A Retrospective Analysis of 12 Immediate-Implant Restorations in the Maxillary Premolar Region
Abstract
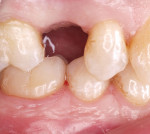
BACKGROUND: A retrospective analysis was performed of 12 consecutive patients who received implant placement with concurrent restorations in the maxillary premolar region as part of the General Practice Residency Program. The emergence profile established during the healing phase was then captured using a customized impression coping prior to fabrication of the final restoration. The patients were followed for a period of at least 1 year.
RESULTS: All 12 cases showed normal healing and resulted in functional implant crowns. Two cases required an additional appointment for re-tightening of the temporary abutment screw.
CONCLUSION: With a favorable occlusal scheme, immediate implant restorations in the maxillary premolar region can be considered when primary implant stability is achieved at the time of placement.
The ultimate goal of dental implant surgery is to provide the patient with a tooth or teeth capable of function from both a masticatory and esthetic aspect. Traditionally, it required patients to first undergo surgical procedures aimed at placement of the implants in the optimal anatomical locations, followed by 4 to 6 months of healing in order to ensure osseointegration. Once osseointegration was confirmed, the restorative clinician would then proceed with providing the patient with a prosthetic replacement.
Over the past decade, significant research has been devoted to reducing the length of time required between the point of initial surgical intervention and placement of the final functioning restoration. Advances in biomechanical technology relative to implant surface characteristics have played a major role in accelerating osseointegration.1 Equally significant has been a progression from the standard parallel implant of the 1980s and early 1990s to the more tapered designs currently available throughout the industry. Furthermore, by utilizing the concept of “platform switching,” whereby the fixture and abutment interface are moved further toward the center of the implant body, the inflammatory component previously seen in this area is reduced, and the crestal bone is maintained at a higher level.2-6 The ability to achieve excellent initial stability through the use of tapered fixtures capable of withstanding relatively high placement torque, coupled with superior bioactive surface characteristics and integrated platform switching designs, is encouraging more clinicians to provide their patients with immediate restorations at the time of initial implant surgery.7
Typically, reports of immediate implant restorations focus on cases in which fixtures have been splinted together in the mandible or even in the maxillary arches if the bone quality is found to be exceptionally sound and the implants can accommodate being immediately loaded.8,9 Reports involving single fixtures frequently deal with the maxillary lateral incisors.10-15 When patients exhibit cuspid-protected occlusions, these specific teeth lend themselves well to placement of immediate restorations. Although there are reports focusing on immediate restorations placed in the maxillary and mandibular molar region, the authors are unaware of any reports that specifically focus on a more limited subset of the posterior dentition, such as maxillary premolars.16 In most patients, maxillary premolars are displayed during full smile and are considered part of the esthetic zone.17 Successful outcomes in this region could introduce a viable esthetic treatment option for patients.
The Study
This report is based on a retrospective analysis of 12 consecutive patients who received placement of dental implants in the maxillary premolar region followed by fabrication and delivery of immediate restorations while treated at the Veterans Administration (VA) Medical Center in Washington, DC.
Material and Methods
A retrospective analysis was performed on 12 consecutive patients who had undergone implant surgery to replace a missing maxillary premolar along with simultaneous placement of the restoration. As these patients were treated within the scope of the General Practice Residency Program, detailed documentation was available for analysis. The minimum period of observation was 1 year.
In general, patients were considered to be candidates for this therapy if they met the following criteria: 1) The patients were free of any systemic condition that might significantly affect osseointegration, such as poorly controlled diabetes, chronic steroid use, tobacco use exceeding five cigarettes per day, an uncooperative mental state, or being immunocompromised; 2) The tapered fixture placed at the time of surgery (NanoTite™ Prevail® Tapered Implant, Biomet 3i, www.biomet3i.com) had to be capable of undergoing a seating torque of at least 50 Ncm, and the occlusal scheme had to permit minimal centric contact and no eccentric contact; 3) At least 4 months had to have elapsed after tooth removal before proceeding with surgery.
