Predictably Replacing Maxillary Incisors with Implants Using 3-D Planning and Guided Implant Surgery
Abstract:
Replacement of multiple adjacent teeth in the esthetic zone with dental implants is a surgical and restorative challenge, especially when an esthetic outcome is essential. Sound diagnosis and treatment planning can be combined with use of cone-beam computed tomography (CBCT) and 3-dimensional (3-D) software to achieve desired results. Placement of implants using guided surgical templates is critical when there is limited space between adjacent teeth or limited bone volume. Slight deviations in implant positioning during placement can lead to implants being too close to adjacent teeth, resulting in bone loss, recession, and encroachment upon adjacent papillae. Placement of implants in anatomically deficient or compromised areas is difficult when using a freehand drill protocol, because attaining the necessary precision cannot be achieved routinely. Esthetically demanding patients require precise implant placement. Use of guided surgical planning and implant placement enables the surgeon to take maximum advantage of available bone in anatomically restricted areas. Restoratively, ideal implant placement facilitates rehabilitation; therefore, all parameters must be observed in order to achieve an esthetically pleasing final restoration.
The principles of guided implant surgery using software to virtually plan implants based on a CT scan and merged final prosthetic outline have undergone constant refinement since they were presented more than two decades ago.1-3 Virtual planning allows clinicians to select the area that is best suited for implant placement—especially in areas of needed support—and to use approaches that enable implant placement in strategically selected sites so that bone grafting can be avoided. The initial guided protocol involved scanning the patient using an inserted scanning template, and the scan was done extraorally as well (ie, double-scan technique). This technique, which is still used for totally edentulous patients, is relatively cumbersome and time-consuming and requires fabrication of a radiographic template and an additional scan.
A recently introduced protocol for partially edentulous patients (NobelClinician® with SmartFusion, Nobel Biocare, www.nobelbiocare.com), however, allows for a much more streamlined digital workflow. Additional information, such as local anatomy and planned final restorations, can be added to the existing preliminary scan anytime during the planning process. This information is merged with the radiographic dataset obtained from a CBCT scan using proprietary algorithms. This information orients and combines the 3D datasets and is based on the CT scan with crowns (natural or prosthetic) in the CT scan. The information is merged with the model using an optical scanner (NobelProcera® 2G, Nobel Biocare). The two datasets are automatically merged, allowing clinicians to view the radiographic data from the scan in the same view with the digitized surface of the patient’s model and the diagnostic wax-up. This allows implants to be optimally placed with regard to available bone and desired final prosthetics. The adjacent soft tissues are also visible. Once the implant positions have been determined, a surgical template can be ordered from a centralized production facility and used either for fully guided surgery or as a 2-mm starter drill template. These templates are extremely precise and accurately fit the model and patient’s teeth. They are based on a high-resolution optical surface scan, and thus have a detailed surface topography. This new workflow is faster, easier, and highly accurate and allows for alterations of the existing plan, such as removing teeth on the cast before they are actually extracted.
Case Report
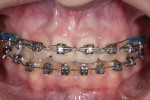
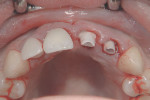
A 20-year-old female patient presented with a request for dental implant treatment subsequent to orthodontic therapy. Clinical examination revealed orthodontic brackets and wires extending across the maxillary arch (Figure 1). All teeth were present. Gingival tissues were healthy, and hard- and soft-tissue morphology was within normal limits. Probing depths ranged from 3 mm to 6 mm. The deepest probings were related to the maxillary anterior teeth. The maxillary anterior teeth had plus-3 mobility. Her smile line was moderately high, with display of the gingival soft tissues surrounding the teeth.
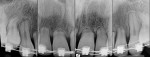
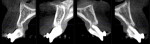
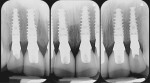
Periapical and CBCT radiographic evaluation (Figure 2 and Figure 3) demonstrated loss of most of the root structure of the maxillary incisors, with normal root anatomy distal to the incisors. Pertinent dental history included multiple orthodontic treatments to correct arch form and crowding. Oral hygiene was excellent, and no other pertinent medical or dental history was presented.
Diagnosis
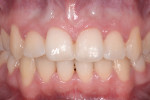
The orthodontic brackets and wires were removed, and the mobile incisors were splinted with interproximal splinting material (Figure 4). A facebow registration was used to mount casts on an adjustable articulator. Due to severe root resorption, the four maxillary incisors were given a hopeless prognosis. All other teeth and supporting structures were within normal limits.
