Contemporary Dental Cements to Meet the Challenges of Today's Restorative Dentistry
Howard E. Strassler, DMD, and Luis Guilherme Sensi, DDS, MS, PhD
Abstract
The search for an all-purpose luting system for final cementation that fulfills the properties necessary for definitive placement of cast metal, porcelain-metal, resin, and all-ceramic full-coverage restorations has been limited by the physical properties of the cements that have been available. Currently the clinician has many choices for cementation. Despite the challenges of the current restorative materials used for laboratory fabricated restorations, the newest cements satisfy many of the required demands.
Introduction
Within any general and restorative dental practice, the clinician is faced with making choices about which cement to use for definitive, final cementation. Cementation or luting is a critical phase in the placement of laboratory fabricated restorations. In the past (and still), the term "permanent" cement has been the catch phrase for describing the use of cement for final, definitive placement of indirect laboratory fabricated restorations. The future trend when describing cementation in restorative dentistry should focus on the placement-cementation so that the restoration cannot be retrieved, hence the description of "definitive cementation."1 In the past, a practitioner had a limited number of choices for which cement they could use. Presently there are many choices of cements that satisfy the requirements of the ceramics, metals, and posts currently used in restorative dentistry. Similarly, among laboratory fabricated restorations are a variety of options to consider when treatment planning, such as fixed or removable partial dentures or implants, full-coverage crowns, partial coverage inlays and onlays, cast post and cores, and prefabricated posts when restoring endodontically treated teeth.
Indirect treatment procedures are generally very involved and require more than one appointment. Throughout the procedures for restorations that will be fabricated by a laboratory, the practitioner spends significant time attending to tooth preparation or implant placement, impressioning and soft tissue management, provisional restorations, selection of tooth shade for esthetic restorations, try-in and adjustment of the restoration, and cementation. In some cases, restorative planning might involve a diagnostic wax-up to preview and develop the case. If one were to create a pie chart to analyze the time spent for each phase, cementation would account for less than 5% of the time required to complete the case. In fact, cost-wise for most restorations—including multi-unit restorations for numerous teeth (e.g. large porcelain veneer cases or long-span fixed partial dentures)—the practitioner may use a cementation system that costs less than $20 or, in the case of the old standby in dentistry, zinc phosphate cement, less than $1.
Clinicians should not discount the requirements for cementing restorations. Incorrect cement selection, as well as poor technique during placement of the restoration, can lead to premature failure of these costly restorations (ie, cost to the practitioner in laboratory fees; cost to the patient for the restoration). This article provides an overview of the requirements for cement selection when placing restorations based on the challenges presented by current restorative materials.
Factors Affecting Cementation Success
While the type of cement is important, other factors affect clinical success. When using cements, it is important that there be excellent marginal integrity following cementation to compensate for any marginal discrepancies between the restorative material and tooth preparation.2-5 Also, the retention of the crown is not only affected by the type of cement used, but also by the taper of the tooth preparation.6 The retentive values of an adhesive resin cement for a 24° taper were 20% higher than the retentive values of zinc phosphate cement and a conventional glass ionomer cement. The resin luting agents yielded retention values that were double those of zinc phosphate and conventional glass ionomer cements. The type of bur or diamond rotary instrument used for preparing for crowns can also affect the retention of a crown placed with different cements.7
One significant issue after cementation is the presence of postoperative sensitivity. Conventional glass ionomer cements have been implicated in higher rates of postoperative sensitivity than other cements.8 Some authors have reported that when following a manufacturer's recommendations, there is little association between zinc phosphate cement or glass ionomer cement.9-11 Recommendations have been made to avoid dessication of the dentin surface before cementation.12 Other studies have described the use of desensitizing agents and dentin sealers as part of the cementation process,13-17 but there has been concern that certain desensitizing techniques can have a negative impact on the adhesion of different cements. However, the use of a 5% glutaraldehyde sealer15,16 or a resin sealer14,16,17 was not detrimental to resin or glass ionomer cements. Oxalate desensitizers, on the other hand, are incompatible with glass ionomer luting agents.18
Factors to be Considered when Selecting a Cement
Is there a single cement that can be used for all indirect applications? Development of a true all-purpose cement has involved quantifying specific physical properties and handling characteristics.19-21 The ideal characteristics of an all-purpose cement include:
- low viscosity for easy seating
- easy to mix
- extended working time
- short setting time
- film thickness compatible with complete seating of a restoration
- insolubility in the mouth
- high shear strength
- high tensile strength
- high compressive strength
- bondable to tooth and restoration
- biocompatible with pulp and soft tissue (ie, no postoperative sensitivity)
- translucent
- radiopaque
- easy post-cementation clean-up
Researchers have evaluated the properties of the various dental cements available in order to identify that elusive "ideal" cement. Currently, within the variety of cements available, a universal cement does not yet exist, although manufacturers have been getting closer to providing the practitioner with an all-purpose cementation system.
