Full-Mouth Rehabilitation: A Staged Approach to Treating the Worn Dentition
Giving the team the opportunity to evaluate how the patient responds to occlusal and esthetic changes
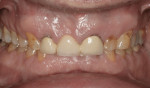
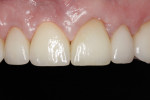
Full-mouth rehabilitation of the worn dentition presents many challenges and potential pitfalls. A systematic approach to diagnosis, treatment planning, and risk management is crucial for a predictable outcome. A staged approach to restoring the worn dentition provides the dental team with an opportunity to evaluate how a patient will respond to occlusal and esthetic changes. In this case, a 61-year-old retired engineer presented with concerns about the wear on his teeth (Figure 1). The case demonstrates the benefits of a staged approach and describes the successful alteration of the initial treatment plan when changes were necessary to better manage risk.
Case Report
The patient reported mild hypertension, which was controlled with medication. He had an acoustic neuroma removed in 1996, which damaged his facial nerve and resulted in right-side facial paralysis.
The patient reported comprehensive orthodontic therapy, including orthognathic surgery to advance his mandible in his late thirties. He had a 30-year relationship with his previous dentist and reported receiving regular preventive dental care during that time. He was not aware of any problems other than the wear on his teeth, which he felt had progressed over the previous 5 years.
The patient’s free gingival margins were equal with or coronal to the cementoenamel junction (CEJ). The patient exhibited thick, buttressing alveolar bone. Moderate horizontal bone loss with pseudo- and real periodontal pocketing was present.
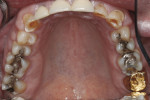
Defective restorations were present on teeth Nos. 14, 18, and 31. Many questionable restorations were noted, including the fixed partial denture (FPD) Nos. 7 through 9 (Figure 2). All molars were structurally compromised. While the caries risk was low, the patient’s overall biomechanical risk was increased due to the number of restored teeth, structurally compromised teeth, and failing restorations.
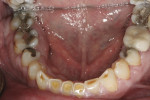
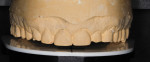
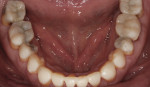
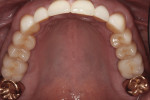
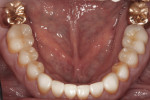
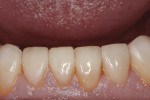
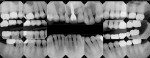
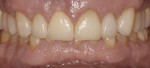
Since the patient had areas of severe wear that he desired to have restored and an actively changing occlusion, a proper functional diagnosis was imperative. The patient denied any muscle soreness or temporomandibular joint (TMJ) symptoms. His maximum opening was within normal limits at 46 mm, and there was no deviation on opening. Joint load and immobilization tests were negative. Severe attrition (> 2 mm) was present on teeth Nos. 6, 11, and 22 through 27 (Figure 3 and Figure 4). It is important to note that the lower incisors, despite being worn nearly to the gingiva, contacted the opposing teeth in maximum intercuspal position (MIP). This indicated that the compensatory eruption of the teeth was keeping pace with the rate of wear.
Nearly all other teeth exhibited moderate attrition. Posterior tooth wear was not consistent with sleep bruxism because cusp tips were preserved and secondary occlusal anatomy was present. The patient was diagnosed with occlusal dysfunction.
The patient’s right-side facial paralysis made esthetic evaluation more challenging. Initially, it was presumed the patient had low lip dynamics; however, after interacting with the patient over several visits it became evident that his smile was guarded. Even though the patient had an unesthetic anterior FPD, he said it did not bother him.
Treatment Plan
All teeth were planned for restorative correction due to the severity of wear on the anterior teeth and the need to increase the vertical dimension of occlusion (VDO).1 To minimize the biomechanical risk of tooth preparation, adhesively retained, enamel-supported restorations were planned wherever possible. Functional analysis was performed using a Kois deprogrammer.2
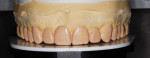
Bite records and a Kois LazrTrak (Kois Center, www.koiscenter.com) facebow record were taken and mounted using a Panadent articulator (Panadent, www.panadent.com) (Figure 5). The Kois Management Considerations: 10-Step Approach (Kois Center), a systematic tool for managing prosthetics utilizing a straightforward method of identifying, assessing, and managing risk, was used to develop a comprehensive and specific treatment plan that would achieve all treatment goals. Crown lengthening was performed on the casts, and a diagnostic wax-up was then completed (Figure 6). A preoperative stent fabricated from the wax-up would then provide guidance for both the periodontal surgery and chairside transitional bonding.
