Learning with Practice
Perseverance makes the difference in masking the dark stump shade of a single tooth
Custom shade matching can be an arduous task for technicians. Often the host of variables with which they must contend are of greater concern to them than they are to the patient or dentist. When a patient presents with a single central tooth that must be matched, and the intrinsic stump shade is a very dark, the challenge of shade selection can be great. Adding to this difficulty may be additional variables such as the lack of prepared tooth structure and minimal opacity of the surrounding natural dentition, prompting dental technicians to question whether they are ready to take on the challenge.
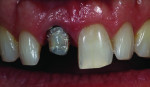
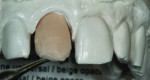
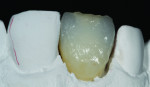
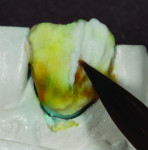
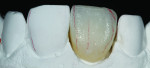
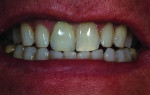
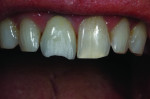
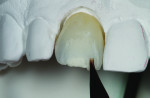
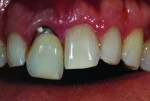
When this combination of factors presented in a 40-year-old male patient, the critical difficulty in the shade-matching process began with dehydration of the surrounding dentition and the speed with which the level of translucency changed with the loss of moisture. As soon as the mucosa was retracted for assessment of tooth shape and size, the loss of hydration changed the level of opacity by more than 50%. The colors present in the adjacent central included beige and orange at the incisal one-third, gray and white on both the mesial and distal aspects, and a crack line extending from the incisal all the way to the gingival line. Preparation of the facial thickness provided approximately 1 mm of room allowance, where 1.5 mm would have helped the author create additional room for porcelain and opacity for masking the dark stump shade. The overlay of a flowable composite helped to lessen some of the dark intrinsic show-through shade (Figure 1).
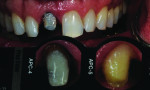
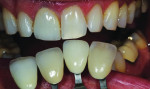
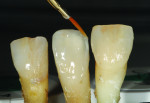
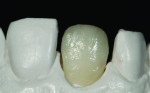
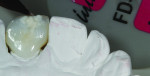
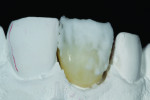
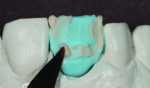
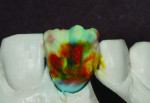
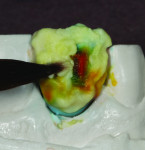
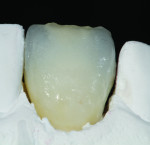
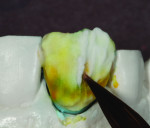
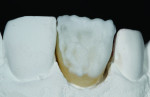
The author chose to create a porcelain restoration in order to combat his space limitations and better match the patient’s adjacent teeth, which exhibited a high-level of translucency. Choosing the best porcelain shade representation for the prepared tooth first required selection of the darkest color present, a C1 base, as well as the mesial and distal aspects, which exhibited significant gray enamel. Color choices were selected using the author’s own Chairside Shade Guide System (LSK121, www.lsk121.com)—custom-made shade tabs created with feldspathic ingots, which have higher levels of translucency (Figure 2). Next, the opacity, translucency, and enamel shades were selected from a porcelain shade guide for additional reference, as were choices of layered porcelain to add over the pressed structure (Figure 3). To get a better understanding of the intricacy of colors found in the patient’s natural dentition, extracted teeth were used to try out various stains and effects. Natural teeth were prepared and colors were layered over dentin and enamel to observe the reaction on the teeth. This provided a tool to better understand how to recreate the translucency and the mammelons that were present on the adjacent central, using hues of orange and white (Figure 4).
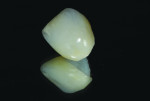
With the custom shade selection completed, the contoured wax-up was compared to the adjacent teeth on the study model (Figure 5). The feldspathic pressed ceramic ingot chosen for this case was a bleach shade, Initial PC-BO (GC America, www.gcamerica.com), because it would provide the most opacity while still allowing a translucent intrinicity (Figure 6). After pressing the ingot, the core foundation was stained using a light orange and brown tone for the first bake (Figure 7). Low-fusing layered fluodentin, Initial FD-93 sand shade (GC America, www.gcamerica.com), was applied to the middle two-third’s incisal aspect and extended along the line, recreating the appearance of the crack from the distal incisal into the middle-body one-third (Figure 8). The facial aspect was layered with enamel opal in blue Initial EOP0-4 and enamel 59 (Figure 9). After firing at 780 C°, the axial walls appeared to have a grayish hue, with additional translucency, and the mammelon characterization on the incisal edge appeared chalky and distinct (Figure 10).
