Enhancing the Gingival Frame With Periodontal Surgery
Albert B. Konikoff, DDS
Abstract: The creation of an esthetic smile is a collaborative process, which at a minimum involves the patient and restorative dentist. Often, however, the participation of other specialists is necessary to fulfill the patient’s expectations. This article explores the periodontist’s role in creating an optimal gingival frame: surgical crown lengthening and a modified subepithelial tissue graft to shorten the clinical crown are the treatments presented. These procedures are part of the periodontal plastic surgical armamentarium as these techniques rise to the highest levels of sophistication.
The evolution of dentistry to its present state has been remarkable. Once a mostly need-based, functional and health-driven treatment protocol, the field has now expanded to include—and even shift its focus to—cosmetic enhancement. This fundamental change has occurred as a result of dentists’ abilities to deliver the optimal result that both they and their patients desire. Thus, a new paradigm of treatment planning has developed. Once a multidisciplinary approach in which each specialist acted independently, the practice of dentistry has become interdisciplinary: treatment planning is a collaborative effort of each discipline’s talents and treatment protocols that will lead to a predictable, optimal result. Nowhere has this collaboration been stronger than with periodontics.
Periodontal therapy evolved as a means to re-establish the health of the periodontium. The mainstays were scaling and root planing, osseous surgery, and mucogingival surgery. The surgical therapy created a condition of health; however, dentists often overlooked the importance of cosmetics, noting that it was better to have longer teeth than no teeth. Or they would advised against worrying about roots showing because the thick band of tissue would prevent further gingival recession. However, these therapies, along with a blossoming interest in facial esthetics and smile enhancement, provided the basis for the development of more sophisticated and cosmetically driven procedures.
Periodontal plastic surgery encompasses many procedures that have been an integral part of periodontal therapy and whose goals were to establish or maintain health. However, the sophistication of the techniques and cosmetic bias of the enhancements have ushered in a new era. Periodontal plastic surgery includes cosmetic crown lengthening, connective tissue and dermal matrix grafting, frenectomies, color alterations, ridge augmentations, exposure of unerupted teeth, and papilla reconstruction.1 The impetus for the development and implementation of these enhancements arose from the realization that, despite the availability of new materials and artistry of the restorations, simply working within the limitations of the environment with which the patient presented often did not achieve the desired esthetic outcome. The need to have gingival tissues in an esthetic position became paramount to attaining the highest esthetic results.
This article will discuss the two periodontal plastic surgical procedures most commonly used to alter the gingival frame: cosmetic crown lengthening to increase the length of the clinical crown, and gingival augmentation to reduce the clinical crown length. To be predictable, these procedures need to have a sound biologic basis and a reproducible clinical protocol, and be performed in a healthy periodontal environment.
Cosmetic Crown Lengthening
Cosmetic crown lengthening is based on the same principles as functional crown lengthening. A biologic width from the osseous crest to the gingival margin must be established to accommodate the connective tissue attachment, junctional epithelium, and sulcular epithelium.2 The difficulty is evaluating these dimensions clinically, using traditional periodontal probing. On the histologic slide, it looks simple. The probe should stop at the most coronal extent of the junctional epithelium: this would provide the information needed to prevent violation of the biologic width (Figure 1). In actuality, probing measures the degree of penetrability of the connective tissue. The amount of inflammation determines how close to the bone the probe tip can be introduced (Figure 2). To eliminate this significant variable, bone sounding is used to evaluate the necessary dimensions. On average, this facial dimension is 3 mm but it can vary.3,4 Interproximally, due to the compressed state of the papilla, the dimension is greater, with 5 mm to the contact area being the most stable relationship.5 Encroachment on the connective tissue by the margin of the restoration can result in an inflammatory response, causing tissue proliferation and bleeding on probing in an average biologic width, and gingival recession in a tissue type with a greater-than-average connective tissue component to the biologic width (Figure 3). In clinical practice, the violations of biologic width that create the greatest problems seem to be those that occur interproximally. Although clinically the position of the soft tissues is the most easily discerned, their relationship to the bone is equally important.