Classification of Dental Cements
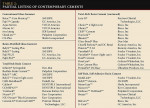
For definitive cementation, dental cements are classified according to their chemistry (Table 1 and Table 2).19 Water-based cements usually undergo an acid-base setting reaction. In some cases, a slight amount of resin is added to improve workability. Among cements in this class are zinc phosphate, zinc polycarboxylate, and glass- and resin-modified (resin-reinforced) glass ionomer cements. The fastest growing category of definitive cements is resin-based cements, which have a chemistry based on current composite resins and bonding adhesives.22 Resin-based cements include composite resin cements that are self-adhesive, those that require an additional bonding adhesive before the cement is placed, and compomer cements.
Each category of cements presents challenges for the practitioner in terms of manipulation in order to achieve clinical success. Within each class, these cements have physical properties that allow for a consistency suitable for cementation, as well as a film thickness that allows complete seating of a restoration during placement. It should be noted that there is variability in the handling characteristics of each class of cement, and differences exist among cements within the same class. In almost all cases, the clinician should not assume that cements within the same class are mixed and manipulated in the same manner. It is critical that dentists and their chairside assistant read the instructions related to material dispensing and mixing before cementing the restoration.1,18,23
Although zinc phosphate cement and zinc polycarboxylate cement are still popular cements, the trends have demonstrated that conventional glass ionomer cement, resin-modified glass ionomer cement, and composite resin cements are the primary cements being used in restorative dentistry. A recent survey of usage of definitive fixed prosthodontic cements found that conventional glass ionomer cement was used 24% of the time, resin-modified glass ionomer cement 46% of the time, composite resin cements 8% of the time, zinc phosphate cement 10% of the time, and zinc polycarboxylate cement 12% of the time.23 However, before dismissing zinc phosphate cement from use in your practice, consider the primary benefit and indication for this family of cements, which is its ability to extend the working time by being mixed on a cooled glass slab; this dissipates the heat of the exothermic reaction. This extended working time allows the cement to be used for long-span fixed partial dentures (ie, five units or longer), whereas other cements set too rapidly to allow for cementation of such long-span prostheses.
Glass ionomer cement
Glass ionomer cements are classified as either conventional glass ionomer cements, which are water-based and without any resin, and resin-modified glass ionomer cements that have approximately 10% resin added to the formula to improve their physical properties. Both types of glass ionomer cements are adhesive to enamel and dentin via ionic bonding of the glass ionomer to the calcium and phosphate ions of the tooth. It usually takes 24 hours for the final adhesive values to be attained. In addition to being self-adhesive through chemical bonding to tooth structure, glass ionomers have the additional benefit of leaching fluoride to the adjacent tooth structure, which provides some protection against recurrent caries. Both types of glass ionomer cement have low solubility.
Conventional glass ionomer is provided as a powder and liquid that can be either hand-dispensed for mixing on a mixing pad with a cement spatula or used in a preloaded capsule that is mixed in a mechanical mixer (e.g. amalgamator, triturator) and has a dispensing tip; the cement is syringed using an applicator gun onto the restoration and preparation. Applicator guns are usually manufacturer specific.
When using a conventional glass ionomer cement, the excess cement at the margins should be protected from moisture and drying using a coating agent or an unfilled bonding resin. It is advisable not to clear away excess cement until it is fully set.
