Adjunctive Treatment of Periodontal Disease with Self-Adhesive Hydrogel Wound Dressing: Case Series
David W. Paquette, DMD, MPH, DMSc; and William Z. Levine, DDS
Abstract
Periodontal disease (periodontitis) is a common inflammatory condition affecting the deep, supporting tissues around teeth. While specific bacteria in plaque biofilm initiate the disease process, host immuno-inflammatory responses are responsible for the majority of tissue destruction. Conventional methods for controlling periodontitis include mechanical removal of the biofilm—with or without surgical access—and the adjunctive use of chemotherapeutics (antimicrobials or host modulators). PerioPatch™ is an approved device product that has been developed as an oral adhesive barrier for promoting healing in inflamed oral/gingival tissues and reducing pain, irritation, and the symptoms of inflammation. In this case series, which documented the adjunctive benefits of PerioPatch therapy in patients with chronic periodontitis, 9 patients who presented with generalized moderate to severe chronic periodontitis were treated with scaling and root planing plus adjunctive PerioPatch devices. Patients applied the devices to identified areas with periodontal pocketing (≥ 6 mm at baseline) twice daily at Day 1, then once daily for Days 2 to 7. Three of the patients additionally applied devices to the treatment sites on Days 15 to 21. Patients were evaluated for changes in probing parameters at 4 to 6 weeks. RESULTS: Clinical examinations performed at baseline and post-treatment indicated consistent pocket depth reductions (mean 2.8 mm) and resolution of bleeding on probing (94%). Patients complied with the application schedule and reported no adverse effects. The authors conclude that within the confines of this case series, the PerioPatch is a novel but simple device that can be used adjunctively with scaling and root planing for the management of chronic periodontitis.
Inflammatory periodontal disease, or periodontitis, is one of the most common, chronic conditions affecting patients and populations worldwide. The condition, marked by destruction of the supporting structures around teeth, affects up to half of the US adult population.1 Periodontitis is the leading cause of tooth loss among adults,2 and observational studies indicate consistent associations with poorer systemic health, including diabetic complications and cardiovascular diseases.3,4
The primary etiology of periodontal diseases is the bacterial biofilm that includes defined pathogenic complexes in a protected matrix adherent to the teeth and proximal to periodontal tissues. In particular, an “orange complex” of bacteria, which includes bacteria such as Fusobacterium nucleatum and Prevotella intermedia, has been highly associated with early periodontitis.5 Similarly, a “red complex” that includes Porphyromonas gingivalis, Tannerella forsythia, and Treponema denticola has been consistently associated with moderate to severe chronic periodontitis.5 These complexes set in motion the myriad of host inflammatory reactions (both local and systemic) that result in the characteristic clinical signs of the disease, such as gingival erythema and edema, bleeding on probing, and, in late stages, periodontal pocket formation, clinical attachment loss, and alveolar bone resorption. Host inflammatory mediators implicated in these local pathophysiological events include beta-glucuronidase (ie, a marker of polymorphonuclear leukocyte function), prostaglandins, matrix metalloproteinases (MMPs), and cytokines such as interleukin-1β (IL-1β) and tumor necrosis factor-α (TNF-α).6 These mediators are consistently elevated in the periodontal tissues or crevicular fluid obtained from periodontally diseased subjects (versus controls) and are lowered following therapy.6-8
The mechanical disruption and removal of the bacterial biofilm via scaling procedures remains the cornerstone of periodontal treatment. Adjunctive approaches using antimicrobial and host modulatory (anti-inflammatory) agents have been adopted as routine clinical practice. The clinical use of adjunctive antimicrobial and host modulatory agents is supported by clinical trials indicating consistent improvements in periodontal parameters such as pocket depth or clinical attachment level beyond mechanical therapy alone in patients.9-11 Interestingly, the control or resolution of inflammation may carry over and positively affect the bacterial biofilm and host healing. In a recent study of experimental periodontitis in rabbits, Hasturk et al demonstrated that treatment with an endogenous, host modulatory lipid derivative (ie, resolvin E1 topically applied) reversed the periodontal inflammatory response, eliminated oral P. gingivalis infection, and regenerated lost periodontal tissues.12 The authors postulated that in “resolving” the local inflammatory lesion, the ecological niche (ie, nutrient source) for P. gingivalis was removed and conditions were favorable for host regeneration of lost tissues. While these data present with limitations, they do highlight the importance of managing the inflammatory component of periodontal diseases.
