Implant Planning Software
A process and technology update
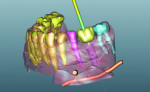
Cone Beam Computed Tomography (CBCT)—also known as dental 3D imaging—was first introduced by NewTom to the European market in 1996 and to the US market in 2001.1 Cone-beam CT produces images in a DICOM (Digital Imaging and Communications in Medicine) format. These images of the patient can be interpreted with software that reconstructs them into both two- and three-dimensional formats. The information delivered by this technology creates invaluable details for numerous dental conditions and is used in treatment planning for dental implant therapy.2 Although its use is not yet considered the definitive standard of care, the industry is moving in that direction. In 2012, the American Academy of Oral and Maxillofacial Radiology (AAOMR) updated its guidelines for dental imaging in implant treatment, suggesting Cone Beam CT as the preferred method for presurgical assessment of dental implant sites.3 As the clinical use of Cone Beam CT has increasingly been adopted into the dental office, so does the use of virtual implant planning software for implant placement. Implant planning software provides the dental team with a number of tools used to analyze existing structures and aid in the planning for precise implant placement. Many software platforms enable the transfer of the virtual implant placement to a surgical guide (template) and then precisely converts the virtual plan into the patient’s surgical site.4,5 CBCT-based surgical guides are currently available, in varying levels of capacity, for all implant systems and any clinical condition from single implant placement to full mouth reconstruction including immediate-load “All-on-4.” Surgical guides are generally designed similar to occlusal splints and contain metal guide tubes in the areas of future osteotomies to precisely control the location, trajectory, and often the depth of the surgical drills (Figure 1). The tubes are designed to work with the clinician’s existing implant surgical armamentarium or a specially designed fully-guided surgical kit.
Guide Design
The first step in the process is to choose the type of surgical guide—tissue-supported, tooth-supported, or bone-supported. All planning software systems can accommodate tooth or tissue supported guides. However, bone-supported guides placed on a fully flapped ridge are accommodated by a limited number of software systems (Simplant, Invivo5, BlueskyPlan). Tissue-supported guides, with or without fixation pins, have the potential to introduce error into the process since the fit of both the scan appliance and surgical guide are based upon the compression of mucosa.6,7 Both tooth- and bone-supported guides fit to hard stable structures reducing the potential for error.6
Software Options
Once the guide type is determined, you will need to select a virtual implant planning software. There are many factors to consider in this decision making process, since thesoftware also affects the protocols involved in the process. Each system has advantages and disadvantages that should be considered. A discussion about software selection with key dental team members who will be collaborating on cases and approving final case plans may be prudent.
Key Software Considerations
Here are some key factors to consider and questions to ask when selecting implant planning software.
Implant Library
Some software programs have a limited library offering while others offer a worldwide selection of popular implant brands.
Software Operation
Does the software require the DICOM data to be reformatted? Can individual structures be segmented? Can virtual teeth be added (Figure 2)? Is there optical scanner integration?
Sophistication
Is there support for guided alveolar surgery, bone reduction, and guided surgery kit compatibility with detailed drilling reports?
Guide Fabrication Time
How much time is required for guide fabrication? Can guides be produced in-house or is the use of a central fabrication center required? Is guide production done domestically or internationally?
Cost
What is the cost of software ownership? It can range from no charge to tens of thousands of dollars. What is the cost to manufacture a guide in-house versus outsourcing?
Collaboration
Is a free version or viewer available to share case plans with dental team members? What other tools aid in communication with clients?
Scan Appliance
Some systems require the use of scan appliances while others allow them to be imported if desired.
When is a Scan Appliance Required?
A scan appliance (aka. radiographic guide) is a rigid acrylic appliance containing the teeth to be restored that fits over the existing teeth and tissue. Although in many situations implant-planning software can be used to create a CBCT-based surgical guide from a CT scan or a CT scan combined with a model or digital impression, some planning software requires the use of a scan appliance in the process of creating a surgical guide.
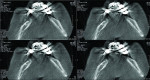
There are certain clinical situations that require the use of a scan appliance. One of those is the presence of metal-based restorations, which can cause excessive scatter the data. Excess scatter can render a scan unusable for guide creation without the use of a scan appliance. The amount of scatter can be determined from a preliminary CT or existing radiograph or panoramic image (Figure 3).
Another clinical situation most often requiring the use of a scan appliance is in reconstructive cases. For surgeries involving the restoration of significant dentition, particularly in the anterior segment, it may be beneficial to have the tooth position verified intraorally with a tooth setup converted to a scan appliance. Edentulous cases also neccesitate from the use of a scan appliance. Without a scan appliance, implant position may not coordinate with final tooth position.
