Transitional Bonding for Segmented Treatment: A Two-Phase Restorative Approach
Abstract:
When extensive dental therapy is needed, as in cases of severe attrition, interim restorations are useful in determining whether or not the proposed treatment will be successful. Transitional resin bonding is one type of interim method. In this case report, a 60-year-old patient presented with severely worn maxillary and mandibular anterior teeth; he desired treatment to be done in a timely fashion so as to be ready to attend an important wedding. Due to the urgency in timing and the complexity of the case, the treatment plan was a two-phase approach that included an initial esthetic and occlusal design to create a diagnostic wax-up followed by placement of transitional composite resin bonding, and then placement of indirect porcelain restorations. This transitional bonding approach allowed comprehensive treatment to be completed at a pace suitable to the patient’s needs.
Severe attrition is a common reason for rehabilitation of an adult dentition.1 The treating dentist is charged with properly diagnosing the cause of the attrition and determining if it is active. The etiology of the attrition—be it occlusal dysfunction, constricted chewing pattern, parafunction, or neurologic disorder— is critical to determining the ultimate restorative plan.2 If the process is active, the prognosis for the final restorations will be more guarded than if the destructive activity is no longer present.
When extensive dental therapy is required, interim restorations are a useful adjunct in determining if the proposed treatment will be successful. Transitional resin bonding is one type of interim method.3 This protocol has the advantage of allowing the practitioner to divide the final treatment into segments that are amenable to both the patient’s scheduling and financial concerns.
Clinical Case Overview
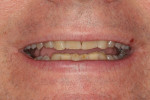
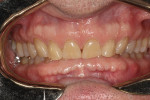
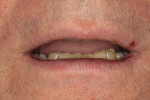
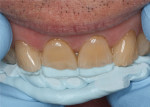
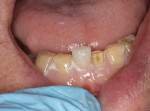
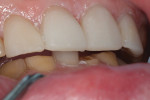
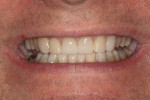
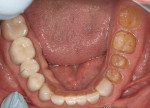
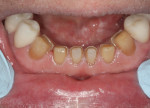
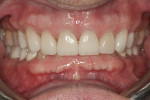
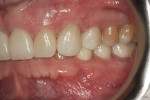
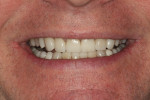
A 60-year-old man, who had been a patient in the practice for more than 20 years, was concerned about his severely worn maxillary and mandibular anterior teeth (Figure 1). The appearance, particularly the mandibular incisors, was a source of embarrassment, and he was extremely self-conscious when smiling (Figure 2). He had regularly inquired about restoring his teeth to their original form at his periodic recare appointments throughout the past 10 years. A full diagnostic work-up was performed in 2004 but he had never proceeded with treatment. At the urging of his family, the patient decided he would finally “fix his teeth” before his daughter’s upcoming wedding in 2 months. Due to the urgency in timing and treatment complexity, the final restorations could not be completed before the ceremony.
The medical history was noncontributory. Because there was some evidence of erosion on the mandibular posterior teeth, he was questioned further about gastroesophageal reflux disease (GERD)4 but denied any history of the problem. A comprehensive examination was completed with full diagnostic records.
Diagnosis, Risk Assessment, and Prognosis
Without proper diagnosis and risk assessment, it is impossible to develop an appropriate treatment plan that decreases the risk for future problems and improves the long-term outlook for success.5 Dentists should avoid being too quick to generate a solution to a patient’s concern. Having a diagnostic and prognostic system in place can help the clinician methodically and rationally choose a proper solution that will increase the likelihood of a successful outcome.
Periodontal: Periodontal probing depths of 2 mm to 3 mm were measured with minimal bleeding.6 The patient exhibited excellent oral hygiene. The gingiva was a thick biotype with no areas of recession, and buccal exostoses were present on both arches.7 Bone levels were consistent with an AAP type I diagnosis.