Absorptive, Flexible Barrier
The PerioPatch™ (Figure 1) (Izun Pharmaceuticals, https://izunpharma.com) is an approved medical device product that is broadly intended for the management of all types of oral wounds, injuries, and ulcerations of the gingival and oral mucosa. The device is a self-adhesive hydrogel wound dressing that provides an absorptive and flexible barrier over the affected, inflamed gingival or mucosal area. The PerioPatch device is elliptical in shape (24 mm x 8 mm x 190 μm) and is provided in a six-unit prescription dose pack. When applied to an inflamed gingival or oral wound, the device fosters repair via protection from further irritation and reduction in the local inflammatory burden.
PerioPatch devices are made entirely of natural ingredients generally recognized as safe (GRAS), including an ethyl cellulose backing plus polyacrylic acid, castor oil, acacia gum, methyl hydroxypropyl cellulose, glycerol, strawberry flavor, and the extracts from three plants (Sambucus nigra, Centella asiatica, and Echinacea purpurea). Following application of the device, the protective backing is shed within 2 hours. A hydrogel film may remain for up to 5 hours, which is intended to reduce chronic wound fluid and the inflammatory infiltrate. The PerioPatch device is indicated for the management of various types of oral conditions, including stomatitis, minor chafing, and traumatic ulcers and abrasions caused by orthodontic appliances or ill-fitting dentures and lesions associated with oral surgery. The device is contraindicated for those patients with sensitivity to any of the device ingredients (eg, plant extracts). Because all of the device components are edible, there is no risk if any part of the PerioPatch is swallowed.
The objective of this case series was to assess the clinical performance of the PerioPatch device when used as an adjunct to scaling and root planing in patients with moderate to severe chronic periodontitis.
Discussion of Case Series
Nine adult patients (six females and three males) diagnosed with generalized moderate to severe chronic periodontitis and with no recent periodontal therapy (ie, within 6 months) were documented for this case series. Patient ages ranged between 56 and 68 years. One of the nine patients had type 2 diabetes mellitus, which was medically controlled. Other medical conditions affecting patients included hypertension and hyperlipidemia, also which were stable and medically controlled.
All patients had a complete periodontal probing examination at baseline. To qualify, patients had to present with at least one tooth with probing depth ≥ 6 mm and bleeding on probing at baseline (Day 1). All patients received full-mouth scaling and root planing treatment using a combination of ultrasonic instruments and hand curettes (with or without local anesthesia). Immediately following completion of scaling procedures (ie, one or two visits over 2 weeks maximum), patients applied PerioPatch devices to identified areas of pocketing (> 6 mm) and bleeding (Day 1). All patients reapplied PerioPatch devices later on that first day (approximately 8 hours) and then once daily for the remainder of the week (Days 2 to 7). A subset of three patients additionally applied devices daily for the second week (Days 15 to 21). If any PerioPatch device fell out within 30 minutes of application, patients reapplied a fresh device to the specified oral area. Patients received detailed verbal and written instructions on PerioPatch applications along with oral hygiene instructions prior to dismissal on Day 1.
Among the nine patients, a total of 17 periodontal sites associated with 13 teeth (ie, five molars, five premolars, and three incisors or canines) were treated according to this adjunctive device protocol. Patients returned for a follow-up periodontal examination at 4 to 6 weeks. Patient compliance with PerioPatch application was monitored via the collection of unused devices and patient interviews conducted at the 4-to-6-week examination.
