Fixed Restorative Options for the Edentulous Maxilla
Aldo Leopardi, BDS, DDS, MS
Abstract
Patients with an edentulous maxilla can be treated with conventional removable prosthetics or implant therapy. Implant prosthetic options can be removable, in the form of overdenture therapy, or fixed. The surgical approaches, implant systems, and prosthetic designs vary significantly. Consequently, the choices for the restorative–surgical team are numerous. This article presents an overview of the maxillary edentulous conditions and how implant therapy impacts on the possible restorative solutions. Various fixed treatment approaches are discussed, as well as guidelines for prosthetic reconstruction.
Dental implant therapy has revolutionized the treatment possibilities for the edentulous condition. The edentulous patient with good maxillary bone support often can be restored to the patient's satisfaction with conventional complete denture therapy.1 However, in those individuals who have a significant atrophic condition and associated chronic prosthetic problems, implant therapy has the potential to provide the patient with improved function, esthetics, taste, and self-esteem, well beyond what conventional removable prosthetics have been able to achieve.1-4
Patients motivated to pursue fixed implant therapy for an edentulous maxilla usually present with a significant atrophic condition. In the Cawood and Howell classification of edentulous atrophy in the maxilla, a class IV jaw requires bone augmentation to allow for implant placement.5 Invariably, posterior sinus regions are significantly pneumatized and, anterior to the sinus, bone ridges may be adequate in height but deficient in width.3 Fortunately, it is possible to prepare implant sites for future therapy with bone and soft-tissue surgical augmentation techniques. These procedures include (but are not limited to): sinus graft, onlay and/or interpositional bone graft, alveolar osteotomies, and distraction osteogenesis.3,6-10 Other surgical approaches include the placement of implants into residual anatomic structures without the need for additional significant bone augmentation, zygomatic implants, and implants in the canine eminence and/or in the pterygomaxillary region.11-14
Restorative Solutions
Restorative implant solutions for the edentulous maxilla can be divided into two main groups: removable (overdenture therapy) and fixed. The advantages of overdenture implant therapy include: open palate, increase in bite force, and improved retention, esthetics, and phonetics.1,2 However, postinsertion complications associated with overdenture therapy have been reported to be significantly higher than those with implant-supported fixed prostheses, particularly during the first 12 months after prosthetic delivery. Problems have included mechanical issues, mucosal complications, and poor patient compliance in nocturnal prosthesis removal.15-20
Fixed prosthetic treatment options can vary significantly, depending on available bone volume, augmentation needs, implant system chosen, desired prosthetic design, surgical–prosthetic team experience, and patient expectations; the permutations are numerous. Consequently, for the purpose of discussion, the prosthetic options available will be broken down into the number of implants and/or system-specific fixed concepts currently available, followed by prosthetic material selection.
Four to Six Dental Implants
The use of tilted implants with delayed loading or the All-on-4™ Brånemark System® technique (Nobel Biocare USA LLC, Yorba Linda, CA) has been reported in the literature as a viable treatment option for the completely edentulous maxilla, minimizing the need for significant additional sinus grafting.21-25 The zygomatic implant, intended for anchorage in the zygoma, was designed with a 45° prosthetic platform. This implant is indicated for patients with moderate to severely resorbed maxillae and has been documented to be successful in supporting fixed maxillary prostheses.11,12,26,27 These posterior zygomatic implants are used in conjunction with two to four anterior conventional root-form dental implants with splinted crossarch support. With this concept, treatment can be in the form of a conventional delayed/two-stage approach or immediate function when patient criteria selection allow.11,28 The prosthesis is often in the form of a fixed-detachable, crossarch splinted, acrylic-fused-to-metal design. The disadvantage with this approach is that it is implant-system specific and technique-sensitive. The final position of the zygomatic implant platform is often palatal to the residual ridge crest, complicating the design and fabrication of the prosthesis. Recent advances in the surgical technique, such as the sinus slot technique, have helped to improve final implant positioning closer to the first molar central ridge crest.13,29
Six to Eight Dental Implants
When six to eight conventional root-form titanium dental implants are placed, they can be distributed broadly from anterior to posterior, minimizing the need for cantilevers. Biomechanically, cantilevers tend to increase the loads on terminal implants by three times.30 To allow for a wide anteroposterior distribution of implants, grafting of the posterior pneumatized sinus regions is required. Longitudinal retrospective studies have shown the implant survival rate in atrophic maxillae augmented with sinus grafts, using a variety of materials and techniques to be high: 80% to 90% success rate at integrating dental implants of at least 10 mm in length.31-35 Consequently, this provides the clinical team (restorative dentist and surgeon) the ability to choose a nonspecific implant system for the rehabilitation of eden-tulous patients. The disadvantages include an additional augmentation surgery and increased treatment time.
