Does a Consistently Reliable Solution Exist for the Successful Placement of Class II Composite Resin Restorations?
Abstract
Many restorative dentists cobble together materials and techniques from different manufacturers to create systems that work for their clinical needs. The author proposes that it may be possible to improve outcomes and continue toward excellence by selecting the ideal restorative solution with materials designed, tested, and intended to be used together. DENTSPLY Caulk’s Class II solution is examined in this article as a means for helping in placement of posterior restorations, namely Class II restorations. A case report is explored.
A famous basketball coach commented, “Excellence is the unlimited ability to improve the quality of what you have to offer.”1 This is especially true for dental materials and, in particular, the evolution of dental composites. Since the introduction of resin-based light-cure composite in the 1970s, practitioners have attempted to leverage materials and techniques to achieve successful placement of composite restorations in many clinical situations. Because placement of composite restorations is exacting and tedious, unique challenges such as isolation, adhesion, materials selection, and polishability can directly impact the procedure’s outcome. With more than 70 restorative composite brands currently on the market, not including flowables and dual-cure composites, today’s dentist has a potentially confusing array of materials to choose.2
Why should restorative dentists not consider a specially designed and coordinated system for the placement of posterior restorations, specifically Class II restorations? Other facets of dentistry currently utilize systems or process solutions, namely implant placement kits, designed for practitioners to follow a path to successful clinical outcomes. If a solution is needed for Class II composite restorations, then the challenges to be overcome include such factors as open interproximal contacts, poor anatomic contour, inadequate marginal seal, postoperative sensitivity, marginal staining, recurrent caries, and fracture.3
Formulating a solution for creating consistently excellent Class II composite restorations requires a process for both materials and techniques. To this point, many dentists have put various equipment and materials together to form their own Class II systems; however, these hodgepodge systems may include materials from various manufacturers. Using the “this works best in my hands” argument, practitioners may assemble their own Class II solutions based on completion of repetitive procedures and clinical observations. However, it may be possible to improve outcomes and continue toward excellence by selecting the ideal restorative solution with materials designed, tested, and intended to be used together.2
DENTSPLY Caulk has designed a Class II composite resin restorative solution based on aligning products to overcome the stated challenges. From isolation of the preparation to finishing of the cured restoration, the DENTSPLY Caulk solution should provide outstanding clinical results with increased efficiency and simplified material choices.
This article discusses DENTSPLY Caulk’s Class II solution, focusing on the processes of isolation, adhesion, composite placement, and polishing as they coalesce to form excellent Class II composite restorations. A clinical case will be presented to illustrate the use and to describe the techniques discussed.
Isolation
A rubber dam is considered the gold standard for isolation of prepared teeth prior to composite resin placement. However, in the case of Class II composite restorations, isolation with a matrix system is the challenge. Not only does the selected matrix system need to seal the preparation to help achieve marginal integrity, it needs to mimic natural tooth contour and facilitate interproximal contact.3 Historically, circumferential matrices (Tofflemire; AutoMatrix®, DENTSPLY) have been used but have inherent limitations. While effective in sealing the preparation, Tofflemire matrices provide little help in creating proper interproximal contact, both in the shape and position of the contact or the actual strength of contact, all of which influence the potential for food impaction.4,5
It was not until 1986 and the introduction of the BiTine™ sectional matrix system (Darway Inc.) that a better system for creating Class II contacts in composite resin was introduced.6 The Palodent® Plus sectional matrix system (DENTSPLY), introduced in 2011, was designed to overcome the inadequacies of the circumferential matrix and the shortcomings of the BiTine system (eg, seating and stabilizing the ring, preventing the ring from collapsing the matrix on a wide buccolingual preparation). The three main parts of the Palodent Plus system are a nickel-titanium ring capable of separating the teeth and sealing the matrix, Palodent Plus EZ Coat matrices that offer a microthin supercurved form and nonstick finish to make matrix removal easier, and wave-shaped wedges7 (Figure 1).
In the past, the wedge was used to separate the teeth and seal the gingival margin of the preparation by adapting the matrix to the tooth.3 The wave-shaped wedges of Palodent Plus have wings that compress during placement and then flare when inserted to help adapt and seal the matrix. The result is improved marginal integrity and anatomic proximal contour of the restoration. Because matrix design is not one size fits all, Palodent Plus is offered with two ring sizes, five matrix sizes, and three wedge sizes, making optimal fit and adaptation simple.7
An additional innovative component of the Palodent Plus system is the wedge guard. To prevent unintended damage to adjacent teeth during preparation, wedge guards attach a thin piece of metal matrix to the top of a wedge. After preparation is complete, the metal guard is easily detached, leaving the wedge available for adaptation of the final matrix and ring placement (Figure 2 and Figure 3).