Resin-modified glass ionomer cement (also referred to as resin-reinforced and hybrid ionomer) is supplied as either a powder-liquid, paste-paste, or a unit dose mixing capsule with a dispensing tip. It is easier to mix than conventional powder-liquid glass ionomers and has improved physical properties while retaining the characteristics of self-adhesion and fluoride release. Some of the resin-modified glass ionomer cements provide a dentin conditioner to improve adhesive bonding. Also, excess resin-modified glass ionomer cement may be removed when it reaches the gel stage or after complete setting. Resin-modified glass ionomer cements are less vulnerable to early moisture.
The primary clinical indication for use of either type of glass ionomer cement is cementation of all-metal and porcelain-metal restorations, alumina or zirconia core all-ceramic restorations, implant-supported crowns and fixed partial dentures, and metal posts. It is the author's cement of choice for placing all-metal and porcelain-metal restorations. Because it is important that the tooth not be overdried when using this class of dental cement, this author usually wets the dentin using a microapplicator so that it appears slightly glossy, with no water pooling on the surface. Also, when glass ionomer cements were first introduced, there was concern about postoperative sensitivity after cementation,7 as previously noted. However, studies have demonstrated that this is not a problem.8-10
Composite resin cements
Within this growing class of resin-based luting agents are adhesive composite resin cements that require a separate adhesive application, and self-adhesive composite resin cements that do not. For easier understanding, these categories will be described separately. In most cases, the indications for cements in this class are the same, while ease of application is different. Adhesive resin cements typically use a total-etch bonding adhesive; self-adhesive resin cements eliminate the need for the initial phosphoric acid-etching of the tooth structure. Also, there are a variety of initiators that are used to promote the resin polymerization. Composite resin cements are supplied as powder-liquid and paste-paste hand-mixing, double-barreled syringe with automixing tips, and unit dose dispensing and mixing systems.
All cements in this category are relatively insoluble and, compared to other dental cements, have the highest mechanical physical properties (e.g. high compressive strength, high flexural strength, good fracture toughness, low coefficient of thermal expansion and contraction, highest stiffness of any dental cement).1,18,23 These cements are based upon the chemistry of direct placement restorative composite resins and are wear- and abrasion-resistant.
Composite resin cements demonstrate greater tooth-like translucency and, in some cases, are available in tooth shades or in several shades to best match the adjacent tooth structure. Also, adhesion of this class of cement to not only tooth structure but also to etched porcelain (Figure 1) and sand-blasted metal has been demonstrated.24-27 When used with etched ceramic restorations, resin cements make the restoration more resistant to fracture.28 In terms of handling, composite resin cements demonstrate easy flow, spread easily over the surface being cemented, are not tacky, are polishable, and have a chameleon effect with the surrounding tooth structure.
Total-etch adhesive resin cements
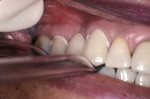
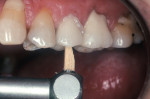
The resin cements in this category require separate tooth etching with phosphoric acid and the application of a separate resin bonding agent. When bonding to dentin, these cements use the adhesive as the bonding interface with the composite cement (Figure 2). The cements can be classified as self-cure (auto polymerizing), dual-cure (light- and self-cure), and light-cure cements. The differences in the polymerization mechanism are based upon the type of chemical initiator. Self-cure composite resin cements use a peroxide-amine initiator-accelerator; dual-cure composite resin cements use a combination of amine and photo-initiator; light-cure resin cements use a photo-initiator only. These composite resin cements can be used for cementation of all types of indirect restorations, but due to potential problems with color stability, it is recommended that translucent all-ceramic restorations such as crowns and veneers be placed with light-cure composite cements29-31 (Figure 3). When using light-cured composite cements with all-ceramic veneers or crowns, the light-curing time should be increased when polymerizing through porcelain thicknesses of 0.5 mm to 2.0 mm.19
There has been concern that self-cure and dual-cure composites are chemically incompatible with light-cure adhesives.32-37 Currently, changes in the chemistry of different systems and the addition of activators to 5th generation adhesives appear to solve this problem. At the current time there is no blanket statement that can be made about self-cure and dual-cure resin cements and total-etch and self-etch adhesives. The results are product specific; practitioners should read each bonding agent's instructions for clinical recommendations. When using a dual-cure resin cement, the light-curing capability offers the additional benefit of ease of clean-up. The excess resin cement is removed from the margin areas, after which the restoration can be light-cured to seal off any potential contaminants. In all cases, with any total-etch adhesive resin cement, care must be taken to inspect and remove excess resin cement. Unlike more traditional cements for which the excess can be easily removed with a scaler or curet, in some cases a rotary diamond or finishing bur is necessary to remove set resin cement.
