Treating the Edentulous Patient with Dental Implant Therapy: A Review of Treatment Considerations
Karen S. McAndrew, DMD, MS
Functionally challenged edentulous patients benefit greatly from treatment options beyond simple tooth replacement. Severe bone resorption renders these patients unable to wear comfortable and serviceable prostheses, limiting function, and adding to a loss of confidence and reduction of social interaction. Their options range from conventional dentures to the complex fixed implant-supported restoration. Successful outcomes depend on proper and adequate treatment planning and a comprehensive team approach.1
Currently, the percentage of completely edentulous patients is declining 10% each decade; however, this is more than offset by the growth of the aging baby boomer population. In reality, an increase in the numbers of completely edentulous cases is being observed. By 2020, an estimated 37.9 million patients will present with one or both fully edentulous arches. According to the National Institute of Health, most of these patients visit their dentist every 14 years, a schedule not conducive to proper maintenance for ensuring properly fitting and functional prostheses.
The problems of edentulism and tooth loss are far more encompassing than just a limitation in function. These issues present many psychosocial implications in patients, such as the fear of aging, social inhibition, and diminished self image. Dental implants not only replace missing teeth and restore functionality and esthetics but also improve confidence and social interaction.2 They also re-establish speech and mastication as well as maintain bone.3 Treatment with dental implants requires not only a comprehensive understanding of dental implant therapy but also a complete mastery of removable prosthodontic principles and techniques. Regardless of the desired restorative outcome, complete capture of the edentulous ridge morphology and anatomy during impression making, assessment of the vertical dimension of occlusion, and proper tooth arrangement with attention to occlusal schemes and biomechanics must be well understood and executed. In addition, it is imperative to achieve optimal esthetics, phonetics, and mastication.1
This article provides an overview of the various restorative options for both the maxilla and mandible, and describes the various dental materials and their benefits that support these restorative options. Approach and treatment is much different for restoration of the maxilla and mandible. Selection of materials and prosthesis design is contingent on many factors. Clinically, assessment of the edentulous ridge anatomy, intra- and interarch spaces, smile line, and need for lip support will aid in determining the optimal prosthetic choice. The opposing dentition, parafunction, and biomechanical loading of the dental implant prostheses also must be considered.
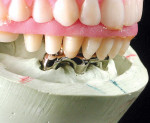
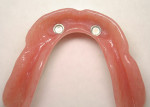
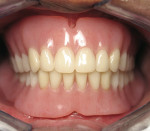
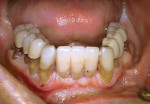
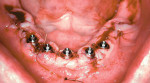
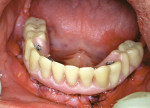
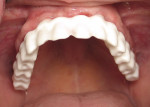
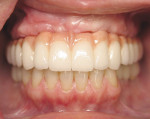
The clinician must understand and identify each patient’s anatomic limitations. An anatomic classification system accounts for the ridge morphology, amount of bone height, muscle attachments, bone shape, and arch form of each edentulous ridge.4 Anatomic relationships between the edentulous ridges will determine the success of the prostheses and establish the need for surgical enhancement and/or preprosthetic surgery. The fabrication of implant prostheses for the edentulous patient must include consideration for the need for adequate space for the implant components, as well as the appropriate restorative material (Figure 1A, Figure 1B, Figure 1C, Figure 1D). This space is not always adequate, and vertical height of bone may need to be removed to facilitate the space requirements for the given prosthesis. It is necessary to account for a larger amount of interarch space to accommodate for the restorative components and prosthetic materials needed to restore the edentulous arch. Fixed restorations need > 10 mm as measured from the soft tissue to the opposing dentition while 12 mm to15 mm of space is minimally required for restoration of an overdenture depending on the type of attachments or substructure utilized in the restorative design.5
The appropriate desired tooth position must be determined to plan treatment of the implant placement. A diagnostic wax-up should be completed and verified intraorally to determine the area that the implant prosthetics must fit within for proper esthetics and function. A surgical guide will then co-localize the implant placement with the desired tooth position.
The maxilla and mandible present very different surgical and restorative challenges because of bone quality and quality, ridge morphologic and resorptive patterns, location of anatomic structures, and biomechanical considerations. With that said, there are two primary ways to restore the edentulous case. The selection of a fixed vs removable prosthesis is based on many factors. Influencing this decision is patient preference, cost, and ease of maintenance, as well as the clinical considerations of anatomy, bone quantity, quality, and arch form. The predictability of the long-term success of the prosthesis depends on design fabrication and material selection.
Numerous restorative options, materials, and techniques are used in dental implant therapy for edentulous cases (Table 1). The biomechanical considerations must be weighed. The lack of periodontal fibers surrounding an implant alters the proprioceptive feedback for the completely edentulous patient who has restorative dental implants. This may result in a greater incidence of material fatigue and fracture. Materials should be selected while keeping in mind that bite force has been found to be as much as three times greater for the edentulous case restored with dental implants when compared with a dentate case.6 Complications such as porcelain and acrylic fracture and loss of denture teeth are common in the completely edentulous patient restored with dental implant therapy.7
Maxilla
Removable
Frequently, because of the resorptive pattern observed in the premaxilla, both hard and soft tissue is lost following loss of the teeth. This necessitates replacing this lost tissue on the vertical and horizontal planes to restore proper function and esthetics. One of the key advantages of a removable prosthesis in the maxilla is the ability to use the denture flange for lip support without the compromise that may be seen with a fixed prosthesis that can hamper patient home care. A maxillary prosthesis requires a splinted metal bar substructure to facilitate removal of the prosthesis palate and provide for retention as well as support. Currently, no literature supports a removable prosthesis in the maxilla with free-standing attachments.8
Fixed
Often, the bone in the maxilla has been grafted because of insufficient vertical height and/or horizontal width. A successful maxillary prosthesis provides for a splinted restoration, providing cross-arch stabilization, and accounts for significant esthetic requirements. On occasion, a reduction in vertical height is needed in patients with a higher lip line to conceal the junction of the prosthesis and gingiva underneath the lip line.