Adhesion
The next step in DENTSPLY Caulk’s Class II composite solution is easy and predictable bonding to enamel and dentin. Since 1955, Buonocore’s acid-etching technique has made bonding to enamel successful.8 However, achieving consistent dentin bonding has been more challenging based on factors such as microleakage, resin infiltration and penetration, hydration versus desiccation, and postoperative sensitivity.9 To mitigate these factors, the evolution of dentin bonding has included a shift from total-etch techniques involving placement of 30% to 40% phosphoric acid on both enamel and dentin surfaces (ie, etch-and-rinse) to self-etch techniques in which phosphoric acid esters are contained within the bonding agent and no etchant gel is placed on the preparation.10
Recently, a third bonding technique has emerged that allows for hybridization of the remaining dentin smear layer and includes phosphoric etching of exposed enamel to maximize bond strength and prevent marginal discoloration. The selective-etch technique is designed to harness the positive attributes of both techniques for improved clinical outcomes. Several recent studies have found selective-etch adhesives to have increased enamel bonding while reporting no postoperative sensitivity.11,12 Heintze and Rousson13 concluded in their meta-analysis that restorations placed with rubber-dam isolation and enamel-etching technique showed the best overall performance.
Prime&Bond Elect™ (DENTSPLY Caulk) is designed as a one-bottle dental adhesive suitable for all three adhesive modes: total etch, self etch, and selective etch. Built from 13 years of proven PENTA (ie, the adhesive resin dipentaerythritol pentaacrylate monophosphate) technology from Prime & Bond® NT™, this new bonding agent provides a unique micromechanical and chemical bond for long-term success.14 It is ideal in cases in which the preparation is primarily in enamel and total-etch technique is indicated; in preparations in mostly dentin, a self-etch technique can be used; and for preparations containing significant enamel and dentin, a selective-etch technique is advised. According to Prime&Bond Elect’s directions for use, practitioners should not fear negative sequelae such as decreased dentin bond strengths if unintended phosphoric etchant gel contacts exposed dentin as with other products (eg, Clearfil SE).15
Composite
Resin composite placement involves using a precise and strategic process to complete. Challenges to the practitioner include: proper adaptation of material to the preparation, bulk-fill versus incremental fill techniques, polymerization shrinkage and shrinkage stress, depth of cure, and handling of the material. Recent data have suggested that incremental fill techniques to minimize C-factor (ratio of bonded to unbonded surfaces) may not be successful in mitigating polymerization shrinkage stress, and new composite technologies and materials are now focusing on bulk-fill techniques (eg, SonicFill™, Kerr; SureFil® SDR® flow, DENTSPLY Caulk).16-19
Historically, practitioners have used flowable composites as liners in Class II preparations because of their increased wetting and ability to adapt to walls. However, concerns about inferior mechanical properties and high polymerization shrinkage of such materials have dictated conservative use in thin layers. Kerr’s Revolution Formula 2™
is a flowable composite that has 59% filler by weight and exhibits 4.9% polymerization shrinkage resulting in 3.2 mPa of shrinkage stress.20-22 Revolution Formula 2 should be placed in layers not exceeding 2 mm.23 In 2009, DENTSPLY Caulk introduced SureFil® SDR® flow. (SDR means stress decreasing resin.) The addition of a polymerization modulator in SureFil SDR flow resin was designed to reduce stress buildup on polymerization without a reduction in the polymerization rate or conversion.24 As a result, SureFil SDR flow has 68% filler by weight and exhibits 3.5% shrinkage resulting in 1.6 mPa of shrinkage stress—a 50% reduction compared with Revolution Formula 2. In addition, SureFil SDR flow can be cured in 4-mm increments (although the manufacturer recommends a 2-mm restorative occlusal cap).25,26 From DENTSPLY’s website: “Through the use of the ‘Polymerization Modulator’, the resin forms a more relaxed network and provides significantly lower polymerization stress.”
The depth and dimensions of a Class II proximal box will vary by the tooth involved and the extent of the carious lesion. Additional factors that may impact the design of the preparation include esthetic requirements, relationship to the adjacent tooth, and rotations and inclinations. Volchansky and Cleaton-Jones27 showed in their study that the clinical crown heights of posterior teeth ranged from approximately 8 mm for first premolars to 4 mm for second molars. In today’s practice, efficiency is gained by not only performing outstanding dentistry, but doing so quickly and without repeated steps.28,29 By combining potential 4-mm increments of SureFil SDR flow, placement steps can be minimized and restorations completed faster.
