A Two-Dimensional Gauge and Protocol for Fitting Oral Appliances Used in Treating Sleep Breathing Disorders
Abstract:
The authors tested whether a novel dental gauge that adjusts the mandibular position in both anterior-posterior (A-P) and vertical directions would improve the airway opening. A pilot study of nine patients with sleep breathing disorder used a snoring sound to guide mandibular vertical and protrusion positions with an adjustable mandibular positioning gauge (AMPG). Volumetric airway changes were confirmed by 2-dimensional (2-D) and 3-dimensional (3-D) measurements taken from cone-beam computed tomography (CBCT) scans. Patients experienced a significant average improvement in airway volumetric increase of 50%. The authors concluded that the AMPG device along with employing a snore sound technique as feedback can be used to ensure an improved awake state airway patency and may prove to be a means to optimize fit for oral appliances in treating obstructive sleep apnea.
This pilot study introduces a new procedure and device for identifying proper specifications for fabrication of a dental device in one office visit to enhance airway openings for patients diagnosed with mild-to-severe sleep apnea. The study tests a new dental gauge (Andra Gauge™, Kosmo Technologies, LLC, www.andragauge.com) that enables mandibular adjustments in two planes of movement and a protocol that allows the health practitioner to position the mandible to improve oropharynx patency. For the purposes of the study, the device is referred to as an adjustable mandibular positioning gauge (AMPG). The AMPG allows a two-axis measurement of the mandibular position for a more precise titration than conventional single-axis devices. In addition, the AMPG permits the practitioner to hold the setting on the device constant to assess patient comfort prior to implementing an appliance specification for oral appliance therapy (OAT).
Over the past two decades, OAT has received wider recognition as an alternative to positive airway pressure (PAP) devices to treat mild-to-moderate obstructive sleep apnea (OSA).1-7 Oral appliances (OA) require no electrical power and are cost-effective, quiet, and portable. OAT can be used as a first-line treatment, or after patient refusal or intolerance of PAP therapies, or in combination with PAP. Studies show PAP compliance is problematic, with from 29% to 83% using their devices less than 4 hours per night.8 Many patients prefer OAT over PAP.6,9,10 Side effects of OAT are low if fitted correctly but can include excessive salivation as well as mouth and/or teeth discomfort.6,11 Adherence rates for OAT are at least equal to PAP when the OA is fitted properly.6,12
Barriers to effective use of OAT by practitioners are twofold. First, practitioners receive no feedback regarding airway patency during mandibular titration to ensure good fit. Second, there is no means to adjust oral appliances for both anterior-posterior (A-P) and vertical positions. Both problems can lead to poor oral appliance fit and potential jaw disorders. This can often translate into repeated visits by the patient to a provider for adjustments or discontinuation of therapy. This trial-and-error procedure becomes time-consuming, costly, and potentially discouraging to the patient. The protocol and device tested by the authors address both of these issues.
The authors tested a protocol that uses auditory feedback from the upper airway and a gauge that enables practitioners to adjust both A-P and vertical axes via a continuous glide. The AMPG device was designed to achieve a finely tuned OA fit in both A-P and vertical positioning. Testing protocol required use of the AMPG with the patients in the supine position and used cone-beam computed tomography (CBCT) measures pre- and post-fitting with patients in a seated position to verify improvement in airway openings.
Materials/Methods/Design
An informed consent form was signed by all participants in the study. The nine OSA patient volunteers (4 male, 5 female) from a sleep apnea clinic included eight who either refused PAP therapy or were found noncompliant after attempting PAP therapy and one who was currently compliant with PAP therapy. Patients were included if they were 18 or older, with OSA diagnoses, not pregnant, and willing to try OAT. Patient demographic data and pretest measures were collected (Table 1). OSA was diagnosed based upon a preliminary overnight polysomnography (PSG) study. The PSG studies were performed using American Academy of Sleep Medicine standards, and results were interpreted by a board-certified sleep physician.
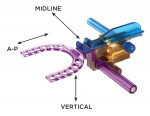
All patients were titrated using the AMPG (Figure 1) by a dentist trained and experienced in sleep dentistry. The device is designed to engage the upper and lower incisors in polycarbonate cradles. Edge-to-edge occlusion for A-P movement is defined as the zero position. Because of the incisor cradle thicknesses, the closed vertical position of the AMPG represents a 2 mm vertical opening as the minimum vertical position.
