Health, Beauty, Prosperity and Periodontics
Preventing disease and maintaining a healthy natural dentition is still the main focus of periodontics, and treatment of periodontal disease and peri-implantitis is becoming more successful and predictable. However, when it is not possible to maintain the natural dentition dental implants provide excellent treatment options for patients. While implants are highly effective, dentists should not forget that they possess a number of new regenerative techniques that when delivered by periodontists in collaboration with a restorative office can allow patients to maintain teeth that would have been lost in the past.
There is little disagreement that a healthy periodontium sets the stage for restorative success. All dentists understand the importance of a periodontium without inflammation, with minimal probing depths, adequate keratinized tissue, stable occlusion, mobility within normal limits, appropriate tooth lengths and gingival contours, a healthy biologic width, elimination of pigmentations or tattoos, full papillae, and intact dentitions. Contemporary periodontal therapy can deliver these elements essential to restorative success on a predictable basis.
Patients may not know or care much about the outcomes mentioned above, but they do care very much care about their benefits. Clinicians who understand what patients really want can present treatment in terms of what is important to patients. When communicating to patients, there needs to be more of an emphasis on health than on disease, so that periodontists and their restorative partners can work together better to offer today’s patients the health promoting treatment and esthetic procedures they desire.
Health Considerations
Identification and control of risk factors have always been important elements in treating periodontal diseases. Local factors include elements such as pre-existing disease, deep probing depths, plaque retentive areas, and defective restorations; systemic factors include, among other things, poorly controlled diabetes, smoking, stress and coping behavior, and osteopenia. Background determinants such as age and genetic influences also may play a role in placing patients at greater risk for periodontal diseases. Including management of these and other risk factors should be part of every treatment plan.
A yearly assessment and formal reevaluation on a regular basis is essential to determine the periodontal diagnosis and prognosis of the dentition and/or dental implants.1 Every patient is different. Patients with furcations and vertical defects are at higher risk of progressing disease than those with horizontal bone loss and no furcation involvement. A patient under 40 years of age with moderate periodontal disease may present more difficulties than that of a 60-year-old patient with moderate disease. These people need to be identified earlier and seek appropriate treatment sooner. This can only be accomplished by conducting comprehensive periodontal evaluations.
The key to treating the enormous number of patients who need periodontal care starts with triage. Risk assessment is important to identify those who can be safely treated in general practice and those who need referral and more sophisticated care. A patient with less than 4-mm probing depths, obvious bacterial etiology, limited tooth mobility, and no furcation involvement as a general rule can be safely treated in a general practice, but patients with persistent inflammation, greater than 5-mm probing depths, furcations, intrabony defects (especially vertical), and mobility are patients who would benefit not only from referral, but referral early in the process.
Add to this the growing awareness of links between periodontal and systemic disease that are driven by inflammation. While the focus was once on bacteria, it now seems that inflammation itself is driving an ever-growing list of chronic diseases. This inflammation is not localized strictly to the mouth, where it manifests as redness, swelling, suppuration, and bleeding on probing, leading to hard and soft tissue loss; it also increases the systemic inflammatory burden. There is growing evidence that chronic adult periodontitis puts patients at risk for a large range of inflammatory diseases: respiratory disease, osteoporosis, chronic kidney disease, rheumatoid arthritis, cardiovascular disease, diabetes, and many more. The linkages with some of these diseases can be bi-directional. In the case of patients who have diabetes, eliminating their periodontal disease may make their glycemic control better; conversely, controlling their diabetes will make it easier to bring their periodontal disease under control. That adult periodontitis is now being seen as one of many chronic diseases of aging that has inflammation as a common denominator underscores the importance of regular assessment and early intervention.
There is no doubt that working together in a collaborative approach offers the opportunity not only to improve the patient’s periodontal health, but overall health as well. Contemporary periodontics offers a wider range of skills and effective procedures than simply the treatment of disease and the placement of implants.
Informed Consumers
As the world moves from a handshake to a keystroke, patients are transforming into informed consumers with an increasing opportunity to select from a wide array of choices. To be successful, clinicians should be prepared to provide those treatment options and to fulfill those expectations.
Case in point is the baby boomers, who began turning 65 years old in 2011. By 2020, 1 in 5 of dental patients will be 65 or older. While the baby boomers, who value prevention, are presenting with more teeth than any other generation in history, they also tend to present with a variety of chronic diseases, and it takes teamwork to be able to manage those diseases effectively. For this reason, risk assessment as mentioned above, to manage their current disease and be proactive against future diseases, will be more important than ever. But for this group, living longer is not enough. They want to live better, and they have the money to pay for it. They are interested in wellness, cosmetics, comfort, and value in the treatment at the dental office. They are more self-reliant in deciding who they will allow to treat them and the types of treatments they will accept.