Risk: Low
Prognosis: Good
Biomechanical: The patient presented with severe attrition, minimal restorations, mild erosion, and chipping on the incisal edges of the maxillary and mandibular anterior teeth. Erosion was present on the posterior teeth of both arches. Cupping of the cusp tips indicated a chemical component to the tooth loss that was more aggressive than the frictional wear.8 There was one small carious lesion on the occlusal of tooth No. 5. Gold restorations were present on teeth Nos. 2 and 30. Successful endodontic treatment was present on tooth No. 30.
Risk: High
Prognosis: Overall poor, but hopeless for tooth No. 5 unless treated
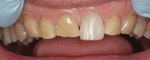
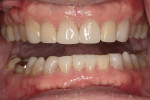
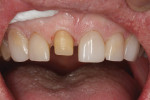
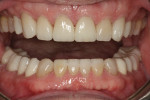
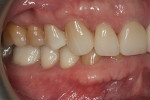
Functional: The patient exhibited a Class I malocclusion with 100% overbite and retroclined maxillary incisors (Figure 3). All teeth were present except for third molars, which were extracted prophylactically as a young adult. All tooth mobility measurements were within normal limits.
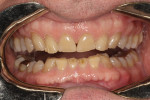
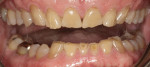
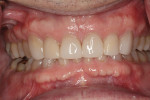
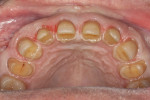
The wear pattern present was consistent with that of a constricted chewing pattern: wear on the lingual surfaces of the maxillary incisors and on the facial surface of the mandibular incisors. The patient indicated that the wear had been present for quite some time but it did not seem to be getting worse. Photographs taken 10 years prior compared to current photographs confirmed that there was little change in the incisal wear over the past 10 years (Figure 4 and Figure 5). The patient could chew comfortably and experienced no joint or masticatory muscle pain at any time. A nightguard had been fabricated 15 years ago following an initial diagnosis of nocturnal bruxism, although the diagnosis was never confirmed and the patient did not wear the appliance because he didn’t feel that he was grinding his teeth. Even though the wear was severe, it did not appear to be active, and upon detailed questioning, the patient denied any symptoms of unacceptable function, leading to a preliminary diagnosis of acceptable function.
A Kois deprogrammer was fabricated and worn by the patient for 3 weeks, and occlusal centric relation (CR) records were secured after confirmation of deprogramming. The models were mounted using a Kois Dento-Facial Analyzer™ (Kois Center, www.koiscenter.com) and a Panadent PCH™ articulator (Panadent, www.panadent.com). Analysis of study casts mounted in CR revealed bilateral contact on the posterior teeth with no anterior or posterior repositioning of the mandible from maximum intercuspal position (MIP). The deprogrammer showed no lateral streaking on the acrylic platform after nighttime wear, which confirmed the absence of parafunction. To confirm the absence of anterior envelope of function violations, the patient was asked to sit up and chew on 200-micron blue articulating paper. No blue marks were present on the lingual surfaces of the maxillary anterior teeth.9
Given the presence of severe attrition, it was important to rule out parafunction as a diagnosis. While one can never be sure of the exact circumstances of observed attrition, it is likely that the original wear in this case was caused by a constricted chewing pattern and the masticatory system adapted during his active phase leading to the current appearance. Given the evidence collected, the diagnosis was acceptable function. A moderate risk for future problems was appropriate given the patient’s past history.
Risk: Moderate
Prognosis: Fair
Dentofacial: The patient exhibited low lip dynamics with minimal tooth display when smiling broadly. In repose (Figure 6), the maxillary cuspids were a negative 2 mm measured from the lip border, indicating a need for additional incisal length.10 The maxillary incisors were short, with serrated edges. A cephalometric analysis revealed a brachyfacial growth pattern with retroclined central incisors and a deep overbite, but no crowding. The gingival architecture was symmetrical with no recession. The mandibular incisors were severely worn and short. Ninety percent of the mandibular teeth were displayed in full smile, but only 1 mm of incisal edge was visible in repose. Given the patient’s age, additional length and display of the mandibular incisors was indicated.