Therefore, not only do the cosmetic demands of the case dictate the positions of the gingiva but the underlying osseous form must support this position. This allows the clinician to determine the most appropriate method to surgically lengthen the clinical crown. The quantity of gingival tissues and the osseous topography determine the surgical modality. In a normal relationship, the bone is 2 mm apical to the cementoenamel junction (CEJ) (Figure 4) and the gingival tissues cover the enamel by 1 mm. Departure from this normal osseous dimension must be considered when undertaking cosmetic corrections. If after removing the necessary gingival tissues, 3 mm of distance from the osseous crest to the gingival margin will exist and at least 3 mm of gingiva remains, then a gingivectomy with an internal or external bevel can be performed. A scalpel, bur, radiosurgery, or laser can be employed. However, after establishing the desired gingival form and a distance of less than 3 mm from the free gingival margin to the osseous crest results, the bony form needs modification (Figure 5).6-8 If removal of the necessary gingiva would result in less than 3 mm of gingiva remaining, a full-thickness flap to preserve the gingiva and to gain access to perform the necessary ostectomy and osteoplasty should be developed. Contouring the bony form can be accomplished with burs, hand instruments, or an Er,Cr:YSGG laser.9 Then, the flap is sutured using a continuous sling vertical mattress suture. The vertical mattress suturing technique is employed to reduce the flattening of the papillae to hasten the re-establishment of its normal form. Following suturing, the clinician should re-sound the facial and interproximal aspects to ensure that a 3 mm dimension is present; otherwise, the restorative dentist is at greater risk for biologic width violation. Complete maturation of the dentogingival complex always takes longer than expected. The author prefers to wait a minimum of 3 months before tooth preparation and recommends bone sounding during tooth preparation to aid in the determination of margin placement, particularly when periodontal surgical treatment has been performed.
The surgical aspect of cosmetic crown lengthening is the most straightforward. Placing the gingival tissues where desired is easy. The gingival height of the central incisors dominates and is identical. The gingival position of the lateral incisors is more variable—anywhere from equal, to 1 mm to 2 mm shorter than the central incisors, but never higher. The gingival height of the canine is then placed on the same plane as the central incisor.10,11 The diagnosis as to where the gingival frame needs to be and the successful transfer of that information provide more challenges. A reference is needed to accurately establish the placement of the new gingival frame. The position of the incisal edges is that reference, which must be determined and communicated before any surgical therapy.12 When the incisal edges are where they will be in the final restoration, or uniform additions or subtractions can be made to their lengths either in the natural teeth or a restoration that will be remade, they are readily used by the surgeon as is. If, for example, an 11-mm central incisor is desired, the osseous crest is placed 14 mm from the incisal edge. These measurements are established tooth-by-tooth and a very accurate result is achieved. In other instances (Figure 6), provisional restorations or diagnostic mock-ups (Figure 7) are used to determine the incisal edge position. Depending on the restorative dentist’s preference, the margins of the provisional restoration are placed at the pretreatment position, or using a laser or radiosurgery, gingival tissues are removed and soft-tissue crown lengthening performed (Figure 8 and Figure 9). This latter method often violates the biologic width; however, the surgeon only has to create a full-thickness flap and place the position of the bone 2.5 mm from the margin of the restoration facially and 4.5 mm from the margin interproximally. Alternatively, this can be done via a closed protocol employing chisels or an Er,Cr:YSGG laser if the bone is thin (Figure 9, Figure 10, Figure 11). The cosmetic advantage is no gap between the margin of the provisional restorations and gingiva. A third method is to establish the incisal edge position and then transfer the gingival position to the surgeon, using a guide (Figure 12, Figure 13, Figure 14). These protocols result in the creation of an esthetic gingival frame that fulfills the expectation of the patient and clinician (Figure 15 and Figure 16).
Gingival Augmentation
Gingival augmentation began with pedicle grafts,14 which evolved into free gingival grafts.15 The pedicle graft provided an esthetic result, sometimes at the expense of the donor tooth. However, many situations were not amenable to pedicle grafting due to the lack of adequate donor tissue. The free gingival graft evolved into a procedure that in most instances could cover denuded root surfaces; however, the cosmetic results were often less than optimal because of color mismatch.16 This changed with the introduction the connective tissue graft.