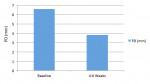
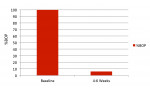
Probing measurements obtained at baseline at the designated treatment sites averaged 6.6 mm in pocket depth (standard deviation [SD] 1.06) with a range between 6 and 10 mm (Figure 2). As per the inclusion criteria, all sites bled on probing (100%) at the baseline examination (Figure 3).
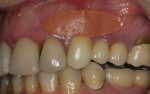
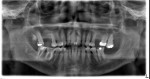
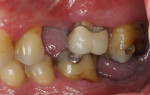
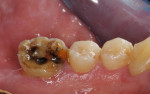
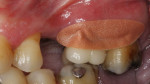
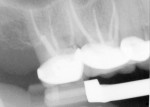
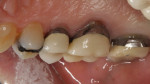
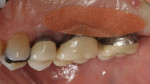
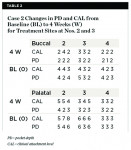
At 4 to 6 weeks, pocket depths at the treatment sites averaged 3.8 mm (SD 0.90) (Figure 2). Indeed, pocket depth reductions from baseline averaged 2.8 mm overall for the treatment sites and ranged from 2 mm to 4 mm. At the 4-to-6-week examination, only one of the 17 treatment sites (6%) bled on probing (Figure 3). Improvements in clinical attachments levels were comparable to the millimeter changes seen in pocket depth (data not shown). Similar pocket depth reductions were observed for the six patients applying PerioPatch devices for 1 week and those applying the devices for 2 weeks total. Meanwhile sites among the nine patients treated with scaling and root planing alone (no adjunctive therapy) responded with probing depth reductions of 1 mm on average (data not shown). Detailed changes in probing parameters exhibited by two of the PerioPatch-treated cases are presented in Table 1 and Table 2. Baseline radiographic and clinical images for the two cases are presented in Figure 4 through Figure 7 (Case 1) and Figure 8 through Figure 10 (Case 2), with the application of the PerioPatch for each case shown in Figure 7 (Case 1) and Figure 10 (Case 2). Counts of returned unused PerioPatch devices, along with patient interviews at the follow-up visit, indicated consistent compliance (> 90%) with the adjunctive protocol as prescribed.
Rationale for Treatment Approach
The rationale for the treatment of this case series with adjunctive PerioPatch devices was to reliably reduce the clinical signs of inflammation and to augment the benefits of conventional mechanical therapy. Human observational studies indicate that reductions in the clinical signs of inflammation, such as pocket depth and bleeding, are strong predictors of periodontal stability in maintenance populations.13,14 In randomized controlled clinical trials, chronic periodontitis patients consistently demonstrate pocket depth and bleeding reductions with scaling and root planing.9-11 The cumulative evidence also demonstrates that adjunctive therapies like antimicrobials and host modulatory agents can improve the effects of mechanical therapy on periodontal probing parameters. For example, Williams et al reported that chronic periodontitis subjects with pocket depth ≥ 6 mm and treated with adjunctive minocycline microspheres exhibited a 1.5-mm pocket depth reduction as compared to 1-mm reduction observed for subjects treated with scaling and root planing alone (over the study interval of 1 to 9 months post-treatment).9 Similarly, periodontitis subjects treated with subgingival chlorhexidine chips exhibited a 1.06-mm pocket depth reduction at 1 month.15 In contrast, the periodontitis patients documented in this case series and treated with scaling and root planing plus PerioPatch devices exhibited pocket depth reductions of 2.8 mm on average at 4 to 6 weeks post-treatment. This case series also indicates consistent reductions in bleeding responses with adjunctive PerioPatch treatment (94% reduction from baseline) versus the values reported for adjunctive minocycline microspheres (26%) and scaling and root planing alone (20%). Hence, within the confines of this case series, the reductions in pocket depth and bleeding observed with the adjunctive PerioPatch use appear to be the result of the local device application and not because of the mechanical therapy alone.