Location/positioning of the implants will vary depending on arch size/shape, final tooth position, available bone, and minimization of adverse prosthetic cantilevers. Whenever possible, a wide spread of implants is recommended.30,36 The advantage of planning for eight dental implants is that should one or more fail during the integration/restorative phase, sufficient implants often remain for the restoration of the case. In a 15-year follow-up study on 76 consecutive patients treated with fixed prostheses in the edentulous maxilla, most implant failures occurred before loading and during the first year of function.37
The restorative solution is usually in the form of a hybrid, fixed-detachable design. These restorations replace both teeth and missing hard/soft tissue, especially in the esthetic zone and buccal corridors. Additional implants would allow for more conventional fixed implant crown-and-bridge dentistry. However, conventional fixed prosthetics, splinted or nonsplinted, are only applicable in maxillae with minimal bone and soft-tissue loss and/or when significant successful bone/soft-tissue augmentation has been achieved and also when financial considerations allow. Considering that most patients presenting with the edentulous condition have an atrophy of the maxilla, the hybrid approach to replace missing teeth and soft-tissue profiles (prosthetic alveolar reconstruction) will prove to be the most feasible providing a cost-effective, functional, and esthetic outcome.
Restorative Design Options
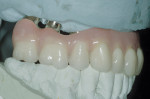
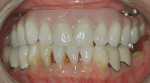
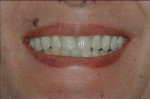
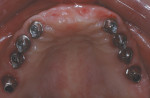
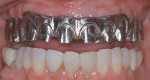
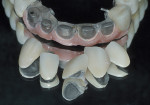
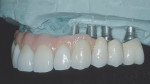
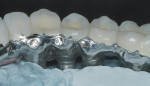
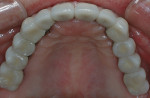
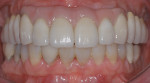
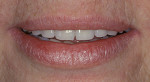
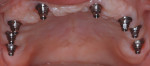
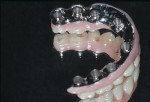
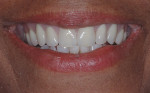
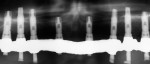
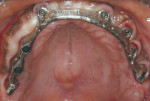
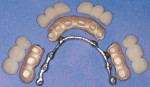
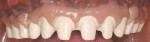
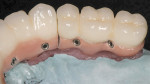
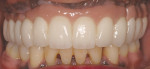
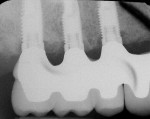
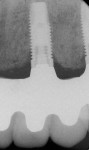
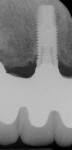
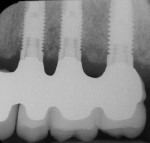
Designs can vary significantly depending on patient expectations and cost considerations. The four cases illustrated highlight the various design options (Figure 1A, Figure 1B, Figure 1C, Figure 1D, Figure 1E and Figure 4J).
Fixed prostheses for the edentulous maxillary arch can be divided according to material selection into three main groups: (1) acrylic-fused-to-metal/gold; (2) porcelain-fused-to-metal/gold; and (3) all-ceramic. The restorations can be fabricated in the traditional fashion by a trained dental technician, or in association with available computer-aided design/computer-aided manufacture (CAD/CAM) systems (computer-milled titanium or zirconium substructures).
Regardless of the type of prosthetic, recommended design features should be used to maximize the successful treatment outcome for the patient. These include (but are not limited to):
- Intaglio anterior-modified ridge-lap design and convex surfaces, from region 5 to 12 for oral hygiene and phonetic seal.
- Posterior interimplant/teeth/pontic sleuth ways for oral hygiene access.
- Crossarch stabilization.
- Group function occlusion.
- Retrievability for maintenance.