Next, the full facial aspect was layered with translucent opal, Initial TO porcelain, up to the cervical height (Figure 11). The incisal two-third’s aspect of mammelon was decreased using beige stain brushed over the top of the translucent addition (Figure 12). More gray enamel opal EOP-4 was added, along with translucent opal TO and translucent blue TM01, and the mottled characterization was brushed onto the facial aspect from the middle one-third to the incisal edge. This was designed to highlight the mammelons and mimic the patterns observed in the natural dentition (Figure 13). Translucent opal TO was added to the mesial, distal, and incisal aspects, and was used to highlight the top of the middle one-third. Each addition of the translucent powders combined to create the depth needed to match the grayish intrinsic hue that was present in the patient’s natural dentition (Figure 14). Enamel E-59 was layered over the enamel opal EOP-4 along the mesial and distal aspects, except where the vertical height and width of additional characterization for the crack line would be built up (Figure 15).
Additional depth was added to the middle body by using more of the translucent grey TM-05 and by adding enamel intensive EI-14 in yellow to the mesial and distal aspects (Figure 16). Enamel 59 was layered over the full facial aspect, and the crack line was defined with gray enamel intensive, EI-11 (Figure 17 and Figure 18). After firing the restoration using the low-fusing firing parameter of 770 C°, the restoration had high levels of translucency on the axial walls, but still lacked translucency in the middle body (Figure 19). More of the enamel intensive EI-14 in yellow was applied over the entire facial surface, leaving the distal one-third, which was covered with a translucent modifier in white, TM-02. The crack line was defined from the incisal edge to the height of the cervical one-third aspect, with TM-02 separating the translucency visually (Figure 20).
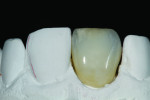
The full facial aspect was then covered with a layer of translucent neutral TN, and the restoration was fired again at 770 C° in the porcelain oven (Figure 21 and Figure 22). After firing, the contours were marked, giving the defined placement of anatomy and texture where reductions were ground down (Figure 23). The patient presented for the try-in, but the placement showed the color was not quite right. The shading needed to be bluer, and the tooth shape needed less mammelon. The gray hue and level of translucency were good, but the beige lesion that presented, which would blend with the adjacent tooth, would need to be built back up to bring the central and the bite back in line (Figure 24).
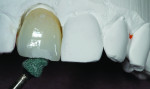
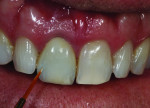
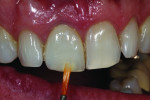
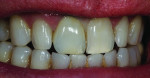
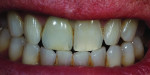
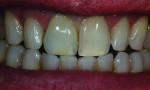
To clearly visualize the proportion of the lesion of the adjacent tooth and adequately restore the characterization in the build-up process, the final cutback was done in the patient’s mouth (Figure 25). The bulk of the porcelain was ground with a greenstone while the restoration was placed over the model (Figure 26). The addition of color was added to the incisal middle two-thirds using cervical translucent in pale orange, CT-23, and the translucent neutral covered the remaining incisal cutback (Figure 27). The fired restoration, as evaluated on the model, showed greater depth and definition to the color of the added characterization of the lesion (Figure 28). But after being placed back into the patient’s mouth, the restoration still was not quite right. At this point, the restoration was more visibly blue and the crack line had disappeared (Figure 29). The incisal one-third required external staining using a combination of orange, beige, and white to create a greater illusion of depth to the character of the lesion (Figure 30). The cervical one-third was stained with pale yellow, and the fired restoration then showed a natural appearance of both the characterization and the translucency (Figure 31). When the patient presented for a third try-in, the color match to the other central looked much closer than in the previous visits (Figure 32). The straight angle picture shows that the shape and shade match of the mesial contact was almost the same as the adjacent tooth and opposing dentition, but the difficulty in maintaining hydration of the enamel made it nearly impossible to determine if the distal aspect was adequately matched (Figure 33). The wider distal aspect of porcelain required to close the interproximal contact made for a long enamel spread (Figure 34). But the proportion of the cervical collar into the gingival margin looked natural, and after thoroughly wetting the teeth, the mesial and distal aspects shared the same level of translucency as the patient’s natural dentition (Figure 35).
Contending with the variables of a difficult shade match to a dark intrinsic stump, less-than-adequate tooth structure after preparation, and the loss of hydration in a case like this one would likely try the patience of any technician. When presented with these complex criteria, technicians may need to ask themselves if they are ready for this difficulty on the day the patient arrives. With the color continuing to change due to dehydration, the eye for detail on any given day may differ for each person. Proper tooth preparation for the best choice of materials may not be within the control of the laboratory. Conquering these challenges are what separate the best laboratories from the competition. Taking all of the factors into consideration, plus careful planning and the acceptance of mistakes, can make a challenging case a rewarding learning experience.
About the author
Luke S. Kahng, CDT
Owner
LSK121 Oral Prosthetics
Naperville, IL
To read more from this author, visit dentalaegis.com/go/idt682.