Self-adhesive resin cements
When seeking the "Holy Grail" of dental cements, the self-adhesive resin cements are approaching the requirements of a true all-purpose cement. Although these authors would not advise their use with translucent ceramic restorations (e.g. pressed ceramic crowns or porcelain veneers)—where a color change in the cement could affect the color of the restoration—they can be used for all other applications. Many of the cements in this category are available in dual-tube automixing configurations or, in some cases,b,c are in preloaded capsules that are mixed in a high-speed mixer (e.g. triturator). These cements are especially useful for cementation of fiber posts. Oned provides a special tip for delivering the cement into the root canal. Special tubesd can be loaded with any brand and type of cement to allow a needle-tip delivery into any root canal for cementing any post system. This type of needle delivery has been shown to be more effective at filling the root canal than a lentulo spiral.38 Even though these cements are self-adhesive using the mechanisms of the self-etch class of adhesives,b,c,e some cementsf require a separate primer on the tooth surface before using the cement.25,39,40 Before using a self-adhesive cement, clinicians should be familiar with the required protocol.
Clinical Technique Recommendations for Resin Cements
Resin cements have well-researched physical properties.5,41-43 They bond well to abraded base metal.27, 44 Research has shown that resin-based cements and resin-modified glass ionomer cements are thixotropic (ie, as viscous liquids, there is a shear-thinning of the fluid phase of the cement that requires a finite amount of time to reach an equilibrium). The different physical characteristics and properties of these cements influence the seating of crowns during cementation.45-47 Using force allows the cement to flow when placing the restoration completely on the tooth preparation. In fact, sustained seating pressure during luting procedures, up to three minutes, increases bond strength and improves marginal integrity of the interfacial margins.48 Clinical techniques have been described to improve seating, include having the patient bite down on a saliva ejector49 (Figure 4) or using a vibrating mechanical device such as a reciprocating hand-pieceg with a wooden seating stick50 (Figure 5). The hydraulic forces needed to completely seat a crown, inlay, and onlay using a resin-based cement or resin-modified glass ionomer require some form of mechanical advantage.
Conclusion
With the increase in the number of material options used for indirect restorations, choosing which cement to use for what type of restoration has become more difficult and confusing for the clinician. Although no one cement fulfills all the needs for all cementation situations, understanding the differences between each class of dental cement will contribute to the clinical success of the restoration.
Disclosure
Howard E. Strassler, DMD, has received grant/research support from DENTSPLY, GC America, Inc., Ultradent Products, Inc., and Den-Mat. He has also received honoraria from GC America, Inc., Den-Mat, Dentatus USA, Bisco, Inc., and Heraeus Kulzer, Inc.
References
1. Rosenstiel SF, Land MF, Fujimoto J. Comptemporary Fixed Prosthodontics. 4th ed. St. Louis, MO: Mosby Elsevier; 2006.
2. Bott B, Hannig M. Effect of different luting materials on the marginal adaptation of Class I ceramic inlay restorations in vitro. Dent Mater. 2003;19:264-269.
3. Rosentritt M, Behr M, Lang R, et al. Influence of cement type on the marginal adaptation of all-ceramic MOD inlays. Dent Mater. 2004;20:463-469.
4. Fabianelli A, Goracci C, Bertelli E, et al. In vitro evaluation of wall-to-wall adaptation of a self-adhesive resin cement used for luting gold and ceramic inlays. J Adhes Dent. 2005;7:33-40.
5. White SN, Yu Z, Tom JF, et al. In vivo marginal adaptation of cast crowns luted with different cements. J Prosthet Dent. 1995;74:25-32.
6. Zidan O, Ferguson GC. The retention of complete crowns prepared with three different tapers and luted with four different cements. J Prosthet Dent. 2003;89:565-571.
7. Ayad MF, Rosenstiel SF, Salama M. Influence of tooth surface roughness and type of cement on retention of complete cast crowns. J Prosthet Dent. 1997;77:116-121.