The mandibular posterior occlusal plane exhibited a step down from the cuspids. A gold crown was evident in the mandible on full smile. The maxillary occlusal plane location was acceptable.
Risk: Low
Prognosis: Moderate
Treatment Goals
The treatment goals were to increase the length and visual display of the patient’s maxillary and mandibular incisors in both full smile and repose. Achievement of the patient’s stated goal was not possible at the current MIP or occlusal vertical dimension (OVD). Increasing the length of the anterior teeth necessitated alteration of the occlusal plane of either the mandibular or maxillary arch or a combination of both. The orthopedic position CR was used to establish the jaw position for the new OVD and centric occlusion (CO).2
The patient’s treatment plan was divided into two phases. The impending wedding created an unrealistic deadline to complete the final restorations. However, it can be beneficial to restore complex cases with transitional materials initially to confirm that the clinical and esthetic changes will be well tolerated and approved by the patient before placing the definitive restorations.3 In this case, the initial phase would include transitional composite resin bonding to increase the OVD and establish a stable CO, which would also restore the anterior teeth to an acceptable length and esthetic display. The initial phase would allow the provider to confirm that the new occlusion and the incisal edge position were stable and correct. In addition, the treatment plan could be segmented to accommodate shorter and less complex appointments.
The second phase would include placement of indirect restorations on the teeth altered by the transitional bonding. The final restorations could be placed segmentally by quadrants as time and finances permitted. With the final occlusion and incisal edge position already established in the transitional phase, duplication of the transitionally bonded dentition would be more predictable. Due to the additive nature of the restorations, this treatment plan would meet the goal of reducing the risk of biologic and functional damage to the patient’s masticatory system.11,12
Treatment Plan
The patient accepted this two phase-approach. The treatment plan would proceed with the initial esthetic and occlusal design for the purpose of creating a diagnostic wax-up, then placement of the transitional composite resin bonding, and, finally, placement of indirect porcelain restorations on the transitionally treated teeth.
Treatment Phases
Step 1: Esthetic and Occlusal Determination
Maxillary and mandibular incisal edge positions were determined using a combination of techniques. First, the amount of tooth display when the patient was viewed both with lips in repose and in full smile was compared to age-appropriate norms.13 The most critical measurement was the relative incisal-cervical position of the maxillary cuspid to the border of the lip in repose.10 This finding indicated an addition of 2 mm to the incisal edges. The incisors were retroclined, so the proposed restorations would need to be positioned facially by approximately 2 mm. Smile Now™ instant dental templates (Smile Now, www.yoursmilenow.com) were placed directly on the patient’s teeth at the determined level to help visualize the proposed edge position.14 The mandibular incisal edge position was determined using the same visual norms when viewed in full smile and repose. The patient approved the simulated appearance.
The maxillary and mandibular posterior occlusal plane positions were evaluated for esthetic position in a full smile. It was determined that the maxillary plane was acceptable in its current level. The mandibular posterior plane exhibited a significant step cervically as compared to the anterior teeth. The needed increase in the patient’s OVD to accommodate the new incisor length could be accomplished by raising the level of the occlusal surfaces of the mandibular posterior teeth. Therefore, the maxillary posterior teeth would only require restoration if necessary for biomechanical reasons.
The Kois Adjustable Platform™ for the Panadent articulator was lowered to add 2 mm of length and 2 mm facially to the maxillary incisal edges of the study casts mounted in CR. Teeth Nos. 6 through 11 were waxed to the desired position without the addition of wax to the lingual surface. The mandibular incisors were then waxed to their proposed incisal edge position. Centric occlusion was established by the addition of wax to the mandibular posterior teeth at the OVD created when the anterior teeth were brought into light contact.