Independent research indicates that the extracts of the three plants included in PerioPatch devices (Sambucus nigra, Centella asiatica, and Echinacea purpurea) have host modulatory properties. Accordingly, monocytes, macrophages, or neutrophils incubated with P. gingivalis or Aggregatibacter actinomycetemcomitans secreted significantly lower pro-inflammatory cytokines such as IL-1 and TNF-α when an extract from Sambucus nigra was added to the media.16 This anti-inflammatory effect of the Sambucus nigra appears to be mediated via the inhibition of nuclear transcription factor activation kappaB (NF-κB) and phosphatidylinositol 3- kinase. Similarly, an ethanol extract of Centella asiatica significantly inhibited mitogenesis of human peripheral blood monocytes and the production of IL-2 and TNF-α.17 Mice treated with the Centella asiatica extracts (100 mg/kg body weight) showed higher antibody responses to bovine serum albumin (BSA) when compared with non-treated controls.17 In addition, mice exposed to radiation and treated with extracts from Echinacea purpurea exhibited less leukopenia and faster recovery of blood cell counts as compared to untreated controls via an observed antioxidant mechanism.18 These collective data indicate that Sambucus nigra, Centella asiatica, and Echinacea purpurea extracts may have direct anti-inflammatory, anti-oxidant, and immune-modulatory activities in host cells involved in wound healing. To the best of the authors’ knowledge, the PerioPatch exerts its effect by absorption of the inflammatory exudate in the periodontal pocket and the gingiva. This reduction in the level of pro-inflammatory mediators allows the body to respond more effectively, fosters tissue repair, and results in a reduction of inflammation and improvement in actual healing.
Grbic and coworkers conducted a proof-of-concept clinical study of the PerioPatch device involving 53 adult subjects with plaque-induced gingivitis.19 The aim of the clinical trial was to determine whether the PerioPatch device applied in a site-specific manner could reduce local inflammation at the targeted area. For inclusion, medically healthy subjects had to exhibit a mean gingival index (GI) score of 1 or greater (maxillary posterior teeth). Following the baseline examination and collection of gingival crevicular fluid, subjects were randomized for either the PerioPatch (active) or a placebo patch (ie, inactive without the plant extracts). Subjects applied three active or placebo patches on the first day and then one patch per day for the following 2 days. Subjects were recalled for clinical examinations and crevicular fluid sampling at Days 2, 4, 8, and 15. Gingival crevicular fluid was analyzed for concentrations of the inflammatory biomarker β-glucuronidase using a chairside enzymatic assay. Results indicated that PerioPatch treatment significantly decreased mean GI scores at Days 4 and 15 as compared to placebo patch treatment. Furthermore, significantly more sites treated with the PerioPatch device responded with a decrease in GI of 1 or greater versus the placebo patch over the 15-day period. Significant intergroup differences were also noted for crevicular fluid levels of β-glucuronidase at Days 4 and 8, with significantly lower concentrations measured for the PerioPatch-treated subjects. The data from this gingivitis clinical trial indicate that site-specific treatment with the PerioPatch is associated with decreases in the clinical signs of inflammation along with decreases in the inflammatory biomarker, β-glucuronidase.
The present case series of periodontitis patients greatly differs from the gingivitis subjects recruited for the trial conducted by Grbic et al in terms of the periodontal diagnosis and extent of inflammation; nevertheless, the present case series further supports the use of the PerioPatch for managing and reducing periodontal and gingival inflammation in patients.
Conclusion
Patients with chronic periodontitis treated with mechanical therapy plus adjunctive PerioPatch devices responded with consistent pocket depth reductions (2.8 mm on average), clinical attachment level gains (2 mm on average), and bleeding resolution at 1 month. Within the confines of this case series, the PerioPatch is a novel but simple device that may be combined with scaling and root planing for the management of chronic periodontitis.
Disclosure
Dr. Paquette serves as a scientific advisor for Izun Pharmaceuticals. Dr. Levine is Chief Executive Officer of Izun Pharmaceuticals.