Treatment Planning
The treatment plan was to replace the maxillary incisors with a fixed implant-supported partial denture. Other considerations were to make a six-unit fixed partial denture or a removable partial denture. The patient declined both of these options and was interested in replacing the four anterior teeth with an implant-supported restoration.
In terms of esthetics, placing multiple implants in the esthetic zone is challenging. This is due to lack of adequate bone and soft tissue.4-8 Esthetically predictable treatment options include placing two implants in the lateral incisor positions, with two ovate pontics replacing the maxillary central incisors, or placing two implants in the central incisor areas with a distal cantilevering the lateral incisors.
For this patient, bone morphology in the area of interest was essentially intact with continuous scalloping of the osseous crest, along with adequate bone height and width to receive implants in the subnasal area. Additionally, soft-tissue morphology was harmonious. Philosophically, this was a “maintenance” case, where existing hard- and soft-tissue structures had been essentially maintained. These types of cases lend themselves to a “maintenance” surgical approach, which includes immediate implant placement after extraction, flapless surgery, and immediate provisionalization to maintain soft-tissue architecture. This scenario is in contrast to situations in which existing 3-D hard- and soft-tissue morphology has been lost and needs to be recreated; for such patients, a more traditional approach, including hard- and soft-tissue grafting, is indicated.
During the consultation and explanation of findings, the patient chose the treatment plan utilizing four adjacent implants in the maxillary anterior sextant. The implants were to be placed at the time of extraction, with immediate provisionalization; she would subsequently be restored with single-crown restorations.
Effective Treatment Flow
From Digital Planning to Implant Insertion
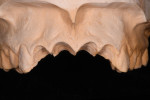
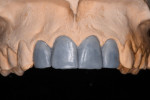
The cast was prepared for scanning by removing the teeth planned for extraction (Figure 5), and a diagnostic wax-up was performed (Figure 6). Using a conoscopic optical scanner (NobelProcera® 2G), both the altered master cast and the diagnostic wax-up were captured and exported as a .nxa file (proprietary NobelProcera surface scan format). Then the previously obtained DICOM files (Digital Imaging and Communications in Medicine) from the CBCT were imported into a virtual diagnostic treatment planning and patient communication program (NobelClinician). Using an automated functionality within the software (SmartFusion), the radiographic data from the DICOM files was automatically and precisely aligned with the clinical data obtained by scanning the master cast along with the diagnostic wax-up (.nxa file) (Figure 7). The patient’s anatomic structures were presented within the same image as the outline of the diagnostic wax-up (Figure 8), forming the basis for planning the ideal implant location.
Using this streamlined approach, the CBCT can be obtained during the initial consultation, and intraoral structures and diagnostic wax-up can be added later, making for an effective workflow. The dental technician can be integrated into the treatment team early on and can preplan the final prosthetic solution prior to any surgical interventions.
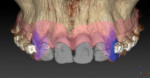
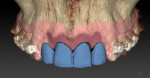
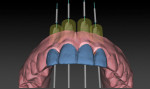
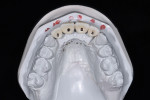
Implants were planned relative to the final tooth position (Figure 9), taking into account the mesio-distal spacing (interproximal embrasure), coronal-apical depth, and bucco-lingual inclination (trajectory is dependent upon the trajectory of bone and whether the implant is screw- or cement-retained). The fourth dimension, the rotational control of the anti-rotational component of the implant–abutment interface, would be addressed at a later time.
The specific implant was selected based on implant design features considered to be important, such as platform switch, tapered design for immediate extraction sockets, and the need to achieve adequate primary stability for immediate provisional restorations.9 NobelActive® implants (Nobel Biocare) were selected, with a narrow platform (3.5 mm) for the lateral incisors and a regular platform (4.3 mm) for the central incisors. The rationale for choosing these implants was based on their back taper design for maximization of bone volume at the ridge crest and potential to achieve high primary stability after placement.
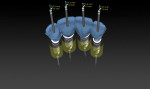
Using these guidelines, the implants were placed precisely within the virtual environment and in relationship to the future free gingival margin position. The implants were aligned for screw access on the lingual of the planned restoration, and for adequate inter-implant spacing of at least 3 mm (Figure 10 through Figure 12). The precision of this method is likely greater than that which is obtainable using freehand implant surgery.