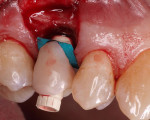
After implant placement, a plastic temporary abutment cylinder (NanoTite Performance Cylinder, Biomet 3i) was seated within the internal connection chamber of the fixture. A strip of rubber dam material was then placed over the abutment to prevent any flowable restorative materials from making contact with the surgical site or the surface of the implant (Figure 1 and Figure 2). Placement of a cotton-tip applicator within the screw access channel followed to ensure patency.
One of three different techniques was then employed to fabricate the temporary crown: In three instances, a preformed polycarbonate shell crown was modified to allow it to slide over the temporary abutment cylinder and was luted in place to the abutment cylinder with a light-cured resin material. Upon removal of the temporary abutment cylinder, additional resin was added to establish the contours in the apical one third of the restoration. The proximal surfaces were fabricated with convex contours, while the facial surface was fabricated with a flat or concave contour. However, with this technique, the contours in the coronal two thirds and the interproximal contacts are limited to the available sizes of the preformed shell.
In three instances, a thin vacu-form overlay was constructed prior to the procedure based on an ideal wax-up. The overlay was then seated over the temporary cylinder in much the same manner as described above.
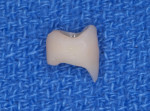
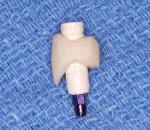
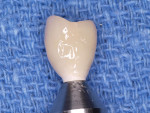
In the remaining six instances a custom temporary shell crown was fabricated in the laboratory before the procedure (Figure 3 and Figure 4). This ensured ideal interproximal contours as well as ideal interproximal contacts.
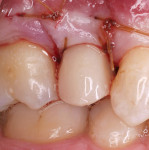
Regardless of the technique employed, once the temporary restoration was fabricated, it was polished and placed with an insertion torque of 20 Ncm (Figure 5 and Figure 6). The soft tissue was then sutured to reestablish ideal contours (Figure 7). The patient was instructed to avoid any masticatory function over this particular area for at least 4 weeks (Figure 8).
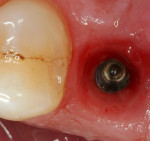
At 6 to 8 weeks, a fixture-level impression was performed. Due to the fact that significant effort was expended to ensure optimal emergence of the restoration from the gingival tissues, use of a standard round impression coping would have compromised the results (Figure 9). Therefore, the emergence contours of the existing temporary crown were used as a template to fabricate a customized impression coping (Figure 10 through Figure 13).18 This was then sent to a laboratory (Atlantis, Waltham, MA) for fabrication of a computer-generated custom abutment. The average length of time, which spanned the original surgery date to placement of the final restoration, was 3.5 months.
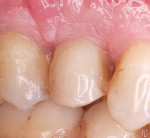
The following measurements were recorded 1 month after placement of the permanent restoration and then again at 1 year (Figure 14): pocket depth, facial recession relative to the mid-buccal aspect of the proximal teeth, and recession from the tips of the proximal papilla to the contact point.
Results
All 12 surgical sites healed uneventfully. Two patients returned to the clinic at 4 weeks with concern that their crowns felt mobile. In both cases, it was found that the abutment screws had become loose, while the fixtures themselves were stable. The screws were re-tightened and the patients were again reminded to minimize masticatory forces at those locations for at least an additional 2 to 3 weeks. Pocket depth for all 12 implant-retained restorations remained at or below 4 mm 1 year after surgical placement.
Although a periosteal release was normally employed to advance the flap 1 mm to 2 mm and reduce subsequent tension, at 3 weeks, all facial flaps stabilized at a favorable level relative to the adjacent teeth. No further recession was noted 1 year after surgery.
