Clinical Case Report: Treatment of Anterior Teeth with an Implant, Veneers, and Full-Coverage Restorations
Background
Age at Initial Presentation: 35
Initial Presentation: June 2007
Treatment Completed: November 2007
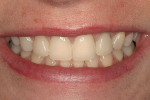
The patient presented with a chief complaint: “I don’t like the way my teeth are different colors; the two front ones are different sizes; there is a black line around my crown; and I don’t like my bridge.” She wanted her four front teeth to match and to have whiter teeth (Figure 1 and Figure 2). The patient did not want another bridge but desired a single-tooth implant.
Medical History
Within normal limits (WNL).
Diagnostic Findings
Temporomandibular Joints: WNL.
Extraoral: WNL; low lip and smile line.
Intraoral: The patient had central incisors that varied in length and width. An old composite veneer was on tooth No. 9. There were gingival height discrepancies. She did not like how the incisal edges did not match, and the dark triangles were an issue for her. She wanted an implant to replace the metal resin-bonded bridge where the left lateral was missing congenitally.
Occlusion: Class I.
Periodontal: WNL; the patient did not want to proceed with periodontal treatment to correct any gingival level discrepancies if deemed minor.
Radiographic Assessment
Adequate bone was available for placement of an implant.
Risk Assessment
Dentofacial: Low
Periodontal: Low
Biomechanical: Low
Functional: Low
Esthetics: Moderate to high
Prognosis
The overall prognosis was good. The patient could have functioned with her existing restorations but chose to replace the crown and bridge and have porcelain veneers placed on the central incisors. The tissue was thin, so a zirconium abutment would be used to help prevent grey shine through the tissue.
Concerns
1. What type of restorations would be placed—ceramic, zirconium, or feldspathic veneers?
2. Could the patient’s esthetic demands be fulfilled?
3. Using different material substrates can affect the overall matching of the restorations.
4. Could an immediate implant and provisional be placed at the time of surgery?
Treatment Plan
The patient chose treatment that consisted of removing the old porcelain fused to metal crown and replacing it with a feldspathic jacket crown. Porcelain veneers would be placed on the central incisors. An implant would be placed in the left lateral position. A zirconium abutment with porcelain that would be fired onto it would be placed, enabling the final jacket crown to be bonded.
Treatment
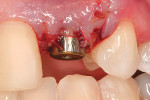
The resin-retained bridge was removed using a pneumatic crown remover (Easy Pneumatic Crown and Bridge Remover II, Dent Corp, White Plains, NY). The crown remover works by hooking it to the connection where the hand-pieces are normally connected and the rheostat is used (Figure 3). It works virtually every time when removing those types of bridges (Figure 4). The patient was sent immediately to the oral surgeon for placement of an implant. After the implant, the patient returned to the office with the healing abutment hand-tightened (Figure 5). An immediate provisional was fabricated because the implant was torqued to 40 ncm. A temporary abutment was placed (Figure 6) and a bisacryl temporary cemented onto the metal post (Figure 7). The provisional was taken out of occlusion, and all excursive movements were checked. The patient was instructed not to function on that tooth directly. The patient returned 12 weeks later for final restorative work (Figure 8).
Restorative Phase
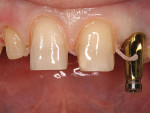
The porcelain fused to metal crown was removed on the right lateral, and the central incisors were prepared for feldspathic porcelain veneers. A feldspathic jacket crown also would be made for the right lateral. Because of the tooth-size discrepancy of the centrals, the contacts were broken on the mesial. This would allow the ceramist to make the centrals symmetrical and close any black triangle. The preparations were minimal with about 0.05 mm removed. The midline also could be corrected in the final restorations. A retraction cord was placed, and an impression coping was placed on the fixture for a fixture level impression. A closed tray was used, and a polyvinyl impression was made (Figure 9 and Figure 10). The impression was sent to the laboratory and the patient scheduled to return in 3 weeks for the insertion.
When the patient revisited the office, the provisionals were removed and the teeth pumiced. The gingival tissue was isolated with a retraction cord. The teeth were etched, and a fourth-generation bonding agent was used (ALL-BOND 2®, Bisco Dental Products, Shaumberg, IL). Resin cement (Insure, Cosmedent® Inc, Chicago, IL) was placed in the restorations, and they were seated and bonded. All areas were light-cured for 60 sec. A special abutment was fabricated for the implant restoration. It is impossible to bond to zirconium, and the author wanted all the restorations to be made of the same material. Feldspathic porcelain was fired onto the zirconium abutment and then etched with hydrofluoric acid so the crown could be bonded with the same resin cement. This was done in the same manner as the previous restorations (Figure 11). The final restorations are shown in Figure 12 and Figure 13.
Commentary
The patient was extremely happy with the final result and appreciated that a removable appliance was not needed during the implant healing. When an abutment and provisional can be made the same day, it is much more comfortable for the patient and better for soft-tissue healing. This case could have been more difficult to achieve a high level of esthetics if different substrates of material had to be used.
Acknowledgments
Implant surgery by John Maletta, DDS, MS; Ceramics by Uri Yarovesky, Opus One Laboratories Inc (Agoura Hills, California).
About the Author
Robert C. Margeas, DDS
Private practice
Iowa City, Iowa
Adjunct Professor
University of Iowa College of Dentistry
Iowa City, Iowa