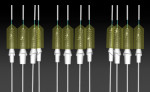
Upon planning the implants, a surgical template (fully guided or 2-mm drill only) can be easily created. The order was sent to a centralized production facility, where a stereolithographic surgical template was made. This template was used to position the analogues within the master cast. Subsequently, the abutments selected during the planning process were placed, and the dental technician created temporary single restorations (Figure 13).
Implant Insertion and Immediate Provisionalization
The goal of implant surgery is the precise delivery of the implants at the exact preplanned position, with adequate primary stability. After administering local anesthesia by infiltration in buccal and palatal sites, sulcular incisions were made around the teeth. The teeth were atraumatically removed. Soft-tissue remnants within the extraction sockets were removed using hand- and rotary instrumentation.
The surgical template was seated, and precision fit was evaluated. This was accomplished by ensuring contact of supporting teeth with the surgical template and by observing the template through the cutouts in the template. The planned anchor pin was inserted between the two central incisor implant positions, ensuring a stable template throughout the procedure.
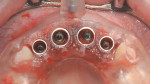
Using the drilling protocol for the chosen implant and altering it according to bone quality,10 the maxillary lateral incisors were inserted first, as they were adjacent to natural teeth that supported the template. Once the two lateral implants were seated, the central incisor sites were prepared and implants were inserted (Figure 14). Care was taken to prepare the osteotomy in relationship to the bone density in order to be able to deliver the implant at the exact coronal-apical depth with adequate primary stability.11
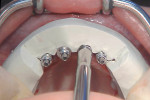
Once all implants were seated, the mounts, anchor pin, and template were removed (Figure 15). In order to be able to deliver abutments and single crowns, the rotation of the internal hex of the implant must be the same as the rotational alignment on the master cast. To achieve this, a hard putty index was created in the laboratory prior to surgery, capturing the hexagon of the insertion assemblies, thus their rotation. The index is used during surgery to align the implant hex at assembly insertion intraorally (Figure 16).
The implants were delivered in the exact preplanned positions and aligned for rotation to coincide with the master cast. Next, the zirconia abutments were seated and tightened to manufacturer’s recommended torque (32 Ncm), and temporary single crowns were tried in (Figure 17). In order to minimize force on the temporary crowns, they were splinted with flowable composite (Figure 18). The temporary restorations were adjusted to eliminate loading in centric occlusion.
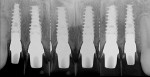
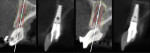
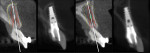
Postoperative periapical radiographs showed precise implant placement (Figure 19). Comparing the planning cross-section with the postoperative CBCT cross-sections of each individual implant also showed the precision of delivery (Figure 20 and Figure 21).
Final Restoration
There are two ways implants can be restored: screw- or cement-retained. When using the cement-retained approach, the original abutments can be used, thus employing the one-abutment, one-time approach.12 In order to avoid packing cord around the abutments, impressions of the individual abutments are taken in the laboratory prior to the intraoral delivery. During healing, transfer copings are fabricated; they are seated on the abutments at the time of final impression, thus avoiding packing of cord. A pick-up impression is performed, and the previously fabricated dies are seated in the impression prior to master cast fabrication. Utilizing this method, precise dies are available for the technician without tissue trauma from packing cords.
Alternatively, screw-retained restorations can be fabricated by removing the temporary restorations, including the abutments, and taking a fixture-level impression. The clinician must decide whether to leave the abutment in place, or whether the benefits of screw-retained restorations might outweigh the risk of epithelialization of the sulcus due to frequent component removal.13,14
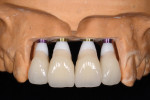
For this patient, fixture-level impressions were taken, and screw-retained restorations were fabricated (Figure 22). The soft tissues adapted to the new architecture, and soft-tissue architecture and health were maintained throughout treatment. The central papilla was entirely maintained, while the papilla between the central and lateral incisors had a slight decrease in height. On the 2-year post-insertion radiograph (Figure 23), the interproximal bone height above the platform of the implants was not fully maintained. The cause for this slight change is unknown. In the future, new technologies may prevent tissue migration adjacent to abutments coronal to the platform.
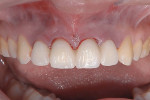
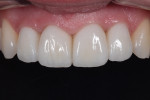
Overall, the patient was very pleased with the treatment approach and results (Figure 24). During treatment the patient always had non-removable, esthetically pleasing teeth, and the outcome exceeded her expectations.