In 11 out of 12 cases, the interproximal papillae were left intact throughout the surgical procedure, thereby ensuring minimal loss of postoperative interproximal height. In one instance, the distal papilla had to be reflected. As this site also displayed a loss of interproximal bone, there was a predictable loss of papillary height noted at the 3-week postoperative visit as well as at the 1-year follow up.19-21
Discussion
To the best of the authors’ knowledge, this is the first published report dealing with the simultaneous placement of a dental implant and its associated temporary restoration on a particular subset of teeth such as maxillary premolars. Recent advances in biomechanical engineering have significantly facilitated the ability of dental implants to achieve greater placement torque and, therefore, accept restorative components much earlier than traditional protocols advocated. Earlier concerns regarding the potential to induce pressure necrosis within the bone when using placement torque exceeding 50 Ncm has not been seen clinically.22 As the restorative components contribute significantly to final tissue contours and esthetic outcomes, it becomes most advantageous to begin developing these contours as early as possible in the healing sequence. The use of a custom temporary crown to shape and condition the gingiva provides for a more predictable esthetic outcome when compared to the traditional use of healing caps and cover screws.13 Upon healing, the gingival contours created during such tissue conditioning can be preserved and reproduced in the master model through the use of a custom impression coping.
Three different techniques were used to fabricate the temporary restorations. It was generally appreciated by both the surgical and restorative provider that the standard stock crown provided the poorest support for the surrounding interproximal tissues. In two cases, contacts had to be left open and the interproximal papillae could not be fully supported. The most predictable technique appeared to be use of a laboratory-fabricated, customized shell crown. The vacu-form overlay technique will also yield acceptable results, although it was found to be more time-consuming.
There are certainly some logistical concerns relative to these procedures. Either the surgical provider must be adept at fabrication of the temporary restoration or the restorative clinician must be available immediately after fixture placement. In the authors’ practice environment, this was generally not a problem. Furthermore, it is imperative that the site is not closed until the temporary is in place in order to properly secure the flap at the desired location. Here again, if both providers are not co-located, the restorative provider needs to feel comfortable with flap closure or the patient has to once again return to the implant surgeon’s office.
Although clinicians may have concern with regard to the amount of time necessary to fabricate such a custom temporary, it was generally found that an experienced restorative provider is capable of fabricating such a restoration in 20 to 30 minutes.
Conclusion
Immediate temporization of dental implants provides the patient with an esthetic alternative to the traditional healing cap. In the past, immediate restorations were limited to anterior cases. With recent improvements to implant surfaces and design, achieving primary stability is now more predictable in posterior regions. Along with primary stability, a favorable occlusal scheme and patient compliance are indications for the use of immediate implant restorations in the premolar region. Providing these restorations in premolar areas can potentially lead to more esthetic tissue results and greater patient satisfaction.
Authors’ Note
In keeping with VA Medical Center policy, this manuscript was submitted to the Research and Development Committee of the Washington, DC, VA Medical Center prior to submission to Compendium. It was reviewed as a retrospective case analysis and approved for submission.
Opinions and assertions contained in the article are those of the authors and are not to be construed as necessarily representing the views of the Department of Veterans Affairs.
References
1. Wennerberg A, Albrektsson T. On implant surfaces: A review of current knowledge and opinions. Int J Oral Maxillofac Implants. 2010;25(1):63-74.
2. Lazzara RJ, Porter SS. Platform switching: A new concept in implant dentistry for controlling postrestorative crestal bone levels. Int J Periodontics Restorative Dent. 2006;26(1):9-17.
3. Calvo-Guirado JL, Ortiz-Ruiz AJ, López-Marí L, et al. Immediate maxillary restoration of single-tooth implants using platform switching for crestal bone preservation: A 12-month study. Int J Oral Maxillofac Implants. 2009;24:275-281.
4. Prosper L, Redaelli S, Pasi M, et al. A randomized prospective multicenter trial evaluating the platform-switching technique for the prevention of postrestorative crestal bone loss. Int J Oral Maxillofac Implants. 2009;24(2):299-308.