To provide a phonetic seal, it is advantageous to minimize air-escape under the prosthesis. However, the ability to access the intaglio region for oral hygiene is the overriding factor dictating the intaglio design of the prosthesis. Consequently, aggressive ridge-lap features (buccal-lingual) are contraindicated. Therefore, a modified ridge lap is recommended (Figure 1A, Figure 1B, Figure 2D, Figure 2E, and Figure 3B). Posteriorly, interimplant sleuth ways and/or wide gingival embrasure spaces can be incorporated to allow for the use of interproximal oral hygiene aids and floss (Figure 1B). The disadvantage of providing oral hygiene access is the potential for air-escape during speech. It may take time for the patient to learn to redirect airflow to the anterior and speak to his or her satisfaction.38 The time needed to relearn speech nuances varies from patient to patient. However, most, if not all, patients regain a level of speech that is satisfactory to them. This is a disadvantage with the maxillary fixed hybrid prostheses that needs to be discussed, with informed consent given, before the commencement of treatment.
Considering off-axis loading/forces are to be minimized,30 a group function occlusal scheme is recommended (Figure1C, Figure 2H, and Figure 4E). When a class II maxillomandibular relationship with associated deep anterior overbite is present, anterior guidance is unavoidable. In these situations, crossarch stabilization is recommended to maximize stress distribution under function to the underlying dental implants.
Where possible, crossarch stabilization generally is recommended.37 However, if implant anteroposterior spread is maximized, crown-to-implant ratio favorable, and parafunctional habits minimal, the prosthesis can be fabricated into various splinted sections (for example, one anterior and two posterior segments).
Abutment selection can be either in the form of available transmucosal abutments: straight/angled (Figure 3A), and/or custom: segmented (Figure 2A) or nonsegmented.39 Transmucosal abutments raise the prosthetic working platform from implant level to gingival crest/supercrestal. Superstructure adaption/fit, therefore, readily can be verified visually and/or radiographically. Soft-tissue impingement during try-in also is minimized. Custom abutments can be used for retrievable or conventional cement-on-prosthesis designs. When implant angulations allow, custom abutments can be fabricated in a one-piece nonsegmented design for conventional occlusal screw access. If occlusal esthetics are to be optimized, and/or implant angulations are to be accommodated, lingual-set screw options also are available (Figure 2F and Figure 4D).
All available prosthetic options will require ongoing maintenance and repair as problems occur. Considering the significant patient investment in time, surgery, and cost, the author recommends retrievable over cement-on designs.
Both acrylic and porcelain options have advantages and disadvantages. Advantages of acrylic-fused-to-metal designs include (but are not limited to): reduced overall prosthetic cost, replacement of teeth and missing hard/soft tissue contours with pink acrylic, and ease of repair/maintenance. Disadvantages include: stain of acrylic teeth/pink gingival areas, resin veneer fractures, and wear over time.37 Wear can be significant. Acrylic teeth require replacement on average every 7 to 10 years, depending on patient habits and parafunctional activity.
Porcelain restorations have the potential to achieve optimal esthetics, with minimal stain and wear resistance. These restorations, therefore, have the potential for longer intraoral lifespan, without the need for complete teeth replacement every 7 to 10 years, as with acrylic designs. However, porcelain is brittle and subject to fracture under function. Maintenance, therefore, needs to be a consideration in prosthetic design. As discussed above, retrievability is an advantage. One option is to construct a subframe with individual tooth preparations that will allow the attachment of individual crowns or splinted crowns (Figure 2B and Figure 2C). If one unit fractures, the clinician has the option of sectioning/removing the failed unit/crown, and then impressing the superstructure for the construction of a new restoration in the conventional manner. Other options include the fabrication of porcelain laminate veneers/onlays to repair fractured porcelain surfaces.
Use of a 2° milled bar subframe, as developed for overdenture therapy, also can be used in a fixed design. The milled bar supports three or more sections of superstructure restorations. These restorations are secured to the milled bar via multiple lingual set-screws (minimum of one screw per implant) (Figure 4A and Figure 4B). The advantage of this concept is that should one or multiple units fail/fracture, these sections can be removed readily, repaired extraorally, and reinserted for conventional impression techniques and provisionalization. Figure 4B shows the individual segments used for the prosthetic. The superstructure is opaqued (Figure 4B and Figure 4C) to allow for the placement of bonded, esthetic, pressed all-ceramic restorations. After bisque-bake try-in procedures, the restorations are bonded to the superstructure and the prostheses polished, ready for delivery (Figure 4D through Figure 4F).
The most significant disadvantage of porcelain restorations is cost. Resin options represent a lower prosthetic entry cost for the patient.34 However, when considering that resin teeth will require replacement every 7 to 10 years, and depending on the overall lifespan of the patient, the total investment for the patient may eventually approximate a porcelain restoration and the maintenance associated with it.