About the Authors
David W. Paquette, DMD, MPH, DMSc
Associate Dean for Education
Stony Brook University School of Dental Medicine
Stony Brook, New York
William Z. Levine, DDS
CEO and Founder
Izun Pharmaceuticals
New York, New York
Director and Founder
Jerusalem Perio Center
Jerusalem, Israel
REFERENCES
1. Eke PI, Dye BA, Wei L, et al. Prevalence of periodontitis in adults in the United States: 2009 and 2010. J Dent Res. 2012;91(10):914-920.
2. Martin JA, Page RC, Kaye EK, et al. Periodontitis severity plus risk as a tooth loss predictor. J Periodontol. 2009;80(2):202-209.
3. Dietrich T, Sharma P, Walter C, et al. The epidemiological evidence behind the association between periodontitis and incident atherosclerotic cardiovascular disease. J Periodontol. 2013;84(4 suppl):S70-S84.
4. Borgnakke WS, Ylöstalo PV, Taylor GW, Genco RJ. Effect of periodontal disease on diabetes: systematic review of epidemiologic observational evidence. J Periodontol. 2013;84(4 suppl):S135-S152.
5. Socransky SS, Haffajee AD, Cugini MA, et al. Microbial complexes in subgingival plaque. J Clin Periodontol. 1998;25(2):134-144.
6. Offenbacher S. Periodontal diseases: pathogenesis. Ann Periodontol. 1996;1(1):821-878.
7. Offenbacher S, Odle BM, Gray RC, Van Dyke TE. Crevicular fluid prostaglandin E levels as a measure of the periodontal disease status of adult and juvenile periodontitis patients. J Periodontal Res. 1984;19(1):1-13.
8. Stashenko P, Jandinski JJ, Fujiyoshi P, et al. Tissue levels of bone resorptive cytokines in periodontal disease. J Periodontol. 1991;62(8):504-509.
9. Williams RC, Paquette DW, Offenbacher S, et al. Treatment of periodontitis by local administration of minocycline microspheres: a controlled trial. J Periodontol. 2001;72(11):1535-1544.
10. Haffajee AD, Socransky SS, Gunsolley JC. Systemic anti-infective periodontal therapy. A systematic review. Ann Periodontol. 2003;8(1):115-181.
11. Caton JG, Ciancio SG, Blieden TM, et al. Treatment with subantimicrobial dose doxycycline improves the efficacy of scaling and root planing in patients with adult periodontitis. J Periodontol. 2000;71(4):521-532.
12. Hasturk H, Kantarci A, Goguet-Surmenian E, et al. Resolvin E1 regulates inflammation at the cellular and tissue level and restores tissue homeostasis in vivo. J Immunol. 2007;179(10):7021-7029.
13. Lang NP, Adler R, Joss A, Nyman S. Absence of bleeding on probing. An indicator of periodontal stability. J Clin Periodontol. 1990;17(10):714-721.
14. Paulander J, Axelsson P, Lindhe J, Wennström J. Intra-oral pattern of tooth and periodontal bone loss between the age of 50 and 60 years. A longitudinal prospective study. Acta Odontol Scand. 2004;62(4):214-222.
15. Jeffcoat MK, Palcanis KG, Weatherford TW, et al. Use of a biodegradable chlorhexidine chip in the treatment of adult periodontitis: clinical and radiographic findings. J Periodontol. 2000;71(2):256-262.
16. Harokopakis E, Albzreh MH, Haase EM, et al. Inhibition of proinflammatory activities of major periodontal pathogens by aqueous extracts from elder flower (Sambucus nigra). J Periodontol. 2006;77(2):271-279.
17. Punturee K, Wild CP, Kasinrerk W, Vinitketkumnuen U. Immunomodulatory activities of Centella asiatica and Rhinacanthus nasutus extracts. Asian Pac J Cancer Prev. 2005;6(3):396-400.
18. Mishima S, Saito K, Maruyama H, et al. Antioxidant and immuno-enhancing effects of Echinacea purpurea. Biol Pharm Bull. 2004;27(7):1004-1009.
19. Grbic J, Wexler I, Celenti R, et al. A phase II trial of a transmucosal herbal patch for the treatment of gingivitis. J Am Dent Assoc. 2011;142(10):1168-1175.