To provide the occlusal cap (the layer of composite restoring the occlusal-most layer of the restoration), DENTSPLY caulk has introduced TPH Spectra™ to provide a strong, durable, and natural-looking restoration. This new composite is based on the resin technology of TPH®3 and contains nanohybrid- and micro-filler components. The result is a composite that has the potential to perform well in either the anterior or posterior, and should have tooth-like translucency, excellent polishability and color stability, and good wear resistance.30-32 TPH Spectra also is available in two handling choices: a creamy light-viscosity formulation and a packable high-viscosity formulation. For both viscosities, the physical properties are similar.33 Because handling preference is subjective and highly individualized, practitioners are now able to select the right viscosity for all clinical situations.
To make shade selection simpler, TPH Spectra is available in the seven most popular shades: B1, A1, A2, A3, A3.5, A4, and C2. According to DENTSPLY’s internal data, the seven shades of TPH Spectra represent more than 80% of total sales from the previous TPH 3 formulation.34 The TPH Spectra shade guide was condensed for several reasons. First, some practitioners may be overwhelmed with the number of current shades—the Vita Classic (Vident) shade guide has 16 shades, and the TPH 3 shade guide has 26. Because only seven of the current 26 TPH 3 shades are regularly purchased, the color difference (ie, Delta-E value) between shades was calculated to determine if a top-seven shade could be used in place of another shade not offered. It will be possible to “cover” all the Vita shades with the existing TPH Spectra offerings by keeping the Delta-E to less than 4 (if the two shades, tooth composite or composite composite, have a Delta-E difference of less than 4, the difference is difficult for the human eye to distinguish).35,36
TPH Spectra also offers excellent color blending between restorative materials and natural tooth, often called, “the chameleon effect.” Again, building and improving from the previous TPH 3 composite formulation, TPH Spectra has a refractive index that falls directly between enamel (1.63) and dentin (1.54).36,37 Because of TPH Spectra’s excellent translucent properties and an appropriate refractive index similar to natural tooth structure, TPH Spectra will have an excellent chameleon effect and create restorations that are unable to be detected.
Polishing
The final step for achieving excellent clinical results with Class II composite resin is gross contouring with a high-speed handpiece followed by finishing and polishing of the restoration.38 The polishability of a composite is based on the filler type, shape, and content. Although a recent study showed that hybrid and microfilled composites perform best clinically, the trend in composite technology is for universal applicability. The creation of ideal surface polish on a composite restoration can improve the esthetics and the longevity of restoration by reducing stain potential, biofilm accumulation, and gingival inflammation, and by minimizing the wear.39 In a study by Berger et al40 examining three composites and polishing systems (DENTSPLY Caulk, 3M ESPE, and Cosmodent), the researchers concluded that, “the polishing system from the same company as the composite resin should be used, as these showed good results in comparison with other polishers.”
DENTSPLY Caulk’s solution to finishing and polishing composite restorations is a two-step process involving Enhance® Finishers (DENTSPLY Caulk) and PoGo® Polishers (DENTSPLY Caulk). Enhance consists of a single-use, premounted, aluminum oxide-impregnated finisher designed to prepare composite surfaces for a final polish. PoGo is very similar to Enhance except that the single-use polishers are diamond impregnated to create a final glossy polish that will appear lifelike and are resistant to stain and wear. Both Enhance and PoGo fit onto a latch-type slow-speed handpiece.
Case Example
A 20-year-old female presented to the office for examination of a noticeable cavity in a maxillary right tooth. After the clinical examination was performed, the patient agreed to a treatment plan that included root canal therapy on tooth No. 4 followed by a core build using direct composite. Because of the patient’s financial constraints, the definitive restoration of tooth No. 4 using full coverage was postponed several months (Figure 4).
