Two Approaches to an Esthetic Anterior Titanium Abutment
Using technology as a tool to achieve exceptional results
Mike Dominguez, CDT, TE
We have always used technology as an extension of ourselves, as a tool to achieve what the mind has conceived. Technology has taken many forms over the eons, from the use of pre-historic stone tools, to the more sophisticated metal cast tools of early civilizations, to the electric industrial revolution of the 1800s, to today’s virtual 3D environment. Regardless of its sophistication and complexity, technology in all its forms remains the same—it’s just a tool.
The dominant technological tool of today’s modern dental laboratory and dental practice is CAD/CAM technology. As with any other technological tool, CAD/CAM requires a skilled hand and knowledgeable mind to use it to its fullest potential.1 Whether we are using a hand tool or a computer-driven tool, both require the skill and mind of a technologist to stack porcelain for an esthetic, natural-looking result or to CAD design the most complex of restorations. Sure, there are libraries of occlusal morphology stored in the CPUs, but the mind and eye of a trained dental professional is required to create a restoration that is esthetic, functional, and relevant to the individual patient. The library of occlusal designs is merely a tool to help us get ever closer to replicating nature. CAD/CAM, well done, requires talented hands and minds.
Technologists’ ultimate goal for creating dental restorations is to attain the highest level of esthetics and stability in an efficient and predictable manner. In the anterior region, customized zirconia implant abutments have been called upon to provide esthetics, but they have been lacking in terms of stability when compared to metal abutments.2,3 UCLA cast-to abutments with porcelain collars around the gingival margin provide proper esthetics and strength, but they can be cost prohibitive and labor intensive.4,5 With the use of CAD/CAM technology—in this case, the NobelProcera™ (Nobel Biocare, www.nobelbiocare.com) scanner—and modern materials such as GC Initial™ Ti and GC GRADIA® ceramic-composite (GC America, www.gcamerica.com), we are able to fabricate customized milled titanium abutments that are stable and esthetic.
In this article, the author will examine how using technology and modern materials can help technologists fabricate an esthetic and stable anterior titanium implant restoration with a fired porcelain or layered ceramic composite collar. Along with the advances in CAD/CAM technology and a solid understanding of modern materials, it is important to be mindful of the traditional methods of fabricating stable and esthetic restorations and use technology to match or exceed those standards and expectations of success with the added efficiency.6
The traditional method of fabricating a metal implant abutment with a porcelain collar begins with a cast-to abutment that is designed in wax. After investing and casting, porcelain is stacked around the gingival margin and is extended at least 1 mm below the gum line in order to mask any metal show-though at the gingiva. Then, the stable and esthetic abutment is ready for a cementable restoration. We can achieve the same esthetics and stability using the NobelProcera scanner and GC Initial Ti or GC GRADIA. Following are two cases and the step-by-step methods to create an esthetic crown on a titanium abutment.
Creating an Anterior Abutment using GC Initial™ Ti
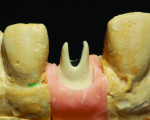
Step 1 In the case-planning phase, the author documented the shade, tissue level, and esthetic goals of the patient. For this case, a custom-healing abutment was fabricated chairside by the clinician. The patient visited the laboratory for a custom shade appointment to replace tooth No. 10. A titanium abutment with a fired porcelain collar and a high-noble PFM restoration with a porcelain shoulder were prescribed by the clinician.
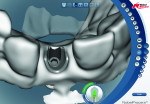
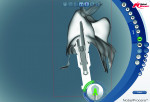
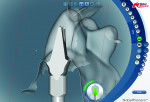
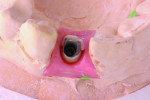
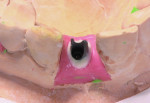
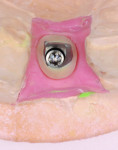
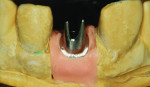
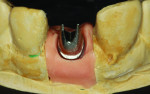
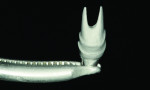
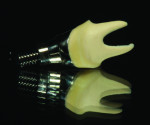
Step 2 Using the NobelProcera scanner to scan the model and CAD software, a titanium abutment was designed and customized to fit snugly into the sulcus. It is important to understand the surgeon’s goal for the fit of the abutment in this area. It is possible to control the amount of pressure exerted on the tissue using the Nobel CAD software (Figure 1 through Figure 3).
Step 3 The abutment design was transmitted to the Nobel Biocare production facility for milling in titanium. When the milled abutment arrived back at the laboratory from Nobel, the author evaluated the fit of the abutment, the gingival margin, as well as the clearance for the PFM restoration.