Discretionary Dentistry
It is clear that there is movement from needs-based dentistry toward wants-based dentistry, therefore dentists need to determine what their patients want. To present treatment in terms of what’s important to their patients, dentists need to ask open-ended questions and listen. Patients may not be interested in resolving inflammation or reducing probing depths, but they are interested in preserving bone, eliminating disease, having fresh breath, enhancing quality of life, and saving time and money in the future.
Dentistry is evolving from disease treatment and prevention to health promotion. Clinicians cannot be prosperous psychologically as well as financially unless they spend most of their time providing services people want, not just need.
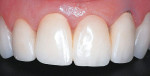
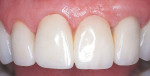
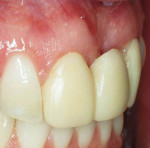
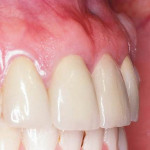
Unfortunately, many dental professionals think that all periodontists have to offer is root planing and scaling, osseous surgery, and single tooth implants. Comprehensive periodontal therapy offers many treatment options that can greatly add to our patient’s quality of life and improve the esthetic results of restorative care. Procedures such as root coverage grafts (Figure 1 and Figure 2), esthetic crown lengthening, ridge augmentation (Figure 3 and Figure 4), and papilla reconstruction are high value treatment options. In addition to these, periodontists are often the best to partner with for full-mouth implant-supported restorations because of their understanding of occlusion and the importance of maintenance care.
Collaboration with a periodontist can also create new revenue streams for the restorative office. For example, periodontal plastic surgery can cover root surfaces even if they have been restored. There are many patients that would be interested in having old crowns and bridges replaced if proper tooth length and gingival contours could be reestablished. This is now possible. The restoration is removed and the new provisional margin is placed at ideal tooth length. The old restorative margin is eliminated and the previously restored root surface is covered with a soft tissue graft. The tooth is prepared at the new gingival margin and restoration is seated.
Computer-guided implant dentistry is another area ripe for collaboration. Implant cases from simple to complex can be treatment planned on the computer with input from both the restorative team and the periodontal surgeon. This allows for precise implant placement which may reduce lab costs and permits in some situations the placement of provisional restorations on the day of implant insertion.
Benefits of Collaborative Care
There is no doubt that periodontists and restorative dentists can improve their practices simply by working together as business partners. One way to improve efficiency is by reducing overhead: There is no reason all clinicians need to own or maintain expensive imaging or CAD/CAM equipment or extensive inventories. Collaborating practitioners can also reduce chair time by concentrating on what they do best. Both laboratory expenses and liability can be reduced by working with a partner who places implants precisely and avoids recession due to well-executed periodontal procedures, and avoids remakes. Collaboration also increases case acceptance, when patients are given the same treatment recommendations by both offices.
Collaboration also offers the flexibility to innovate and increase the clinician’s scope of practice without significant capital outlay, and to have options—for example, conscious sedation or sophisticated regenerative procedures—otherwise unavailable in a solo clinician’s practice. Other potential benefits of collaborating include co-marketing and coordinating patient education.
Ultimately, the greatest benefit of collaborative care is the opportunity to offer the superior outcomes people—especially baby-boomers—expect, while also giving them the value they appreciate as an added benefit. Value is what they remember long after they forgot which tooth was worked on. A collaborative approach increases value in their experience in the clinician’s office.
On the Horizon
Periodontics is not standing still. For example, research using living cells, growth factors and a variety of matrices is allowing periodontists to regenerate both hard and soft tissue more predictably and often without donor sites. Computer-guided implant placement and digital impressions married with CAD/CAM devices will allow them to deliver implants and their restorations more rapidly and with greater precision. Drugs, both local and systemic, will allow them to manage periodontal diseases and peri-implantitis more effectively by reducing inflammatory mediators and stabilizing attachment loss. Chair side diagnostics will give real time assessment of disease activity and allow them to personalize treatment. Perio plastic procedures will continue to be refined and the regeneration of the papilla will finally be possible. All of this and more is just around the corner and the journey will be best traveled together for the benefit of patients.
Conclusion
With a collaborative approach, restorative dentists and periodontists can help not only patients’ periodontal health, but their overall health. Also, working together, especially doing the kind of dentistry described, positions clinicians perfectly in the marketplace by providing two commodities—health and beauty—to a customer base who particularly values these outcomes.
References
1. AAP Statement on Comprehensive Periodontal Therapy. J Periodontol. 2011;82(7):943-947.
About the Author
Michael K. McGuire, DDS
PerioHealth Professionals™
Houston, Texas