Treatment Phases
Periodontal pocket reduction surgery was performed for all posterior teeth. This provided more favorable clinical crown heights for the necessary restorative treatment. Teeth Nos. 6 through 11 and 23 through 26 had esthetic crown-lengthening surgery to expose the entire anatomical crowns. After the completion of initial periodontal therapy and surgery, the patient was placed on a 3-month maintenance schedule.
After a 3-month healing period, the patient was appointed for maxillary transitional bonding and a provisional FPD on teeth Nos. 7 through 9. Once anesthesia was administered, the retainers were sectioned and the FPD was removed.
At this time it was noted that tooth No. 7 had previously been over-prepared and, thus, the tooth had greater structural compromise than expected. Replacing the FPD now seemed like a less favorable option, and implant placement in site No. 8 with individual crowns on teeth Nos. 7, 8, and 9 was discussed. Given the greater biomechanical risk of using tooth No. 7 as a fixed bridge retainer, it was determined that future complications could be more easily prevented and managed with an implant and individual crowns. The patient elected to delay his decision about an implant until after the upper arch transitional bonding and provisional FPD were fabricated to allow evaluation of the occlusal scheme and esthetics.
After the chairside discussion about site No. 8, the transitional bonding was placed. Retentive grooves were cut in the occlusal surfaces of amalgam restorations and crowns. A clear silicone matrix had been made from the diagnostic wax-up. A bis-glycidyl methacrylate (bis-GMA) provisional FPD Nos. 7 through 9 was made from this matrix. The maxillary teeth were etched with 35% phosphoric acid, and a dental adhesive (OptiBond™ FL, Kerr Corp., www.kerrdental.com) was applied and light-cured. The clear silicone matrix was filled with heavy- and light-viscosity composite (RSVP™, Cosmedent, Inc., www.cosmedent.com) and seated over the teeth. The composite was light-cured through the matrix. The mandibular arch was treated in a similar manner at a subsequent appointment the same week (Figure 7).
A second Kois deprogrammer was fabricated from alginate impressions taken after the transitional bonding was completed. Because the initial deprogramming was challenging and took longer than usual, a second deprogrammer was used to verify the occlusal position and equilibrate the transitional bonding.
After occlusal equilibration, the patient was seen for follow-up appointments and minor adjustments. He reported that his bite felt comfortable, and no chips or fractures were noted on the composite. He functioned in the transitional bonding for more than 2 months before proceeding with definitive restorations.3
Definitive Restorations
Since care had been taken in establishing a stable occlusal reference point before beginning treatment and the patient had functioned well with the restorative prototypes, the teeth could now be prepped segmentally: full arch, quadrant, or even one or two teeth at a time. This approach gave the dentist greater flexibility and predictability than if all the teeth are prepared at once without “test driving” the occlusion and esthetics with transitional bonding.4 Maintaining solid posterior occlusal stops was critical during treatment since the patient’s VDO had been increased and length added to the anterior teeth. The decision was made to prepare all the molars on the left side first (teeth Nos. 14, 15, 18, and 19) and cement these restorations, and then prepare the molars on the right side (teeth Nos. 2, 3, 30, and 31). The second molars received full gold crowns to reduce the risk of chipping porcelain. After the molars were restored, the patient decided that he was ready to proceed with implant placement in site No. 8. A 4-mm x 13-mm implant (Astra Tech OsseoSpeed™, DENTSPLY Implants, www.dentsplyimplants.com) was placed, and the provisional FPD was adjusted to provide temporization during the healing period.5
Initially, since a metal ceramic FPD was planned for teeth Nos. 7 through 9, porcelain-fused-to-metal (PFM) crowns were planned for all porcelain-faced, cohesively retained restorations to maximize the esthetic result by using the same type of veneering porcelain. Teeth Nos. 3, 14, and 19 had been restored with PFM crowns before the patient elected to have an implant placed in site No.8. Once the FPD was eliminated from the treatment plan, lithium disilicate (e.max®, Ivoclar Vivadent, www.ivoclarvivadent.com) became the material of choice; monolithic lithium disilicate was selected to restore the remaining posterior teeth,6 and lithium-disilicate cores with layered e.max porcelain were to be used for teeth Nos. 6 through 11 and 22 through 27 (Figure 8 and Figure 9). The implant replacing tooth No. 8 would be restored with a custom-shaded zirconia abutment (Atlantis™, DENTSPLY Implants) and a layered lithium-disilicate crown.
The remaining maxillary teeth (Nos. 4 through 13) were prepared for lithium-disilicate (e.max) restorations. The impression for the No. 8 implant was made at this time also. Lastly, mandibular teeth Nos. 20 through 29 were prepared. Tooth No. 20 was unrestored and only required a direct composite to bring the tooth into occlusion. Notably, teeth Nos. 21 through 30 were all enamel-supported adhesively retained e.max restorations. The selection of conservative restorations limited the biomechanical risk to the teeth by reducing the amount of tooth preparation required. The teeth were prepared with the transitional bonding in place, allowing for minimal occlusal and, at times, facial reduction for many teeth.7,8 The case was prepared in four segments, and the final restorations for each segment were cemented before preparing the next section.