5. Romanos GE, Nentwig GH. Immediate functional loading in the maxilla using implants with platform switching: Five-year results. Int J Oral Maxillofac Implants. 2009;24(6):1106-1112.
6. Chang CL, Chen C-S, Hsu ML. Biomechanical effect of platform switching in implant dentistry: A three-dimensional finite element analysis. Int J Oral Maxillofac Implants. 2010;25(2):295-304.
7. Ottoni JM, Oliveira ZF, Mansini R, Cabral AM. Correlation between placement torque and survival of single–tooth implants. Int J Oral Maxillofac Implants. 2005;20(5):769-776.
8. Hinze M, Thalmair T, Bolz W, Wachtel H. Immediate loading of fixed provisional prostheses using four implants for the rehabilitation of the edentulous arch: A prospective clinical study. Int J Oral Maxillofac Implants. 2010;25(5):1011-1018.
9. Weber HP, Morton D, Gallucci GO, et al. Consensus statements and recommended clinical procedures regarding loading protocols. Int J Oral Maxillofac Implants. 2009; 24 suppl:180-183.
10. De Rouck T, Collys K, Cosyn J. Immediate single-tooth implants in the anterior maxilla: A 1-year case cohort study on hard and soft tissue response. J Clin Periodontol. 2008;35(7):649-657.
11. Block M, Finger I, Castellon P, Lirettle D. Single tooth immediate provisional restoration of dental implants: Technique and early results. J Oral Maxillofac Surg. 2004;62(9):1131-1138.
12. Degidi M, Nardi D, Piattelli A. Immediate versus one-stage restoration of small diameter implants for a single missing maxillary lateral incisor: A three-year randomized clinical trial. J Periodontol. 2009;80(9):1393-1398.
13. Norton MR. A short-term clinical evaluation of immediately restored maxillary TiOblast single-tooth implants. Int J Oral Maxillofac Implants. 2004;19(2):274-281.
14. Locante WM. The nonfunctional immediate provisional in immediate extraction sites: a technique to maximize esthetics. Implant Dent. 2001;10(4):254-258.
15. Kupeyan HK, May KB. Implant and provisional crown placement: A one stage protocol. Implant Dent. 1998;7(3):213-219.
16. Atieh MA, Payne AGT, Duncan WJ, et al. Immediate placement or immediate restoration/loading of single implants for molar tooth replacement: A systematic review and meta-analysis. Int J Oral Maxillofac Implants. 2010;25(2):401-415.
17. Van der Geld P, Oosterveld P, Kuijpers-Jagtman AM. Age-related changes of the dental aesthetic zone at rest and during spontaneous smiling and speech. Eur J Orthod. 2008;30(4):366-373.
18. Hinds, KF. Custom impression coping for an exact registration of the healed tissue in the esthetic implant registration. Int J Periodontics Restorative Dent. 1997;17(6):585-591.
19. Choquet V, Hermans M, Adriaenssens P, et al. Clinical and radiographic evaluation of the papilla level adjacent to single-tooth dental implants. A retrospective study in the maxillary anterior region. J Periodontol. 2001;72(10):1364-1371.
20. Gastaldo JF, Cury PR, Sendyk WR. Effect of the vertical and horizontal distances between adjacent implants and between a tooth and an implant on the incidence of interproximal papilla. J Periodontol. 2004;75(9):1242-1246.
21. Romeo E, Lops D, Rossi A, et al. Surgical and prosthetic management of interproximal region with single-implant restorations: 1-year prospective study. J Periodontol. 2008;79(6):1048-1055.
22. Meltzer A, Baumgarten H, Testori T, Trisi P. Pressure necrosis and osseointegration. Biomet 3i–Clinical Research Publication. 2009;9:1-6.
About the Authors
Adam A. Sarnowski, DMD
General Dentist
Dental Service
Veterans Administration (VA) Medical Center
Washington, DC
Brian F. Paul, DMD, MSEd
Periodontist
Dental Service
Veterans Administration (VA) Medical Center
Washington, DC