8. Reported sensitivity to glass ionomer luting cements. Council on Dental Materials, Instruments, and Equipment. J Am Dent Assoc. 1984;109:476.
9. Kern M, Kleimeier B, Schaller HG, et al. Clinical comparison of postoperative sensitivity for a glass ionomer and a zinc phosphate luting cement. J Prosthet Dent. 1996;75:159-162.
10. Smales RJ, Gale MS. Comparison of pulpal sensitivity between a conventional and two resin-modified glass ionomer luting cements. Oper Dent. 2002;27:442-446.
11. Hilton T, Hilton D, Randall R, et al. A clinical comparison of two cements for levels of post-operative sensitivity in a practice-based setting. Oper Dent. 2004;29:241-248.
12. Rosenstiel SF, Rashid RG. Postcementation hypersensitivity: scientific data versus dentists' perceptions. J Prosthodont. 2003;12:73-81.
13. Brannstrom M. Reducing the risk of sensitivity and pulpal complications after the placement of crowns and fixed partial dentures. Quintessence Int. 1996;27:673-678.
14. Johnson GH, Hazelton LR, Bales DJ, et al. The effect of a resin-based sealer on crown retention for three types of cement. J Prosthet Dent. 2004;91:428-435.
15. Johnson GH, Lepe X, Bales DJ. Crown retention with use of a 5% glutaraldehyde sealer on prepared dentin. J Prosthet Dent. 1998;79:671-676.
16. Yim NH, Rueggeberg FA, Caughman WF, et al. Effect of dentin desensitizers and cementing agents on retention of full crowns using standardized crown preparations. J Prosthet Dent. 2000;83:459-465.
17. Magne P, Kim TH, Cascione D, et al. Immediate dentin sealing improves bond strength of indirect restorations. J Prosthet Dent. 2005;94:511-519.
18. Strassler H, Suh BI, Wang Y. Compatibility of oxalate desensitizer with glass ionomer cements. J Dent Res. 2006;85(Special Issue A): Abstract #1885.
19. Powers JM, Sakaguchi RL. Cements. In: Powers JM, Sakaguchi RL, eds. Craig's Restorative Dental Materials. St. Louis, MO:Mosby Elsevier; 2006:480-511.
20. Rosenstiel SF, Land MF, Crispin BJ. Dental luting agents: A review of the current literature. J Prosthet Dent. 1998;80:280-301.
21. McComb D. Adhesive luting cements--classes, criteria, and usage. Compend Contin Educ Dent. 1996;17:759-762,764.
22. Platt JA. Resin-based luting cements. Compend Contin Educ Dent. 2000;21: 740-742,744.
23. Traditional crown and bridge cements. The Dental Advisor. 2006;23:1-5.
24. de Menezes MJ, Arrais CA, Giannini M. Influence of light-activated and auto-and dual-polymerizing adhesive systems on bond strength of indirect composite resin to dentin. J Prosthet Dent. 2006;96:115-121.
25. Burke FJ, Fleming GJ, Abbas G, et al. Effectiveness of a self-adhesive resin luting system on fracture resistance of teeth restored with dentin-bonded crowns. Eur J Prosthodont Restor Dent. 2006;14:185-188.
26. Escribano N, de la Macorra JC. Microtensile bond strength of self-adhesive luting cements to ceramic. J Adhes Dent. 2006;8:337-341.
27. O'Connor RP, Nayyar A, Kovarik RE. Effect of internal microblasting on retention of cemented cast crowns. J Prosthet Dent. 1990;64:557-562.
28. Pallis K, Griggs JA, Woody RD, et al. Fracture resistance of three all-ceramic restorative systems for posterior applications. J Prosthet Dent. 2004;91:561-569.
29. Nathanson D, Banasr F. Color stability of resin cements—an in vitro study. Pract Proced Aesthet Dent. 2002;14:449-455.
30. Hekimoglu C, Anil N, Etikan I. Effect of accelerated aging on the color stability of cemented laminate veneers. Int J Prosthodont. 2000;13:29-33.
31. Lu H, Powers JM. Color stability of resin cements after accelerated aging. Am J Dent. 2004;17:354-358.
32. Tay FR, Pashley DH, Peters MC. Adhesive permeability affects composite coupling to dentin treated with a self-etch adhesive. Oper Dent. 2003;28:610-621.
