Simplifying Complex Full-arch Cases by Using an Indirect Provisional Technique
William C. Strupp, Jr., DDS, FAACD
Abstract
Following a proper protocol for fabricating provisional restorations is a key component for success in complex cosmetic and restorative dentistry. The clinical management of full-arch cases can be simplified considerably by using an indirect technique to fabricate provisional restorations. The purpose of this article is to identify the objectives for provisional restorations in full-arch cases and to provide the clinician with step-by-step instruction for a predictable technique that can be employed successfully by auxiliary personnel on a routine basis. Utilizing the simple technique described in this article can make full-arch cases enjoyable, predictable, profitable, inexpensive, and great practice builders. Simultaneously, the protocol will not compromise the health of the patient.
Full-arch cases require specific treatment protocols to assure predictable long-term clinical success. The biggest cause for failures commonly associated with full-arch treatment is odontogenic infection.1-9 Fabrication of provisionals using an indirect technique is a specific protocol that can be useful in achieving success.10,11 In addition, the clinical management of full-arch cases can be simplified considerably using an indirect technique to fabricate provisional restorations.12 The purpose of this article is to identify the objectives for provisional restorations in full-arch cases and provide the clinician with a predictable technique that can be employed by auxiliary personnel to achieve these objectives on a routine basis.
Eight objectives for provisionals when treating full-arch cases are:
- Cosmetic programming
- Maintaining tissue health
- Establishing appropriate occlusion
- Achieving required vertical dimension of occlusion
- Realizing proper phonetic design
- Protecting the pulp
- Providing patient comfort
- Inexpensive fabrication
Each of these objectives must be achieved in order to predictably and routinely manage full-arch cases with ease, preserve the patient's biology, satisfy the patient, and maximize the dentist's profitability.
Cosmetic Programming
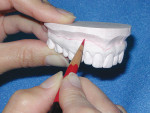
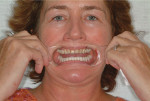
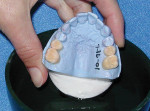
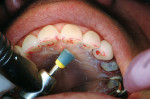
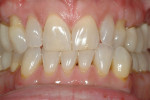
Some of the elements of smile design that must be incorporated into the full-arch provisional to assure a good cosmetic outcome are appropriate incisal plane, incisal length, incisal profile, proportion, incisal embrasure spaces, buccal corridors, plane of occlusion, midline, axial inclination, and lip support.13,14 When these elements are built into the provisional restorations, a model of the provisionals can be given to the laboratory technician, along with detailed instructions, to serve as a blueprint for the success of the case. In addition, accurate photographs of the provisionals that focus on each of these elements can provide the technician with all of the necessary cosmetic information to fabricate the final restorations to perfection.15 Avoiding expensive remakes and patient disappointment add immeasurably to the bottom line of a cosmetically oriented restorative practice (Figure 1 and Figure 2).
Tissue Health
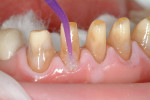
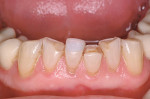
Long-term success of any restorative case is dependent on the health of the gingival tissue on the day of cementation. When the restorations are cemented into a pool of blood because the tissue could not or would not be cleaned around the provisionals, the case is an instantaneous failure. Such failure manifests itself clinically as sensitivity, pulp death, red gums, and periodontal infection. These odon-togenic infections can be difficult, if not impossible, to correct and correlate to systemic disease that can potentially kill the patient.16-27 For gingival tissue to be healthy on the day of cementation, the patient's cemented provisionals must fit properly and he or she must follow appropriate home care.
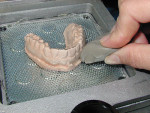
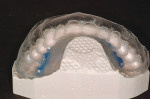
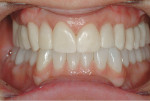
The primary indication that crown and bridge dentistry has been successful is healthy tissue long after the treatment is complete. When the patient's gums are red and bleed easily, something went wrong. Frequently, poorly fitting provisionals that cannot be properly cleaned free of microbes are the primary reason for failure. Using an indirect technique to fabricate provisionals that fit perfectly and are cemented, as well as allow the patient to properly brush and floss the provisionals free of microbes during the provisionalization phase, is preferable to employing a technique that does not facilitate such preventive measures (Figure 3 and Figure 4).