Mandible
Removable
Loss of the posterior teeth and the resorption that ensues often creates height issues above the inferior alveolar nerve, making implant placement complex or impossible without extensive grafting or nerve repositioning. The primary area for dental implant placement is in the anterior mandible between the mental foramen. The McGill Consensus Statement on Overdentures solidified the importance of dental implant therapy in the mandible and advocated two dental implants “as a minimal treatment objective.”9
Fixed
The success of a fixed restoration in the mandible is often determined by arch form. Maximizing anterior-posterior spread allows for a bilateral distal cantilever and a fixed restoration typically to the first molar.10 Predictability for success is high in the anterior mandible, irrespective of implant type, surface topography, and prosthesis design with success rates reported as 90%-100%.11
Immediate Placement/Immediate Load Dental Implants
Treatment protocols have been predictably enhanced with immediate placement of dental implants at the time of tooth extraction and immediate load and restoration of the implants during their placement (Figure 2A, Figure 2B, Figure 2C). This enables the preservation of bone and soft-tissue morphology while significantly shortening the treatment completion time. Adherence to these protocols (Table 2)helps ensure the success of the implant fixtures. Loading of these implants has many benefits (Table 3) with predictable long-term results. However, understanding the risks (Table 4) could help prevent failure of the fixture and/or prosthesis.11
CT Imaging and Computer-Generated Planning via Software Imaging Systems
State-of-the-art implant planning uses computer-generated software to “virtually” plan the implant placement via 3-dimensional imaging of the patient’s edentulous ridge, including an image of a denture representing an ideal denture set-up of desired tooth position. Once the dental implant planning has co-localized the desired planning with the planned prosthetic tooth placement, a surgical guide can be fabricated to aid in the actual placement of the dental implants. In some cases, these implants can be immediately loaded at the time of surgical placement. Traditional cast gold frameworks can be used to fabricate these fixed restorations with veneered porcelain or acrylic with denture teeth. More recently, CAD/CAM milled frameworks are being used which overcome all the negatives found in cast structures such as framework distortion during casting and need to have solder or laser joints and provide stronger solid frameworks. Improvements in dental materials now allow fabrication of these prostheses with zirconia substructures and veneered porcelain (Figure 3A, Figure 3B, Figure 3C) or titanium frameworks with acrylic and denture teeth.
Conclusion
Treating edentulous cases with dental implants can be rewarding, providing possibly the highest levels of patient satisfaction. Restoration of esthetics, function, and self confidence while enhancing the biologic benefits of bone preservation are a few of the reasons that patients pursue dental implant therapy. However, the determination of the success of a given prosthesis is established by many clinical, restorative material, and biomechanical considerations. Comprehensive treatment planning will aid in the execution of functionally predictable prostheses.
Disclosure
The author is a lecturer for Nobel Biocare.
Acknowledgement
Laboratory work and prostheses fabrication was performed by Bay View Dental Laboratory in Chesapeake, Virginia.
References
1. Mericske-Stern RD, Taylor TD, Belser U. Management of the edentulous patient. Clin Oral Impl Res. 2000:11(suppl 1):108-125.
2. Misch CE. Contemporary Implant Dentistry. St. Louis, MO: Mosby; 1999:175-192.
3. Albrektsson T, Zarb GA, Worthington P, Eriksson AR. The long-term efficacy of currently used dental implants: a review and proposed criteria of success. Int J Oral Maxillofac Implants 1986;1(1):11-25.
4. McGarry TJ, Nimmo A, Skiba JF, et al. Classification system for complete edentulism. The American College of Prosthodontics. J Prosthodont. 1999;8(1):27-39.
5. Zitzmann NU, Scharer P. Oral Rehabilitation with Dental Implants. Clinical Compendium. Vol. 3. University of Zurich, Switzerland, Department of Fixed and Removable Prosthodontics and Dental Material Sciences; 1997:81-110.
6. Mericske-Stern R. Oral tactile sensibility recorded in overdenture wearers with implants or natural roots: a comparative study. Int J Oral Maxillofac Implants. 1994;9(1):63-70.
7. Zarb G, Lekholm U, Albrektsson T, Tenenbaum H. Aging, Osteoporosis, and Dental Implants. Chicago, IL: Quintessence; 2002:156.
8. Cavallaro JS Jr, Tarnow DP. Unsplinted implants retaining maxillary overdentures with partial palatal coverage: report of 5 consecutive cases. Int J Oral Maxillofac Implants. 2007;22(5):808-814.
9. Fiene JS, Carlsson GE, Awad MA, et al. The McGill consensus statement on overdentures. Mandibular two-implant overdentures as first choice standard of care for edentulous patients. Int J Prosth. 2002;15(4):413-414.
10. Engelman M. Clinical Decision Making and Treatment Planning in Osseointegration. Chicago, IL: Quintessence; 1996.
11. Attard NJ, Zarb GA. Immediate and early implant loading protocols: a literature review of clinical studies. J Prosthet Dent. 2005;94(3):242-258.
About the Author
Karen S. McAndrew, DMD, MS
Private Practice
Richmond, Virginia