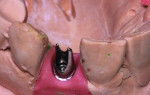
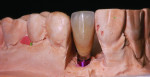
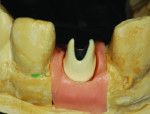
Step 4 The author prepped the milled abutment along the gingival margin to create room for the porcelain collar. The prepped area should be at least 1 mm subgingival in order to mask the metal from show-through. For stability, the cutback should not exceed 2 mm.7 The author reduced the circumference of the abutment by about 0.75 mm to provide room for porcelain. Because this will be a PFM restoration with a porcelain margin, technicians must be sure that their porcelain collar will be wide enough in that area (Figure 4).
Step 5 The author sandblasted the layering area of the abutment using 125 μm AlO2 from Renfert ( www.renfert.com) and thoroughly rinsed the area and allowed it to bench set for 5 minutes. It helps to sandblast the abutment while it is screwed into a spare model analog in order to keep the connection free of abrasion (Figure 5).
Step 6 A layer of GC Bonder was applied to the abutment. GC Bonder powder is mixed into the Bonder Liquid for 1 minute or until the bonder granules are completely dissolved. The solution was briskly applied on the area to be layered. Applying the Bonder aggressively and liberally over the surface ensures that the surface tension will be broken and full-coverage porcelain can be applied without voids. The brush was dried and used to draw out any puddles of the solution from undercut areas. The goal is to produce even coverage throughout. After firing, the applied area should be black and shiny.
Step 7 A thin white wash of OM1 opaque modifier was applied to the abutment and fired, after which two thin layers of shaded opaque were applied (Figure 6). The abutment was then lightly sandblasted to remove only the oxide layer using 125 μm AlO2 (Renfert) with two bars pressure (Figure 7).
Step 8 The author used Iso-Stift (Renfert) as a separating medium on the tissue model. The abutment was placed onto the model and stacked with GC Initial Ti Opacious Dentin in the void created by the cutback. The author removed the abutment from the model and filled in any voids along the emergence and finish line and fired the abutment. Note: After firing, the porcelain will shrink, but it is not recommended to try and compensate for that. Let it shrink and add to the gap with the second firing. This method is more accurate and efficient than trying to grind in an over-build (Figure 8 and Figure 9). There is no need to re-apply Iso-Stift for the second firing.
Step 9 After firing, the author filled in any voids for proper fit using opacious dentin and fired (Figure 10 and Figure 11). After firing the second bake, the porcelain was lightly ground to fit back into the tissue model. The margin should then be reduced to equi-gingval or supra-gingival. The author polished the metal and porcelain along the emergence profile. If the abutment was initially fit into the sulcus prior to cut back, then a clean finish line will emerge at the completion of this step (Figure 12)
Step 10 The coping was designed for proper porcelain support, and a porcelain margin cutback was created. The author then prepared the coping for the opaque layer by sandblasting, rinsing, and firing on the oxide cycle.
Step 11 A thin white wash was then applied on the coping using OM1, then two layers of shaded opaque were added (Figure 13).
Step 12 The author used Iso-Stift on the abutment as a separating medium for the porcelain margin. For the porcelain margin, the author applied GC Initial MC Shoulder Opacious Powder first and overlaid it with Shoulder Trans Powder (Figure 14).
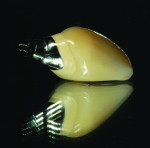
Step 13 The crown was stacked to full contour using GC Initial MC and the information collected at the custom shade appointment, then contoured and finished (Figure 15 through Figure 17).
Creating an Anterior Titanium Abutment using GC GRADIA®
The author followed Steps 1-5 from above (Figure 18 through Figure 19).
Step 6 GC Metal Primer was applied over the abutment, which was then set aside to dry. In this case, the cementable restoration was a layered IPS e.max® pressed crown (Ivoclar Vivadent, www.ivoclarvivadent.com) for tooth No. 8. Note: It was necessary to opaque the entire cementable portion of the abutment to take advantage of the translucent properties of the lithium disilicate restoration (Figure 20).
Step 7 The author applied a thin layer of Foundation Opaque onto the abutment and step cured it for 10 seconds on each side using the Optilux (Demetron) hand-held light cure unit. Two layers of shaded opaque were then applied, and each layer was light cured for 10 seconds on each side.
Step 8 The opaque layers were final cured in the Pentron Sculpture Curing unit (Pentron Clinical, www.pentron.com) for 2 minutes.
Step 9 The author then applied Iso-Stift to the tissue model as a separating agent and screwed the abutment into the tissue model.
Step 10 GC GRADIA Opacious Dentin was applied into the void created by the cutback and light cured for 10 seconds on each side (Figure 21).