Clear stents (Temporary Splint Material .020, www.buffalodental.com) were fabricated from the diagnostic waxing. The stents were filled with temporary resin (Turbotemp™, Danville Materials, www.danvillematerials.com) and placed on the patient’s teeth for esthetic confirmation. The patient again approved the esthetic changes.
Step 2: Transitional Resin Bonding
The goal for this appointment was to place composite resin veneers on the maxillary and mandibular anterior teeth, establishing the new OVD and CO using the Kois deprogrammer.15 This would allow the patient to be able to attend his daughter’s wedding with a new smile and stable occlusion.
A polyvinylsiloxane (PVS) stent (BluBite™, Henry Schein Dental, www.henryschein.com) was fabricated from the diagnostic waxing to aid in establishing the new incisal edge position (Figure 7). Composite resin veneers were individually placed on teeth Nos. 6 through 11 with shade A1 Estelite® microfill composite (Tokuyama Dental, www.tokuyama-us.com) (Figure 8). On the unprepared teeth, a total-etch technique was utilized with 35% phosphoric acid for a 15-second etch followed by a thorough 5-second rinse. A single-bottle light-cured adhesive (Prime & Bond® NT™, DENTSPLY, www.dentsply.com) was agitated on the tooth surface for 10 seconds. The adhesive was blown dry and light-cured for 10 seconds. The composite resin was adapted into the PVS stent to form the new lingual surface and incisal edge position, then light-cured for 40 seconds. A reverse mylar matrix was placed interproximally and wrapped subgingivally to the buccal. The composite resin facial surface was sculpted with a gold composite instrument and a brush coated with Brush & Sculpt™ (Cosmedent, www.cosmedent.com) to form the desired contour, then light-cured for 40 seconds. The restorations were contoured and polished with an ET 9 carbide bur (Brasseler USA, www.brasselerusa.com) followed by a progressive series of mini FlexiDiscs™ polishing disks (Cosmedent) (Figure 9).
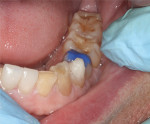
Composite resin was placed on one lower mandibular incisor to the previously determined appropriate size and length using a PVS stent (Figure 10). The Kois deprogrammer was then placed in the patient’s mouth and the platform adjusted until the newly restored lower incisor lightly touched the lingual surface of the maxillary incisor, establishing the new OVD (Figure 11). This technique was used to position the mandible in CR. With the deprogrammer in place, a nanohybrid composite resin, shade A1 (Venus®, Heraeus Kulzer, www.heraeus-kulzer-us.com), was added to the buccal cusp tips of the mandibular bicuspids and occlusal surfaces of the first molars to create the new CO using the previously described bonding protocol (Figure 12). The teeth were restored from front to back and left to right one tooth at a time to reduce inaccuracies from mandibular flexure.16 The composite was placed on each tooth, then the patient closed into CR on the Kois deprogrammer and the restorative material was light-cured. Additional composite was added to the sides of the cusps to achieve a smooth profile. The remaining mandibular incisors were then veneered utilizing the same technique as the maxillary anterior teeth at the new OVD (Figure 13 and Figure 14).
There are other ways to accomplish the same transitional goal. This technique, however, was chosen because it is simple and less costly than laboratory-fabricated composite occlusal onlays for the posterior teeth. Other operators may prefer prefabricated interim restorations.
Step 3: Final Restorations
Four months after the transitional bonding was placed, the patient decided to proceed with the final restorations, as he was happy with the esthetics. There was no evidence of attrition or chipping on the incisal edges of the anterior teeth. The patient reported that he had no temporomandibular muscle pain, the “bite” felt even, and there were no problems chewing. The goal of the final restorations was to duplicate the transitional bonding with a more long-lasting material. Models of the transitional restorations were made and used as a template for the fabrication of both the temporary and final restorations
Segmental restoration by quadrants allowed for easier duplication of the transitional occlusion and anterior esthetics than preparing both arches simultaneously. The sequence of treatment would proceed with the mandibular left posteriors (teeth Nos. 18 through 21), followed by the mandibular right posteriors (teeth Nos. 28 through 31). Restoration of maxillary teeth Nos. 5 through 12 would precede restoration of the mandibular anterior teeth. All maxillary teeth requiring restoration were done at the same time to maintain color consistency. The remaining maxillary posterior teeth were not restored, because the maxillary occlusal plane was acceptable and these teeth were caries-free. The patient requested a 6-month treatment window for his comfort and because of business obligations.