Conclusion
Restoration of completely edentulous atrophic maxillae can be facilitated with fixed solutions using multiple dental implants for support. Prosthodontic restorative solutions vary significantly, depending on the implant system chosen and experience of the restorative–surgical team. Considering the many available techniques and methods for fabrication, no one design can be recommended. Consequently, this article presented design-feature guidelines, which can be incorporated into the definitive prosthetic to maximize successful treatment outcomes for patients with an edentulous maxillary condition.
References
1. de Albuquerque Júnior RF, Lund JP, Tang L, et al. Within-subject comparison of maxillary long-bar implant-retained prostheses with and without palatal coverage: patient-based outcomes. Clin Oral Implants Res. 2000;11(6):555-565.
2. Henry PJ. Future therapeutic directions for management of the edentulous predicament. J Prosthet Dent. 1998;79(1):100-106.
3. Jensen OT, Leopardi A, Gallegos L. The case for bone graft reconstruction including sinus grafting and distraction osteogenesis for the atrophic edentulous maxilla. J Oral Maxillofac Surg. 2004;62(11):1423-1428.
4. Zitzmann NU, Marinello CP. Treatment outcomes of fixed or removable implant-supported prostheses in the edentulous maxilla. Part I: patients' assessments. J Prosthet Dent. 2000;83(4):424-433.
5. Cawood JI, Howell RA. A classification of the edentulous jaws. Int J Oral Maxillofac Surg. 1988;17(4):232-236.
6. Jensen OT, Cockrell R, Kuhlke L, et al. Anterior maxillary alveolar distraction oteogenesis: a prospective 5-year clinical study. Int J Oral Maxillofac Implants. 2002:17(1):52-68.
7. Isaksson S, Alberius P. Maxillary alveolar ridge augmentation with onlay bone-grafts and immediate endosseous implants. J Craniomaxillofacial Surg. 1999;20(1):2-7.
8. Rasmusson L, Meredith N, Cho IH, et al. The influence of simultaneous versus delayed placement on the stability of titanium implants in onlay bone grafts. A histologic and biomechanic study in the rabbit. Int J Oral Maxillofac Surg. 1999;28(3):224-231.
9. Waite PD, Sastravaha P, Lemons JE. Biologic mechanical advantages of 3 different cranial bone grafting techniques for implant reconstruction of atrophic maxilla. J Oral Maxillofac Surg. 2005;63(1):63-67.
10. Widmark G, Andersson B, Carlsson GE, et al. Rehabilitation of patients with severely resorbed maxillae by means of implants with or without bone grafts: a 3- to 5-year follow-up clinical report. Int J Oral Maxillofac Implants. 2001;16(1):73-79.
11. Bedrossian E, Stumpel L, Beckely M, et al. The zygomatic implant: preliminary data on the treatment of severely resorbed maxillae. A clinical report. Int J Oral Maxillofacial Implants. 2002;17(6):861-865.
12. Schmidt BL, Pogrel MA, Young CW, et al. Reconstruction of extensive maxillary defects using zygomaticus implants. J Oral Maxillofac Surg. 2004;62(9 Suppl 2):82-89.
13. Peñarrocha M, García B, Martí E, et al. Rehabilitation of severely atrophic maxillae with fixed implant-supported prostheses using zygomatic implants placed using the sinus slot technique: clinical report on a series of 21 patients. Int J Oral Maxillofac Implants. 2007;22(4):645-650.
14. Balshi TJ, Wolfinger GJ, Balshi SF 2nd. Analysis of 356 pterygomaxillary implants in edentulous arches for fixed prosthesis anchorage. Int J Oral Maxillofac Implants. 1999;14(3):398-406.
15. Ekfeldt A, Johansson LA, Isaksson S. Implant-supported overdenture therapy: a retrospective study. Int J Prosthodont. 1997;10(4):366-374.
16. Jemt T, Book K, Lindén B, et al. Failures and complications in 92 consecutively inserted overdentures supported by Brånemark implants in severely resorbed edentulous maxillae: a study from prosthetic treatment to first annual check-up. Int J Oral Maxillofac Implants. 1992;7(2):162-167.
17. Widbom C, Söderfeldt B, Kronström M. A retrospective evaluation of treatments with implant-supported maxillary overdentures. Clin Implant Dent Relat Res. 2005;7(3):166-172.
18. Sadowsky SJ. Treatment considerations for maxillary implant overdentures: a systematic review. J Prosthet Dent. 2007;97(6):340-348.
19. Naert I, Gizani S, van Steenberghe D. Rigidly splinted implants in the resorbed maxilla to retain a hinging overdenture: a series of clinical reports for up to 4 years. J Prosthet Dent. 1998;79(2):156-164.