Appropriate Occlusion
Establishing the proper occlusal scheme in the absence of infection results in stability and long-term success in full-arch cases. Centric relation is the preferred joint position for every school of occlusal philosophy. The exception is the neuromuscular school.
Centric relation is the easiest and least complex joint position to achieve with full-arch cases. Occlusion is a tool, not a religion. It has a specific function as it relates to preservation of the dentition. Regarding occlusion as anything other than a tool wastes time and money and detracts attention from factors that truly matter in full-arch cases. The complete elimination of odontogenic infections, preservation of the patient's biology, and simple preventive maintenance of the restorative dentistry are far more important than occlusion theory.
Anterior guidance angles must be used in the final restorative treatment that fit the periodontal support of the dentition being restored.28 Provisional restorations should reflect these angles within an acceptable anterior envelope of function. The envelope of function is altered in virtually every full-arch case. Some clinicians claim the envelope of function cannot be changed without dire consequences. The point is moot, however, because it is impossible to restore a case with extreme wear without altering the envelope of function. The key to altering the envelope of function and establishing an acceptable anterior guidance is to enable the anterior guidance to disclude the posterior teeth by transferring forces onto anterior teeth that have adequate periodontal support to carry the load.
Required Vertical Dimension of Occlusion
The vertical dimension of occlusion (VDO) is not a treatment position goal in any occlusal philosophy, other than the neuromuscular philosophy. In all other occlusal theories, VDO is considered a concept rather than an actual position in space.29 VDO is a necessity and can be easily established at the appropriate level in full-arch restorative cases by following simple procedures, which will be described later in this article.
Phonetic Design
The anterior teeth should be designed for proper speech.30,31 The provisional restorations should reflect that proper design. Three sounds should be evaluated after the patient has worn the full-arch provisional for at least one week.
The "th" sound is influenced by the contour of the cingulum areas of the maxillary anterior teeth. If the contour is too thick, the "th" sound is compromised. In most cases, patients will adapt to overcontoured cingulum areas.
The incisal length of the maxillary incisors influences the "f" and "v" sounds. The incisal edges should just contact the wet/dry line of the lower lip during enunciation of words such as "very" and "fine."
The "s" sound is influenced by the lingual contours and the shape of the incisal edges of the maxillary and mandibular anterior teeth.32 In order to create a crisp "s" sound, a thin sheet of air must be compressed by teeth against other teeth or the tongue against the teeth. It is important to evaluate and correct phonetics in the provisional phase in order to ensure that the technician will have a cast that reflects appropriate phonetic contours to be incorporated into the final restorations of a full-arch case.
Pulp Protection
One of the fundamental concepts in restorative dentistry is to do no harm. Pulp death is common in restorative dentistry. In fact, reports of pulp death are as high as 50% in some cases, and published data routinely show 10% pulp death following restorative procedures. One of the primary causes of pulp death is microbial invasion into open dentin tubules as a result of microleakage under poorly fitting, poorly cemented, or non-cemented provisional restorations. As soon as microbes invade the tubules to the pulp, the outcome is predictable.
Cementing a provisional restoration with an antimicrobial cementa decreases pulp death and sensitivity in restorative dentistry.33 When used in conjunction with appropriate core build-ups, pulp death can be reduced from a rate of 10% to 50% to less than 0.1%.34 When patients experience pulp death of one tooth in 1,000 restorations vs. one tooth in 10 restorations, the impact on a dentist's practice health is stunning.
Patient Comfort
By definition, direct provisional techniques involve the use of objectionable materials in the patient's mouth and typically require a licensed dentist to accomplish the work. When an indirect technique is used, dental assistants perform the bulk of the management in the laboratory. The patient is more comfortable during this process, and the dentist is free to proceed to other cases that are productive. There is no profit in grinding on provisionals.
Inexpensive Fabrication
Laboratory processed provisionals are costly. Provisionals fabricated indirectly by a dental assistant are very inexpensive. Courses are available that are designed to teach dental assistants the art of provisional fabrication using an indirect technique. Note: one such course is taught by the author's assistants and can be found at www.strupp.com.
The Clinical Technique
The following is the technique the author has used for more than 25 years to fabricate provisionals for full-arch cases.