Mandibular Posterior Restorations
Fluorapatite porcelain e.max® (Ivoclar Vivadent, www.ivoclarvivadent.com) veneered zirconia core crowns were used to restore the posterior teeth. Since the OVD was increased by 1 mm to 1.5 mm, the preparation design required minimal occlusal reduction, and only axial reduction consistent with the demands for a zirconia core crown was needed.17 A coarse KS 2 diamond bur (Brasseler USA) was used to prepare the teeth. A double-cord technique was employed for the final full-arch impression.18 A stock tray (Master Tray®, Water Pik, Inc., www.professional.waterpik.com) and PVS impression material (Imprint™ 3, www.3MESPE.com) were used. Since the CO was maintained by the transitionally bonded occlusal surfaces on the unprepared side, the patient closed into a simple wax tab bite (Great Lakes Orthodontics, www.greatlakesortho.com) for the occlusal record without jaw manipulation. A Kois Dento-Facial Analyzer Facebow™ (Panadent) record was used to relate the maxillary cast to the Panadent articulator. The patient approved the Vita™ Shade A1 that was used in the transitional bonding. Interim restorations were fabricated using bis-acrylic temporary resin (Turbotemp) in the clear plastic stent fabricated from the transitional restoration study models.
At the delivery appointment, the interim restorations were removed and the preparations micro-abraded with 27-micron aluminum oxide at 40 psi (PrepStart™, Danville Materials). The restorations were tried-in to evaluate fit and proximal contacts. The occlusion was confirmed one tooth at a time from front to back for the presence of bilateral contact with shimstock and 40-micron articulating paper (Bausch, www.bausch.com). Before cementation, the crowns were rinsed and their zirconia cores cleaned with Ivoclean™ (Ivoclar Vivadent) then treated with Z-Prime Plus™ (Bisco, www.bisco.com) to aid in retention of the cement to the crown’s internal surface.19 After the teeth were thoroughly rinsed, the crowns were cemented with a self-adhesive resin cement (Unicem™, 3M ESPE). The margins were briefly light-cured to facilitate removal of the excess cement. Cement removal was completed with floss, a curette, and a #12 scalpel blade. The occlusion was re-evaluated for bilateral contact. The patient was instructed to simulate chewing on the 200-micron blue articulating paper to assess the buccal and lingual cuspal inclines for any chewing envelope violations.9 Any blue streaks in the envelope of function were relieved and then polished with Brownie FG Mini™ points (Shofu, www.shofu.com).
The mandibular left posterior teeth were restored 1 month later, using the same materials and techniques (Figure 15).
Maxillary Anterior Restorations
The patient was very happy with the appearance of the composite veneers, so the challenge in placing the definitive restorations was to duplicate the size and position of the maxillary incisors. The study casts and facebow record of the transitional restorations recorded the maxillary incisal edge position and shape of the transitional restorations. After placement of soft compound in the anterior area, this same facebow was reseated after preparation of a single central incisor to record the relationship between the prepared tooth and the non-prepared teeth (Figure 16). After completing all preparations, the maxillary working cast could then be placed into the facebow and the relationship of the prepared teeth to the proposed incisal edge position would be accurately represented on the Kois Adjustable Platform.