The AMPG is designed to allow for 7 mm anterior to 5 mm posterior adjustments and from 2 mm to 9 mm vertical adjustments. It can be adjusted via the patient’s mandibular movement or driven by the dentist via a rack and pinion gear set for each A-P and vertical axis. Each axis can be locked once a preferred position has been achieved. The AMPG device used in this study also has a +/- 3 mm sagittal movement option that was not implemented as part of the study. The gauge is polycarbonate allowing it to be used in conjunction with radiological instruments.
The testing protocol is referred to as the “step back technique” (SBT). The SBT protocol consisted of the following steps:
The patient was seated in a dental chair in a supine position, and the AMPG was placed in the patient’s mouth.
The patient was asked to make a snoring sound emanating from the throat and with the tongue placed behind his or her lower front incisors.
With the AMPG unlocked, the patient was asked to protrude the jaw as far forward as possible.
The practitioner then stepped the protrusion back 1 mm to 2 mm per step, following with alternating 1 mm to 2 mm adjustments to the vertical opening.
A-P and vertical adjustments were made in a stair-step fashion until the patient could no longer snore, the snore sound was significantly reduced, and/or the practitioner could hear that the airway had non-labored breathing that accompanies an increase in airway opening.
To assure patient comfort, a 1 to 10 discomfort scale was used throughout each procedure, with 10 indicating high discomfort; all patients experienced a comfort level of 1 during the procedure. After positioning, the patient relaxed for 10 minutes with the locked AMPG in the mouth to assure the determined position was comfortable; none of the tested patients requested adjustment after the 10-minute period.
After SBT fitting, the patient then had two cone-beam scans performed—one in the pre-fitting habitual position and the other while in the final position determined by the SBT using the locked AMPG. The CT scans were performed using a 360-degree CBCT portable scanner (Kodak Model 9500 Cone Beam CT, Carestream Dental, www.carestream.com) while in a seated position. (Authors’ note: In all cases, lowest possible dosage was used by the CBCT technician. The maximum dose of the Kodak 9500 CBCT for the study procedure was 93 microsieverts.)
The first scan was taken with the patient relaxed, breathing through the nose, with the tongue placed behind the front incisors. The second scan was taken with the AMPG—still locked in its final position—placed back in the patient’s mouth, with the patient breathing through the nose and with the tongue placed behind the front incisors. The patients’ CBCT scans were measured using Invivo5 software (Anatomage Dental, https://dental.anatomage.com). The measurements were taken at the same slices for the pre- and post-treatment scans. To provide a sense of procedural time, from start to finish, each cone-beam procedure required about 20 to 25 minutes from setup to completion. The titration of each patient’s mandible took less than 20 minutes. Outcome measures included pre- and post-fitting airway data, temporomandibular joint (TMJ) position, and tongue position. The airway measurements were taken from the CBCT scans at the narrowest portion of the oropharynx. A-P measurements were defined from the patient’s habitual bite position.
Results
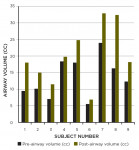
All patients showed an increase in oropharynx volume after using the step back technique. Baseline airway volumes averaged 13.51 cubic centimeters (SD = 6.08). After the mandibular position adjustment using the SBT protocol with the AMPG, airway volumes increased to 19.97 cubic centimeters (SD = 8.81), a 50% increase. This increase was significant, based on a paired sample t-test, t (8) = -4.27, p = 0.003. Pearson correlations showed that vertical and A-P adjustments were unrelated, at r = -0.20, n.s. (n.s. = non-significant). Neither the A-P (r = 0.19, n.s.) nor the vertical (r = 0.15, n.s.) adjustment alone related to significant airway change.
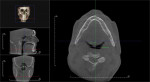
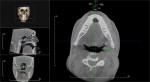
Table 2 summarizes the results of each patient’s adjusted mandibular position along with the pre- and post-test airway volume. Figure 2 and Figure 3 show pre- and post-test CBCT scans of patient No. 5, and Figure 4 shows each patient’s A-P and vertical setting with resulting area airway opening and volumetric increases.