Connective tissue grafting was proposed in 198017,18 as an alternative to the free gingival graft. The benefits of this new procedure included reduced palatal discomfort as subepithelial tissues were used (replacing the excoriated palatal wound with a wound that would heal by primary intention) and the more predictable integration of the tissues into the surrounding tissues with regard to color and contour. The original procedure involved the use of vertical incisions to prepare a recipient site and to coronally advance the marginal tissue and cover the connective tissue. This often resulted in scarring, which detracted from the final result. When grafting multiple sites, loss of papillary height could also occur. Modifications were developed to reduce the scarring by first eliminating the vertical incisions while still separating the papillary tissues and then creating pouches or tunnels to insert the connective tissue.19,20 From a periodontal plastic surgical perspective, this latter modification produces the optimal result. The author has labeled this a minimally invasive subepithelial tissue (MIST) graft. This is minimally invasive because no external incisions are made on the facial surfaces, and the tissue harvested is not purely connective tissue but a mixture of connective tissue, fat, and minor salivary glands. With this procedure, the clinician is able to cover root surfaces with a high degree of predictability, if the interproximal tissues are in an appropriate position21 (Figure 17, Figure 18, Figure 19, Figure 20). Essentially, in this author’s experience, root surfaces can be covered to the length of the interproximal tissue complex coronal to the surface to be augmented. Exposures due to toothbrush abrasion, abfraction, or prominent teeth with thin tissue can be predictably covered once the etiologic factors are eliminated. Even teeth with restorations or decayed surfaces can be grafted once the restoration or decay is removed (Figure 21, Figure 22, Figure 23).
The procedure for the MIST graft is similar to other connective tissue grafting techniques. It begins with thorough scaling and root planing of the exposed root surfaces, although no attempt is made to plane the root to an extent that it is within the confines of the alveolus. The author uses tetracycline HCl for surface modification, applying it for approximately 30 secs per tooth. The pouch or tunnel is then created using blunt dissection. The dentist should ensure the dissection is sufficiently extensive both apically and laterally to enable the tissues to be coronally advanced to the CEJ. The donor tissue is harvested from the palate with a single straight line incision without including the epithelium.22 Then, this tissue is tucked into the pouch or tunnel and secured to the papillae with interrupted 5-0 gut sutures (Figure 24). No attempt is made to cover the subepithelial tissue. With the extensiveness of the dissection used, even with significant recession, a minimal area of exposed subepithelial tissue is present. Then, this tissue is covered with ß-cyanoacrylate. No periodontal dressing is employed. The tissues mature in 7 to 10 days, after which the donor tissue is indistinguishable from the adjacent tissues.
MIST grafting can also be used around dental implants, as long as the interproximal tissues support the facial tissues. The greatest challenge is that often the interproximal tissues are deficient. Correcting these potential problems prior to implant placement is the most predictable approach.
Other modalities, such as the intrusion and extrusion of teeth with orthodontic therapy, should be considered when patients are already receiving orthodontic treatment. When orthodontics would eliminate the need for restorative treatment or when the root form is narrow and surgical crown lengthening would create too much of a tapered form, orthodontic therapy should be employed.
Conclusion
Cosmetic crown lengthening and MIST grafting can address many gingival frame issues. Having the choice of these and other procedures enables clinicians to realize the expectations of both patients and themselves. Dentists simply need to observe and open their minds to all possibilities. Morton Amsterdam astutely said, “There may be different ways of treating a disease (problem), but there can be only one correct diagnosis.”23
References
1. Miller PD Jr. Concepts of periodontal plastic surgery. Pract Periodontics Aesthet Dent. 1993;5(5):15-22.
2. Gargiulo AW, Wentz FM, Orban B. Dimensions and relations of the dentogingival junction in humans. J Periodontal. 1961;32:261-267.
3. Kois J. Altering gingival levels: the restorative connection. Part I: biologic variables. J Esthetic Restorative Dent. 1994;6(1):3-9.
4. Vacek JS, Gher ME, Assad DA, et al. The dimensions of the human dentogingival junction. Int J Periodont Res Dent. 1994;14(2):154-165.
5. Tarnow DP, Magner AW, Fletcher P. The effect of the distance from the crest of bone on the presence or absence of the interproximal papilla. J Periodontol. 1992;63(12):995-996.