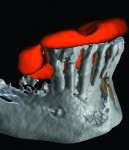
The design of scan appliances varies from software to software. However, software programs typically include radiopaque markers (Figure 4) for registering and merging the appliance in the planning software with multiple sets of DICOM data and/or a physical scan of a model. The proper fabrication of the scan appliance is the critical first step in the process. In many situations the final surgical guide is a digital duplicate of the scan appliance, so design and fit are crucial (Figure 5). Final impressions and master casts must be precise to ensure fit at the time of surgery. Considerations include material thickness, proper placement of radiopaque markers, density of material, and adequate tooth and tissue coverage for guide sleeves.
Can I Avoid Using a Scan Appliance?
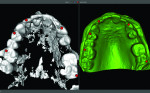
Due to advancements in CBCT planning software and optical scanners during the past few years, the process for treatment planning, guide manufacturing, and surgical guidance has become more streamlined, affordable, and accessible. For example, when using some software planning systems in combination with accurate in-laboratory scanners, a scanned STL model can now be merged with DICOM data (Figure 6). This eliminates the need for CT scan appliances in some circumstances. Not only does this eliminate an appointment, it reduces case cost, decreases treatment time, improves the fit of the appliances on the model, and, most importantly, provides improved planning information. A CBCT scan allows an implant to be planned according to visible radio-opaque objects, the bone and scan appliance. The incorporation of a scan model adds the complement of soft tissue location and improved tooth details.3
Partially edentulous treatment plans that have remaining teeth on both sides of the arch without metal restorations are candidates for the no scan appliance technique. Metal creates scatter, rendering it difficult or impossible to register a CT Scan with the model scan. No-scan technique uses the virtual placement of teeth or a scan of a functional diagnostic wax-up to determine tooth position for virtual surgical planning. The scanned model image is intimately superimposed over the DICOM data, rendering accurate hard and soft tissue surfaces in the software from which improved clinical decisions can be made.
Other Software Considerations
Other systems allow a guide to be planned and manufactured directly from the DICOM data (Invivo 5). Some companies espouse a more direct approach and allow a surgical guide to be made directly in the office on the day of surgery (Sirona). Sirona advocates a multiphase direct/indirect approach by combining CEREC® design software with DICOM data from their Galileos CT scanner. Conversely, other software modules, such as 3Shape’s Implant Studio, Dental Wings’ DWOS CoDiagnostiX, and Planmeca’s Romexis offer a more laboratory-centric approach. After the guide is fabricated for export in the software, the implant position can be imported back into the dental system software for the fabrication of provisional prosthesis and custom healing abutments, as well as the final restoration.
As the adoption of cross-sectional imaging obtained from CBCT technology continues to increase, and the interpretation software to produce guides evolve, dental technicians will continue to have the opportunity to help clinicians use these tools and technology for the benefit of the patient. There has been and will always be practices that would prefer to adopt a singular approach in the treatment of their patients and create guides in-office or work directly with a centralized guide production. However, many other clinicians find benefit in collaboration with dental technicians and value their restorative-based perspective in the planning process.
References
1. Hatcher DC. Operational principles for cone-beam computed tomography. JADA 2010;141(10S):3S-6S.
2. Arison V, Karabuda CZ, Mumcu E, Özdemir T. Implant positioning errors in freehand and computer-aided placement methods: a single-blind comparative study. Int J Oral Maxillofac Implants. 2013;28(1):190-204.
3. Tyndall DA, Price JB, Tetradis S, et al. Position statement of the American Academy of Oral and Maxillofacial Radiology on selection criteria for the use of radiology in dental implantology with emphasis on cone beam computed tomography. Oral Surg Oral Med Oral Pathol Oral Radiol. 2012;113(6):817-826.
4. Sarment DP, Sukovic P, Clinthorne N. Accuracy of implant placement with a sterolithographic guide. Int J Oral Maxillofac Implants. 2003;18(4):571-577.
5. Alamri HM, Sadrameli M, Alshalhood MA, et al. Applications of CBCT in dental practice: a review of the literature. Gen Dent. 2012;60(5):390-402.
6. D’haese J, Van De Velde T, Komiyama A. Accuracy and complications using computer-designed stereolithographic surgical guides for oral rehabilitation by means of dental implants: a review of the literature. Clin Implant Dent Relat Res. 2012;14(3):321-335.
About the author
BJ Kowalski is the President of ROE Dental Laboratory in Cleveland, OH.