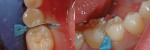
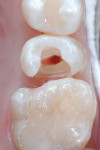
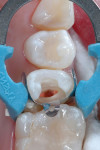
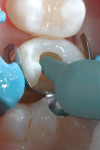
After local anesthesia with one carpule of 4% Articadent™ with 1:100,000 epinephrine (DENTSPLY Pharmaceutical) was administered, root canal therapy was completed conventionally under rubber dam isolation without complication. The patient had difficulty tolerating the rubber dam, so it was removed during the restoration of tooth No. 4. The coronal portion of the gutta-percha filling material was burned down so composite restorative materials could be placed into the orifice (Figure 5). Generally, a selective-etch adhesive technique should be chosen for situations in which there is a large amount of exposed dentin to maximize enamel bonding and prevent over-etching.12,41
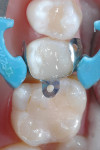
The exposed enamel surfaces were etched with 34% phosphoric acid for 20 seconds and then thoroughly rinsed with water. Isolation of the preparation was achieved using Palodent Plus (Figure 6). Prime&Bond Elect was scrubbed into the preparation for 20 seconds, followed by a 5-second air drying to remove the solvent. The bonding agent was light cured for 20 seconds.
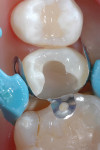
An initial layer of SureFil SDR flow was placed into the preparation, followed by a 20-second light-cure (Figure 7 and Figure 8). TPH Spectra High-Viscosity shade A2 was packed into the preparation and cured in 2-mm increments (Figure 9 and Figure 10).
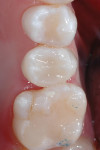
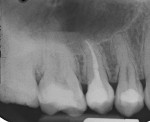
The final restoration was finished with fluted composite burs and polished with Enhance and PoGo (Figure 11). The final radiograph of the restoration shows high radiopacity of the resin restorative materials and no junction can be discerned between the flowable and restorative materials (Figure 12).
Conclusion
Current dental materials are technologically advanced and capable of spectacular results when utilized carefully and precisely. Systems exist in dentistry to provide step-by-step solutions to clinical situations that, if followed, can lead to positive outcomes. These solutions have existed in implantology and fixed prosthodontics, and now DENTSPLY Caulk has created a predesigned, coordinated Class II solution for placement of consistently outstanding composite restorations.
DISCLOSURE
Dr. Goodchild is a DENTSPLY Caulk employee.
References
1. Rick Pitino quotes. Thinkexist.com.https://thinkexist.com/quotation/excellence_is_the_unlimited_ability_to_improve/151330.html. Accessed March 13, 2013.
2. Devoto W. Saracinelli M, Manauta J. Composite in everyday practice: how to choose the right material and simplify application techniques in the anterior teeth . Eur J Esthet Dent. 2010;5(1):102-124.
3. Shuman I. Excellence in class II direct composite restorations . Dent Today. 2007;26(4):102,104-105.
4. Kurtzman GM. Improving proximal contours for direct resin restorations . Dent Today. 2010;29(4):106,108-109.
5. Strassler HE, Trushkowsky RD. Predictable restoration of Class 2 preparations with composite resin . Dent Today. 2004;23(1):93-99.
6. Karst LE. The elusive tight contact with composite restorations. How to achieve it . Dent Today. 2003;22(11):76-79.
7. DENTSPLY Caulk Palodent Plus. https://palodentplus.com. Accessed March 13, 2013.
8. Buonocore MG. A simple method of increasing the adhesion of acrylic filling materials to enamel surfaces . J Dent Res. 1955;34(6):849-853.
9. Alex G. Is total-etch dead? Evidence suggests otherwise . Compend Contin Educ Dent. 2012;33(1):12-4,16-22,24-25.
10. Perdigão J, Geraldeli S, Hodges JS. Total-etch versus self-etch adhesive: effect on postoperative sensitivity . J Am Dent Assoc. 2003;134(12):1621-1629.
11. Frankenberger R, Lohbauer U, Roggendorf MJ, et al . Selective enamel etching reconsidered: better than etch-and-rinse and self-etch? J Adhes Dent. 2008;10(5):339-344.
12. Perdigão J. New developments in dental adhesion . Dent Clin North Am. 2007;51(2):333-357.
13. Heintze SD, Rousson V. Clinical effectiveness of direct class II restorations—a meta-analysis . J Adhes Dent. 2012;14(5):407-431.
14. Van Landuyt KL, Snauwaert J, De Munck J, et al. Systematic review of the chemical composition of contemporary dental adhesives . Biomaterials. 2007;28(26):3757-3785.
15. Yazici AR, Akca T, Ozgünaltay G, Dayangaç B. Bond strength of a self-etching adhesive system to caries-affected dentin . Oper Dent. 2004;29(2):176-181.
16. Versluis A, Douglas WH, Cross M, Sakaguchi RL . Does an incremental filling technique reduce polymerization shrinkage stresses? J Dent Res. 1996;75(3):871-878.