6. Allen EP. Surgical crown lengthening for function and esthetics. Dent Clin North Am. 1993;37(2):163-179.
7. Rosenberg ES, Garber DA, Evian CI. Tooth lengthening procedures. Compend Contin Educ Dent. 1980;1(3):161-173.
8. Kay HB. Esthetic considerations in the definitive periodontal prosthetic management of the maxillary anterior segment. Int J Periodontics Restorative Dent. 1982;2(3):44-59.
9. Lowe RA. Clinical use of the Er,Cr: YSGG laser for osseous crown lengthening: redefining the standard of care. Pract Proced Aesthet Dent. 2006;18(4):S2-S9.
10. Rufenacht CR. Fundamentals of Esthetics. Chicago, IL: Quintessence Publishing; 1990
11. Garber DA, Salama MA. The aesthetic smile: diagnosis and treatment. Periodontol 2000. 1996;11:18-28.
12. Spear FM, Kokich VG, Mathews DP. Interdisciplinary management of anterior dental esthetics. J Am Dent Assoc. 2006;137(2):160-169.
13. Spear FM. Construction and use of a surgical guide for anterior periodontal surgery. Contemp Esthet and Restor Pract. 1999;4:12-24.
14. Grupe H, Warren R. Repair of gingival defects by sliding flap operations. J Periodontol. 1956;27(2):92-99.
15. Nabers CL. Free gingival grafts. Periodontics. 1966;4:243-245.
16. Miller PD Jr. Root coverage using a free soft tissue autograft following citric acid application. Part 1: technique. Int J Periodont Rest Dent. 1982;2(1):65-70.
17. Langer B, Calagna L. The subepithelial connective tissue graft. J Prosthet Dent. 1980;44(4):363-367.
18. Langer B, Langer L. Subepithelial connective tissue graft for root coverage. J Periodontol. 1985;56(12):715-720.
19. Raetzke PB. Covering localized root exposure employing the “envelope” technique. J Periodontol. 1985;56(7):397-402.
20. Allen AL. Use of supraperiosteal envelope in soft tissue grafting for root coverage. II. Clinical results. Int J Periodontics Restorative Dent. 1994;14(4):302-315.
21. Miller PD Jr. Classification of marginal tissue recession. Int J Periodontics Restorative Dent. 1985;5(2):8-13.
22. Lorenzana ER, Allen EP. The single-incision palatal harvest technique: a strategy for esthetics and patient comfort. Int J Periodontics Restorative Dent. 2000;20(3):297-305.
23. Amsterdam, M. Periodontal prosthesis: twenty-five years in retrospect. Alpha Omegan. 1974;67(3):8-52.
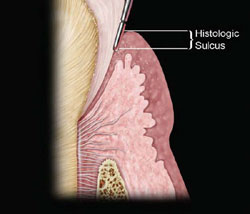 Figure 1 Ideal conception of probing. | 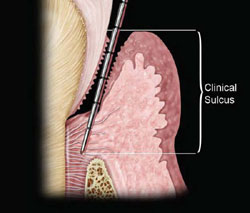 Figure 2 Actual probe penetration based on inflammation. | ||||||
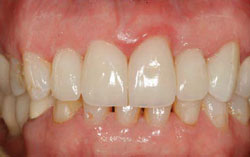 Figure 3 Biologic width violation resulting in inflammation and hyperplasia. | 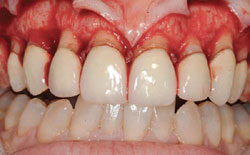 Figure 4 Normal bone to CEJ dimension. | ||||||
