CBCT: Facilitating Comprehensive, High-Tech Diagnostics
Not since the intraoral video camera has an advanced imaging technology captured the dental profession so rapidly as cone beam computed tomography (CBCT). A high-technology, high-priced item—retail prices of units range from $70,000 to $300,000—CBCT is being far more rapidly adopted than digital x-ray imaging,1 which has been around for more than 20 years. This is primarily because of the 3-dimensional (3-D) technology’s impact on most dental procedures about which dentists make clinical decisions. While many articles2-4 have been written on the applications of CBCT for dentists and dental specialists, complete citation of such articles is beyond the scope of this report; however, the reader only has to type “dental CBCT” in any web browser to find an abundance of information.
A sampling of manufacturers of CBCT machines sold in North America is listed in Table 1. Some of these companies also manufacture and distribute products under a different label; for example, Imaging Sciences International, LLC also produces machines sold under the names Gendex (www.gendex.com) and KaVo (www.kavousa.com). Because of varying needs between dentists and dental specialists, several manufacturers make different platforms with different fields of view (FOVs). Notably, dentists do not need to have a CBCT machine to avail themselves to the advantages of this technology. Since all manufacturers have at least some level of digital imaging and communications in medicine (DICOM) conformancy, the volume of data can be exported out of a CBCT system for use in third-party software. This capability has also helped to rapidly expand the adoption of CBCT.
Updated Information
While some new machines and many more platforms have entered the dental profession as a few machines have exited the marketplace, there are still only two types of image capture devices used with CBCT. The NewTom 3G (ImageWorks), the Galileos® (Sirona Dental Systems), and the MyRay SkyView (Cefla Dental Group) all still use an image intensifier (II) fixed to a charge coupled device (CCD). Other manufacturers use a flat-panel detector for image capture. Because most medicine fields are abandoning image intensification for tasks such as mammography and angiography due to the cost of replacement of the II unit, dentistry will probably follow suit and manufacturers of these units will likely adopt flat-panel detectors. When considering this technology clinicians should be aware that FOVs expressed in diameter (ie, of a circle) use image intensification; when FOVs are expressed in square centimeters (cm2), it means that the system’s receptor device is a flat-panel. Additionally, there has been a significant increase in the number of mobile CBCT systems. For example, the NewTom VGi Flex (ImageWorks) has been adapted for use in large vans.
While product manufacturers constantly look for competitive advantages, such as the “smallest voxel size on the market,” clinicians should know that image quality and spatial resolution are dependent on many parameters. These include focal spot size in the target anode, voxel size, receptor type, reconstruction algorithm, added filtration, kilovoltage and milliamperage specification, grayscale bit depth, and type of head positioner (to limit motion “noise”). Purchasing this technology requires due diligence and comparison shopping in earnest.
Applications and Benefits
There are a number of diagnostic tasks for which CBCT image data sets improve clinical decision-making or surgical planning. These include, though are not limited to, airway assessment, temporomandibular joint (TMJ) complex assessment, paranasal sinus assessment, periodontal bone architecture, endodontic assessment, implant site assessment, orthodontic assessment, surgical guide construction, implant placement, and third molar extraction assessment. Eventually, CBCT data sets could be used to create a virtual articulator using virtual models. Numerous articles in the literature support CBCT for these applications.2-4 Once more, the reader is urged to research the Internet for further supporting documentation.
In addition to the benefits to the clinician, patients receive the benefit of improved diagnostic information with a lower absorbed radiation dose than conventional CT. Thus, CBCT is now the preferred modality for implant site assessment rather than medical CT as used previously by “cutting-edge” implantologists simply due to the reduced x-ray dose.5 There is no need for medical CT use for dental implants. In addition, CBCT is being adopted by many otolaryngologists as their standard radiographic examination procedure. So too, if needed, CBCT can be used by dentists and dental specialists if evaluation of the paranasal sinuses is required for procedures like sinus lifts and grafts and evaluation of headache in the dental office if the paranasal sinus origin is suggested.
How to Integrate CBCT
CBCT devices can be easily integrated into a dental environment. Of course, the dental office must be sufficiently “digital” to integrate this new modality. Machines come with a workstation preloaded with software sold by the manufacturer. Depending on the tasks for which the machine will be used, clinicians may want to purchase and use additional third-party software. In addition, the file size of the data sets, while variable, is quite large relative to 2-dimensional (2-D) image sizes. CBCT volumes can range in size from 30 MB to more than 250 MB. This requires larger storage capacity within the dental office. Most clinicians who use the technology regularly depend on an office server or a set of servers with additional off-site storage for patient information. It may be wise to obtain the services of a dental integrator or information technology (IT) personnel to assist with the implementation.
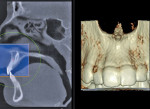
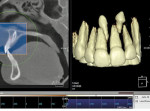
Finally, whether clinicians purchase or simply use the data from CBCT machines in their practice, it is important—perhaps imperative—that they obtain training beyond the manufacturer’s hands-on, in-office introduction. Until trained, a dentist or dental specialist is simply not used to seeing a patient image in the axial plane of section. These types of images, as well as the images in the coronal and sagittal planes and the anatomic data within them, must be mastered before a clinician can feel comfortable using CBCT (Figure 1, Figure 2, and Figure 3).
Because of this, the dentist should consider establishing a relationship with an oral maxillofacial radiologist to offer a second opinion or perhaps review the cases on an ongoing basis. This will reduce the dentist’s stress and potential liability.
Disclosure
The author serves as a consultant to Planmeca USA and CyberMed Inc.
References
1. Miles DA. Interpreting the cone beam data volume for occult pathology. Semin Orthod. 2009;15(1):70-76.
2. Miles DA, Danforth RA. A Clinician’s Guide to Understanding Cone Beam Volumetric Imaging (CBVI). Academy of Dental Therapeutics and Stomatology. PennWell Publications. 2007;(special issue):1-13.
3. Miles DA. Clinical experience with cone-beam volumetric imaging: report of findings in 381 cases. Touch Briefings. https://www.touchbriefings.com/pdf/2262/miles.pdf. 2006. Accessed September 27, 2011. Reprinted in J Modern Dentistry. 2008;4(3):35-42.
4. Miles DA. Color Atlas of Cone Beam Volumetric Imaging for Dental Applications. Hanover Park, IL: Quintessence Publishing; 2008.
5. Roberts JA, Drage NA, Davies J, Thomas, DW. Effective dose from cone beam CT examinations in dentistry. Br J Radiol. 2009;82(973):35-40.
About the Author
Dale A. Miles, BA, DDS, MS
Professor of Radiology
Arizona School of Dentistry & Oral Health
A.T. Still University
Mesa, Arizona
Adjunct Professor of Radiology
University of Texas
San Antonio, Texas