Discussion
This pilot study provided encouraging results. With the simple use of a throaty snoring sound as an immediate feedback mechanism to assist in positioning an OA, the authors’ sleep and dental team could quickly identify an airway opening that represented significant improvement. This was confirmed by before and after CBCT scans of each patient’s airway.
Pre- and post-test results indicate at least three conclusions. First, each person’s mandibular adjustment needs are unique and require an individual approach to adjusting their mandible for oropharynx patency. As shown in Table 2, A-P final measurements varied from -3.5 mm to +4 mm and vertical measurements varied from 6 mm to 8.5 mm. The adjustment to the A-P does not appear to covary with adjustment to the vertical (r = -0.20, n.s.). As shown in Table 2, some airways opened with the most adjustment to A-P, some required most adjustment to vertical, and some required both. The absence of a correlation between adjustment size and change in cross-sectional airway was also found by Gale et al.13 If confirmed with a larger sample size, this indicates that personal adjustment for airway openings needs to be accomplished without any a priori set of adjustments as the goal.
Second, in this study, adjusting the mandible in the vertical plane was important in achieving airway improvement for most patients. Past research and practice has yielded a variety of recommendations regarding vertical adjustment as opposed to only A-P adjustments. Some have only manipulated the A-P13,14 while others have manipulated both.15,16 Based on research findings, some recommend manipulating only the A-P16,17; others recommend manipulating both A-P and vertical.18 In the current study, some patients needed minimal vertical adjustment and others needed both vertical and A-P. Thus, the authors recommend considering both dimensions when fitting appliances.
Third, the authors found that the AMPG provided a comfortable and finely adjustable device for taking measurements for the oral appliances. Mandibles move in at least three dimensions, but past and current practices of fitting an OA have often relied on adjustments in only one dimension. Dental professionals have a need for rapid and effective measurements to determine proper appliance specifications; the AMPG used in the current study was effective. Test results suggest that successful titrations can be managed effectively during a single office visit.
Use of a snoring sound to assist with determining airway opening is a subjective technique, but one that has been used effectively in past research.19,20 Esaki used this feedback method in A-P fitting for setting OAs while titrating in small intervals. A future airway feedback technique that can instantaneously provide a nonsubjective metric would enhance the feedback protocol. Furthermore, the biomechanics of OAT are still not well known.21,22
Conclusions
When fitting an OAT to treat OSA it is desirable to have an immediate feedback of the resulting airway changes to determine reduced pressure and obstruction. Utilizing snore sound as feedback with an AMPG is a subjective methodology that provides a guide in not only finding the optimal setting for reduced airway resistance but it also allows the practitioner to work with the patient for comfort.
Disclosure
Messrs. Hanewinkel, Andra, and Gleeson are stock shareholders with Kosmo Technologies, LLC.
About the Authors
Michael Van Leeuwen, DMD
Private Practice, Van Leeuwen Dentistry, Salt Lake City, Utah; Board of Advisors, Kosmo Technologies, LLC, Salt Lake City, Utah
Rodolfo Martinez-Ferrate, MD
Board Certified Sleep Physician, practicing medicine in South Jordan, Utah; Founding Partner, Kosmo Technologies, LLC, Salt Lake City, Utah
Derek Preble
President, C Inside LLC, Salt Lake City, Utah
William Hanewinkel, BSME
President, Kosmo Technologies, LLC, Salt Lake City, Utah
Michael Gleeson
Founding Partner, Kosmo Technologies, LLC, Salt Lake City, UT
Jeremy Andra
Founding Partner, Kosmo Technologies, LLC, Salt Lake City, UT
References
1. Holley AB, Lettieri CJ, Shah AA. Efficacy of an adjustable oral appliance and comparison with continuous positive airway pressure for the treatment of obstructive sleep apnea syndrome. Chest. 2011;140(6):1511-1516.
2. Dieltjens M, Vanderveken OM, Heyning PH, Braem MJ. Current opinions and clinical practice in the titration of oral appliances in the treatment of sleep-disordered breathing. Sleep Med Rev. 2012;16(2):177-185.