20. Watson RM, Jemt T, Chai J, et al. Prosthodontic treatment, patient response, and the need for maintenance of complete implant-supported overdentures: an appraisal of 5 years of prospective study. Int J Prosthodont. 1997;10(4):345-354.
21. Fortin Y, Sullivan RM, Rangert BR. The Marius implant bridge: surgical and prosthetic rehabilitation for the completely edentulous upper jaw with moderate to severe resorption: a 5-year retrospective clinical study. Clin Oral Implants Relat Res. 2002;4(2):69-77.
22. Malo P, Rangert B, Nobre M. All-on-4 immediate-function concept with Brånemark System implants for the completely edentulous maxillae: a 1-year retrospective clinical study. Clin Implant Dent Relat Res. 2005;7(Suppl 1):S88-S94.
23. Mattsson T, Kondell PA, Gynther GW, et al. Implant treatment without bone grafting in severely resorbed edentulous maxillae. Int J Oral Maxillofac Surg. 1999;57(3):281-287.
24. Aparicio C. Tilted implants as an alternative to maxillary sinus grafting: a clinical, radiologic, and periotest study. Clin Implant Dent Relat Res. 2001;3(1):39-49.46-52.
25. Jaffin RA. Rehabilitating the failing dentition: full-arch immediate placement, immediate load therapy. Functional Esthetics and Restorative Dentistry. 2007;1(2):46-52.
26. Brånemark PI, Gröndahl K, Ohrnell LO, et al. Zygoma fixture in the management of advanced atrophy of the maxillae: technique and long-term results. Scand J Plast Reconstr Surg Hand Surg. 2004;38(2):70-85.
27. Malevez C, Abarca M, Durdu F, et al. Clinical outcome of 103 consecutive zygomatic implants: a 6-48 months follow-up study. Clin Oral Implants Res. 2004;15(1):18-22.
28. Bedrossian E, Rangert B, Stumpel L, et al. Immediate function with the zygomatic implant: a graftless solution for the patient with mild to advanced atrophy of the maxilla. Int J Oral Maxillofac Implants. 2006;21(6):937-942.
29. Stella JP, Warner M. Sinus slot technique for simplification and improved orientation of zygomaticus dental implants: a technical note. Int J Oral Maxillofac Implants. 2000;15(6):889-893.
30. Krämer A, Weber H, Benzing U. Implant and prosthetic treatment of the edentulous maxilla using a bar-supported prosthesis. Int Oral Maxillofac Implants. 1992;7(2):251-255.
31. Keller EE, Yolman DE, Eckert SE. Maxillary antral-nasal inlay autogenous bone graft reconstruction of compromised maxilla: a 12-year restrospective study. Int J Oral Maxillofacial Implants. 1999;14(5):707-721.
32. Raghoebar GM, Timmenga NM, Reintsema H, et al. Maxillary bone grafting for insertion of endosseous implants: results after 12-124 months. Clin Oral Implants Res. 2001;12:279-286.
33. Jensen OT, Shulman LB, Block MS, et al. Report of the Sinus Consensus Conference of 1996. Int J Oral Maxillofac Implants. 1998;13(Suppl):11-45.
34. Del Fabbro M, Testori T, Francetti L, et al. Systematic review of survival rates for implants placed in the grafted maxillary sinus. Int J Periodontics Restorative Dent. 2004;24(6):565-577.
35. Wallace SS, Froum SJ. Effect of maxillary sinus augmentation on the survival of endosseous dental implants. A systematic review. Ann Periodontol. 2003;8(1):328-343.
36. Benzing UR, Gall H, Weber H. Biomechanical aspects of two different implant-prosthetic concepts for edentulous maxillae. Int J Oral Maxillofac Implants. 1995;10(2):188-198.
37. Jemt T, Johansson J. Implant treatment in the edentulous maxillae: a 15-year follow-up study on 76 consecutive patients provided with fixed prostheses. Clin Implant Dent Relat Res. 2006;8(2):61-69.
38. Heydecke G, McFarland DH, Feine JS, et al. Speech with maxillary implant prostheses: ratings of articulation. J Dent Res. 2004;83(3):236-240.
39. Lewis S, Beumer J 3rd, Hornburg W, et al. The "UCLA" abutment. Int J Oral Maxillofacial Implants. 1988;3(3):183-189.
About the Author
Aldo Leopardi, BDS, DDS, MS
Private Practice
Denver, Colorado