33. Hillam R, Pasciuta M, Cobb D. Shear bond strength of primer/adhesives with proprietary dual cure resin cement. J Dent Res. 2002;81(Special Issue A): Abstract #369.
34. Pasciuta M, Cobb D, Denehy G. Shear bond strength of dual cure primer/adhesives with dual cure resin cements. J Dent Res. 2002;81(Special Issue A): Abstract #405.
35. Christensen G. Self-etch primer (SEP) adhesives update. CRA Newsletter. 2003;27:1-5.
36. King N, Tay P, Pashley DH, et al. Incompatiblity profiles of all-in-one adhesives. J Dent Res. 2004;83(Special Issue A): Abstract #23.
37. Brown PL, Schiltz-Taing M, Sharp LJ, et al. Microtensile strength of adhesives using indirect and direct composites. J Dent Res. 2004;83(Special Issue A): Abstract #1526.
38. Strassler HE, Campbell R, Wycall B, et al. Evaluation of two techniques for cement application into root canals. J Dent Res. 2000;79(IADR Abstracts): Abstract #2332.
39. Al-Assaf K, Chakmakchi M, Palaghias G, et al. Interfacial characteristics of adhesive luting resins and composites with dentine. Dent Mater. 2006;Epub ahead of print.
40. Pisani-Proenca J, Erhardt MC, Valandro LF, et al. Influence of ceramic surface conditioning and resin cements on microtensile bond strength to a glass ceramic. J Prosthet Dent. 2006;96:412-417.
41. White SN, Yu Z. Physical properties of fixed prosthodontic, resin composite luting agents. Int J Prosthodont. 1993;6:384-389.
42. White SN, Yu Z. Compressive and diametral tensile strengths of current adhesive luting agents. J Prosthet Dent. 1993;69:568-572.
43. White SN, Yu Z, Tom JF, et al. In vivo microleakage of luting cements for cast crowns. J Prosthet Dent. 1994;71:333-338.
44. Asmussen E, Attal JP, Degrange M. Adherence of resin-based luting agents assessed by the energy of fracture. Acta Odontol Scand. 1993;51:235-240.
45. Wang CJ, Millstein PL, Nathanson D. Effects of cement, cement space, marginal design, seating aid materials, and seating force on crown cementation. J Prosthet Dent. 1992;67:786-790.
46. White SN, Yu Z, Kipnis V. Effect of seating force on film thickness of new adhesive luting agents. J Prosthet Dent. 1992;68:476-481.
47. Goracci C, Cury AH, Cantoro A, et al. Microtensile bond strength and interfacial properties of self-etching and self-adhesive resin cements used to lute composite onlays under different seating forces. J Adhes Dent. 2006;8:327-335.
48. Strassler HE, Gonzales R. Unique delivery systems for temporary cements for provisional restorations. Contemp Esthet Restor Pract. 2005;9:70-72.
49. Strassler HE, Coviello V. FujiCEM resin reinforced glass ionomer cement. Contemp Esthet Restor Pract. 2001;5:84-87.
50. Strassler HE. An auto-mixing resin ionomer cement. Compend Contin Educ Dent. 2002;23:350-352, 354, 356.
a RelyX™ ARC, 3M ESPE, St.Paul, MN
b G-Cem™, GC America, Inc., Alsip, IL
c RelyX™ Unicem, 3M ESPE, St. Paul, MN
d Accudose Needle Tubes ™, Centrix, Shelton, CT
e BisCem™, Bisco, Inc., Schaumberg, IL
f MultiLink®, Ivoclar Vivadent, Amherst, NY
g Profin, Dentatus USA, New York, NY
h GC FujiCEM™, GC America, Inc., Alsip, IL
i Infinity®, Den-Mat, Santa Maria, CA
About the Authors
Howard E. Strassler, DMD
Professor and Director of Operative Dentistry
Department of Endodontics, Prosthodontics, and Operative Dentistry
University of Maryland Dental School
Baltimore, Maryland
Luis Guilherme Sensi, DDS, MS, PhD
Assistant Professor – Endodontics, Prosthodontics, and Operative Dentistry
University of Maryland Dental School
Baltimore, Maryland