Fluorapatite porcelain (IPS e.max® Ceram, Ivoclar Vivadent) veneered e.max core restorations were used for the anterior teeth since sufficient enamel was present on the facial surface and at the margins to allow for a bonded protocol. Because the new incisal edge was facially repositioned, the only facial tooth reduction required was for margin definition. Lingual reduction was used for additional retention and resistance form; however, the cingulums were left intact because it has been shown that tooth stiffness is minimally affected when they are not involved in the preparation (Figure 17). KS1 diamonds (Brasseler USA) were used for tooth reduction. A double-cord technique was used for a full-arch PVS impression as described for the posterior permanent restorations. The posterior restorations established the occlusion in CO, so a wax occlusal record was secured without the need for jaw manipulation.
A stent fabricated from the cast of the transitional restorations was used for the provisional restorations, which were fabricated using bis-acrylic temporary resin in shade A-1 (Turbotemp). The provisional restorations were splinted for ease of retrieval and stability.
At the delivery appointment, the interim restorations were removed and the preparations micro-abraded with 27-micron aluminum oxide at 40 psi. Prior to placing the crowns in the mouth for try-in, a silane coupler (Silane Bond Enhancer™, Pulpdent, www.pulpdent.com) was applied to the internal surface of the crowns for 1 minute, then dried.20 The restorations were evaluated for fit and proximal contacts. The occlusion was confirmed one tooth at a time starting with the central incisors using shimstock and 40-micron articulating paper, then moving posteriorly.
A dual-cure resin cement (RelyX™ Ultimate, 3M ESPE) was used for the final cementation. The e.max crowns were cleaned with phosphoric acid then rinsed with water and dried. The gingival sulci were checked for bleeding and packed with retraction cord where necessary. The teeth were etched with 35% phosphoric acid for 15 seconds and rinsed thoroughly. A single-bottle adhesive supplied with the cement (Scotchbond™ Universal Adhesive, 3M ESPE) was applied to the internal surface of the crown and on the tooth. Both surfaces were air-dried and light-cured. The cement was mixed according to manufacturer’s specifications then placed inside the crowns. The restorations were seated with finger pressure, and floss was used interproximally to remove excess cement. The margins were flash-cured for 1 second and gently cleaned with a curette. Both facial and lingual surfaces were light-cured for 20 seconds. Final cement removal was accomplished with a curette, #12 scalpel blade, Enhance® Finishing Cups (DENTSPLY), fine diamonds, and a brownie point.
The patient was instructed to simulate chewing on 200-micron blue articulating paper to identify any chewing envelope violations. Any blue streaks visible on the lingual surfaces of the anterior teeth were relieved and then polished. The posterior teeth were also checked for blue streaks on cuspal inclines.
After 6 months the final quadrant—the mandibular anteriors—was restored. The mandibular incisors had sufficient enamel circumferentially to use a lithium-disilicate bonded restoration (e.max core veneered with e.max Ceram). The facial surfaces were minimally reduced to create a margin, and the lingual surfaces were prepared incisal to the cingulum (Figure 18). The same protocol was used for impressions and provisionalization. Dual-cured resin cement (RelyX Ultimate) was utilized for final cementation. The occlusion was re-evaluated a final time to assure bilateral simultaneous contacts and no blue streaks from the 200-micron articulating paper on the lingual surfaces of the anterior teeth (Figure 19 through Figure 22).
The recare protocol included 6-month prophylaxis, evaluation for signs of erosion, evidence of incisal wear or chipping, and other symptoms of temporomandibular disorder. Since there were no signs or symptoms of bruxing before treatment, an occlusal guard was not warranted.
Conclusion
The correct diagnosis of a patient’s observed dental attrition is paramount to developing an acceptable treatment plan for the restoration of a worn dentition. Transitional bonding is an effective method for evaluating the proposed occlusal and esthetic changes before final restorations are fabricated. An added benefit of transitional bonding is the ability to segment the final treatment. This allows patients to complete comprehensive dental treatment at a pace that suits their scheduling and financial concerns. In this case, the final result was esthetically pleasing and functionally sound (Figure 23).