Conclusion
Replacing multiple teeth with dental implants in the esthetic zone is a clinical challenge. Diagnostic skills are imperative to achieving success. Treatment options include fixed partial dentures with implants not placed next to each other, or a single-tooth replacement strategy resulting in multiple implants placed next to each other. A comprehensive diagnostic work-up assessing hard- and soft-tissue conditions (type, level, volume, defect) as well as the establishment of the final restorative result is crucial. Achieving the desired result is only possible if all biological factors that affect treatment outcome are given adequate consideration.
The delivery of multiple implants in the esthetic zone requires a high degree of precision, as the space in the esthetic zone is very limited. Inter-implant as well as tooth-to-implant minimum distances are well established and need to be followed. This leaves little room for surgical error. Three-dimensional planning is the most predictable way to deliver implants when precision is required. Adherence to established biologic and restorative principles is needed for successful virtual planning and is a precondition for success. Using an integrated treatment flow for partially edentulous patients allows clinicians to obtain a CBCT scan at the onset of treatment, and subsequent addition of intraoral information such as diagnostic casts and final prosthetic outcome can be added at any time later, with automatic high-precision alignment. Once the implants have been carefully planned, the clinician can order a surgical template that delivers the implant precisely to the predetermined location.
Disclosure
The author is a consultant to Nobel Biocare, Zürich, Switzerland. He has no financial interest in any of the products mentioned in this article.
References
1. van Steenberghe D, Glauser R, Blombäck U, et al. A computed tomographic scan-derived customized surgical template and fixed prosthesis for flapless surgery and immediate loading of implants in fully edentulous maxillae: a prospective multicenter study. Clin Implant Dent Relat Res. 2005;7(1 suppl):S111-S120.
2. Verstreken K, Van Cleynenbreugel J, Marchal G, et al. Computer-assisted planning of oral implant surgery: a three-dimensional approach. Int J Oral Maxillofac Implants. 1996;11(6):806-10.
3. Jacobs R, Adriansens A, Naert I, et al. Predictability of reformatted computed tomography for pre-operative planning of endosseous implants. Dentomaxillofac Radiol. 1999;28(1):37-41.
4. Tarnow DP, Cho SC, Wallace SS. The effect of inter-implant distance on the height of inter-implant bone crest. J Periodontol. 2000;71(4):546-9.
5. Wöhrle PS. Single-tooth replacement in the aesthetic zone with immediate provisionalization: fourteen consecutive case reports. Pract Periodontics Aesthet Dent. 1998;10(9):1107-1114.
6. Kois JC. Predictable single-tooth peri-implant esthetics: five diagnostic keys. Compend Contin Educ Dent. 2004;25(11):895-900.
7. Chu SJ, Tarnow DP. Managing esthetic challenges with anterior implants. Part 1: midfacial recession defects from etiology to resolution. Compend Contin Educ Dent. 2013;34(spec no 7):26-31.
8. Novaes AB Jr., Barros RR, Muglia VA, Borges GJ. Influence of interimplant distances and placement depth on papilla formation and crestal resorption: a clinical and radiographic study in dogs. J Oral Implantol. 2009;35(1):18-27.
9. Irinakis T, Wiebe C. Clinical evaluation of the NobelActive implant system: a case series of 107 consecutively placed implants
and a review of the implant features. J Oral Implantol. 2009;35(6):283-288.
10. Bahat O. Treatment planning and placement of implants in the posterior maxillae: report of 732 consecutive Nobelpharma implants. Int J Oral Maxillofac Implants. 1993;8(2):151-161.
11. Patzelt SB, Bahat O, Reynolds MA, Strub JR. The All-on-Four Treatment Concept: A Systematic Review. Clin Implant Dent Relat Res. 2013 Apr 5. doi:10.1111/cid.12068.
12. Abrahamsson I, Berglundh T, Lindhe J. The mucosal barrier following abutment dis/reconnection. An experimental study in dogs. J Clin Periodontol. 1997;24(8):568-572.
13. Wadhwani C, Pineyro A, Hess T, et al. Effect of implant abutment modification on the extrusion of excess cement at the crown-abutment margin for cement-retained implant restorations. Int J Oral Maxillofac Implants. 2011;26(6):1241-1246.
14. Assenza B, Tripodi D, Scarano A, et al. Bacterial leakage in implants with different implant-abutment connections: an in vitro study. J Periodontol. 2012;83(4):491-497.
About the Author
Peter S. Wöhrle, DMD, MMedSc, CDT
Private Practice limited to Implant Dentistry and Prosthodontics
Newport Beach, California