Step 1: Obtain Study Casts
Study casts must be obtained and mounted in centric relation at the correct VDO so they can be waxed to achieve the desired changes in smile design and phonetics. Photographs must be taken to communicate every parameter of the case to the technician assigned to wax the casts.
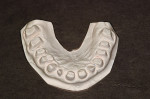
This process begins with excellent polyvinyl siloxane (PVS) or alginate impressions of both arches. The advantage of PVS is that it can be accurately poured multiple times. In addition, the PVS impression serves as a permanent record of what the case was before it was started. Regardless of the impression material chosen, it is important to record every area of soft tissue anatomy (eg, the palate, vestibular areas, and retromolar pads). These areas are the only ones that will provide support to properly position a matrix. If the soft tissue is not captured properly, the impression should be discarded and a new one fabricated (Figure 5).
Step 2: Capture Centric Relation Along with the Horizontal Plane and the Midline of the Face with a Bite Record at the Correct VDO
A bite record must be obtained that will relate the casts to each other on an articulator in centric relation at the correct VDO. The midline and horizontal plane of the face should also be recorded with the same bite record so that the casts can be positioned properly on the articulator.
The simplest way to make this bite record is to establish the correct VDO and then make the bite record at that VDO. The correct VDO is determined solely by the room required for the chosen restorative materials. The existing VDO is determined by hav-ing the patient close into centric occlusion and measuring with 3½-inch dividersb from the free gingival margins of two opposing anterior teeth.
In the extreme wear case, the VDO typically must be opened to provide sufficient room for the technician to make the restorations. Determining the VDO in such a case is accomplished by rebuilding the lingual contour of one maxillary central incisor in flowable resin composite, and then rebuilding the desired length and shape of the opposing mandibular incisor in the same material. The zones of occlusal contact of both teeth should be anatomically correct.
Lower incisors without wear are approximately 9.0 mm, an excellent length for cosmetics. The minimum length for proper cosmetics is 7.0 mm. Longer or shorter lower central incisors can be fabricated, but only by compromising the cosmetic result.
After these contours are rebuilt, the patient will make occlusal contact at a new VDO, which will be the correct VDO for the case. A new measurement from the free gingival margins of the same opposing teeth that were measured previously is made. The difference between the two measurements is the amount the VDO will be opened.
After the correct VDO is established, fresh flowable resin composite is placed onto the centric holding contact area, and the patient is manipulated into a centric relation closure arc as described by Dr. Peter Dawson until contact is achieved between the two rebuilt teeth. The resin composite is then light activated to freeze the centric holding contact in such a way that the mandible cannot move in any direction except through rotation into centric relation. The mandible is forced into centric relation simply by having the patient clench. Since the anterior stop preserves the VDO and the lower incisor cannot move forward, backward, left or right, the only movement that the mandible can make when strong clenching forces are applied is to rotate around the anterior stop, serving as a fulcrum point and seating the condyles into centric relation (Figure 6). No manual technique equals the accuracy of the patient's own mastication muscles.
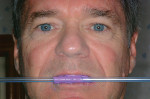
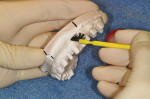
While the patient is seated in an upright position to cancel the effect of gravity, position the tip of the tongue in the back of the palate to provide space for the PVS material and clench forcefully to seat the condyles into centric relation. Injecting a PVS bite record materialc between the teeth will record centric relation at the correct VDO. Excess PVS material is injected in the anterior, and a straw is positioned to record the horizontal plane. The straw is rotated to retain it in the PVS material. The midline of the face is marked with a periodontal probe. This entire process takes about 10 minutes.
The patient is asked to stand in a relaxed position with feet shoulder-width apart and arms by the sides while not leaning against the wall. The straw should be perfectly positioned in the horizontal plane (Figure 7). If it is not, the straw should be removed and a new one tacked in place with fresh PVS material to reflect the horizontal plane.
Step 3: Photographs
A full-face photograph is then made to verify the cast positions on the articulator relative to the horizontal plane and the midline. A preoperative full-face photograph with the patient standing in a like manner with lips retracted, as well as in a full smile, are required to evaluate the existing incisal plane relative to the horizontal plane and the dental midline relative to the middle of the face (Figure 8 and Figure 9). This information is used by the technician to make necessary changes by waxing the study casts. These changes will be reflected in the provisionals.