3. Aarab G, Lobbezoo F, Hamburger HL, Naeije M. Oral appliance therapy versus nasal continuous positive airway pressure in obstructive sleep apnea: A randomized, placebo-controlled trial. Respiration. 2011;81(5):411-419.
4. Chan AS, Lee RW, Cistulli PA. Dental appliance treatment for obstructive sleep apnea. Chest. 2007;132(2):693-699.
5. Aarab G, Lobbezoo F, Heymans MW, et al. Long-term follow-up of a randomized controlled trial of oral appliance therapy in obstructive sleep apnea. Respiration. 2011;82(2):162-168.
6. Hoffstein V. Review of oral appliances for treatment of sleep-disordered breathing. Sleep Breath. 2007;11(1):1-22.
7. Lim J, Lasserson TJ, Fleetham J, Wright J. Oral appliances for obstructive sleep apnoea. Cochrane Database Syst Rev. 2006;(1):CD004435.
8. Weaver TE, Grunstein RR. Adherence to continuous positive airway pressure therapy: the challenge to effective treatment. Proc Am Thorac Soc. 2008;5(2):173-178.
9. Ferguson KA. The role of oral appliance therapy in the treatment of obstructive sleep apnea. Clin Chest Med. 2003;24(2):355-364.
10. Ferguson KA, Cartwright R, Rogers R, Schmidt-Nowara W. Oral appliances for snoring and obstructive sleep apnea: a review. Sleep. 2006;29(2):244-262.
11. Cistulli PA, Gotsopoulos H, Marklund M, Lowe AA. Treatment of snoring and obstructive sleep apnea with mandibular repositioning appliances. Sleep Med Rev. 2004;8(6):443-457.
12. Vanderveken OM, Dieltjens M, Wouters K, et al. Objective measurement of compliance during oral appliance therapy for sleep-disordered breathing. Thorax. 2013;68(1):91-96.
13. Gale DJ, Sawyer RH, Woodcock A, et al. Do oral appliances enlarge the airway in patients with obstructive sleep apnoea? A prospective computerized tomographic study. Eur J Orthod. 2000;22(2):159-168.
14. Zhao M, Barber T, Cistulli P, et al. Computational fluid dynamics for the assessment of upper airway response to oral appliance treatment in obstructive sleep apnea. J Biomech. 2013;46(1):142-150.
15. Pitsis AJ, Ali Darendeliler MA, Gotsopoulos H, et al. Effect of vertical dimension on efficacy of oral appliance therapy in obstructive sleep apnea. Am J Respir Crit Care Med. 2002;166(6):860-864.
16. Gao X, Otsuka R, Ono T, et al. Effect of titrated mandibular advancement and jaw opening on the upper airway in nonapneic men: A magnetic resonance imaging and cephalometric study. Am J of Orthod Dentofacial Orthop. 2004;125(2):191-199.
17. Vroegop AV, Vanderveken OM, Van de Heyning PH, Braem MJ. Effects of vertical opening on pharyngeal dimensions in patients with obstructive sleep apnoea. Sleep Med. 2012;13(3):314-316.
18. Raphaelson MA, Alpher EJ, Bakker KW, Perlstrom JR. Oral appliance therapy for obstructive sleep apnea syndrome: progressive mandibular advancement during polysomnography. Cranio. 1998;16(1):44-50.
19. Esaki K, Kanegae H, Uchida T, et al. Treatment of sleep apnea with a new separated type of dental appliance (mandibular advancing positioner). Kurume Med J. 1997;44(4):315-319.
20. Wilson K, Stoohs RA, Mulrooney TF, et al. The snoring spectrum acoustic assessment of snoring sound intensity in 1,139 individuals undergoing polysomnography. Chest. 1999;115(3):762-770.
21. Kyung SH, Park YC, Pae EK. Obstructive sleep apnea patients with the oral appliance experience pharyngeal size and shape changes in three dimensions. Angle Orthod. 2005;75(1):15-22.
22. George PT. Selecting sleep-disordered-breathing appliances: Biomechanical considerations. J Am Dent Assoc. 2001;132(3):339-347.
Related Content
Incorporating Dental Sleep Medicine into a Practice: Avoiding the “7 Deadly Sins”