All crowns were cemented with RelyX™ Unicem 2 (3M ESPE), except the No. 8 implant crown, which was cemented with a resin-reinforced glass ionomer (GC Fuji PLUS®, GC America Inc., www.gcamerica.com). E.max onlays (Nos. 20, 28, 29, and 30) were cemented with a dual-cure resin cement (RelyX™ Ultimate, 3M ESPE), and e.max veneers (Nos. 22 through 27) were cemented with a light-cure resin cement (RelyX™ Veneer, 3M ESPE).
The patient was appointed for postoperative photographs and radiographs (Figure 10 through Figure 13). For added protection, a hard acrylic splint was fabricated by the laboratory for the patient to wear while sleeping.
Conclusion
This case illustrates a method to systematically diagnose, plan, and stage treatment to restore a patient’s worn dentition. The patient’s partial facial paralysis made esthetic evaluation more challenging. The patient’s repose position was the guiding determinant of anterior tooth length.9
The patient was extremely pleased with the final result and exhibited a full smile with considerably more tooth display than preoperatively (Figure 14). As a result of his improved esthetics, he says he has taken an increased interest in his oral hygiene, showing a marked improvement. The patient’s severely worn dentition was restored, a stable, comfortable occlusion was provided, and care was taken to minimize biomechanical risk.
Editor’s Note
This article originally appeared in the May 2014 issue of Compendium of Continuing Education in Dentistry.
Acknowledgments
The authors would like to thank and recognize Roberta Shaklee, DDS, MS, for periodontal surgery and Tony Kardelis, DDS, MS, for implant surgery.
References
1. Kois JC. New challenges in treatment planning: incorporating the fundamentals of patient risk management. Part 2. Journal of Cosmetic Dentistry. 2011;27(1):110-123.
2. Jayne D. A deprogrammer for occlusal analysis and simplified accurate case mounting. Journal of Cosmetic Dentistry. 2006;21(4):96-102.
3. Bakeman EM, Kois JC. The myth of anterior guidance: 10 steps in designing proper clearance for functional pathways. Journal of Cosmetic Dentistry. 2012;28(3):56-62.
4. Bynum JH. Clinical case report: Testing occlusal management, previewing anterior esthetics, and staging rehabilitation with direct composite and Kois deprogrammer. Compend Contin Educ Dent. 2010;31(4):298-306.
5. Kois JC, Kan JY. Predictable peri-implant gingival aesthetics: surgical and prosthodontic rationales. Pract Proced Aesthet Dent. 2001;13(9):691-698.
6. Valenti M, Valenti A. Retrospective survival analysis of 261 lithium disilicate crowns in a private general practice. Quintessence Int. 2009;40(7):573-579.
7. Magne, P, Beleser U. Novel porcelain laminate preparation approach driven by a diagnostic mock-up. J Esthet Restor Dent. 2004;16(1):7-16.
8. Palmer KM. Use of additive dentistry decreases risk by minimizing reduction. Compend Contin Educ Dent. 2012;33(5):346-352.
9. Misch CE. Guidelines for maxillary incisal edge position—a pilot study: the key is the canine. J Prosthodont. 2008;17(2):130-134.
About the Authors
Kenneth E. LeVos, DDS, received his DDS in 2002 from West Virginia University School of Dentistry and completed a general practice residency in 2003 at the Loma Linda VA Medical Center in 2003. He is a Fellow of the Academy of General Dentistry and a Mentor at the prestigious Kois Center in Seattle, Washington. He is in private practice in Evergreen, Colorado.
Angelika Oeckl graduated in 1983 from a 3.5-year dental technician program in Berlin, Germany and has lived in Seattle, Washington since 1999. She is the owner of Subrisi Smile Technology in Kirkland, Washington. She has attended many lectures and education programs in the US and internationally and is currently attending the Kois program.
Read More
For more information on implants, check out these articles.
Contemporary Treatment of the Fully Edentulous Mandible
Barry McArdle, DMD
dentalaegis.com/go/idt720
The Evolution of Implant Abutments for Fixed Partially Edentulous Restorations
Mark Stueck, CDT
dentalaegis.com/go/idt721
Guidelines for Single-Tooth Implant Success
Lyndon F. Cooper, DDS, PhD; and Oliver C. Pin-Harry, DDS, MS
dentalaegis.com/go/idt729
Cone-Beam Computed Tomography and Dental Implant Placement
Daniel Alter, CDT, MDT
dentalaegis.com/go/idt727
Achieving Exceptional Implant Esthetics
Jeffrey A. Babushkin, DDS
dentalaegis.com/go/idt728