Step 4: Ideally Wax the Case
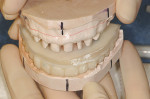
The information provided in the photographs is used in conjunction with the correct spatial relationship of the study casts on the articulator and the desired cosmetic outcome of the patient and dentist to wax the casts to ideal. The parameters of smile design mentioned earlier in the article should be created precisely in the wax-up (Figure 10). The more attention to detail that is paid to the wax-up, the less work the assistants will have when making the provisionals.
Step 5: Duplicate the Wax-up
Alginate can be used to duplicate the wax-up. PVS reproduces more detail of the wax-up. If alginate is used, the waxed model should be soaked in cold water for 15 minutes so it is completely saturated with water (Figure 11). In this way, it will not "suck" the alginate dry and stick. If PVS is used, the wax-up is frequently damaged, although this can also occur when using alginate. The impression of the wax-up is poured in die stone to provide a model that does not easily chip or become damaged.
Step 6: Create a Matrix
A matrix can be formed in one of two ways: by vacuum adapting a plastic material to the duplicated wax-up, or making a PVS impression of either the wax-up or duplicate model. The easiest to use is the vacuum-adapted plastic matrix, because it allows visualization of the proper position of the matrix (Figure 12). It is also called a shim.
Step 7: Create a Stone-Seating Index
A stone-seating index is formed over the shim while it is positioned on the duplicated model. The purpose of the index is to force the shim into the proper spatial relationship without distortion when it is filled with acrylic (Figure 13).
Step 8: Create a Master Provisional Model
Immediately after the master PVS impression of the prepared teeth is removed and before the tissue can collapse, a second PVS impression is made. It is poured in setting stone.d The provisional impression is poured a second time immediately after the retrieval of the primary provisional cast (Figure 14).
Frequently, a third pour of the provisional impression is used. Since the provisional impression is poured several times, it is critical that the tray used for the impression properly retain the impression material. A custom tray is usually used for full-arch cases for both the master impression and the impression for provisionals because of the requirement of precision fit for the final and provisional restorations.
Step 9: Fit the Matrix to the Provisional Model and Draw Indexing Lines
The plastic shim and stone-seating index must seat completely on the master provisional model so that when it is filled with acrylic, it can be positioned properly in space (Figure 15). This will minimize the amount of occlusal and cosmetic adjustment required after the acrylic sets. Indexing lines are drawn on the model to aid the assistant in properly positioning the shim and index.
Step 10: Place Appropriate Separators
An insulating or liquid separating producte is applied to the master provisional cast wherever acrylic will come into contact with it so that it will not stick (Figure 16). After it completely sets, a second separator, a die lubricant,f is applied. This die lubricant is blown thin because it does not set.
Step 11: Fill the Shim with Acrylic and Place the Provisional Model into It
The shim is filled to the gingival line with an acrylicg and positioned properly with the stone-seating index on the primary provisional model (Figure 17). The index is secured with rubber bands, and the model/shim/index is placed in hot water for 10 minutes to facilitate a complete set of the acrylic.
Step 12: Divest, Section, Trim, and Shape the Provisional
When the full-arch provisional is carefully removed from the model without fracture, it is sectioned into three parts: Nos. 6 through 11, Nos. 2 through 5, and Nos. 12 through 15, if it is a maxillary case; and Nos. 22 through 27, Nos. 18 through 21, and Nos. 28 through 31, if it is a mandibular case. It is then trimmed and shaped to precisely identify all cosmetic parameters and margin fit (Figure 18). The intaglio is then air abraded to remove debris and create a textured surface for enhanced cement retention.
Each section is seated on the second pour model to verify and correct margin discrepancies. One of the chief advantages of this recommended acrylicg is its ability to trim the margin to exact precision and easily add material if too much was removed during initial trimming. Additions can be made with an autopolymerizing acrylic resin,h which sets in one minute.
Step 13: Try-in; Adjust Occlusion, Cosmetics, Phonetics, and VDO
The anterior section is tried in first and the VDO is verified by measuring with dividers, as previously described. The anterior envelope of function is adjusted as necessary (Figure 19). Centric holding contacts are adjusted or added, as necessary. Phonetic parameters are verified and adjusted, if necessary. Cosmetic details are refined.
After this is accomplished, the posterior sections are tried in one side at a time and adjusted so that equally intense centric holding contacts exist on all of the teeth. Lateral excursions are adjusted so that only the anterior guidance previously established on the six anterior teeth makes contact in excursive movements.