Acknowledgements
The author wishes to thank laboratory technician Juan Escobar, CDT, of Midwest Dental Arts, Swisher, Iowa, as well as the author’s dental assistants, Ms. Cynthia Clark and Ms. Alissa Longshore, for their contributions. The majority of the concepts in this article are based on the teachings of the Kois Center, Seattle, Washington.
About the Author
Jeffrey C. Grabiel, DDS
Clinical Instructor
Kois Center
Seattle, Washington
Private Practice
Birmingham, Michigan
References
1. Benazzi S, Nguyen HN, Schulz D, et al. The evolutionary paradox of tooth wear: simply destruction or inevitable adaptation? PLoS One. 2013;8(4):e62263.
2. Kois J, Hartrick N. Functional occlusion: science-driven management. Journal of Cosmetic Dentistry. 2007;23(3):54-57.
3. Hulac S. “Training teeth”: transitional resin bonding for diagnostic purpose. Compend Contin Ed Dent. 2013;34(9):686-690.
4. Gregory-Head B, Curtis DA. Erosion caused by gastroesophageal reflux: diagnostic considerations. J Prosthodont. 1997:6(4):278-285.
5. Bakeman EM, Kois J. Maximizing esthetics/minimizing risk: the line of predictable success. Inside Dentistry. 2005;1(1):16-24.
6. Khan S, Cabanilla LL. Periodontal probing depth measurements: a review. Compend Contin Educ Dent. 2009;30(1):12-22.
7. Horning GM, Cohen ME, Neilis TA. Buccal alveolar exostoses: prevalence, characteristics, and evidence for buttressing bone formation. J Periodontal. 2000;71(6):1032-1042.
8. Lussi A, Hellwig E, Ganss C, Jaeggi T. Buonocore Memorial Lecture. Dental erosion. Oper Dent. 2009;34(3):251-262.
9. Nishigawa K, Nakano M, Bando E. Study of jaw movement and masticatory activity during unilateral chewing with and without balancing side molar contacts. J Oral Rehabil. 1997;24(9):691-696.
10. Misch CE. Guidelines for maxillary incisal edge position-a pilot study: the key is the canine. J Prosthodont. 2008;17(2):130-134.
11. Kois JC. New challenges in treatment planning: shifting the paradigm toward risk assessment and perceived value–Part 1. Journal of Cosmetic Dentistry. 2011;26(4):62-69
12. Kois JC. New challenges in treatment planning: incorporating the fundamentals of patient risk assessment–Part 2. Journal of Cosmetic Dentistry. 2011;27(1):110-121.
13. Arnett GW, Gunson MJ. Facial analysis: the key to successful dental treatment planning. Journal of Cosmetic Dentistry. 2005;21(3):20-33.
14. Kois DE, Schmidt KK, Raigrodsji AJ. Esthetic templates for complex restorative cases: rationale and management. J Esthetic Dent. 2008;20(4):239-248.
15. Seay A. Transitional bonding with the Kois deprogrammer: a conservative treatment approach. Compend Contin Educ Dent. 2012;33(10):758-763.
16. Omar R, Wise MD. Mandibular flexure associated with muscle force applied in the retruded axis position. J Oral Rehabil. 1981;8(3):209-221.
17. Chaiyabutr Y, Kois JC. Effect of preparation height on the retention of cemented all-ceramic crown under fatigue load: zirconia crowns. Kois Center Research. 2014
18. Cloyd S, Puri S. Using the double-cord packing technique of tissue retraction for making crown impressions. Dent Today. 1999;18(1)54-59.
19. Dias de Souza GM, Thompson VP, Braga RR. Effect of metal primers on microtensile bond strength between zirconia and resin cements. J Prosthet Dent. 2011;105(5):296-303.
20. Chaiyabutr Y, Kois JC. Evaluation of shear bond strength of resin cements to ceramic conditioned with different ceramic primers. Kois Center Research. 2013.