Step 11 The abutment was removed and any voids on the emergence profile were filled in and light cured. Note: There is minimal shrinkage with this material, which makes finishing easier. The abutment was placed in the curing unit and final cured for 2 minutes.
Step 12 Using a carbide bur, the author lightly ground the abutment into place and smoothed the margin so that it was equi-gingival or supra-gingival. Note: If the abutment was initially fit into the sulcus prior to cutback, you will find a clean finish line at the completion of this step (Figure 22).
Step 13 The author polished the metal and GRADIA collar and fabricated the lithium disilicate restoration according to the information gathered at the custom shade appointment.
Step 14 The final crown was contoured and finished (Figure 23 and Figure 24).
Conclusion
The efficacy of CAD/CAM technology is realized when a skilled technician can design the abutment on the scanner and send the CAD file for milling, and then return to work on other cases while the abutment is being milled. When compared to the traditional methods of abutment and final crown fabrication—waxing, investing, burning out, casting, cooling, divesting, and fitting the abutment—the use of a CAD/CAM process is much more production workflow efficient.
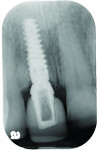
In addition to stability, esthetics, and an efficient process, there are specific advantages to using either GC Initial Ti or GC Gradia for the porcelain collar. The bond strength of GC Initial Ti to titanium is 59 MPa,8 which is comparable to a traditional PFM. In addition, this porcelain is radiopaque, so the marginal integrity can be verified with an x-ray as well as manually. Lastly, GC Initial Ti is fired porcelain and the process will be familiar to those accustomed to the traditional method of stacking porcelain to the cast-to UCLA abutment.
There are unique advantages to using GC GRADIA as well. It is important to keep the interface between the abutment and fixture as pristine as possible to reduce micro-movement. When using GC GRADIA for the porcelain collar, there will be no oxide layer to sandblast or polish because this ceramic composite is light cured. This is especially important for conical connections. The bond strength for GC GRADIA to metal is 29 MPa, which is higher than the ISO9693 standard for metal ceramics.9 For this material, adding mechanical retention, like undercuts, will improve the bond strength. Also, GC GRADIA is radiolucent, so marginal integrity will have to be verified manually or visually if the finish line is supra-gingival. However, the radiolucent properties of GRADIA do have advantages when clinicians use an x-ray to find errant cement that needs to be removed (Figure 25). Highly radiopaque cement is a must for implant dentistry.
Traditional methods for fabricating an esthetic and stable implant abutment can be streamlined with CAD/CAM technology and modern materials. Technology, as a tool, can marry the traditional approach of esthetic dentistry to the efficiency that today’s pace demands. Advanced technologies like CAD/CAM, in skilled hands, will produce stable and esthetic restorations in an efficient and predictable manner.
References
1. van Noort R. The future of dental devices is digital. Dent Mater. 2012;28(1):3-12.
2. Foong JK, Judge RB, Palamara JE, Swain MV. Fracture resistance of titanium and zirconia abutments: An in vitro study. J Prosthet Dent. 2013;109(5):304-312.
3. Martínez-Rus F, Ferreiroa A, Özcan M, et al. Fracture resistance of crowns cemented on titanium and zirconia implant abutments: a comparison of monolithic versus manually veneered all-ceramic systems. Int J Oral Maxillofac Implants. 2012;27(6):1448-1455.
4. Lewis SG, Llamas D, Avera S. The UCLA abutment: a four-year review. J Prosthet Dent. 1992;67(4):509-515.
5. Vigolo P, Majzoub Z, Cordioli G. Measurement of the dimensions and abutment rotational freedom of goldmachined 3i UCLA-type abutments in the as-received condition, after casting with a noble metal alloy and porcelain firing. J Prosthet Dent. 2000;84(5):548-553.
6. Kensel RP, Lin D. Retrospective analysis of porcelain failures of metal ceramic crowns and fixed partial dentures supported by 729 implants in 152 patients: patient-specific and implant-specific predictors of ceramic failure. J Prosthet Dent. 2009;101(6):388-394.
7. Geminiani A, Lee H, Feng C, Ercoli C. The influence of incisal veneering porcelain thickness of two metal ceramic crown systems on failure resistance after cyclic loading. J Prosthet Dent. 2010;103(5):275-282.
8. Lee HR, Schille CH, Woo YH, et al. Bond strength between cast/machined titanium and ceramics. Tübingen, Germany: Eberhard Karls Universität Tübingen.
9. Fernandes CA, Fibeiro JC, Larson BS, et al. Microtensile bond strength of resin-based composites to Ti-6Al-4V. Dent Mater. 2009;25(5):655-661.
About the Author
Mike Dominguez, CDT, TE
Owner
Kymata Dental Arts
Seattle, WA