Step 14: Polish and Cement
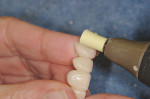
The provisionals are polished on a lathe with a pumice,i protecting the margins with the fleshy part of the finger (Figure 20). This will avoid polishing off the precisely fitting margins. Gloves should not be worn since serious injury may occur should the glove get caught in the rag wheel.
The provisionals are cemented with the previously mentioned cementa based on its antimicrobial activity and sedative effect on the pulp. Every vestige of excess cement must be removed or granulation tissue will form that will compromise the field with blood at cementation. Intense home care instructions with interproximal brushes in the posterior, along with aggressive toothbrushing and flossing instructions, are given to the patient. The aforementioned acrylic, unlike bisacryl resins, will flex enough to allow easy removal of provisionals cemented with the antimicrobial cement. Bisacryl resins are brittle and frequently must be cut off to remove them when they are cemented with the antimicrobial cement.
Step 15: Cement Check and Esthetic Evaluation Appointment
In approximately one week, the patient returns so that the dental staff can ascertain that all cement has been removed, occlusion is correct, cosmetic parameters are acceptable, phonetics are perfect, pulps are healthy, home care is perfect, and there are no complications that might compromise the end result (Figure 21). In addition, it is important to ascertain whether the patient is satisfied. Afterwards, an impression is made of the provisionals to serve as a three-dimensional blueprint for the technician to fabricate the case. The provisional cast is mounted against the opposing model and is used to make indexes that aid in fabricating the final restorations. While the patient is standing, full-face photographs of a full smile, with and without retractors in place, are taken to illustrate the incisal plane so it may be compared to the horizontal plane.
Conclusion
Following a proper protocol for fabricating provisional restorations is fundamental to success in complex cosmetic and restorative dentistry (Figure 22 and Figure 23). Using the simple technique for indirect fabrication described in this article can make full-arch cases enjoyable, predictable, simple, profitable, inexpensive, and great practice builders.
a Durelon™ Carboxylate Luting Cement, 3M ESPE, St. Paul, MN b Starrett Jewelry Supplier, East Brunswick, NJ c Occlufast Rock, Zhermack, Inc., Eatontown, NJ d Snap-Stone, Whip Mix, Louisville, KY e Acrylic & Plaster Separator, Dental Ventures of America, Inc., Corona, CA f Isolit®, Dentsply International, York, PA g Jet Acrylic, Lang Dental Mfg. Co., Inc., Wheeling, IL h Super T, American Consolidated Mfg. Co., W. Conshohocken, PA i Henry Schein Pumice, Henry Schein, Inc., Melville, NY
References
1. De Backer H, Van Maele G, De Moor N, et al. Survival of complete crowns and periodontal health: 18-year retrospective study. Int J Prosthodont. 2007;20:151-158.
2. Goodacre CJ, Bernal G, Rungcharassaeng K, et al. Clinical complications in fixed prosthodontics. J Prosthet Dent. 2003;90:31-41.
3. Cheung GS, Lai SC, Ng RP. Fate of vital pulps beneath a metal-ceramic crown or a bridge retainer. Int Endod J. 2005;38:521-530.
4. Jackson CR, Skidmore AE, Rice RT. Pulpal evaluation of teeth restored with fixed prostheses. J Prosthet Dent. 1992;67:323-325.
5. Zoellner A, Herzberg S, Gaengler P. Histobacteriology and pulp reactions to long-term dental restorations. J Marmara Univ Dent Fac. 1996;2:483-490.
6. Christensen GJ. Tooth preparation and pulp degeneration. J Am Dent Assoc. 1997;128:353-354.
7. Groten M. Complete esthetic and functional rehabilitation with adhesively luted all-ceramic restorations—case report over 4.5 years. Quintessence Int. 2007;38:723-731.
8. Amiri-Jezeh M, Rateitschak E, Weiger R, et al. [The impact of the margin of restorations on periodontal health—a review.] Schweiz Monatsschr Zahnmed. 2006;116:606-613.
9. Reitemeier B, Hänsel K, Walter MH, et al. Effect of posterior crown margin placement on gingival health. J Prosthet Dent. 2002;87:167-172.
