the scanning is completed, the laboratory instructions, including shade, abutment material selection (titanium or zirconia), and crown material selection, are then placed into the prescription to the milling center and laboratory and sent via the Internet for the fabrication process to begin. At this point the model, abutment, and crown may be made by the same laboratory or separate facilities depending on the scanning system being utilized (Figure 6 through Figure 8). Once the abutment and crown are completed, the insertion visit is no different from a usual implant abutment and crown delivery appointment to seat the completed abutment and crown cementation (Figure 9 through Figure 11).
Advantages of Digital
With the advent of digital impression techniques all the advantages of crown fabrication remain intact with the addition of several advantages in the fabrication of the implant abutment. One of the major advantages in the digital implant impression is the elimination of the unpleasant taste and gagging sensation that the patient experiences with a traditional impression.5,7 As clinicians are well aware, patients for years have disliked, and even feared, dental impressions to the point of avoiding dentist visits entirely. In one recent study with 24 patients (12 male, 12 female) who had no prior experience with either conventional or digital impressions, 100% of the patients preferred the digital impressions (CEREC® Omnicam, Sirona Dental Inc., www.sirona.com) over their conventional counterparts. This study reinforces the need to continue the evolution of digital solutions in impression and fabrication of dental restorations on patients.7
Of course, patients’ preferences should not dictate treatment decisions; therefore, it is important to examine all the factors that impact dentists on a daily basis and the materials and techniques used to complete the procedures. The primary concern of dentists when adopting new techniques or technology is whether or not the new method is as accurate, fast, comfortable, predictable, and cost-effective as what they used in the past. It is difficult to find a technology that encompasses all of these improvements, and there are usually tradeoffs.
Accuracy when restoring implants has long been known to be a key in implant survival and esthetics.8 Poorly fitting restorations and abutments can lead to implant and restoration failure. There are many steps involved in the traditional implant impression, and each step incrementally adds to increased distortion of the final restoration. This includes inherent dimensional stability of the impression material and the dental stone used to pour the models. As mentioned earlier, the original scanning of dental implants took place in the laboratory on a gypsum model obtained from the traditional impression techniques, thus all distortions created from traditional impression techniques were just added to the overall distortion of those restorations. Currently, with the many intraoral scanners on the market, implant impressions are scanned directly and either milled or 3-D printed. In fact, the virtual model can be used to design and mill the abutment and restoration as well as a physical model with a removable implant analog. Multiple studies have shown that direct scanning of dental implants is as accurate as its traditional counterpart.2,9
Chairtime is one of the largest components to the cost of any procedure in a dental office.4,5 Numerous studies have shown that digital impression systems save time in the chair during the impression stage, but, moreover, they also reduce the number of retakes and laboratory remakes to almost zero since the impression and virtual mounted model can be evaluated prior to sending to the dental lab.10,11 Once at the lab, the 3-D models can also be evaluated for clearance, contacts, and position prior to fabrication of any abutments and crowns. Frequently, problems are found prior to fabrication, which can save all parties involved, including the patient, lab, and dentist, valuable time and money. Laboratory fees are another significant part of office overhead. The digital solution can be executed in a model-less manner avoiding implant lab analogs and costly mounted models and articulators; in all cases expensive impression material and trays are avoided. The only additional cost incurred in the digital solution is the cost of the scanner, but this cost is more than offset by the savings in chairtime and materials over time.12
Conclusion
One of the biggest hurdles a restorative dentist still needs to overcome is the realization that intraoral scanning of crowns and dental implants is now just as accurate, faster, and, in the long run, less costly than traditional impression techniques. In essence, the greatest challenge is the dentist’s own fear of an unknown clinical procedure and technique that has now existed for quite a few years. Consider that most clinicians today are using a digital radiography system, yet in the 1990s very few had adopted that technology; and in the 1980s most practitioners were not using practice management software, which, of course, is used almost universally today.
The decision to adopt this new technology should be carefully evaluated, as it is advancing at a rapid rate. Most systems are now powderless, and the scanners are becoming faster and more versatile in their functionality. The systems can be used in applications ranging from simple restorative inlays and onlays, to crowns, bridges, and dental implants, and even clear aligner therapy.
About the Author
Brian L. Wilk, DMD
Private Practice
Restorative
Esthetic and Implant Dentistry
Chalfont, Pennsylvania
References
1. Boudet CA. Scannable abutments: digital impressions for dental implants. Chairside. 2012:7(3):45-48.
2. Moreira AH, Rodrigues NF, Pinho AC, et al. Accuracy comparison of implant impression techniques: a systematic review. Clin Implant Dent Relat Res. 2015; Apr 1. doi:10.1111/cid.12310. [Epub ahead of print]
3. Kachalia PR, Geissberger MJ. Dentistry a la carte: in-office CAD/CAM technology. J Calif Dent Assoc. 2010;38(5):323-330.
4. Patzelt S, Lamprinos C, Stampf S, Att W. The time efficiency of intraoral scanners: an in vitro comparative study. J Am Dent Assoc. 2014;145(6):542-551.
5. Joda T, Brägger U. Patient-centered outcomes comparing digital and conventional implant impression procedures: a randomized crossover trial. Clin Oral Implants Res. 2015; Apr 12. doi:10.1111/clr.12600. [Epub ahead of print]
6. Knight R. Top 6 benefits of digital impressions and a model-less workflow. Dental Products Report. 2013;5:1-5.
7. Wismeijer D, Mans R, van Genuchten M, Reijers HA. Patients’ preferences when comparing analogue implant impressions using a polyether impression material versus digital impressions of dental implants. Clin Oral Impl Res. 2014;25(10):1113-1118.
8. Bhakta S, Vere J, Calder I, Patel R. Impressions in implant dentistry. Br Dent J. 2011;211(8):361-367.
9. Lee SJ, Betensky RA, Gianneschi GE, Gallucci GO. Accuracy of digital versus conventional implant impressions. Clin Oral Implants Res. 2015;26(6):715-719.
10. Smith R. Creating well-fitting restorations with a digital impression system. Compend Contin Educ Dent. 2010;31(8):640-644.
11. Nayar S, Mahadevan R. A paradigm shift in the concept for making dental impressions. J Pharm Bioallied Sci. 2015;7(suppl 1):S213-S215.
12. Hakim F, Kachalia PR. Implementation strategies for incorporating new technologies into the dental practice. J Calif Dent Assoc. 2010;38(5):337-341.