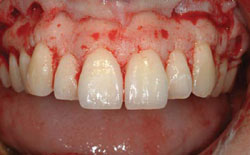 Figure 5 Bone has not moved apically to create normal bone to CEJ dimension. | 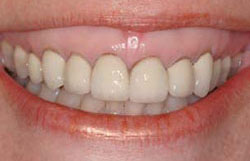 Figure 6 Patient with vertical maxillary excess not considering orthognathic surgery. | ||||||
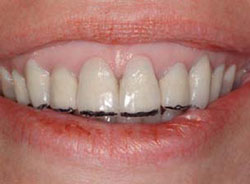 Figure 7 Mock-up to determine incisal length and gingival extent of restorations. | 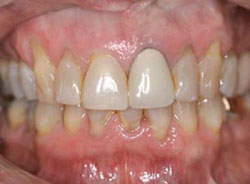 Figure 8 Preoperative view of another patient. Notice recession and need for adjusting gingival of teeth Nos. 8 and 9. | ||||||
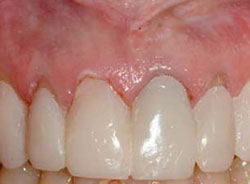 Figure 9 Provisionals placed with soft-tissue removal of teeth Nos. 8 and 9.Margins of provisionals allow for placement of MIST grafts. | 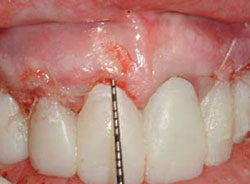 Figure 10 Probe demonstrates need for creation of adequate biologic width. | ||||||
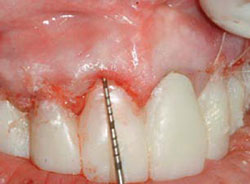 Figure 11 Acceptable biologic width established. | 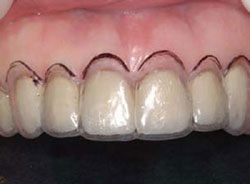 Figure 12 Surgical guide placed in the first patient seen in Figures 6-7. | ||||||
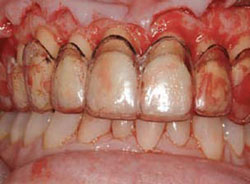 Figure 13 Relation of bone to surgical guide to ensure adequate osseous recontouring. | 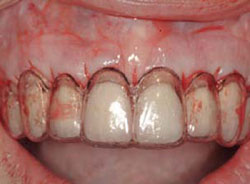 Figure 14 Surgical guide for final gingival position. | ||||||
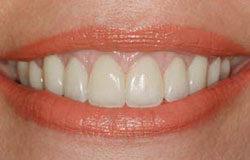 Figure 15 Eighteen months postoperative view of the patient seen in Figures 6-7 and Figures 12-14. Restoration by Dr. Robert Korman,Virginia Beach,Virginia. | 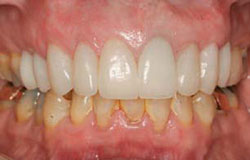 Figure 16 Final result with creation of esthetic gingival frame of the patient seen in Figures 8-11 and Figure 24. Restoration by Dr. John Cranham,Virginia Beach,Virginia. | ||||||
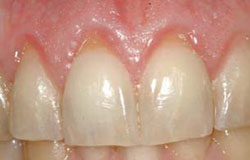 Figure 17 Prereoperative view of another patient. Note recession of teeth Nos. 7, 8, and 9. | 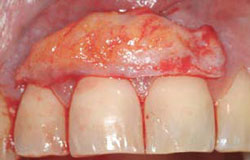 Figure 18 Size of subepithelial tissue. | ||||||
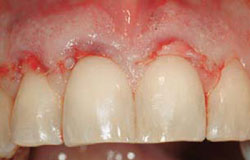 Figure 19 Tissue in place and sutured. | 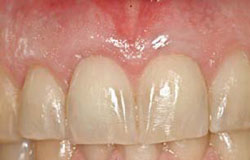 Figure 20 Six months postoperative view with roots fully covered. | ||||||
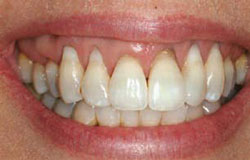 Figure 21 Preoperative view. Note the presence of the restorations. | 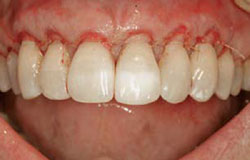 Figure 22 Restorations on root removed, leaving restoration where enamel would be. | ||||||
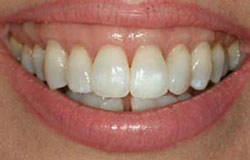 Figure 23 Postoperative view with complete root coverage. | 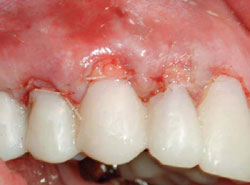 Figure 24 MIST graft in place for patient seen in Figures 8-11 and Figure 16. | ||||||
| |||||||