10. Fondriest JF. Using provisional restorations to improve results in complex aesthetic restorative cases. Pract Proced Aesthet Dent. 2006;18:217-223.
11. Thongthammachat-Thavornthanasarn S. Treatment of a patient with severely worn dentition: a clinical report. J Prosthodont. 2007;16:219-225.
12. Small BW. Indirect provisional restorations. Gen Dent. 1999;47:140-142.
13. Davis NC. Smile design. Dent Clin North Am. 2007;51: 299-318, vii.
14. Chu SJ. A biometric approach to predictable treatment of clinical crown discrepancies. Pract Proced Aesthet Dent. 2007;19:401-409.
15. Snow SR. Strategies for successful esthetic dental treatment. J Calif Dent Assoc. 2007;35: 475-484.
16. Ford PJ, Yamazaki K, Seymour GJ. Cardiovascular and oral disease interactions: what is the evidence? Prim Dent Care. 2007;14:59-66.
17. Moutsopoulos NM, Madianos PN. Low-grade inflammation in chronic infectious diseases: paradigm of periodontal infections. Ann N Y Acad Sci. 2006;1088:251-264.
18. Demmer RT, Desvarieux M. Periodontal infections and cardiovascular disease: the heart of the matter. J Am Dent Assoc. 2006;137 Suppl:14S-20S.
19. Beck JD, Offenbacher S. Systemic effects of periodontitis: epidemiology of periodontal disease and cardiovascular disease. J Periodontol. 2005;76(11 Suppl):2089-2100.
20. Scannapieco FA, Bush RB, Paju S. Associations between periodontal disease and risk for atherosclerosis, cardiovascular disease, and stroke. A systematic review. Ann Periodontol. 2003;8:38-53.
21. Genco R, Offenbacher S, Beck J. Periodontal disease and cardiovascular disease: epidemiology and possible mechanisms. J Am Dent Assoc. 2002;133 Suppl:14S-22S.
22. Mattila KJ, Nieminen MS, Valtonen VV, et al. Association between dental health and acute myocardial infarction. BMJ. 1989;298:779-781.
23. Desvarieux M, Demmer RT, Rundek T, et al. Periodontal microbiota and carotid intima-media thickness: the Oral Infections and Vascular Disease Epidemiology Study (INVEST). Circulation. 2005;111:576-582.
24. Meurman JH, Sanz M, Janket SJ. Oral health, atherosclerosis, and cardiovascular disease. Crit Rev Oral Biol Med. 2004;15:403-413.
25. Jin LJ, Chiu GK, Corbet EF. Are periodontal diseases risk factors for certain systemic disorders—what matters to medical practitioners? Hong Kong Med J. 2003;9: 31-37.
26. Deshpande RG, Kahn MB, Genco CA. Invasion of aortic and heart endothelial cells by Porphyromonas gingivalis. Infect Immun. 1998;66:5337-5343.
27. Scannapieco FA. Periodontal inflammation: from gingivitis to systemic disease? Compend Cont Educ Dent. 2004;25(7 Suppl 1):16-25.
28. Dawson PE. Determining the determinants of occlusion. Int J Periodontics Restorative Dent. 1983;3:8-21.
29. Koka S. Vertical dimension of occlusion. Int J Prosthodont. 2007;20:342.
30. Small BW. Location of incisal edge position for esthetic restorative dentistry. Gen Dent. 2000;48: 396-397.
31. Pound E. Utilizing speech to simplify a personalized denture service. 1970. J Prosthet Dent. 2006;95:1-9.
32. Runte C, Lawerino M, Dirksen D, et al. The influence of maxillary central incisor position in complete dentures on /s/ sound production. J Prosthet Dent. 2001;85: 485-495.
33. Lewinstein I, Matalon S, Slutzkey S, et al. Antibacterial properties of aged dental cements evaluated by direct-contact and agar diffusion tests. J Prosthet Dent. 2005;93:364-371.
34. Strupp WC. Critical factors for clinical success with all ceramic restorations. Crown and Bridge UPDATE. 2003;8(3-4).
Note: the entire case is presented in Volume 12 of "Crown & Bridge UPDATE," which can be viewed at www.strupp.com.
About the Author
William C. Strupp, Jr., DDS, FAACD
Lecturer, William C. Strupp School of Postgraduate Dentistry
Clearwater, Florida