17. Moorthy A, Hogg CH, Dowling AH, et al. Cuspal deflection and microleakage in premolar teeth restored with bulk-fill flowable resin-based composite base materials . J Dent. 2012;40(6):500-505.
18. Braga RR, Hilton TJ, Ferracane JL. Contraction stress of flowable composite materials and their efficacy as stress-relieving layers . J Am Dent Assoc. 2003;134(6):721-728.
19. Van Ende A, De Munck J, Van Landuyt KL, et al. Bulk-filling of high C-factor posterior cavities: effect on adhesion to cavity-bottom dentin . Dent Mater. 2013;29(3):269-277.
20. Competitive Product Comparison. https://multimedia.3m.com/mws/mediawebserver?mwsId=66666UF6EVsSyXTtnxM_nXn2EVtQEVs6EVs6EVs6E666666--. Accessed March 13, 2013.
21. Kleverlaan CJ, Feilzer AJ. Polymerization shrinkage and contraction stress of dental resin composites . Dental Mater. 2005;21(12):1150–1157.
22. Attar N, Tam LE, McComb D. Flow, strength, stiffness and radiopacity of flowable resin composites . J Can Dent Assoc. 2003;69(8):516-521.
23. Revolution Formula 2 [product brochure] . Orange, CA: Kerr Corporation. 2011. https://www.kerrdental.com/cms-filesystem-action?file=/kerrdental-products-dfu/2011_Revolution_Formula_2.pdf. Accessed March 13, 2013.
24. DENTSPLY Caulk Surefil SDR Flow. https://www.surefilsdrflow.com. Accessed March 13, 2013.
25. Surefil SDR Flow Manual [product brochure] . Milford, DE: DENTSPLY Caulk. 2011. https://www.surefilsdrflow.com/sites/default/files/SureFil_Technical_Manual.pdf. Accessed March 13, 2013.
26. Surefil SDR Flow Directions for Use [product brochure] . Milford, DE: DENTSPLY Caulk. 2011. https://www.surefilsdrflow.com/sites/default/files/SureFil_DFU.pdf. Accessed March 13, 2013.
27. Volchansky A, Cleaton-Jones P. Clinical crown height (length)—a review of published measurements . J Clin Periodontol. 2001;28(12):1085-1090.
28. Jackson RD. Placing posterior composites: increasing efficiency . Dent Today. 2011; 30(4):126,128,130-131.
29. Goodchild JH, Conte NR. Leveraging composite characteristics to produce superior results . Inside Dentistry. 2013;9(4):102-106.
30. Garg N, Garg A. Tooth preparation for composite restorations. In: Textbook of Operative Dentistry. New Delhi, India: Jaypee Brothers Medical Publishing; 2010:260.
31. LeBlanc BJ. Nanohybrid composite restorations: dentistry’s most versatile solution. Dental Economics. May 1, 2009. https://www.dentaleconomics.com/articles/print/volume-99/issue-5/features/nanohybrid-composite-restorations-dentistry39s-most-versatile-solution.html. Accessed January 17, 2013.
32. Vargas M. Nanomicrohybrid composites make posterior placement easier . Dent Today. 2012;31(5):128,130-1.
33. TPH Spectra. DENTSPLY Caulk. https://tphspectra.com. Accessed March 13, 2013.
34. DENTSPLY Caulk . Data on file. 2012.
35. Jaju RA, Nagai S, Karimbux N, Da Silva JD. Evaluating tooth color matching ability of dental students . J Dent Educ. 2010;74(9):1002-1010.
36. Using TPH Spectra. DENTSPLY Caulk. https://tphspectra.com/using-tph-spectra. Accessed March 6, 2013.
37. Meng Z, Yao XS, Yao H, et al. Measurement of the refractive index of human teeth by optical coherence tomography . J Biomed Opt. 2009;14(3):034010.
38. Gönülol N, Yilmaz F. The effects of finishing and polishing techniques on surface roughness and color stability of nanocomposites . J Dent. 2012;40(suppl 2):e64-70.
39. Morgan M. Finishing and polishing of direct posterior resin restorations . Pract Proced Aesthet Dent. 2004;16(3):211-217.
40. Berger SB, Palialol AR, Cavalli V, Giannini M. Surface roughness and staining susceptibility of composite resins after finishing and polishing . J Esthet Restor Dent. 2011;23(1):34-43.
41. Ritter R. Using the selective etch technique for esthetic restorations . Inside Dentistry. 2011;7(3). https://www.dentalaegis.com/id/2011/03/using-the-selective-etch-technique-for-esthetic-restorations. Accessed January 23, 2013.